[box type=”bio”] What to Learn from this Article?[/box]
Morel-Lavellee Syndrome is an extremely rare complication of anterior hip dislocation and hence such patients should be closely followed up as it manifests as a late complication.
Case Report | Volume 6 | Issue 4 | JOCR September-October 2016 | Page 73-76 | Supreeth Nekkanti, C Vijay, Sujana Theja, R Ravi Shankar, Anubhav Verma DOI: 10.13107/jocr.2250-0685.578
Authors: Supreeth Nekkanti[1], C Vijay[1], Sujana Theja[1], R Ravi Shankar[1], Anubhav Verma[1]
[1]Department of Orthopaedics, JSS Hospital, Mysore, Karnataka, India.
Address of Correspondence
Dr. Supreeth Nekkanti, No. 160, 11th Cross, 5th Main, 1st Stage, NGEF Layout, Nrupatunganagar, Nagarbhavi, Bengaluru – 560 072, Karnataka, India.
Phone: +91-9742551646.
E-mail: drsupreethn@gmail.com
Abstract
Introduction: Hip dislocations are serious injuries as hip joint is an extremely stable joint. It requires significant amount of force to produce such an injury. Anterior dislocations are uncommon. Potential complications of anterior hip dislocations are neurovascular injury to femoral vessels or acetabular fractures.
Case presentation: We report a rare late complication of Morel Lavallee syndrome occurring three weeks after an anterior dislocation of the hip in a 43 year old male. The patient presented to us with history
Conclusion: Morel Lavalle syndrome is a rare complication. However if diagnosed early, can be successfully treated with minimal burden to the patient. The authors recommend surgeons to have a high index of suspicion for this syndrome and a stringent follow-up examination of the patient.
Keywords: anterior hip dislocation, Morel Lavalle syndrome, complication.
Introduction:
Anterior dislocations of the hip joint are unusual injuries. They are relatively rare and constitute 10-15% of all dislocations.[1, 2] The strong anterior capsule and ligament of Bigelow make these injuries rare. Anterior dislocations usually lead to fractures of the anterior acetabular wall or femoral head fractures or neurovascular injuries of the femoral vessels. We report a rare case of Morel Lavallee lesion complicating an anterior dislocation of the hip.
Case Presentation:
A 43 year old presented to the emergency department following a history of road traffic accident. He was apparently standing on the road when a four wheeler hit him from behind. The patient felt a snap following which he was unable to stand up on his affected limb. Clinical examination revealed that the limb was in external rotation and flexion. A hard mass was palpable on the anterior aspect of the groin. X-ray revealed an anterior dislocation of the hip. (Fig.1)
A closed reduction under general anesthesia was performed within two hours of the accident. The patient was laid down in a supineposition; the pelvis was fixed by an orthopedic surgeon while another orthopedic surgeon performed a continuous axial extension of the right leg till the femoral head was located distal the acetabulum, which was checked by fluoroscopy. At that moment the hip was flexed and internal rotated. This procedure was followed by a snap sound. The reduction of the hip joint was confirmed with C-arm. (Fig.2)
The limb was immobilized in a Thomas splint. The patient was kept under observation for 48 hours and discharged. The patient presented to us after three weeks with severe pain over the antero-medial aspect of thigh. There was a tense cystic swelling with ecchymosis over the medial side of thigh. (Figure.3) Ultrasonography showed multiple hypo echoic masses floating in a cystic cavity in the thigh. Aspiration using an 18 gauge needle yielded around 120 ml of blood mixed with clots. (Figure.4, 5) After aspiration, a compressive bandage was applied and antibiotics were given. The patient improved and was asymptomatic. The patient was taught pelvic bridging exercises to avoid bed sores, isometric adductor, gluteal and hamstring strengthening exercises initially. The patient was also encouraged ankle range of movement exercises initially. He was then made to perform quadriceps strengthening and range of movement exercises of the knee joint. after 4 weeks. At the end of six weeks, the patient was made to weight bear. The patient continued all his normal activities by the end of third month. The patient achieved full range of movements by the end of six months.
Ultrasonography showed multiple hypo echoic masses floating in a cystic cavity in the thigh. Aspiration using an 18 gauge needle yielded around 120 ml of blood mixed with clots. (Figure.4, 5) After aspiration, a compressive bandage was applied and antibiotics were given. The patient improved and was asymptomatic. The patient was taught pelvic bridging exercises to avoid bed sores, isometric adductor, gluteal and hamstring strengthening exercises initially. The patient was also encouraged ankle range of movement exercises initially. He was then made to perform quadriceps strengthening and range of movement exercises of the knee joint. after 4 weeks. At the end of six weeks, the patient was made to weight bear. The patient continued all his normal activities by the end of third month. The patient achieved full range of movements by the end of six months.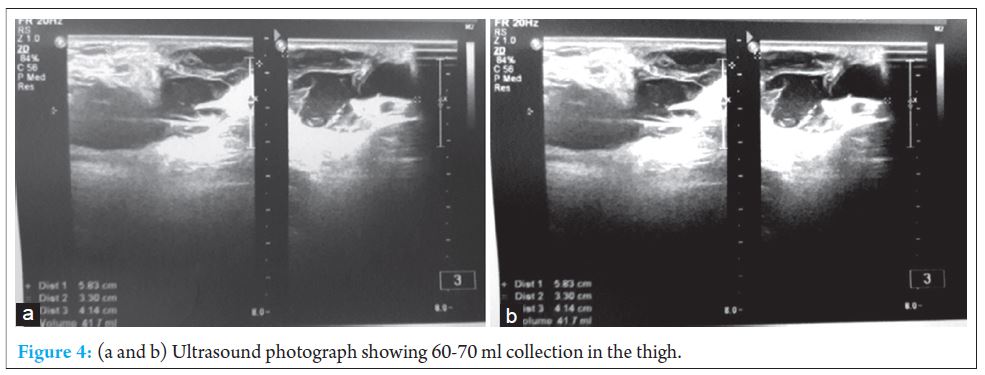
Discussion:
Anterior dislocations are extremely rare injuries. They constitute 10-15% of all dislocations [1, 2]. About 75% of anterior dislocations occur in males [1, 2]. Almost 35% of patients who suffer from anterior dislocations are in their third decade of life [1, 2]. On the contrary, our patient was 43 years old and in the fourth decade of life. The ratio of anterior to posterior dislocations variesfrom 1:10 to 1:19. [1, 3, 4] The rarity of these injuries is due to the strong anterior capsule and the ligament of Bigelow. Anterior dislocations are of two types, the superior iliac or pubic type and the inferior obturator type. In our patient, it was of theobturator variety of anterior dislocation.
The mechanism of injury in anterior dislocation of the hip is usually one of the three types. One is due to dashboard injury when the thigh is abducted. The second likely mode of injury is fall from a height. Lastly blow to the back when the patient is squatting seems to be a relatively more common mode of injury. [1, 3, 4] Our patient was hit from behind by a four wheeler. We suspect that the limb probably was forced into external rotation, abduction and hyperextension at the hip joint at the time of impact.
The sequence of events that occur following trauma are the neck of the femur or the greater trochanter impinges on the rim of the acetabulum, which in turn levers out the femoral head out of the acetabulum socket. The femoral head usually pushes itself out through a tear in the anterior capsule. [1, 3]
The hip joint ideally should be reduced within six hours of fall. The incidence of avascular necrosis keeps increasing as time passes. The incidence of avascular necrosis of the femoral head in an unreduced hip after six hours varies from 0-22%. [1, 3] Aware of these statistics, a successful attempt was made to reduce the hip joint within two hours of trauma under general anesthesia.
The authors don’t recommend reduction of the hip joint under the effect of muscle relaxants, as more often than not the relaxation is not adequate to successfully reduce the joint. Moreover excessive manipulation is required which may lead to trauma of the retinacular or circumflex vessels. This in turn leads to avascular necrosis. The recommendations are to reduce the hip joint under general anesthesia.
The usual complications after an anterior dislocation of the hip include neurovascular injury of the femoral vessels [1, 5], femoral head fracture [1, 6] and acetabulum fractures [1]. Our patient did not have any of the above mentioned complications. Our patient developed Morel Lavallesyndrome three weeks after his accident. Morel-Lavelle lesion refers to a cystic lesion secondary
toblunt injury and especially in deglovinginjuries. The mechanism behind these injuries is when a tangential shearing force acts on the relatively mobile tissue, it gets torn away from the underlying firm muscle fascia.[7] This creates a dead space between the two tissue planes which is filled with blood and/ or lymph from the disrupted perforating vessels or capillaries[7, 8]
Morel-Lavelle lesions are more often encountered over the trochanteric region or the proximal thigh; however it has been reported in other locations such as the lower lumbar region or the calf. Also they have been associated with pelvicor acetabular fractures [7, 9]. In our patient, during the course of the dislocation of the femoral head anteriorly, it induces a shearing force on the subcutaneous tissues which get dragged along with it. This results in the dead space as explained above.
The key steps of the process have been identified; after the initial formation of the potential blood filled space, there is evolution of this haematoma with absorption of the blood, which is replaced by serosanguineous fluid [7, 10]. The last step in this chain ofevents is the formation of a peripheral fibrous capsule secondaryto an anti-inflammatory reaction.The entrapment of
fluid within the cystmay maintain a degree of chronic inflammationthat could cause the gradual enlargement of the lesionover a long period of time.
In our patient, we aspirated hematoma clots from the site of injury i.e. along the antero-medial aspect of thigh. The diagnosis was made clinically by palpating an extremely tender area on the antero-medial aspect of thigh. Diagnosis was confirmed with ultrasonography.
Most authors however agree that the imagingmodality of choice is MRI. However the findings of anMRI may vary significantly, based on the chronicity andinternal contents of the lesion. Despite the rarity of thislesion, MRI imaging has been used for the only so faravailable classification system [7, 11].
The available treatment modalities depend on the timing of identification of aMorel-Lavellelesion. If it is detected during the acute phase, percutaneousdrainage and compression may be sufficient. However in later stages, surgical aspiration or excision of the fibrous capsule may be warranted.[7, 12, 13] After surgery, it would be necessary to place suction drain to drain out any remnant fluid from the cyst.The differential diagnosisof a Morel-Lavelle lesion includes posttraumatic fat necrosis,coagulopathy-related hematoma and posttraumatic earlystage myositis ossificans [7, 12].
Conclusion:
In conclusion, we presented a rare case of a Morel-Lavelle lesion following anterior dislocation of the hip. Although rare, this particular entity should be looked for as it may present as a late complication such as our case.MRI is the best imaging modality for characterizingMorel-Lavelle lesions. Aspiration, compressive bandaging and antibiotics are sufficient if diagnosed early. The results are usually good. However, surgical excision is thepreferable treatment modality when the lesion is advanced.
Clinical message:
Anterior hip dislocations are rare. Atypical complications like Morel Lavalle syndrome after hip dislocations present an unusual challenge during the treatment of the patient. Early clinical diagnosis of this condition is critical. Aid of MRI must be sought in case of doubt. Most cases respond well with almost immediate relief if diagnosed early and managed promptly. This reduces significant physical and financial burden to the patient. A diagnosis of Morel Lavalle syndrome should be thought of as a potential late complication.
References:
1. Akhil A. Tawari*, Vishal D. Bahuva, Arvind B. Goregaonkar et al. A rare case of open anterior hip dislocation. JSCR 2013; 1-4
2. Whitehouse GH. Radiological aspects of posterior dislocation of the hip.ClinRadiol 978;29:431–41.
3. Sahin V, Karakas¸ ES, Aksu S, Atlihan D, Turk CY, Halici M. Traumaticdislocation and fracture-dislocation of the hip: a long-term follow-upstudy. J Trauma 2003;54:520–9.
4. Amihood S. Anterior dislocation of the hip. Injury 1975;7:107–10.
5. Schwartz DL, Haller JA, Jr. Open anterior hip dislocation with femoralvessel transection in a child. J Trauma 1974;14:1054–9.
6. Jacob JR, Rao JP, Ciccarelli C. Traumatic dislocation and fracturedislocation of the hip. A long-term follow-up study. ClinOrthopRelatRes 1987;214:249–63.
7. ElissaiosKontis, AntoniosVezakis, VasilikiPsychogiou, PanagiotisKalogeropoulos et al. Morel-Lavallée Lesion: Report of a Case of Unknown Mechanism, “Case Reports in Surgery “Volume 2015, 1-3.
8. Bonilla-Yoon, S. Masih, D. B. Patel, White EA, Levine BD, Chow K, et al., “TheMorel-Lavall´eelesion: pathophysiology, clinical presentation, imaging features,and treatment options,” Emergency Radiology, vol. 21, no. 1, pp.35–43, 2014.
9. D. J. Hak, S. A. Olson, and J.M.Matta, “Diagnosis andmanagementof closed internal degloving injuries associatedwith pelvic and acetabular fractures: the Morel-Lavelle lesion,” Journal of Trauma, vol. 42, no. 6, pp. 1046–1051, 1997\
10. H. Li, F. Zhang, and G. Lei, “Morel-Lavelle lesion,” ChineseMedical Journal, vol. 127, no. 7, pp. 1351–1356, 2014.
11. J. M. Mellado and J. T. Bencardino, “Morel-Lavellelesion:review with emphasis on MR imaging,” Magnetic ResonanceImaging Clinics of North America, vol. 13, no. 4, pp. 775–782,2005.
12. A. V. Nair, P. K. Nazar, R. Sekhar, P. V. Ramachandran, and S.Moorthy, “Morel-Lavelle lesion: a closed degloving injury thatrequires real attention,” Indian Journal of Radiology and Imaging,vol. 24, no. 3, pp. 288–290, 2014.
13. T. P. Nickerson, M. D. Zielinski, D. H. Jenkins, and H.J. Schiller, “The Mayo clinic experience with morel-lavall´eelesions: establishment of a practice management guideline,”Journal of Trauma and Acute Care Surgery, vol. 76, no. 2, pp.493–497, 2014.
14. Nekkanti S, Vijay C, Theja C, Shankar RR, Verma A. A Rare Case of Morel-Lavallee Syndrome Complicating an Anterior Dislocation of Hip Joint. Journal of Orthopaedic Case Reports 2016 Sep-Oct;6(4):1-4.
| How to Cite This Article: Nekkanti S, Vijay C, Theja C, Shankar RR, Verma A. A Rare Case of Morel-Lavallee Syndrome Complicating an Anterior Dislocation of Hip Joint. Journal of Orthopaedic Case Reports 2016 Sep-Oct;6(4): 73-76. Available from: |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com





