[box type=”bio”] Learning Points for this Article: [/box]
Safe procedure for patients who are high risk for anaesthesia and with morbid obesity, where prone position is not possible.
Case Report | Volume 7 | Issue 6 | JOCR November- December 2017 | Page 46-49| Milind V Pimprikar, Madhu Geddam, Hitendra G Patil. DOI: 10.13107/jocr.2250-0685.944
Authors: Milind V Pimprikar [1], Madhu Geddam [1], Hitendra G Patil [1]
[1] Department of Arthroscopy and sports medicine, Nashik, Maharashtra India
Address of Correspondence:
Dr. Milind V Pimprikar,
Dr. Pimprikar’s ADTOOS Clinics, Govind Nagar, Nashik – 422009, Maharashtra, India.
E-mail: drmpimprikar@yahoo.co.in
Abstract
Introduction: The main objective of this case report is to demonstrate endoscopic calcaneoplasty (ECP) using two lateral portals.
Case Report: The patient is middle-aged male aged 40 years, with higher basal metabolic index (BMI) and was diagnosed having a Haglund’s bump and was on conservative treatment for a period of over 6 months, with minimal relief. We did ECP with the patient in lateral decubitus position using two lateral portals instead of using one medial and one lateral portal, his American Orthopaedic Foot and Ankle Society score has improved from 64 to 98, and his Fowler-Philip angle is reduced from 71° to 45°.
Conclusion: ECP using two lateral portals with patient in lateral position is comfortable for the patients with higher BMI and the surgical time can also be reduced. However, we need to perform more number of cases through this technique to conclude to the results.
Keywords: Endoscopic calcaneoplasty, two lateral portals, Haglund’s bump.
Introduction
The common causes for the retrocalcaneal pain are the insertional tendinitis of Achilles tendon, Haglund’s syndrome, and retrocalcaneal bursitis [1, 2]. In 1928, the Swedish orthopedic surgeon, Patrick Haglund described Haglund’s syndrome as a painful osseous prominence of the posterosuperior corner of the calcaneus with large posterior palpable callus, and retrocalcaneal bursitis which was caused by rigid heel counters [3]. This is also known as “pump-bump”. The disorder is caused mechanically from abnormally high pressure between the posterosuperior corner of the calcaneus and the Achilles tendon, and the impingement of the retrocalcaneal bursa between the both leading to the inflammation of the bursa and not by the intrinsic disease of the tendon. Haglund disease is usually observed bilaterally, in the women in their second or third decade [4]. The diagnosis is made with typical history of pain for the initial few steps of walking after a period of rest, proper clinical examination and interpretation with radiographs [5] and ultrasonography (USG) if required. Other pathologies causing pain in the posterior heel should be clearly distinguished. Tenderness caused by isolated sub-tendinous bursitis can best be isolated by palpation just anterior to both the medial and lateral edge of the distal Achilles tendon. Tenderness due to insertional Achilles tendinitis is located slightly more distal, where the Achilles tendon inserts onto the posterior calcaneus [5]. Surgical intervention is the treatment of choice for patients in whom conservative treatment has failed for over 6 months. Open and endoscopic are the two surgical methods. Classic endoscopic calcaneoplasty (ECP) uses one medial and a lateral portal with patient in prone position. In this case report, we are going to discuss about the ECP using two lateral portals with patient in semi-prone or lateral decubitus position.
Case Report
The patient is a 40-year-old male patient with moderate obesity complaining of pain and swelling in the left retrocalcaneal region. X-ray and USG of ankle were taken and diagnosed having Haglund’s bump with retrocalcaneal bursitis, calcification in tendon is ruled out by USG. He was given 6 months of conservative treatment, but there was no improvement. His American Orthopaedic Foot and Ankle Society (AOFAS) score was 64 and Fowler- Philip angle is 71 (Fig. 1). Surgical intervention was planned. Surgical technique: The patient in spinal anesthesia is placed in lateral decubitus position. Tourniquet is placed in the thigh and the other limb is flexed at hip and knee so that it will not interfere with the procedure. The limb is scrubbed and draped, tourniquet inflated. Bony landmarks and the portals are marked.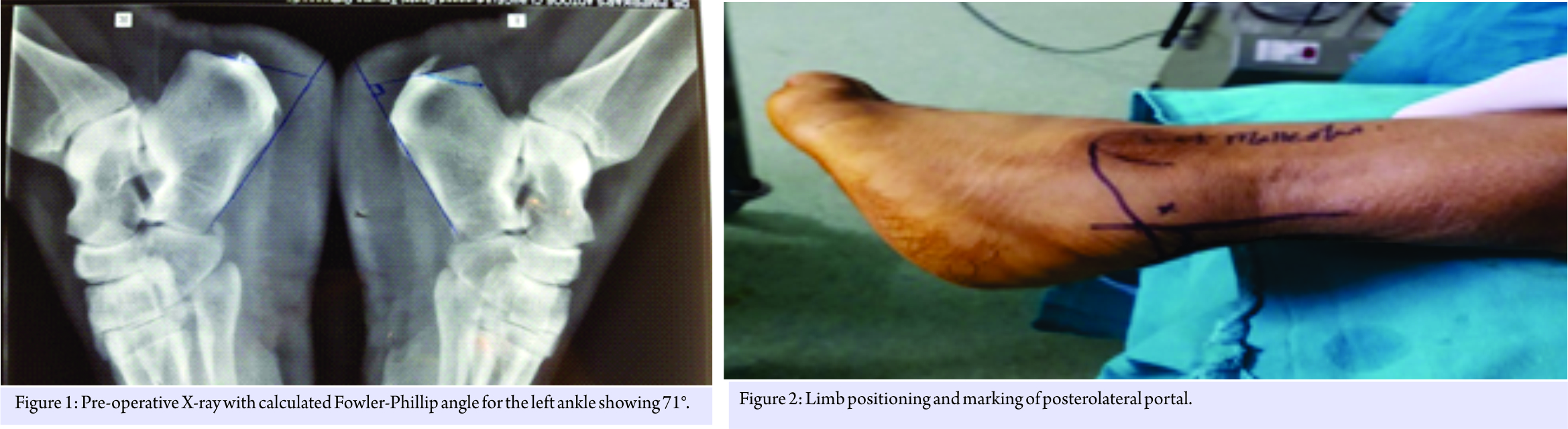
With the ankle in the neutral position, a line was drawn from the tip of the lateral malleolus to the Achilles tendon, parallel to the foot sole. The posterolateral portal was situated just above the line, in front of the Achilles tendon (Fig. 2). A small vertical skin incision is given, blunt trocar was used to reach the retrocalcaneal space and is replaced with 30° 4 mm arthroscope (directing towards 1st web space).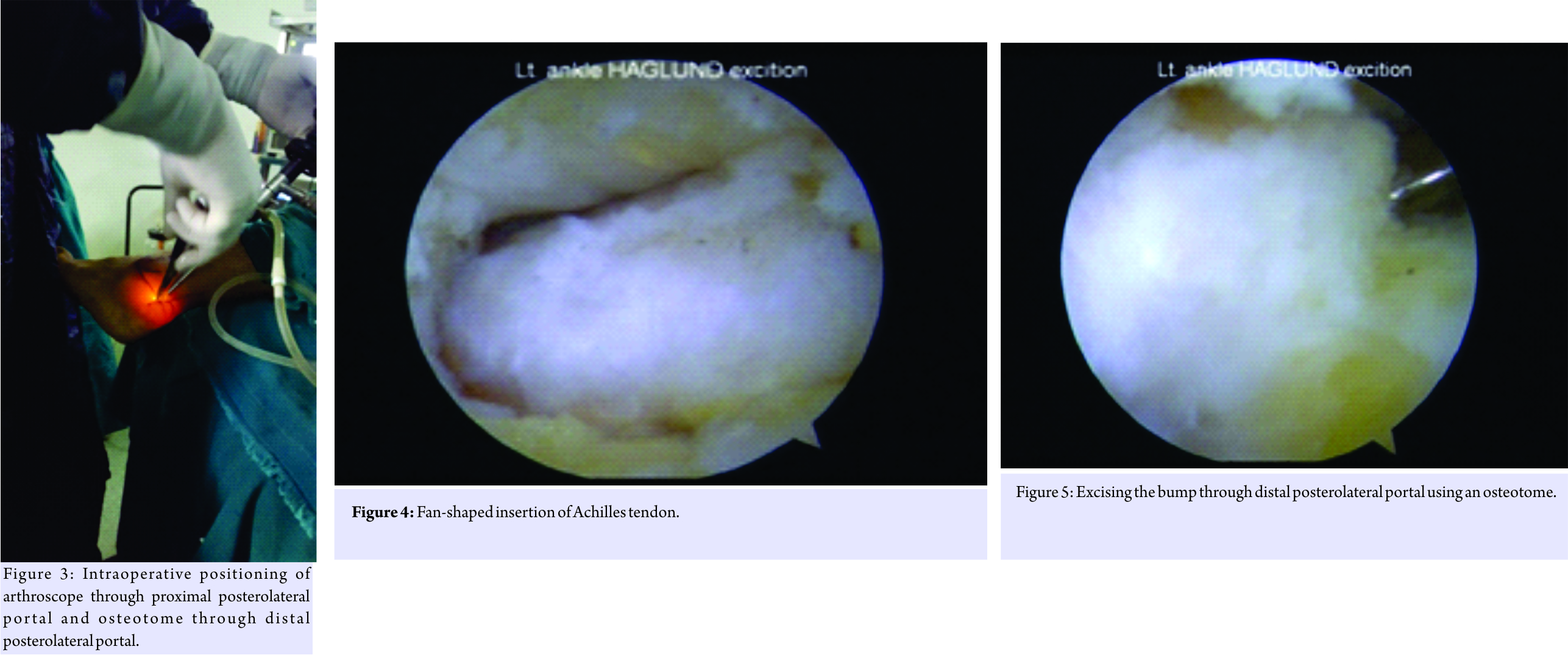
Then, an accessory lateral portal is created by giving a stab incision below the posterolateral portal using a needle as a guide so as to reach the posterolateral corner of the calcaneum. A stab incision is given, spread with mosquito forceps while entering the retrocalcaneal space. The bursa is shaved with a shaver tip facing away from the Achilles tendon. The medial and lateral corners of the Haglund’s bump are viewed after the bursa is shaved off. An osteotome is passed through the accessory lateral portal (Fig. 3) and the Haglund’s bump is removed and is confirmed on fluoroscopy and by plantar flexing the ankle to see whether the sufficient amount has been removed or not. The sharp edges are smoothened using an acromioniser (Fig. 4 and 5). The skin is closed using non-absorbable sutures, and pressure dressing is applied, tourniquet is released (Fig. 6).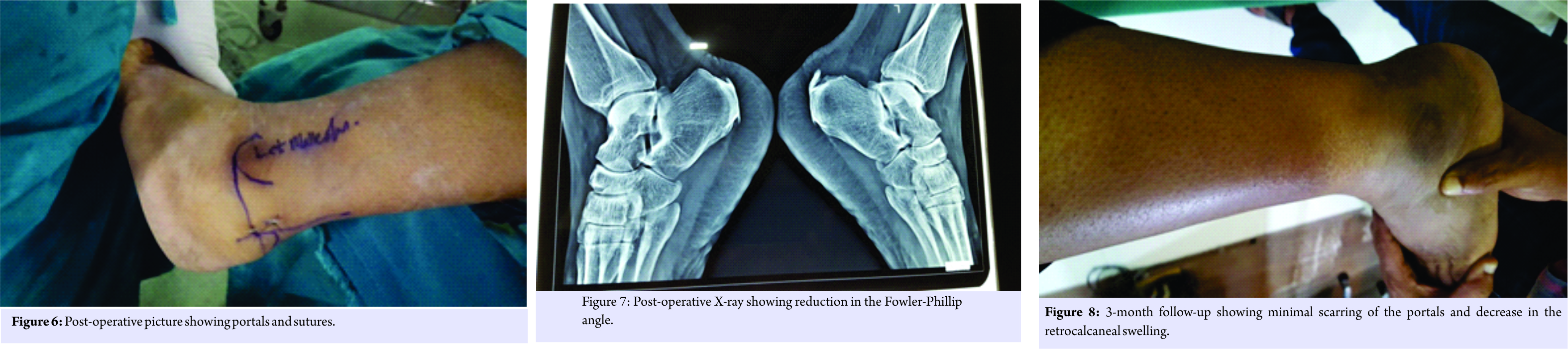
The patient started full ankle range of movements and weight-bearing as tolerated from the 1st post-operative day (P.O.D). He was discharged on the 2nd P.O.D after primary dressing and suture removal was done on the 12th P.O.D. Patient started full weight-bearing from the 13th P.O.D. His post-operative X-ray showed reduction in Fowler-Phillip angle from 71 to 45 (Fig. 7). We did not encounter any complications during intraoperative and post-operative follow-up period. He was followed on the 1st, 3rd, and 6 months postoperation and his AOFAS score improved from 64 to 98 at 6-month follow up. Patient is pleased as there was no swelling in the retrocalcaneal region with minimal scar tissue formation (Fig. 8) and early rehabilitation.
Discussion
Haglund’s syndrome is a common cause for retrocalcaneal heel pain. Biomechanical studies show an increasing pressure on the retrocalcaneal bursa during dorsiflexion of the foot and a decrease of the pressure in plantar flexion [6]. Symptoms often worsen when the person first initiates an activity after a period of rest. Tenderness due to insertional Achilles tendinitis is located slightly more distal, where the Achilles tendon inserts onto the posterior calcaneus. While in Haglund’s disease, tenderness is usually 3–4 cm proximal to the insertion of the Achilles tendon [5]. In the open procedure, the surgical goal is to achieve complete exposure of the retrocalcaneal space and to perform the resection of the bump without weakening the insertion of the Achilles tendon [7, 8]. The same goal can be achieved endoscopically. Following open surgery, various complications have been reported such as skin complications [7], hyperesthesia in the area of the scar [9], irritation of the scar [10], Achilles tendon lesions [11], weakness of the calcaneus after removing the posterosuperior bony prominence [12], persistent pain [13], and irritation of the whole heel [13]. Advantages of endoscopic technique over open surgeries are short recovery time, rapid return to work and sports, small incision, and good scar healing [4, 14]. Because endoscopic treatment for Haglund’s syndrome is a new procedure and experience is limited, modification of endoscopic techniques has continued to evolve, aiming to avoid complications and improve outcome. Wu et al., [15] in 2012 used three portal techniques for ECP for 23 patients and achieved good results. They used two lateral portals, proximal posterolateral (primary viewing), and distal posterolateral and one distal posteromedial portal (working portals). In our case, we made only proximal and distal posterolateral portals. Interchanging of portals was not required as we used an osteotome for excising the Haglund’s bump through distal posterolateral portal, thereby creating enough space for the shaver to reach posteromedial corner of the heel to excise the inflamed bursa if present. We achieved an excellent result using this technique. The operating time was only 20 min. However, we need to perform more number of cases through this technique to conclude to the results.
Conclusion
Using two lateral portals with patient in lateral decubitus position is comfortable and less time consuming for obese patients for ECP and can be a viable option for classic procedure using medial and lateral portals.
Clinical Message
Normally, ECP is done in prone position using medial and lateral portals. However, in our case, the patient was obese with higher basal metabolic index (BMI). Prone position in such patients is a higher anesthesia risk and can create complications. Hence, placing these patients in lateral decubitus position can avoid such complications. We used two lateral portals instead of taking one medial and one lateral portal, as it is technically difficult to create medial portal in lateral decubitus position. Thus, it becomes advantageous to operate these patients in lateral decubitus position using two lateral portals and can be a good option in patients with central obesity, high BMI, as well as high-risk patients.
References
1. Clancy WG. Runners’ injuries. Part two. evaluation and treatment of specific injuries. Am J Sports Med 1980;8:287-9.
2. Fiamengo SA, Warren RF, Marshall JL, Vigorita VT, Hersh A. Posterior heel pain associated with a calcaneal step and Achilles tendon calcification. Clin Orthop Relat Res 1982;162:203-11.
3. Haglund P. Beitragzur klinik der Achilles tendon. Zeitschr Orthop Chir 1928;49:49-58.
4. Jerosch J, Schunck J, Sokkar SH. Endoscopic calcaneoplasty (ECP) as a surgical treatment of haglund’s syndrome. Knee Surg Sports Traumatol Arthrosc 2007;15:927-34.
5. Van Dijk CN, van Dyk CE, Scholten PE, Kort NP. Endoscopic calcaneoplasty. Foot Ankle Clin 2006;2:439-46.
6. Jerosch J. Endoscopic calcaneoplasty. Foot Ankle Clin 2015;20:149-65.
7. Pauker M, Katz K, Yosipovitch Z. Calcaneal osteotomy for haglund’s disease. J Foot Surg 1992;31:558-89.
8. Keck SW, Kelly PJ. Bursitis of the posterior part of the heel: Evaluation of surgical treatment of 18 patients. J Bone Joint Surg Am 1965;47A:267-73.
9. Angermann P. Chronic retrocalcaneal bursitis treated by resection of the calcaneus. Foot Ankle 1990;10:285-7.
10. Leach RE, Dilorio E, Harney RA. Pathological hindfoot conditions in the athlete. Clin Orthop 1983;177:116-21.
11. Le TA, Joseph PM. Common exostectomies of the rearfoot. Clin Podiatr Med Surg 1991;8:601-23.
12. Periman MD. Enlargement of the entire posterior aspect of the calcaneus: Treatment with the Keck and Kelly calcaneal osteotomy. J Foot Surg 1992;31:424-33.
13. Nesse E, Finsen V. Poor results after resection for haglund’s heel. Analysis of 35 heels treated by arthroscopic removal of bony spurs. Acta Orthop Scand 1994;65:107-9.
14. Jerosch J, Nasef NM. Endoscopic calcaneoplasty – Rationale, surgical technique, and early results: A preliminary report. Knee Surg Sports Traumatol Arthrosc 2003;11:190-5.
15. Wu Z, Hua Y, Li Y, Chen S. Endoscopic treatment of haglund’s syndrome with a three portal technique. Int Orthop 2012;36:1623-7.
 |
 |
 |
| Dr. Milind Pimprikar | Dr. Madhu Geddam | Dr. Hitendra Patil |
| How to Cite This Article: Pimprikar MV, Geddam M, Patil HG. Endoscopic Calcaneoplasty for Haglund’s Excision Using Two Lateral Portals. Journal of Orthopaedic Case Reports 2017 Nov-Dec; 7(6): 46-49 |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




