[box type=”bio”] What to Learn from this Article?[/box]
Heel pad avulsion injuries with exposed and ruptured tendoachilles should be managed within golden period and with minimal implant.
Case Report | Volume 6 | Issue 4 | JOCR September-October 2016 | Page: 44-48 | Shameem Ahmed, Syed Ifthekar, R Pathan Rameez Ahmed Khan, Rahul Ranjan. DOI: 10.13107/jocr.2250-0685.564
Authors: Shameem Ahmed[1], Syed Ifthekar[1], R Pathan Rameez Ahmed Khan[1], Rahul Ranjan[2]
[1]Department of Orthopaedics, Hindu Rao Hospital, New Delhi, India.
[2]Department of Orthopaedics, Lady Hardinge Medical College, New Delhi, India.
Address of Correspondence
Dr. Syed Ifthekar,
Department of Orthopaedics, Hindu Rao Hospital, New Delhi, India.
E‑mail: dr.ifthekar@gmail.com
Abstract
Introduction: The management of heel pad avulsion injuries has been challenging because of the precarious blood supply. The difficulties get compounded when it is associated with tendoachilles rupture and calcaneal fracture. Here is a description of a case with the above features managed with a unique technique.
Case presentation: A 63-year-old woman presented to casualty with injury to right ankle after a road traffic accident. On clinical and radiological examination there was avulsion of heel pad with calcaneal tuberosity fracture and tendoachilles rupture. It was managed with debridement of the wound, repair of tendo achilles and fixation of calcaneal tuberosity and heel pad. The functional outcome was assessed in terms of ability of the patient to return to painless barefoot weight bearing.
The uniqueness of this method is the combined use of suture material(Ethibond) and stainless steel[Cannulated Cancellous Screws(CCS)] ,by tying the Ethibond from Tendo Achilles to the head of CCS rather than bone. When the CC Screws were tightened , two things were achieved , one being the reduction of the fracture and the second to bring a good apposition of Tendo Achilles with the Calcaneum. As this method worked on tension band principle and Ethibond was used instead of stainless steel wire,if no objectiions, this technique can be called as “soft tension band technique” .
Conclusion: This case report illustrates a method of preserving heel pad when it is viable along with definitive treatment of associated soft tissue and bony injuries by a simple technique.
This method has described the fixation of open fracture of calcaneal tuberosity with Tendo Achilles rupture with heel pad avulsion in one sitting with excellent clinical results.
Key words: Heel pad avulsion, calcaneal tuberosity fracture, tendo-achilles rupture.
Introduction
The heel pad is a specialized soft-tissue structure for the purpose of weight bearing.[1] Because of the uniqueness and complex nature of the heel pad structure , the heel pad avulsions throw a constant challenge to the surgeons.[1] The evolution of the heel pad in the form of tight honey comb arrangement of elastic fibrous septa enclosing tightly packed fat cells is to accept very high loading stresses. In the event of heel pad injury its virtually impossible to replace it with other structures of the body.[1].Heel pad avulsion combined with a calcaneal tuberosity fracture and tendo-achilles rupture, is all the more difficult to manage as the soft tissue healing is in question[1]. Heel pad avulsion is usually the result of high-energy trauma and can have severe consequences regardless of the status of the neurovascular bundle or skeletal integrity. The dense fibrous septae normally hold the fat pad to the undersurface of the calcaneus in a honeycomb pattern and resist migration[2]. Partial or complete degloving of the heel pad can occur, often as a result of road accidents. Complete or subtotal avulsions of the heel pad, or those with extensive neurovascular damage, will need replantation with use of microvascular surgical techniques or reconstruction with soft-tissue flaps[3]. In situations of partial avulsion of heel pad, when the sensations are intact and the heel pad is viable, it may be possible to debride and reattach the flap. One of the goals in the management of severe open injuries of foot is to obtain adequate soft tissue coverage[4]. Simple suturing to reattach the heel edges is not secure enough, or it can lead to increased wound pressure, resulting in wound breakdown, infection, and flap necrosis. We are presenting a case of partial heel pad avulsion with open calcaneal tuberosity fracture with tendo-achilles rupture. Calcaneal tuberosity fracture was fixed with partially threaded cannulated cancellous screws and the torn end of tendo-achilles was tied to the heads of cannulated cancellous screws with Ethibond suture. Heel pad was successfully re-attached to the calcaneus with the help of Schanz pin and primary suturing of the wound in layers followed by above-knee cast application. Patient got excellent functional recovery after 12 weeks.
Case Presentation:
A 63-year-old woman presented with injury to right ankle after a road traffic accident. Following initial resuscitation and stabilization of the patient, assessment for other injuries was done. Physical examination showed right heel pad avulsion as shown in [Fig.1]. The extent of the wound contamination, soft-tissue loss, skeletal injury, and sensation and viability of the avulsed flap was done. Wound was contaminated and there was no skin loss. Radiographs were obtained to identify the skeletal injury which showed fracture of right calcaneal tuberosity as shown in the [Fig.2]. Finally, the compound fracture was classified according to Gustilo-Anderson classification as grade IIIA. Broad spectrum antibiotics with gram positive, gram negative and anaerobic coverage were started intravenously. The patient was counseled about the potential complications of re-implantation of heel pad and the possible necessity for additional surgical procedures. Under regional anesthesia, the wound was debrided and thoroughly lavaged. Fixation of the calcaneal tuberosity was done temporarily with kirschner wires, followed by two 4.5 mm cannulated cancellous screws. But final tightening of the screws was not done. Tendo-achilles was sutured using Ethibond no 5 suture with Krackow`s technique and the two ends were tied to the head of the screws over washers. Once properly tied, the final tightening of screws was done. Thus giving a secure fixation to calcaneal tuberosity and tendo-achilles [Fig. 3]. The heel pad was later fixed using Schanz pin in the centre and primary suturing of the wound was done [Fig. 4]. This provides a stable anchorage for the heel pad over the calcaneus.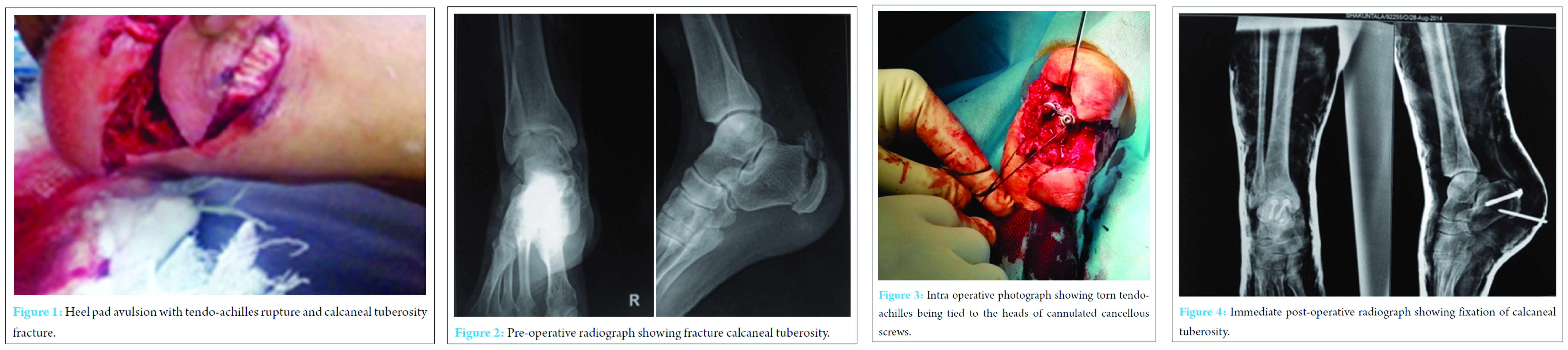 The soft tissue was sutured in two layers, subcutaneous tissue using vicryl and skin using silk. This method makes the avulsed heel pad immobile, thus jamming any movement in sagittal and coronal plane. Over this an above-knee cast was applied keeping the knee in 30 degrees of flexion and ankle in 30 degrees of equinus. After the cast dried, a window was made in the heel for wound inspection and dressing.
The soft tissue was sutured in two layers, subcutaneous tissue using vicryl and skin using silk. This method makes the avulsed heel pad immobile, thus jamming any movement in sagittal and coronal plane. Over this an above-knee cast was applied keeping the knee in 30 degrees of flexion and ankle in 30 degrees of equinus. After the cast dried, a window was made in the heel for wound inspection and dressing.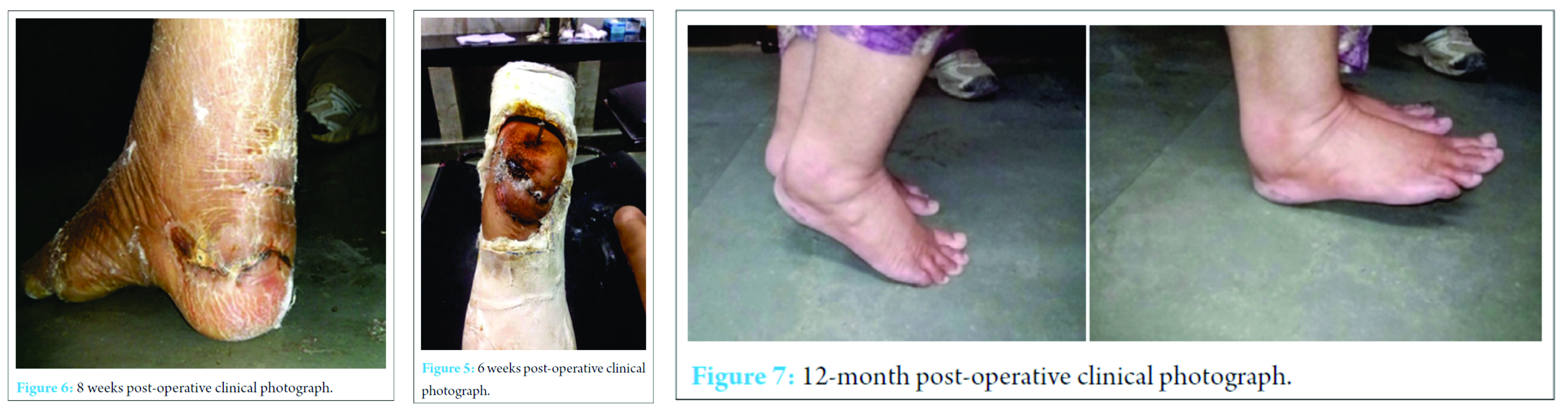
After two days, the patient was shifted to oral antibiotics. Broad spectrum antibiotics covering both gram positive and gram negative organisms were administered. [Tab Amoxicillin+clavulanic acid 625mg TDS]. Window was created on second day, through which wound inspection and required dressing was done. Wound and flap healing was assessed weekly [Fig 5]. Toe-touch down weight bearing was allowed after 2 weeks. Schanz pin was removed after 6 weeks. And below-knee cast was applied keeping the foot plantigrade. Full weight bearing was allowed in a gradual manner, over the next 4 weeks.[fig 6]. Over a period of 12 weeks, patient achieved good functional range of movements and the patient was followed up for 1 year and her fracture was united.[Figs.7, 8 & 9]. We have included the X-ray which is more than one year old. The implant was not removed as there were no complaints related to implant. It is also clinically evident that the fracture is united as the patient is walking full weight bearing without support and standing on heel and toes independently.
We have included the X-ray which is more than one year old. The implant was not removed as there were no complaints related to implant. It is also clinically evident that the fracture is united as the patient is walking full weight bearing without support and standing on heel and toes independently.
Discussion:
Heel pad avulsions with associated bony fractures usually result from road traffic accidents [5]. The separation of the heel flap occurs in a posterior to anterior direction and can even separate and tear the skin from the deep fascia due to the torsional and compressive forces at different levels of sub cutaneous tissue and fascia [5]. When heel pad viability is evident, sensation is present, and detachment is incomplete, it is reasonable to consider debridement and reattachment [6]. Frequently the injury to the heel pad results in a compromise of the blood supply to the region, namely the medial calcaneal branch of the posterior tibial artery [3]. Because of the unique load-bearing function of the heel pad and its complex architecture, every attempt should be made to retain the original tissues in cases of partial de-gloving of the heel with intact vascularity [3, 5, 7]. The application of free flaps to this area has been reported, but the amount of pressure and shear that this transferred and insensate tissue must endure during stance or ambulation is often too overwhelming to allow a good functional result. If a free flap is undertaken, a custom stress-relieving shoe insert is imperative to decrease the almost certain pressure sore at the most plantar aspect of the tuberosity due to altered physiological pressure distribution during gait. The avulsed fracture patterns are as follows [8]; Type I is a ‘simple extra-articular avulsion’ fracture, Type II is the ‘beak’ fracture, Type III is an infrabursal avulsion fracture from the middle third of the posterior tuberosity, and finally in Type IV there is the ‘beak’, but a small triangular fragment is separated from the upper border of the tuberosity. Out of which type I is the most common. All fibers within the achilles tendon are involved in both type I and II fractures. However, only the superficial fibers are involved in type III fractures, whereas the deep fibers are involved in type IV fractures [8]. Our technique comprised of starting the treatment within six hours, the so called “Golden period”. Thorough debridement and copious lavage with normal saline ensures lessening of chances of infection. It is followed by stable anchorage of the heel flap to calcaneus using a Schanz pin and primary suturing of the soft tissue. Above knee cast keeps the limb in position so that the stresses are minimized over the detached flap and it keeps the gastrocnemius pull to minimum. Utmost care is taken to minimize the risk of infection which may lift the flap from bone and impedes the healing and prevent buildup of fluid pressure under the flap. The blood supply to the heel arises posteriorly from the medial calcaneal branch of the posterior tibial artery along with a minor contribution from the lateral calcaneal branch of the peroneal artery, and the anterior part is supplied primarily by the lateral plantar artery [9]. However, there are rich vascular anastomoses among these vessels at a subdermal and periosteal level in the heel. The vessels travel within the fibrous septa that anchor the skin of the heel to the periosteum of the Calcaneus [2].
Conclusion:
Although it is very difficult to conclude based on a single case, but it seems that simple and stable reattachment of the flap to the bone is sufficient enough for the survival of the heel flap. The use of Schanz pin and primary suturing provides a simple and effective technique to salvage partial avulsion of the heel pad without requiring a complicated microsurgical procedure. This technique can be replicated without having sophisticated equipment facilities.
Clinical Message
The management of heel pad avulsions when associated with bony and soft tissue injuries( as described above) are technically demanding. This case report can be an example of excellent functional outcome in the complex injury when managed by appropriate technique in the golden period( within 6 hours after injury).
References
1. Mohammed R, Metikala S. Anchorage of Partial Avulsion of the Heel Pad with Use of Multiple Kirschner Wires. JBJS Case Connector. 2012 May 9;2(2):e20.
2. Cichowitz A, Pan WR, Ashton M. The heel: anatomy, blood supply, and the pathophysiology of pressure ulcers. Annals of plastic surgery. 2009 Apr 1;62(4):423-9.
3. Graf P, Biemer E. [Degloving injuries of the soft tissues of the heel. An indication for microvascular revascularization!]. Der Chirurg; Zeitschrift fur alle Gebiete der operativen Medizen. 1994 Jul;65(7):642-5.
4. Basile A, Stopponi M, Loreti A, de Simeonibus AU. Heel coverage using a distally based sural artery fasciocutaneous cross-leg flap: report of a small series. The Journal of Foot and Ankle Surgery. 2008 Apr 30;47(2):112-7.
5. Jeng SF, Wei FC. Classification and reconstructive options in foot plantar skin avulsion injuries. Plastic and reconstructive surgery. 1997 May 1;99(6):1695-703.
6. Lim H, Han DH, Lee IJ, Park MC. A simple strategy in avulsion flap injury: prediction of flap viability using wood’s lamp illumination and resurfacing with a full-thickness skin graft. Archives of plastic surgery. 2014 Mar 1;41(2):126-32.
7. Jeng SF, Hsieh CH, Lin TS, Kuo YR, Wei FC. Classification and reconstruction options in foot plantar skin avulsion injuries: follow-up. Plastic and reconstructive surgery. 2003 Jul 1;112(1):220-1.
8. Lee SM, Huh SW, Chung JW, Kim DW, Kim YJ, Rhee SK. Avulsion fracture of the calcaneal tuberosity: classification and its characteristics. Clinics in orthopedic surgery. 2012 Jun 1;4(2):134-8.
9. Andros G. Bypasses to ankle and foot. The Surgical Clinics of North America. Philadelphia: PA:W.B. Saunders, Aug 1995;75(4):717
| How to Cite This Article: Shameem Ahmed, Syed Ifthekar, R Pathan Rameez Ahmed Khan, Rahul Ranjan. Partial Heel Pad Avulsion with Open Calcaneal Tuberosity Fracture with Tendo-achilles Rupture – A Case Report. Journal of Orthopaedic Case Reports 2016 Sep-Oct;6(4): 44-48. Available from: https://www.jocr.co.in/wp/2016/10/10/2250-0685-564-fulltext/ |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com





