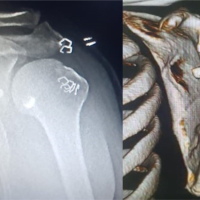
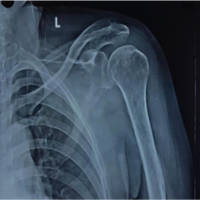
[box type=”bio”] Learning Point for this Article: [/box]
A high index of suspicion along with additional use of a 70 degree arthroscope leads to a higher rate of pick up of subscapularis tears.
Case Report | Volume 8 | Issue 2 | JOCR Mar – Apr 2018 | Page 51-53| Waqar Saadat, Fraser Taylor, Rahul Kakkar, Puneet Monga. DOI: 10.13107/jocr.2250-0685.1046
Authors: Waqar Saadat[1], Fraser Taylor[2], Rahul Kakkar[2], Puneet Monga[3]
[1]Department of Trauma and Orthopaedic, Furness General Hospital, Barrow-in-Furness, UK.
[2]Department of Trauma and Orthopaedic, John Flynn Medical Centre, John Flynn Private Hospital, Brisbane,Queensland, Australia.
[3]Upper Limb Unit, Wrightington, Wigan and Leigh NHS Trust, UK.
Address of Correspondence:
Dr. Waqar Saadat,
Furness General Hospital, Barrow-in-Furness LA14 4LF, UK.
E-mail: waqarsaadat@yahoo.com
Abstract
Introduction: Subscapularis tendon plays an important role in shoulder stability and functions. There has been much interest recently in the prevalence of subscapularis tears and outcomes following repair of subscapularis tears. We aimed to assess whether there is an increase in pick up rate of subscapularis tears in patients who underwent arthroscopic rotator cuff repair following routine additional use of a 70° arthroscope during shoulder arthroscopy.
Materials and Methods: A retrospective review of a single surgeons practice was performed to assess the frequency of identifying and repairing subscapularis tears among a cohort of 58 consecutive arthroscopic rotator cuff tears performed over a 12 months period. The patients’ had an age ranged between 42 and 71 years (mean 54.4). The case mix was a combination of degenerative and traumatic tears. All-arthroscopic procedures had an additional assessment with a 70° arthroscope, in addition to routine assessment with a 30° arthroscope. The follow-up ranged from 30 to 120 days. The prevalence of subscapularis tendon tears was noted intraoperatively. This was compared to the pre-operative incidence as determined by the various clinical examination and radiological techniques.
Results: Of the 58 arthroscopic rotator cuff repairs, subscapularis tear was identified in 25 patients (43.1%). Among the imaging modalities used pre-operative magnetic resonance imaging scanning reported a subscapularis tear in 71.4% and pre-operative ultrasound scanning reported a tear in 78.6.
Conclusion: The use of a 70° arthroscope can facilitate the recognition and management of subscapularis tears which may not be recognized with a routine 30° shoulder arthroscope. A combination of high index of suspicion, judicious use of pre-operative imaging and careful arthroscopic assessment aids identification of subscapularis tendon tears.
Keywords: Subscapularis tear, 70° arthroscope, shoulder arthroscopy.
Introduction
Rotator cuff tears are a frequent cause of shoulder dysfunction and pain in adults. Compared to supraspinatus tear, subscapularis tendon tears are less common. Visualization of the complete tendon’s insertion on the lesser tuberosity can be challenging as the viewing portal is posterior and the subscapularis tendon insertion is over the anterior aspect of the humeral head. Hence, routine 30° arthroscopic evaluation may miss certain lesions [1]. Subscapularis tears were once thought to be uncommon; however, the literature suggests the incidence of subscapularis tear by arthroscopic evaluation may range from 27% to 43% [2, 3, 4]. The subscapularis important in arm elevation and to balance the posterior forces of rotator cuff [5, 6], therefore recognition and repair of a subscapularis tear are very important to restore function following surgical input. Comprehensive arthroscopic assessment of the medial wall of the bicipital groove and the medial biceps sling is needed to detect these tears which can be easily missed [7]. To assess the integrity of the subscapularis tendon, 70° arthroscope is advisable [7]. It will help in the complete visualization of the tendon’s insertion on lesser tuberosity which may be otherwise challenging as one has to look “over the hill” from the posterior viewing portal. The aim of this study was to assess whether there is an increase in pick up rate of subscapularis tears in patients who underwent arthroscopic rotator cuff repair following routine additional use of a 70° arthroscope during shoulder arthroscopy.
Materials and Methods
This was a retrospective study involving assessment of the prevalence of subscapularis tears among a cohort of 58 consecutive arthroscopic rotator cuff tears performed over 12 months at our institution by a single surgeon. All the procedures were done in standard beach chair position. Data were collected concerning intraoperative arthroscopic findings and details of surgical interventions. The case mix was a combination of degenerative and traumatic tears. All patients who had a routine assessment with 30° arthroscope also had an additional assessment with a 70° arthroscope. Average follow-up ranged from 30 to 120 days. Secondary measures including the pre-operative clinical examination findings and radiological findings as reported by the radiologist were also gathered and compared with the intraoperative findings.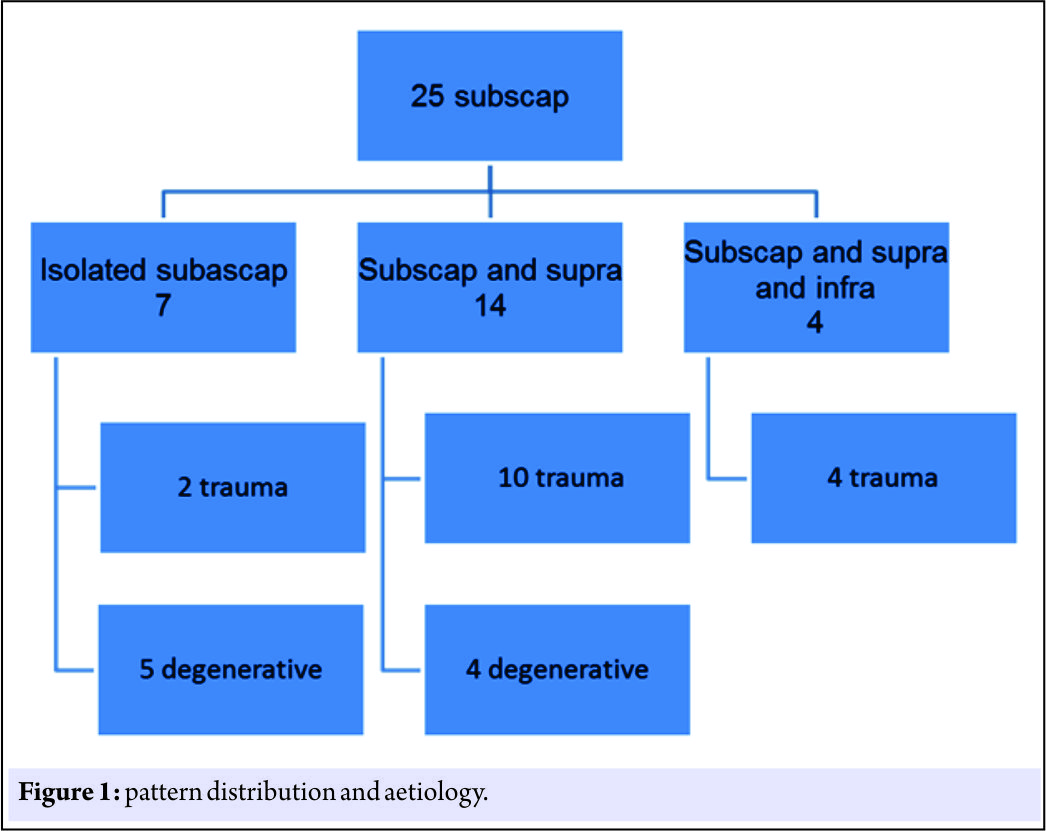
Results
During the study, clinical notes of all 58 patients were reviewed. The patients’ had an age ranged between 42 and 71 years (mean 54.4). The interval time from the date of an assessment in outpatient to surgical procedure was 30–120 days. Out of a cohort of 58 patients who underwent arthroscopic assessment, 25 patients’ had subscapularis tear. 7 patients had isolated subscapularis tear, 14 had both subscapularis and supraspinatus tear, and 4 patients had subscapularis, supraspinatus and infraspinatus tear resulting after trauma to their shoulder (Fig. 1). Clinical examination was able to pick up subscapularis tears in 56% cases, although these were mainly full thickness tear. The sensitivity of magnetic resonance imaging (MRI) scan to diagnose subscapularis tear was 71%, and that of ultrasound scan was 78%. Clinical examination, ultrasound and MRI were not conclusive in pre-operative planning in 7 patients who were later diagnosed to have isolated subscapularis tear when additional assessment with the 70° scope was carried out. These 7 patients had isolated partial thickness subscapularis tear.
Discussion
The precise prevalence rates of subscapularis tear are unclear. Kim et al. noted a prevalence of 19% subscapularis tendon tears during arthroscopic procedures on 314 consecutive shoulders [9]. In this study, the prevalence rate of subscapularis tear was 43% in 58 shoulder arthroscopies performed for rotator cuff pathology. Higher incidence of subscapularis tears in comparison to the study reported by Kim et al. [9] is perhaps due to the fact that in this study only arthroscopies that had rotator cuff repair were included while in latter, all arthroscopies performed for other pathologies like instability were also considered. With the refinements in clinical examination tests and despite recent advances in using MRI for the detection of rotator cuff tears, lesions of the subscapularis tendon are still an underdiagnosed [10]. The studies have shown great variation in the MRI finding with regard to rotator cuff pathologies, with sensitivity values ranging from 0.41 to 1.0 and specificity from 0.1 to 0.79 [11]. In this study, the ultrasound scan was more sensitive, perhaps due to the special interest of the observer and hence an increased awareness. This study confirms that clinical examination was able to pick up subscapularis tear in 56% of patients mainly that had full thickness tear. The clinical tests are helpful in raising the suspicion about possible subscapularis pathology, but the sensitivity and specificity of the tests remain low [12]. Limitation of the study was that it is a retrospective cohort study. There may also be a bias in the interpretation of what constitutes a tear during the intraoperative assessment. The study does not comment on the clinical outcomes of subscapularis tendon repairs and future studies looking at outcomes of repair of partial subscapularis tendon tears would be recommended.
Conclusion
The combination of detailed history, clinical examination and pre-operative imaging and arthroscopic assessment helps in identification of subscapularis tear. Using a 70° arthroscope facilitates recognition of subscapularis tears.
Clinical Message
Additional use of a 70° arthroscope during shoulder arthroscopy facilitates the recognition of subscapularis tears.
References
1. David TS, Bravo H, Scobercea R, Arthroscopic visualization of sub scapularis tendon lesions. Orthopaedics 2009;32:9.
2. Bennett WF. Arthroscopic repair of isolated subscapularis tears: A prospective cohort with 2-to 4-years follow-up. Arthroscopy 2003;19:131-4.
3. Adams CR, Schoolfield JD, Burkart SS. The results of arthroscopic subscapularis tendon repairs. Arthroscopy 2008;24:1381-9.
4. Park YB, Park YE, Koh KH, Lim TK, Shon MS, Yoo JC. Subscapularis tendon repair using suture Bridge technique. Arthrosc Tech 2015;23:133-7.
5. Kelly BT, Williams RJ, Cordasco FA, Backus SI, Otis JC, Weiland DE,et al. Differential patterns of muscle activation in patients with symptomatic and asymptomatic rotator cuff tears. J Shoulder Elbow Surg 2005;14:165-71.
6. Burkhart SS, Esch JC, Jolson RS. The rotator crescent and rotator cable: An anatomic description of the shoulder’s “suspension bridge”. Arthroscopy 1993;9:611-6.
7. Burkhart SS, Koo SS.Subscapularis tendon tears: Identifying mid to distal footprint disruption. Arthroscopy 2010;26:1130-4.
8. Narasimhan R, Shamse K, Nash C, Dhingra D, Kennedy S. Prevalence of subscapularis tears and accuracy of shoulder ultrasound in pre-operative diagnosis. Int Orthop 2016;40:975-9.
9. Kim TK, Rauh PB, McFarland EG. Partial tears of subscapularis tendon found during arthroscopic procedures on the shoulder: A statistical analysis of sixty case. Am J Sports Med 2003;31:744-50.
10. Lafosse L, Jost B, Reiland Y, Audebert S, Toussaint B, Gobezie R. Structural integrity and clinical outcomes after arthroscopic repair of isolated subscapularis tears. J Bone Joint Surg Am 2007;89:1184-93.
11. Quinn SF, Sheley RC, Demlow TA, Szumowski J. Rotator cuff tendon tears: Evaluation with fat-suppressed MR imaging with arthroscopic correlation in 100 patients. Radiology 1995;195:497-500.
12. Beaudreuil J, Nizard R, Thomas T, Peyre M, Liotard JP, Boileau P, et al. Contribution of clinical tests to the diagnosis of rotator cuff disease: A systematic literature review. Joint Bone Spine 2009;76:15-9.
 |
 |
| Dr. Waqar Saadat | Dr. Puneet Monga |
| How to Cite This Article: Saadat W, Taylor F, Kakkar R, Monga P. Using a 70° Scope Facilitates Pick up Rates of Subscapularis Tears. Journal of Orthopaedic Case Reports 2018. Mar- April; 8(2): 51-53. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com