[box type=”bio”] What to Learn from this Article?[/box]
1. Management of multiple congenital joint dislocation, sequence and principles?
2.Differentials of multiple congenital joint dislocations?
Case Report | Volume 3 | Issue 2 | JOCR April – June 2013 | Page 21-24 | Tiwari M, Sharma N
Authors: Mukesh Tiwari[1], Nishith Sharma[1]
[1] NIMS Medical College, Jaipur. Rajasthan, India
Address of Correspondence:
Dr Mukesh Tiwari: NIMS Medical College, Jaipur. Rajasthan, India E-mail- wakeuptum@gmail.com
Abstract
Introduction: Reduced intrauterine space gives rise to ‘packaging disorder’ which may involve joint dislocations or contractures. We present an unique case where mutiple joints were dislocated involving left congenital knee dislocation (CDK), bilateral congenital hip dislocation (CDH) and congenital talipes equino varus (CTEV)deformities.
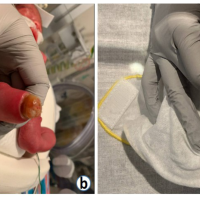
Case Report: A preterm baby boy born to mother with diagnosed oligohydramios presented with left CDK bilateral DDH and CTEV. The knee dislocation was treated first with gradual streaching and weekly above knee cast. At 7th week good flexion was achieved at both knees and abduction splint for DDH (using double diaper) with ponseti cast for CTEV was done. At one year follow up all joints were reduced and maintained well with baby able to stand with support.
Conclusion: Packaging disorders may present with multiple dislocations and deformities. Early intervention with serial casting and manipulation minimises disability and prevents ambulatory problems. In our case there was a good response to manipulation and serial casting. This differs from cases with inherent pathology like arthrogryposis where response to treatment is not so good.
Keywords: Congenital genu recurvatum, Develpmental dysplasia hip, CTEV, Clubfoot, serial manipulation, packaging disorders.
Introduction
Congenital knee dislocation (CDK) is a rare malformation characterized by hyperextension of the knee and marked limitation of flexion with associated anomalies. The Chanssier first reported about such case in 1812 followed by Swiss physician Chatelaine in 1822 [1]. Diagnosis is simple and can be done by checking the hyperextension at the knee and palpating the excessively prominent femoral condyles. The estimated incidence of this anomaly is 1:100000 live birth second to incidence of CDH. Combination of CDK and DDH quite rare. Congenital hyperextension of the knee can be divided into three grades (By Laurence) [2] according to severity: grade 1, congenital hyperextension; grade 2, congenital hyperextension with anterior subluxation of the tibia on the femur; and grade 3, congenital hyperextension with anterior dislocation of the tibia on the femur [1].The etiological factor for genu recurvatum are still not known in details but factors which have contributed are breech position, lack of intrauterine space, trauma to mother, quadriceps contracture or fibrosis, absence of suprapatellar pouch, deficient or hypoplastic ACL [3]. Except these intrinsic causes there are also extrinsic factors which can lead to genu recurvatum this include intrauterine pressure leading to malposition of knee and foot. A combination of intrauterine pressure build up with reduced intrauterine space may lead to ‘packaging disorder’ causing malposition of multiple joints like hip, knee and foot too. Spontaneous reduction has been mentioned with extrinsic causes while the intrinsic causes may be finally tackled with surgery but this may not be always true [4]. We present one such case with multiple dislocation of joints in a new born involving congenital genu recurvatum of left knee joint with bilateral congenital hip dysplasia with quadriceps contracture with CTEV.
Case Report
Our case was a preterm (35 weeks) baby boy born by normal vaginal delivery with history of oligohydraminios, presented with extreme hyperextension of left knee with toe almost touching the abdomen (Fig.1 ) with associated anomalies present; patient had CDH(Fig.3 and 4), Quadriceps contracture(Fig.2 ) and CTEV in the same involved lower limb. Left hip showed acetabular dysplasia. The affected left side shows presence of increase in depth of iguinal fold, abduction is limited at the left hip, the Ortolani and Barlow test was positive. Telescopic sign was positive. The feet on both side were inverted to about 30 degree and foot was pointing down wards. The ankle was in equines the feet were supinated and adducted, dorsiflexion beyond 90 degree was not possible. Tibia was normal and was not having an internal torsion. Passive stretching followed by above knee (toe to groin) POP splints was used from the first day. The basic principal of correction of adduction first followed by varus & then equines is followed. The splints were changed every seventh day with gradual bending. In about a month time knee flexion range of movement about 70 degree was achieved. There is need to be cautious at this time to avoid excessive & forceful correction as this may lead to damage to epiphysis & future growth abnormalities. As mentioned by Nogi et al, when there is concurrent presence of DDH with this knee abnormality then knee problem should be treated first as good knee movements can help with correction of hip abnormality [19]. In three months’ time, the left knee adopted a normal shape and position. The splints were discontinued and the mother was advised to continue passive stretching. The CDH was treated by abduction splints (wearing of double diapers) for six weeks. CTEV was treated with serial manipulation and POP Casts. A follow up at the age of one year showed normal position of both knees(Fig.5) as well as both hips.
Discussion
Congenital genu recurvatum is an uncommon condition first described in 1822 that present more commonly in girls than in boys [2, 3, 4] and in more than half of the cases it is bilateral.. Associated anomalies are CDH, CTEV, spina bifida, scoliosis, coxa valga, dislocation of the elbow, anomalies of the toes, cleft palate, mongolism, hydrocephalus, facial paralysis, and cryptorchidism [4]. Associated anomalies are very common, with an incidence variously reported as from 60 to 100 % [2, 5]. The most frequent associated anomaly is congenital dislocation of the hip. In a study of 155 children with congenital dislocation of the knee, Katz, Grogono, and Soper found other musculoskeletal abnormalities in 82 children; 45 had congenital dislocation of the hip [3]. In their study of 15 knees with congenital hyperextension and anterior subluxation of the tibia, Curtis and Fisher found an abnormality of the hip in 11 patients [6]. Johnson, Audell, and Oppenheim found other abnormalities in 88% of their 17 patients [7], and Nogi and MacEwen reported congenital hip dysplasia in eight of 17 patients [8]. The incidence of breech presentation is significantly higher than in normal children. The role of Oligohyraminios in CDK is still unclear may be the position in utero may influence the development of dislocation of the knees. The limited movements of the foot with presence of internal rotation of feet is postulated as a cause for the club foot [14]. The less availability of space in utero may lead to tight ‘Packaging’ of limbs leading to multiple dislocations as seen in our case. Similar picture with multiple dislocation is also seen in cases where there is pathological soft tissue like arthrogryposis multiplex congenita. Possibly the point of differentiation between the two will be ease of correction and localized affection of one or two limbs with involvement of all fours limbs in arthrogryposis. Also in cases with arthrogryposis there will not only be joint dislocations but also associated severe soft tissue contractures
The aim of treatment should be to obtain a stable straight limb that would permit ambulation. The treatment options depend on the age of the patient and the severity of the dislocation at presentation. Non-operative treatment is mainstay and is usually successful, if commenced at birth [7,10,11,12,13]. Early gentle manipulation, combined with serial splinting and casting is the mainstay of treatment in CDK. All cases with extrinsic reason like packaging disorder should be treated conservatively. In case of intrinsic causes like arthrogryposis one should evaluate first the reducibility of the knee. If the reduction is not achievable then a period of manipulation and casting or a period of traction (1-2 weeks )may be necessary. If at this stage the reduction cannot be maintained by manipulation or a period of traction then surgery is indicated. If in CDK, 90 degree of flexion can not be maintained even after 3 months conservative treatment then surgical options should be opted. The surgical options include Percutaneous needle tenotomy, Z plasty of quadriceps mechanism, V-Y advancement, Achillies tendon graft and release of anterior capsule and intra articular adhesions [19,20,21, 22]. The best time of surgery is before the child starts to walk. Late presentation may require surgical release of the anterior soft tissue structures of knee, quadricepsplasty, and osteotomy of the distal part of the femur [19,20]. In our case we did early gentle manipulation with serial POP splints and we achieved full correction within a short period of time. The key to success was the gradual change in the angle of the splints and stable correction which allowed early correction. Emphasis should be laid on the immediate recognition and treatment of the condition to avoid destructive surgical procedure later on. Same applies to other deformities in ‘Packaging’ disorders and prognosis seems to be quite good with conservative management.
Conclusion
Multiple joint dislocations are not common and may be due to packaging disorder in utero. Starting the treatment early will be helpful in achieving good results by conservative modalities.
References
1. Campbell operative orthopaedics 11th edition. Congenital Hyperextension and Dislocation of the Knee: 1113-1115.![]()
2. Fernandez PF, Silva JR. Congenital dislocation of the knee. International Orthopaedics 1990; 14:17-19.![]()
3. Katz MP, Grogono BJ, Soper KC. The aetiology and treatment of congenital dislocation of the knee. Journal of Bone Joint Surgery [Br] 1967; 49B:112-119.![]()
4. Niebauer JJ, King DE. Congenital Dislocation of the Knee. Journal of Bone and Joint Surgery [Am] 1960; 42-A: 207-225.![]()
5. Curtis BH, Fisher RL. Heritable congenital tibiofemoral subluxation. Clinical features and surgical treatment. J Bone Joint Surg Am. 1970 Sep;52(6):1104-14.![]()
6. Curtis BH, Fisher RL. Congenital hyperextension with anterior subluxation of the knee. Surgical treatment and long-term observations. J Bone Joint Surg Am. 1969 Mar;51(2):255-69.![]()
7. Johnson E, Audell R, Oppenheim WL. Congenital dislocation of the knee. J Pediatr Orthop. 1987 Mar-Apr;7(2):194-200.![]()
8. Nogi J, MacEwen GD. Congenital dislocation of the knee. J Pediatr Orthop. 1982;2(5):509-13.![]()
9. Provenzano RW. Congenital Dislocation of the Knee. Report of a Case. New England Journal Medicine 1947 236: 360-362.![]()
10. Reach JW, Richard BS. Instructional Case: Congenital Dislocation of the knee. Journal of Paediatric Orthopaedics 1988; 8:226-229.![]()
11. Muhammad KS, Koman LA, Mooney JF 3rd, Smith BP. Congenital dislocation of the knee: overview of management options. J South Orthop Assoc. 1999 Summer;8(2):93-7.![]()
12. Mohammad AI, Abdullah AS, Eman AK. Case Report: Congenital Genu Recurvatum with Dislocation of the Knees. Kuwait Medical Journal 2004; 36 (3):203-205.![]()
13. Finder JG. Congenital Hyperextension of the Knee. In Proceedings of the Joint Meeting of Orthopaedic Associations. Journal of Bone Joint Surgery [Br] 1964; 46B: 783.![]()
14. Sharon A.Aufox. Oligo hydroamnios sequence. Healthline.2012![]()
15. Uhthoff HK,Ogata S. early intrauterine presence of congenital dislocation of knee.J Pediatr Orthop 1994;14:254-257.![]()
16.Laurence M.genu recurvatum congenitum.J Bone Joint Surg Br February 1967 49-B:121-134.![]()
17. Katz MP, Grogono BJ, Soper KC. The etiology & treatment of congenital dislocation of knee. J Bone Joint Surg Br 1967;49-B:112-120.![]()
18. Ko JY, Shih CH, Wenger DR. Congenital dislocation of knee,J Pediatr Orthop.1999;19:252-259.![]()
19. Ooishi T, Sugioka Y, Matsumoto S, Fujii T. Congenital dislocation of knee. Its pathologic features & treatment. Clin Orthop Relat Res 1993;287:187-192.![]()
20.Roach JW, Richards BS. Congenital dislocation of knee. J Pediatr Orthop 1988 ;8:226-229.![]()
21.Söyüncü Y, Mihçi E, Ozcanli H, Ozenci M, Akyildiz F, Aydin AT. Reconstruction of quadriceps tendon with Achilles tendon allograft in older children with congenital dislocation of the knee. Knee Surg Sports Traumatol Arthrosc. 2006 Nov;14(11):1171-5.![]()
22. Patwardhan S, Shyam AK. Use of Percutaneous Needle Tenotomy for Treatment of Congenital Knee dislocation – Technical note. J Orthopaedic Case Reports 2012 July Sep;2(3):25-27.![]()
|
How to Cite This Article: Tiwari M, Sharma N. Unilateral Congenital Knee and Hip Dislocation with Bilateral Clubfoot – A rare Packaging disorder. Journal of Orthopaedic Case Reports 2013 April-June;3(2): 21-24. Available from: https://www.jocr.co.in/wp/2013/04/13/2250-0685-096-fulltext/ |
(Figure 1) | (Figure 2) | (Figure 3) | (Figure 4) | (Figure 5)
[Abstract] [Full Text HTML] [Full Text PDF]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com