[box type=”bio”] What to Learn from this Article?[/box]
Surgical reconstruction of a rare disease where surgical options are reported infrequently.
Case Report | Volume 5 | Issue 3 | JOCR July-Sep 2015 | Page 54-56 | Deshmukh Ranjit, Shyam Ashok K. DOI: 10.13107/jocr.2250-0685.308
Authors: Deshmukh Ranjit[1], Shyam Ashok K[2]
[1] Department of orthopedics, Deenanath Mangeshkar Hospital and Research Centre, Pune. India.
[2] Department of orthopedics, Sancheti Institute for Orthopedics and Rehabilitation, Pune. India.
Address of Correspondence
Dr. Deshmukh Ranjit
Department of orthopedics, Deenanath Mangeshkar Hospital and Research Centre, Erandawane, Pune 411004.
E mail – drranjitdeshmukh@gmail.com
Abstract
Introduction: The Mirror foot is a rare congenital anomaly associated with duplication of the structures of the foot. Verghese et al have classified these feet into three types. Type three is associated with a Dysplastic tibia of which only 5 have been reported. Surgical management has been reported in only two of these five cases which are in the form of amputation.
Case Report: We would like to present the reconstruction of a Mirror foot associated with a dysplastic tibia. Our case which is only the sixth reported case attempts to present a surgical reconstruction to a plantigrade foot. Reconstruction was attempted in this case since the child showed a good quadriceps function at the knee.Reconstruction consisted of excision of the preaxial polydactyly to achieve a more cosmetic appearance to the foot as well as improve the ability to wear foot wear. The dysplastic tibia was osteotomized to correct the varus deformity and achieve a plantigtade foot. This helped the child to ambulate more easily with a shoe raise and a brace to maintain the correction achieved. At a five year follow up the child was walking and running with a shoe raise for a 9 cm limb length discrepancy. There was however recurrence of the deformity due to fibular overgrowth. The child’s parents refused further reconstruction and were satisfied with the present function and appearance of the child.
Conclusion: Reconstruction can therefore be attempted in these limbs associated with good quadriceps function.
Keywords: Mirror Foot; Reconstruction; Dysplastic tibia; Child; Polydactyly.
Introduction
Mirror Foot or duplication of the foot is a rare congenital anomaly which involves duplication of the structures of the foot. They are associated with anomalies of tarsal bones, tibia, fibula and also upper limbs [1]. Some such as the Lauren Sandrow syndrome and Martin Syndrome are associated with nasal abnormalities [2, 3]. Association with tibia abnormality was studied in some detail by Verghese et al [1] who classified these into three types; type I – mirror polydactyly with fibular dimelia, type II- mirror polydactyly with tibia Hypoplasia and type III – mirror polydactyly with trapezoidal tibia [dysplastic tibia]. In their series they described 3 cases of trapezoidal tibia; however the management of these cases was not described. Karchinov [4] has reported a case of trapezoid or dysplastic tibia with accessory foot elements constituting two toes and metatarsals with tarsal bones. They treated the leg with amputation. Recently Kadir et al [5] described another case of mirror foot with dysplastic tibia and syndactly which was again treated with amputation. Thus there are 5 reported cases of dysplastic tibia with mirror foot deformity but none of these cases have been reported with reconstruction and clinical results. We present our case of preaxial polydactyly in a child with mirror foot deformity in the foot associated with a dysplastic tibia. We believe this to be sixth such case and first case to describe reconstruction of the leg with mid-term follow up.
Case report
A one year and four months old male child presented with preaxial polydactyly of the right foot and dysplastic tibia associated with shortening and varus deformity in the right leg and foot. On examination the child was found to have normal mental and physical milestones. Obstetric history of the mother revealed no previous history of abortion. No history of any previous pregnancy. She was a primigravida with the first child being the present one with no siblings. The child was born from a full term pregnancy with caesarean for pregnancy induced hypertension. There was no history of consanguineous marriage in the family. On examination the child had a varus deformity in the right leg with a shortening of 5cm (Figure 1). The right leg as maintained in an attitude of flexion at the knee. Extension was possible actively with grade 3+ power in the right knee. Active flexion was possible up to 100 degrees. Complete range of movements possible at the hip however the ankle was fixed in a rigid equinovarus position. No instability was associated at the knee or ankle. Radiographs relevealed a trapezoid tibia with preaxial polydactyl (Figure 2a, b). At the time of presentation the child was 1 year 3 months but unable to walk. Since the other milestones both physical and mental had progressed well, the child’s inability to walk was attributed to the deformity in the left foot and tibia associated with shortening. Other associated anomalies included a preaxial polydactyly at the right hand with an additional right thumb. The child had an undescended testis on the left side with an absent kidney on the right side as well as no testes on the right side.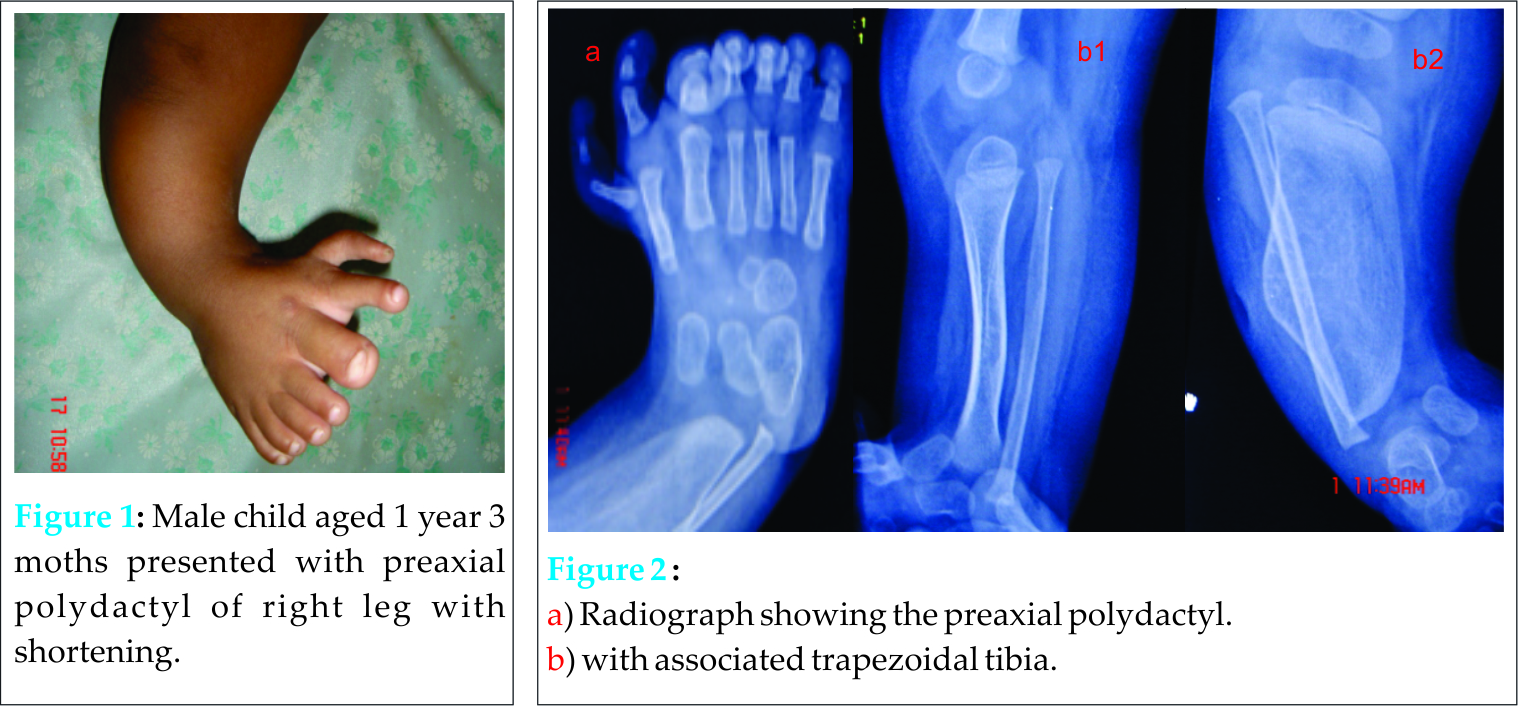
Problem faced by the child at the time of presentation were mainly: shortening, severe varus deformity of the tibia and foot which were not passively correctible, preaxial polydactyly causing inability to wear footwear and also giving the foot a grotesque cosmetic deformity. Aim of surgery at this stage was to provide the child with a plantigrade foot, improve cosmosis and enable child to wear footwear. Surgical procedure: Surgery was performed under general anesthesia with intubation. Surgery involved two stages. The first part was removal of the preaxial polydactyly in the foot. This was performed with a racquet shaped incision in which the toes were removed with the metatarsals. This procedure did not include excision of the duplicated talus. Thus 2 metatarsals and 2 sets of phalanges were excised. The wound was then closed over the medial aspect. The second part of the surgery was correction of the varus deformity in the trapezoid tibia. This varus deformity was corrected by a lateral incision over the leg on the most prominent part of the tibia. This was also marked by a small dimple in the skin. The tibia was dissected out subperiostialy. Two guide wires were used to mark out a lateral closed wedge osteotomy. A fibular osteotomy was done with excision of 1 cm of fibula to allow correction to occur at the osteotomy site. Correction was achieved with a lateral closed wedge osteotomy held in place with a pair of K wires. Closure of the wound was done. Cast maintained for a period of 2 months till the osteotomy site healed completely. K wires removed at 4 weeks of cast change when check x-ray showed good healing at osteotomy site. Post operatively the child was given a supportive clam shell brace extending up to the thigh with a shoe raise. This facilitated the child’s ability to walk and run. It also was expected to maintain the correction achieved. At 2 years follow up there was recurrence of varus deformity (Figure 3 a, b, c). There was overgrowth of the fibula with prominence of the fibular head. However the child was walking and running with help of orthosis and parents refused to undergo corrective surgery. The patient was lost to follow and finally was traced back 5 years after corrective surgery. At this time the tibia vara had increased with ankle inversion and overgrowth of fibula, however ankle dorsiflexion was 90º and plantar flexion was 30º. There was a limb length discrepancy of 9 cm, however the child was able to walk and run with shoe raise (Figure 4 a, b, c). Knee quadriceps was grade 5 with no flexion deformity and full range of knee movements. At present again the child’s parents are not ready for corrective surgeries but promise to keep regular follow up.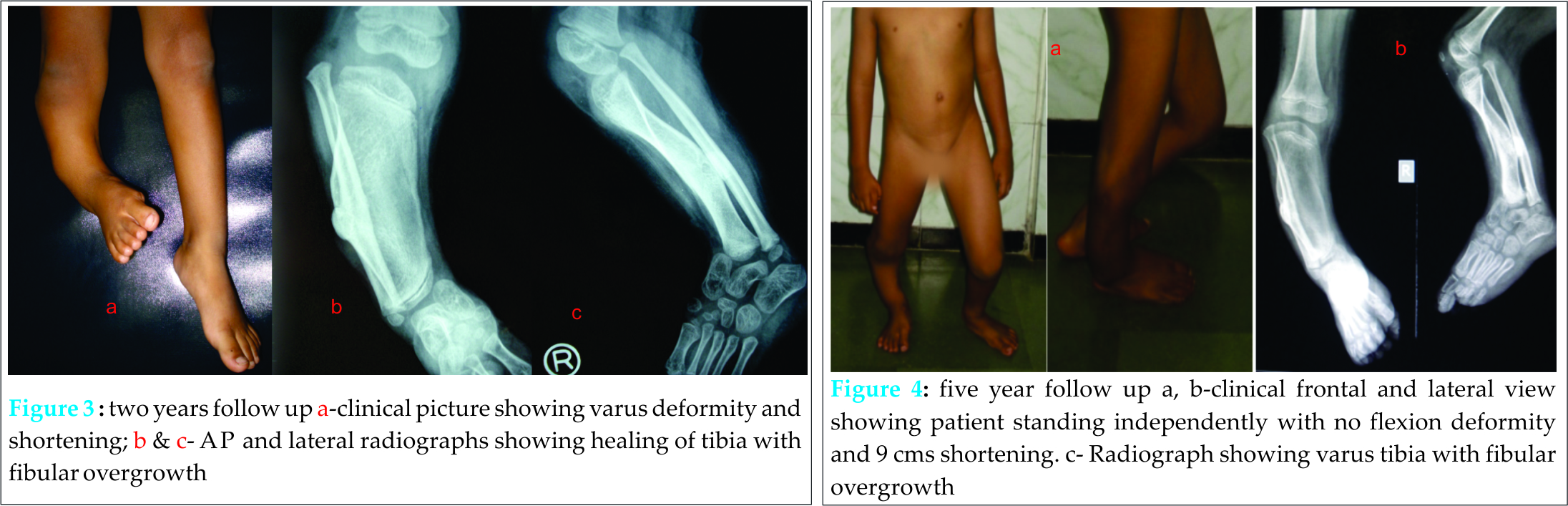
Contemplated surgeries for the future are a repeat osteotomy of the tibia and epiphysiodesis of the fibular head to prevent further growth at the fibula from causing recurrence of the deformity.
Discussion
Mirror feet associated with tibia dysplasia are much rare with only 5 cases reported in literature. No consensus on the management protocol exists and two reports that have described surgical management have opted for amputation. We describe a case of reconstruction of preaxial mirror foot with dysplastic tibia. Mirror foot should strictly involve duplication of all skeletal elements of foot on the tibial side with fibular hemimelia and absent great toe [4]. However all cases of preaxial polydactyly is been loosely termed as mirror foot [1]. Genetic defects like translocation breakpoint at 14q13 have been suggested by Matsumoto et al [6] and Kondoh et al [7]. Recently Klopocki et al [8] implicated deletion of PITX1 of being involved in spectrum of lower limb abnormalities including clubfoot and mirror foot. Autosomal dominant mode of transmission is suggested [2, 3], however not all cases have such associations. In our case too there was no hereditary history. These genetic abnormalities might give rise to spectrum of associated abnormalities with mirror foot most notable amongst which are tibia hypoplasia [4], fibula duplication, renal agenesis [9], imperforate anus, cardiac defects and muscle and tendon abnormalities [10,11]. In the present case renal agenesis and undescended testes with polydactyly of the right hand was seen. Although renal agenesis with mirror foot has been reported by Hamanishi et al [9], to best of our knowledge, no reports of combined presentation with testicular agenesis is reported. Developmentally the renal and the genital system are closely linked [12] and this may explain the unilateral absence of kidney and testis in the present case. Classification of mirror feet by Verghese et al has described the associated tibia abnormalities in mirror foot. According to their classification our case falls into category of pre-axial mirror polydactyly and tibial dysplasia. As described earlier only 5 such cases have been reported and this is the sixth case. Verghese et al made observation of presence of talar duplication in these cases. They also associated talar duplication without other tarsal duplication with good quadriceps function. In the present case too there was talar duplication without any other tarsal duplication and quadriceps power was grade 3. This is an important observation and has bearing on decision for reconstruction as against amputation. Factors that are generally accepted for such decision making are shortening, ankle and foot deformities and quadriceps function [1]. In our case since shortening was not much, ankle and foot deformities were not severe and quadriceps function was good, a decision for surgical reconstruction was taken. We were able to achieve good alignment of the limb and a good cosmetic appearance of the foot. Although the limb varus has recurred, still the patient is mobile and active since last 5 with prosthesis and future surgeries will be contemplated as need arises. On a separate note patient and parents circumstances and socio-economic factors play a great role while delivering the optimal healthcare services especially in country like India.
Conclusion
In conclusion mirror foot with dysplastic tibia generally has good quadriceps function. Reconstruction may be offered to these patients if they present early in life although multiple surgeries might be required in the growth period.
Clinical Message
Reconstruction of Mirror foot with a dysplastic trapezoid tibia is possible in the presence of quadriceps function to give a fairly good function if addressed early.
Reference
1. Verghese R, Shah H, Rebello G. Pre-axial mirror polydactyly associated with tibial deficiency: a study of the patterns of skeletal anomalies of the foot and leg. J Child Orthop. 2007; 1:49–54.
2. Sandrow RE, Sullivan PD, Steel HH. Hereditary ulnar and fibular dimelia with peculiar facies. A case report. J Bone Joint Surg Am. 1970; 52(2):367-70.
3. RA Martin, MC Jones, KL Jones. Mirror hands and feet with a distinct nasal defect, an autosomal dominant condition. Am J Med Gene.t 1993; 46:129–31.
4. Karchinov K. Congenital diplopodia with hypoplasia or aplasia of the tibia. A report of six cases. J Bone Joint Surg Br. 1973; 55:604–11.
5. Kadir KH, Abdul Rashid AH, Das S, Ibrahim S. A rare case of diplopodia and syndactyly: anatomical and surgical considerations. J Foot Ankle Surg. 2011; 50(2):252-6.
6. Matsumoto N, Ohashi H, Kato R, Fujimoto M, Tsujita T, Sasaki T, Nakano M, Miyoshi O, Fukushima Y, Niikawa N. Molecular mapping of a translocation breakpoint at 14q13 in a patient with mirror-image polydactylyy of hands and feet. Hum Genet. 1997; 99(4):450-3.
7. Kondoh S, Sugawara H, Harada N, Matsumoto N, Ohashi H, Sato M, Kantaputra PN, Ogino T, Tomita H, Ohta T, Kishino T, Fukushima Y, Niikawa N, Yoshiura K. A novel gene is disrupted at a 14q13 breakpoint of t (2; 14) in a patient with mirror-image polydactyly of hands and feet. J Hum Genet. 2002; 47(3):136-9.
8. Klopocki E, Kähler C, Foulds N, Shah H, Joseph B, Vogel H, Lüttgen S, Bald R, Besoke R, Held K, Mundlos S, Kurth I. Deletions in PITX1 cause a spectrum of lower-limb malformations including mirror-image polydactyly. Eur J Hum Gene.t 2012; 20(6):705-8.
9. Hamanishi C, Ueba Y, Iwashita Y, Yamamuro T. Diplopodia with reversed foot. Normal gait after operation at 8 years of age. Acta Orthop Scand. 1985; 56:439–41.
10. Jones D, Barnes J, Lloyd-Roberts GC. Congenital aplasia and dysplasia of the tibia 625 with intact fibula. Classification and management. J Bone Joint Surg Br 1978;60:31– 39.
11. Rivera RE, Hootnick DR, Gingold AR, Levinsohn EM, Kruger LM, Packard DS Jr. Anatomy of a duplicated human foot from a limb with fibular dimelia. Teratology. 1999; 60:272–82.
12. Kumar KH, Rao BS, Shiradhonkar S, Jha R, Narayan G, Modi KD. The right sided syndrome, congenital absence of kidney and testis. Saudi J Kidney Dis Transpl. 2011; 22:315-8.
| How to Cite This Article: Ranjit D, Shyam AK.Reconstruction of Mirror Foot with Dysplastic Tibia. Journal of Orthopaedic Case Reports 2015 July – Sep;5(3): 54-56 . Available from: https://www.jocr.co.in/wp/2015/07/10/2250-0685-308-fulltext/ |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com





