[box type=”bio”] What to Learn from this Article?[/box]
Mycetoma should be considered as a diagnosis, especially in tropical countries with barefoot walkers even in the absence of classical signs.
Case Report | Volume 7 | Issue 1 | JOCR January – February 2017 | Page 12-15 | Amit Grover, Prashanth Nagaraj, Vinay M Joseph, Daksh Gadi. DOI: 10.13107/jocr.2250-0685.666
Authors: Amit Grover[1], Prashanth Nagaraj[1], Vinay M Joseph[1], Daksh Gadi[1]
[1]Department of Orthopaedics, MS Ramaiah Medical College, Bengaluru, Karnataka, India.
Address of Correspondence
Dr. Amit Grover,
Department of Orthopaedics, Room No 10, Neelgiri Block, MS Ramaiah Medical College, MSR Nagar,
BEL Road, Bengaluru – 560 064, Karnataka, India.
E-mail: amitgrover88@gmail.com
Abstract
Introduction: Mycetoma is a chronic granulomatous infection. It is caused by actinomycetes or fungi. It is common in tropical countries and males. Predisposing conditions include malnutrition, poor hygiene, history of trauma, wounds on barefeet, and systemic infections. Eumycotic mycetoma commonly involves lower extremities whereas actinomycosis affects the cervicofacial, thoracic, and abdominal regions. Mycetoma presents with a chronic indurated ulcerated plague with swelling and yellowish discharge of sulfur granules.
Case Report: We report a rare case of a 40-year-old male with a left foot plantar swelling of 4 months duration with no discharging sinuses, fever, and pain. There was no history of trauma or barefoot walking. Clinical and magnetic resonance imaging (MRI) findings were suggestive of a soft-tissue malignancy. The mass was excised and sent for histopathology. Histopathology reported it as a mycetoma. Complete resolution was seen after 3 months of antifungal treatment and excision of the mass. This was unusual since there were no discharging sinuses, nodules, and even MRI reported as a fibrous or muscular mass. The diagnosis was made only after a histopathological examination.
Conclusion: Mycetoma is a rare infection caused by fungal or bacterial organisms. In the absence of ulceration and sinuses, diagnosis can be difficult. Diagnosis requires a high degree of suspicion in the absence of such clinical signs. Definitive diagnosis should be made on histopathological examination. Once diagnosis is made, surgical excision with appropriate antifungals can result in complete cure without recurrence.
Keywords: Mycetoma, foot, unusual presentation, case report.
Introduction
Mycetoma is a chronic granulomatous infection. It is caused by actinomycetes or fungi. There is a granulomatous inflammatory reaction in the dermis which extends into the bone [1, 2]. There is a formation of sinus and fistulas with discharge of sulfur granules [3]. Mycetoma is common in tropical countries [4, 5]. It is more common in males [6]. Predisposing conditions include malnutrition, poor hygiene, history of trauma, wounds on barefeet, and systemic infections [7]. It commonly affects barefoot walkers in third and fourth decades of life. Eumycotic mycetoma commonly involves lower extremities whereas actinomycosis affects the cervicofacial, thoracic, and abdominal regions [8, 9]. Mycetoma presents with a chronic indurated ulcerated plague with swelling and yellowish discharge [9]. Draining sinuses are characteristic of mycetoma. Differential diagnosis includes botryomycosis and other fungal infections, syphilis, yaws, elephantiasis, and malignancy [1]. We report a rare case of a 40-year-old male with a left foot plantar swelling of 4 months duration with no discharging sinuses, fever, and pain. There was no history of trauma or barefoot walking. Clinical and magnetic resonance imaging (MRI) findings were suggestive of a soft-tissue malignancy. The mass was excised and sent for histopathology. Histopathology reported it as a mycetoma. This was unusual since there were no discharging sinuses, nodules, and even MRI reported as a fibrous or muscular mass.
Case Report
A 40-year-old male presented to us with a history of a left foot plantar swelling for 4 months (Fig. 1). The swelling was gradually progressive, firm in consistency, 7.5×8 cm, and non-tender. There was no lymphadenopathy. There was no history of fever, discharging sinuses, or pain. There was no history of trauma or barefoot walking.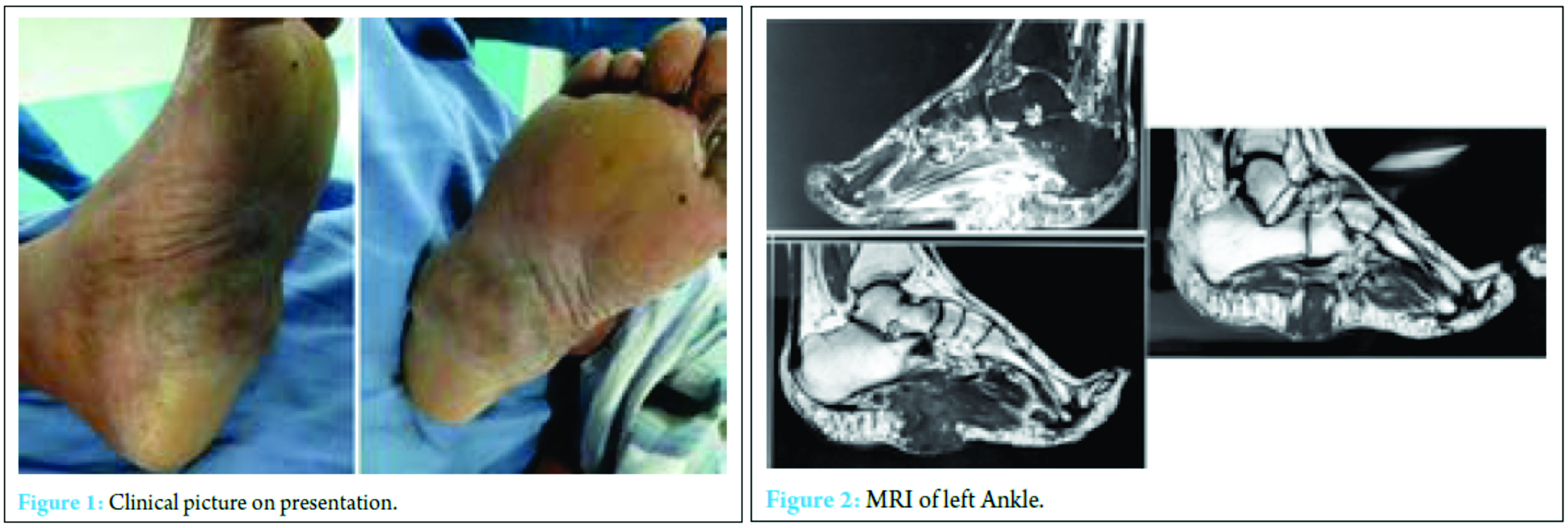
Routine blood investigations including total counts, differential counts, ESR, and alkaline phosphatase were within normal limits. MRI showed a fibrous or muscular origin mass (Fig. 2 and 3). Working diagnosis of a soft-tissue malignancy was made. The patient was taken up for an excision biopsy, and tissue was sent for histopathological examination (Fig. 4). Histopathological report surprisingly revealed a mycetoma of the left foot (Fig. 5). The patient was started on antifungal treatment for 3 months. They were given in cycles comprising amikacin 15 mg/kg twice daily for 3 weeks and cotrimoxazole in a dose of 1.5 mg/kg twice daily for 5 weeks; the cycles were repeated till 3 months. At 3-month follow-up, there was a complete resolution of the mass with no recurrence (Fig. 6).
This is a unique case as it did not present like a mycetoma which is characterized by ulceration, nodules, and discharging sinuses. There were no predisposing factors such as barefoot walking, malnutrition, or history of trauma. MRI was also suggestive of a fibrous or muscular mass. The diagnosis was made only after a histopathological examination.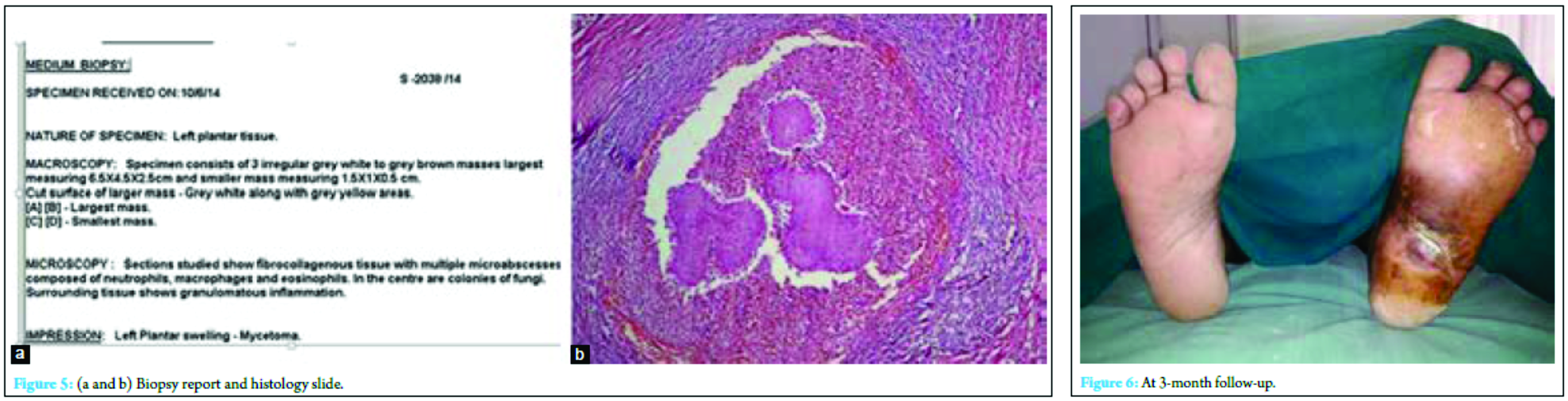
Discussion
Diagnosis of mycetoma is usually made clinically. The triad of indurated edema, multiple draining sinuses with grain-filled purulence and location on the foot makes the diagnosis easy [10]. Differential diagnosis would include blastomycosis, botryomycosis, chromoblastomycosis, cutaneous squamous cell carcinoma, verrucous carcinoma, malignancy, and osteomyelitis. However, in the absence of these features and history, the diagnosis can be confusing. X-rays can provide information regarding osseous involvement. MRI can provide information about soft-tissue involvement. Definitive diagnosis should be made on histopathological examination. Talwar et al. [11] conducted a study on 60 cases of suspected mycetoma. Of these cases, 20 were confirmed by histopathological examination. Dogra et al. [12] reported a case of actinomycosis in a young female. The diagnosis was confirmed by histopathology. Combined surgical and medical management is the mainstay of management [13, 14]. Medical management includes a combination of streptomycin and dapsone. Dapsone can be replaced by cotrimoxazole if there is no response to therapy. Excellent response is found with Welsh regimen which consists of amikacin and cotrimoxazole [15]. Surgical excision of the mass with appropriate antifungals is preferred. Surgical excision alone leads to recurrence; therefore, antifungals should be administered for 3 months.
Conclusion
Mycetoma is a rare infection caused by fungal or bacterial organisms. In the absence of ulceration and sinuses, diagnosis can be difficult. Diagnosis requires a high degree of suspicion in the absence of such clinical signs. Definitive diagnosis should be made on histopathological examination. Once diagnosis is made, surgical excision with appropriate antifungals can result in complete cure without recurrence.
Clinical Message
Mycetoma should be considered as a possible diagnosis, especially in tropical countries with barefoot walkers even in the absence of classical signs and should be treated after confirming with appropriate investigations.
References
1. Turiansky GW, Benson PM, Sperling LC, Sau P, Salkin IF, McGinnis MR, et al. Phialophora verrucosa: A new cause of mycetoma. J Am Acad Dermatol. 1995;32:311-315.
2. McGinnis MR, Fader RC. Mycetoma: A contemporary concept. Infect Dis Clin North Am. 1988;2(4):939-954.
3. Mariat F, Destombes P, Segretain G. The mycetomas: Clinical features, pathology, etiology and epidemiology. Contrib Microbiol Immunol. 1977;4:1-39.
4. Develoux M, Ndiaye B, Dieng MT. Mycetomas in Africa. Sante. 1995;5(4):211-217.
5. Sindhuphak W, Macdonald E, Head E. Actinomycetoma caused by Nocardiopsis dassonvillei. Arch Dermatol. 1985;121(10):1332-1334.
6. Fahal AH, Sheik HE, Homeida MM, Arabi YE, Mahgoub ES. Ultrasonographic imaging of mycetoma. Br J Surg. 1997;84(8):1120-1122.
7. Desai SG, Pardanani DS, Sreedevi N, Mehta RS. Studies on mycetoma. Clinical, mycological, histologic, radiologic studies on 40 cases of mycetoma with a note on its history and epidemiology. Indian J Surg. 1970;32(9-10):427-447.
8. Klokke AH, Swamidasan G, Anguli R, Verghese A. The causal agents of mycetoma in South India. Trans R Soc Trop Med Hyg. 1968;62(4):509-516.
9. Deodhar SD, Shirahatti RG, Vora IM. Primary actinomycosis of the anterior abdominal wall (a case report). J Postgrad Med. 1984;30(2):133-134.
10. Vanbreseghem R. The early diagnosis of mycetoma. Dermatol Int. 1967;6(3):123-140.
11. Talwar P, Sehgal SC. Mycetomas in North India. Sabouraudia. 1979;17(3):287-291.
12. Dogra A, Minocha YC, Gupta M, Khurana S. Actinomycotic mycetoma. Indian J Dermatol Venereol Leprol. 2000;66(6):318-319.
13. Morris MI, Gurevitch A, Edwards JE. Dematiaccae and agents of supedicial mycoses. In: Gorbach SL, Bartlett JG, Blacklow NR, editors. Lnfexians Diseases. Philadelphia PA: WB Saunders; 1992.
14. Young BA, Fee MJ, Giacopelli JA, Granoff DP, Kobayashi W. Mycetoma. J Am Podiatr Med Assoc. 2000;90(2):81-84.
15. Welsh O. Mycetoma. Current concepts in treatment. Int J Dermatol. 1991;30(6):387-398.
| How to Cite This Article: Amit Grover, Prashanth Nagaraj, Vinay M Joseph, Daksh Gadi. Unusual Presentation of Mycetoma of the Foot: A Rare Case Report. Journal of Orthopaedic Case Reports 2017 Jan-Feb;7(1):12-15. Available from: https://www.jocr.co.in/wp/wp-content/uploads/7.-2250-0685.666.pdf |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com





