[box type=”bio”] What to Learn from this Article?[/box]
The reversed less invasive stabilisation system-distal femur technique should be considered as a salvage procedure in rare cases such as in osteogenesis imperfecta whenever intramedullary nailing is difficult.
Case Report | Volume 7 | Issue 3 | JOCR May – June 2017 | Page 71-75| Markus S Hanke, Marius Johann Keel, Inga A Todorski, Johannes Dominik Bastian. DOI: 10.13107/jocr.2250-0685.812
Authors:
Markus S Hanke[1], Marius Johann Keel[1], Inga A Todorski[1], Johannes Dominik Bastian[1]
[1] Department of Orthopaedic and Trauma Surgery, University of Bern, Inselspital, Bern, Switzerland.
Address of Correspondence
PD Dr. Johannes Dominik Bastian,
Department of Orthopaedic and Trauma Surgery, University of Bern, Inselspital, Freiburgstrasse 3, 3010 Bern, Switzerland.
E-mail: johannes.bastian@insel.ch
Abstract
Introduction: The aim of this study was to report the surgical management and to discuss the options for fracture fixation in an adult patient with osteogenesis imperfecta (OI) who sustained a trochanteric femoral fracture after a simple fall from standing position.
Case Report: As a result of multiple fractures during childhood, this adult patient with OI presented with a short stature. The radiographs revealed a displaced, intertrochanteric fracture with subtrochanteric extension of the left femur. The intramedullary canal was narrow, the femur presented with a severe bowing deformity, and the bone quality was poor. The implant of choice was plating using the reversed less invasive stabilisation system-distal femur (LISS-DF) technique. This technique was introduced for the management of subtrochanteric fractures in the elderly with poor bone stock. In addition, a locking plate attached to the LISS-DF allowed for additional screw placement at the apex of the curvature of the femur although the plate was not in line with the femur at this site. Cerclages were used for metaphyseal reduction and fixation. 4-month postoperatively, the patient was ambulatory without any assistance with full weight bearing. At the latest follow-up 1-year postoperatively, the patient was still free of complaints and at her preinjury activity level.
Conclusion: The presented technique was successful as a salvage procedure in a rare case of adult OI presenting with a femoral fracture with characteristics influencing the decision-making in treatment options.
Keywords: Femur, fracture, osteogenesis imperfect, reversed, less invasive stabilisation system-distal femur.
Introduction
Surgical treatment with open reduction and fixation of displaced trochanteric femur fractures in adult patients with osteogenesis imperfect (OI) is challenging. Intramedullary nailing in the presence of a femoral bowing deformity is demanding; three-dimensional correction of the alignment might become necessary to allow for nail insertion while potential changes of soft-tissue restrains have to be considered as well. In addition, the use of plates instead of intramedullary nails might be questionable as the shape of the plate might not fit the deformed alignment of the femur and the poor implant anchorage in the weak bone might result in failure. We present a case of a displaced and comminuted trochanteric fracture in an adult patient with OI presenting with a poor bone stock which was treated successfully by the reversed less invasive stabilisation system-distal femur (LISS-DF) technique.
Case Report
A 29-year-old female South American tourist with known OI was admitted to our emergency department after a stumble fall on her left side. According to the typical presentation of her basic disease, an anterolateral bowing of the left femur was present before the injury, whereas correction osteotomy was performed earlier on her right femur in South America (Fig. 1). She reported about forty fractures and more than thirty surgical treatments since birth. The patient is of a short stature with 1.24 m. On presentation, the patient was conscious, orientated, hemodynamically stable, and complained massive pain on her left hip and femur. The left lower limb presented with shortening and malpositioning in distinct external rotation. The diagnostic workup revealed an intertrochanteric fracture with subtrochanteric extension of the left femur (Fig. 2) with severe bowing deformity (Fig. 3).
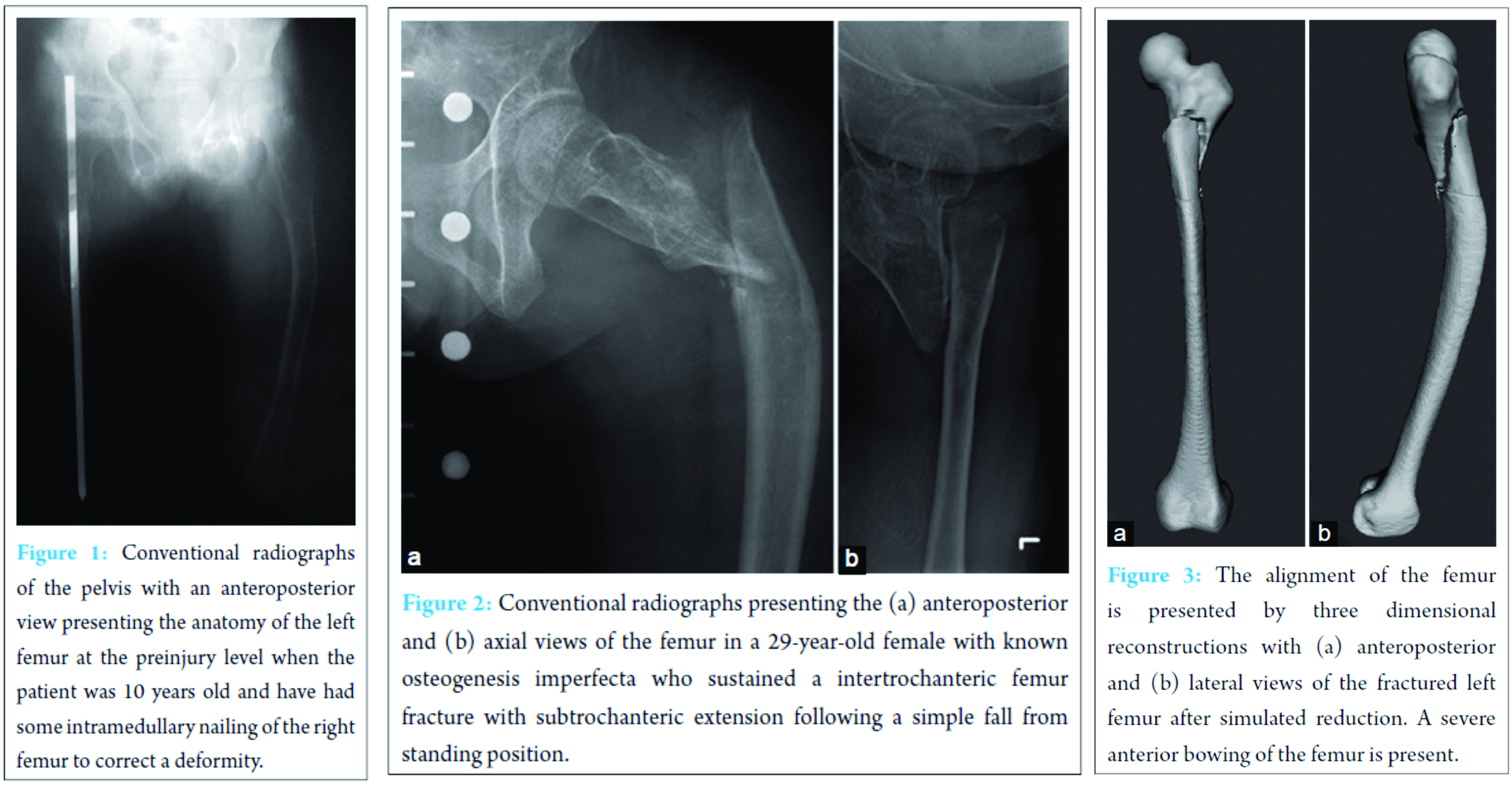 An initial closed reduction of the distinct dislocation of the fracture under analgosedation was performed. Then, the fracture was treated with a LISS-DF (LISS® for the distal femur, DePuy Synthes, Zuchwil, Switzerland) in reversed contralateral application (Fig. 4) [1]. The patient was placed in the lateral decubitus position, and a subvastus approach to the left femur was performed. Fracture reposition was achieved with axial traction, rotation, and a k-wire as joystick in the proximal trochanteric fragment. Preliminary reposition was achieved using cerclages. The insertion of the LISS-DF in reversed contralateral application was performed after pre-bending of the proximal plate in a slight valgus direction to match the patient anatomy. A preliminary k-wire fixation and fluoroscopic control followed by screw fixation of the plate were performed. Furthermore, impaction grafting of the proximal metaphyseal fracture comminution with allograft was carried out. To limit the length of the bridging osteosynthesis, a locking attachment plate was used. This plate facilitated additional screw placement at the apex of the curvature of the femur although the plate was not in line with the femur at this site (Fig. 5b).
An initial closed reduction of the distinct dislocation of the fracture under analgosedation was performed. Then, the fracture was treated with a LISS-DF (LISS® for the distal femur, DePuy Synthes, Zuchwil, Switzerland) in reversed contralateral application (Fig. 4) [1]. The patient was placed in the lateral decubitus position, and a subvastus approach to the left femur was performed. Fracture reposition was achieved with axial traction, rotation, and a k-wire as joystick in the proximal trochanteric fragment. Preliminary reposition was achieved using cerclages. The insertion of the LISS-DF in reversed contralateral application was performed after pre-bending of the proximal plate in a slight valgus direction to match the patient anatomy. A preliminary k-wire fixation and fluoroscopic control followed by screw fixation of the plate were performed. Furthermore, impaction grafting of the proximal metaphyseal fracture comminution with allograft was carried out. To limit the length of the bridging osteosynthesis, a locking attachment plate was used. This plate facilitated additional screw placement at the apex of the curvature of the femur although the plate was not in line with the femur at this site (Fig. 5b).
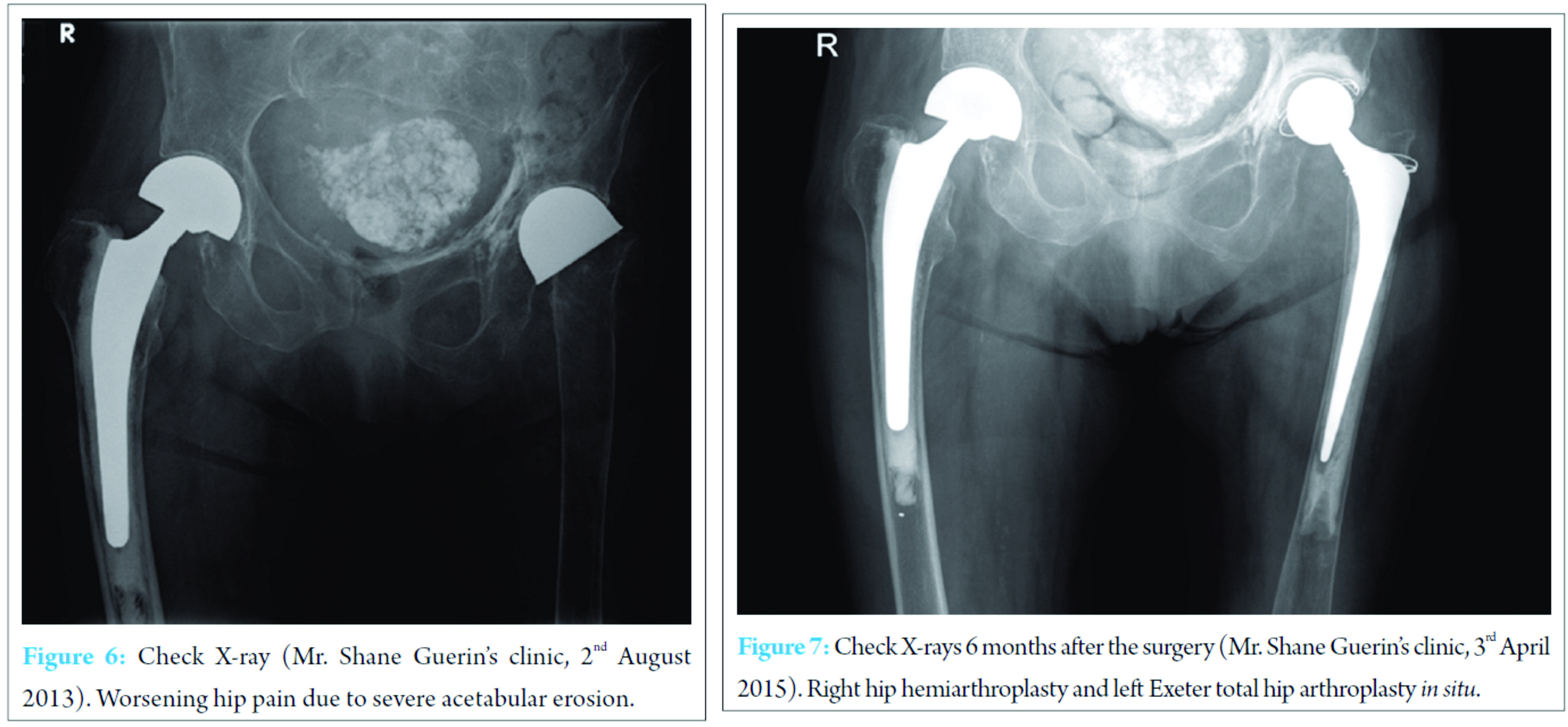
The post-operative regimen consisted of non-weight bearing mobilization for 8 weeks with crutches. Clinical and radiographic follow-up showed no displacement with consolidation of the fracture after 8 weeks (Fig. 5). Hence, the patient was allowed to progress with partial weight bearing for 4 weeks, followed by full weight bearing. The patient was followed up for 12 months and presented already after 5 months with a physical status comparable to the pre-operative level without any limitations (Fig. 6, 7, 8).
Discussion
In general, intramedullary fixation is recommended for the treatment of long bone fractures in OI [2]. However, in long bones, the intramedullary diameter remains small so that only nails with small diameters are applicable, being at risk for nonunion due to inadequate stability [2]. Accordingly, non-union was noted in 24% of fractures and 52% of osteotomies [3]. In addition, proximal femoral fractures are difficult to nail in patients with short skeleton and severely bowed or deformed femurs [4]. Elastic stable intramedullary nailing (ESIN) might be another option for intramedullary osteosynthesis; however, a significantly higher complication rate and a four times higher complication rate in length-unstable fractures (comminution fractures) for ESIN compared to plate osteosynthesis were reported, with the most common complication fracture malalignment at the time of radiographic union [5]. Sink et al. [6] reported in concordance to Li et al. higher complication rates in length-unstable fractures and limited the use of ESIN in these fractures. Our patient presented with a comminuted fracture with a posterolateral fragment, and due to the rather high complication rate in unstable fractures, ESIN was not considered as an osteosynthesis of choice. Due to the comminution, the narrow femoral canal, the severe femoral bowing, and the above mentioned concerns with intramedullary nailing our treatment of choice were plating using a locking compression plate (LCP) without correction of the deformity. The rationale for using a LCP was as follows: OI leads to impaired bone quality comparable to osteoporotic bone. Compared to conventional plate constructs, locking plate constructs have mechanical advantages, and in osteoporotic bone, these are of particular benefit [7, 8]. Besides an increased implant anchorage in the weak bone, the LCP should act as a bridging osteosynthesis alike an internal fixator aiming on relative stability to allow for secondary fracture healing. Due to the short stature of the patient, a locking compression pediatric hip plate might be considered. However, our patient presented with a subtrochanteric extension of the intertrochanteric fracture preventing the use of the relatively short pediatric LCP for the lack of stable fixation. However, a long proximal femoral LCP might be unsuitable as well as due to its lack of anterior curvature and limited options available for screw insertion [9]. Therefore, the reversed LISS-DF technique was used for the following reasons: This plate and technique (1) offers multiple options of fixation and is curved matching the anterior curvature of the femur [1, 10, 11], (2) is able to bear more axial load compared to the standard proximal femoral compression plate offers thus a biomechanical advantage [12], (3) provides a plate head consisting of five-threaded 5.0mm peripheral screw holes accepting locking screws enabling the surgeon to insert two rows of long locking screws up to the femoral calcar to achieve sufficient stability [10, 11], and (4) is effective in avoiding a coxa vara deformity and the use is recommended in patients with severe osteoporosis [13]. The reversed LISS-DF technique showed promising results in biomechanical tests for complex, unstable trochanteric fractures in the elderly or as a salvage procedure [14, 15]. In clinical studies, Acklin et al. [1] recommended the use as a possible alternative in young patients with multifragmentary proximal femoral fractures. Ma et al. [4] recommended the use as an option for fractures that are expected to be difficult to nail. Han et al. [13] recommended the use in patients with severe osteoporosis. Gogna et al. [11] reported promising results in fixation of subtrochanteric fractures. Moreover, this technique was used for successful revision in patients with nonunion of proximal femoral fractures including subtrochanteric fractures after failed intramedullary nailing [10].
Conclusion
The reversed LISS-DF technique was the treatment option of choice and successful in the management of a comminuted femur fracture in an osteoporotic bone in our adult patient suffering from OI with specific anatomic conditions, namely, pronounced bowing of the femur, short skeleton, and narrow endomedullary femoral canal as an alternative to intramedullary nailing.
Clinical Message
The reversed LISS-DF technique was successfully used as a salvage procedure in a rare case of adult OI presenting with a comminuted fracture in a proximal femur poor bone quality and a pre-existing bowing deformity and a narrow intramedullary canal in a patient with a short stature.
References
1. Acklin YP, Bereiter H, Sommer C. Reversed LISS-DF in selected cases of complex proximal femur fractures. Injury 2010;41(4):427-429.Acklin YP, Bereiter H, Sommer C. Reversed LISS-DF in selected cases of complex proximal femur fractures. Injury 2010;41(4):427-429.
2. Cho TJ, Lee K, Oh CW, Park MS, Yoo WJ, Choi IH. Locking plate placement with unicortical screw fixation adjunctive to intramedullary rodding in long bones of patients with osteogenesis imperfecta. J Bone Joint Surg Am 2015;97(9):733-737.
3. Munns CF, Rauch F, Zeitlin L, Fassier F, Glorieux FH. Delayed osteotomy but not fracture healing in pediatric Osteogenesis imperfecta patients receiving pamidronate. J Bone Miner Res 2004;19(11):1779-1786.
4. Ma CH, Tu YK, Yu SW, Yen CY, Yeh JH, Wu CH. Reverse LISS plates for unstable proximal femoral fractures. Injury 2010;41(8):827-833.
5. Li Y, Heyworth BE, Glotzbecker M, Seeley M, Suppan CA, Gagnier J, et al. Comparison of titanium elastic nail and plate fixation of pediatric subtrochanteric femur fractures. J Pediatr Orthop 2013;33(3):232-238.
6. Sink EL, Faro F, Polousky J, Flynn K, Gralla J. Decreased complications of pediatric femur fractures with a change in management. J Pediatr Orthop 2010;30(7):633-637.
7. Miranda MA. Locking plate technology and its role in osteoporotic fractures. Injury 2007;38 Suppl 3:S35-S39.
8. Cornell CN, Ayalon O. Evidence for success with locking plates for fragility fractures. HSS J 2011;7(2):164-169.
9. Patil SS, Karkamkar SS, Patil VS, Patil SS, Ranaware AS. Reverse distal femoral locking compression plate a salvage option in non-union of proximal femoral fractures. Indian J Orthop 2016;50(4):374-378.
10. Vaishya R, Agarwal AK, Gupta N, Vijay V. Reversed distal femoral locking plate for failed proximal femoral nail with non-union of proximal femoral fractures. Int Orthop 2016;40(8):1709-1715.
11. Gogna P, Mukhopadhyay R, Singh A, Devgan A, Arora S, Batra A, et al. Contralateral reversed distal femoral locking plate for fixation of subtrochanteric femoral fractures. Chin J Traumatol 2015;18(5):279-283.
12. MacLean SB, Evans S, O’Hara JN. A comparison of reversed locking compression-distal femoral plates and blade plates in osteotomies for young adult hip pathology. Hip Int 2013;23(6):565-569.
13. Han N, Sun GX, Li ZC, Li GF, Lu QY, Han QH, et al. Comparison of proximal femoral nail anti-rotation blade and reverse less invasive stabilization system-distal femur systems in the treatment of proximal femoral fractures. Orthop Surg 2011;3(1):7-13.
14. Chen Y, Liu S, Lin P, Wang Y, Wang J, Tao J, et al. Comparative biomechanical study of reversed less invasive stabilization system and proximal femoral nail antirotation for unstable intertrochanteric fractures. Chin Med J (Engl) 2014;127(23):4124-4129.
15. Konstantinidis L, Hauschild O, Beckmann NA, Hirschmüller A, Südkamp NP, Helwig P. Treatment of periprosthetic femoral fractures with two different minimal invasive angle-stable plates: Biomechanical comparison studies on cadaveric bones. Injury 2010;41(12):1256-1261.
 |
 |
 |
 |
| Dr. Markus S Hanke | Prof. Dr. Marius Johann Keel | Dr. Inga A Todorski | PD Dr. Johannes Dominik Bastian |
| How to Cite This Article: Hanke MS, Keel MJ, Todorski IA, Bastian JD. The Reversed Less Invasive stabilisation System-Distal Femur Technique: Application in an Adult Patient with Osteogenesis Imperfecta Sustaining a Femoral Fracture. Journal of Orthopaedic Case Reports 2017 May-June;7(3):71-75. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




