[box type=”bio”] Learning Point of the Article: [/box]
Streptococcus Pyogenes can cause a wide range of diseases, including some serious conditions. Early diagnosis is challenging due to unspecific symptoms. When suspected, surgical management should be considered as first-line treatment.
Case Report | Volume 8 | Issue 5 | JOCR September – October 2018 | Page 57-60| Mariano Oscar Abrego, Javier EduardoSanchez Saba, Carolina Halliburton, Danilo Roger Eric Taype, Carlos Federico Sancineto. DOI: 10.13107/jocr.2250-0685.1212
Authors: Mariano Oscar Abrego[1], Javier EduardoSanchez Saba[1], Carolina Halliburton[1], Danilo Roger Eric Taype[1], Carlos Federico Sancineto[1]
[1]Department of Orthopedics and Trauma, Carlos E. Ottolenghi, Hospital Italiano de Buenos Aires, Juan D. PeronStreet 4190, C1181ACH, Ciudad Autónoma de Buenos Aires, Argentina.
Address of Correspondence:
Dr. Mariano Abrego,
Department of Orthopedics and Trauma, Carlos E. Ottolenghi, Hospital Italiano de Buenos Aires, Juan D. Peron street 4190, C1181ACH,Ciudad Autónoma de Buenos Aires, Argentina.
E-mail: mariano.abrego@hospitalitaliano.org.ar
Abstract
Introduction: Fasciitis of the limb and toxic-shock syndrome due to Streptococcus Pyogenes infection is considered a surgical emergency. This condition may occur in previously healthy patients. It is a life-threatening condition with high morbidity rates when treatment is delayed due to poor diagnosis and non-surgical intervention.
Case Report: 17-year-old male patient sustained a minor ankle trauma while skating. Initials findings were a 1 cm wound in relation with his left lateral malleolus and moderate swelling. About 6 h later, the patient was admitted at the emergency room with disproportionate limb pain, increased swelling, persistent fever, paleness, tachycardia, and hypotension. The patient was intubated due to his unstable hemodynamic condition and underwent fasciotomy of the limb. A vacuum-assisted closure device was used. After the first surgical procedure, patient’s condition radically improved. He was extubated with good clinical prognosis. He underwent several surgical procedures in a 3-weeks lapse until the wound finally healed.
Conclusion: Streptococcal toxic-shock syndrome and limb fasciitis have no specific early signs or symptoms. It seems that clinical dissociation (disproportionate pain together with a minor wound) should become an alarm sign to trauma surgeons. It is important to contemplate this serious condition as differential diagnosis in every patient undergoing trauma with torpid evolution. Aggressive surgical management is the gold standard treatment and should not be delayed.
Keywords: Case report, lower limb fasciitis, streptococcal toxic-shock syndrome.
Introduction
Streptococcus Pyogenesis the anaerobic bacterium responsible for a variety of diseases including tonsillitis, pharyngitis, scarlet fever, and soft tissue conditions such as streptococcal pyoderma, erysipelas, and cellulitis. Erysipelas is an infection of the superficial dermis with a bright-red area of raised skin. Some authors state that erysipelas is a sharply demarcated variant of cellulitis (chira, raff, and gunderson). Cellulitis is an infection of the deep dermis and subcutaneous layers, presenting as an acute, poorly demarcated area of erythema (raff). Much less common but still lethal is fasciitis caused by this pathogen. Fasciitis is a severe infection involving superficial fascias and deep dermal layers of the skin. On early stages, fasciitis can mimic cellulitis. This can lead to insufficient treatment. Statistics show that mortality rates have been reported as high as 78%. Toxicity and severe pain increase the likelihood of fasciitis over other soft tissue conditions such as cellulitis[4, 5]. Typical clinical profile refers to a swollen limb in previously healthy patients, with a wound susceptible to outside contaminated environment. Trauma is the most frequent cause [6]. The progression of the disease is rapid, and the whole limb can become affected in a few hours [7]. Initial symptoms can be unspecific, and physicians may tend to relate them to mild infections [8, 9]. Severe streptococcal infection may develop into shock-toxic syndrome. Diagnosis is determined by the fast evolution into shock and multiorganic failure together with the isolation and identification of the microorganism [10].
The diagnostic criteria of shock-toxic syndrome are listed as follows[11]:
1. Sustained arterial hypotension combined with tissue hypoperfusion signs.
2. Acute kidney failure.
3. Disseminated intravascular coagulation or any other coagulation disorder.
4. Hepatic impairment.
5. Respiratory distress.
6. Diffuse erythema.
7. Skin and soft tissue necrosis.
Diagnosis is made with at least two criteria plus sustained arterial hypotension. Wide-spectrum empirical antibiotic therapy alone shows limited action. Surgical debridement and drainage together with antibiotic therapy are considered the gold standard treatment [6, 8]. In this paper, we present the case of a patient that sustained a minor ankle trauma with torpid outcome which develops into lower limb fasciitis and multiorganic failure. We discuss its surgical management and evolution.
Case Report
A 17-year-old male patient sustained a minor ankle trauma while skating. He was first admitted to a local health department. Initial findings were a 1 cm long wound in relation with his left lateral malleolus together with moderate swelling. No other sign or symptom was reported. Plain radiographs were performed with nopathological findings. About 6 hours later, the patient was admitted at our emergency room with disproportional limb pain, increased swelling, persistent fever, paleness, tachycardia, and hypotension (Fig. 1a and b). Blood tests showed anemia, leukocytosis, and elevated creatine phosphokinase (Table 1). The general condition of the patient got worse, with the need of mechanical ventilation and vasopressors due to the hemodynamic instability. Empiric antibiotic therapy was established with a triple scheme (ceftriaxone, vancomycin, and clindamycin). A computed tomography (CT) scan was done to find the presence of collections (Fig. 2a, b, c). The patient underwent his first surgical procedure which consisted of double fasciotomy of the leg, toexamine and release the tension of the four compartments involved (Fig. 3a and b). Mubarak and Owen [12] technique was used. Purulent material was obtained with no signs of necrosis. Drainage of the medial thigh compartment was performed at the same procedure. A vacuum-assisted closure device was used. Both leg incisions were primary closed (Fig. 4a and b). Multiple samples were forwarded to cultivation. Culture media demonstrated the presence of Streptococcus Pyogenes. The acute toxic-shock syndrome yielded immediately after fasciotomy. 24 hours later, the patient did no longer need mechanical ventilation and blood tests showed almost normal results. The patient underwent two more surgical procedures with the purpose of vacuum-assisted closure management and thigh wound healing. 1 week later, the patient was discharged from our institution. After 3 years of follow-up, the patient has fully recovered, with a functional limb with no restrictions.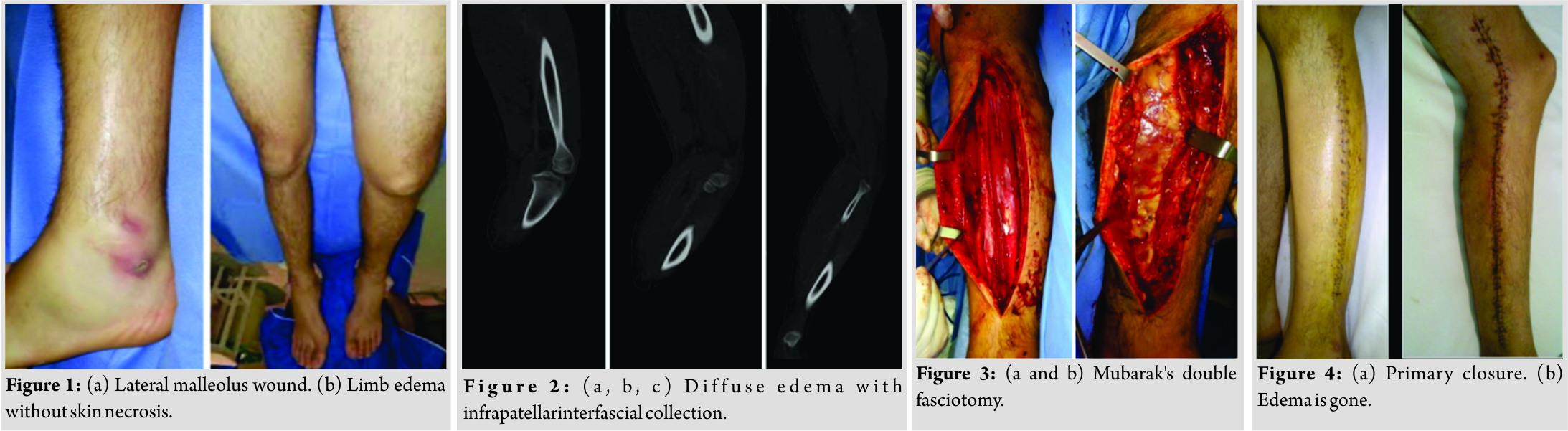
Discussion
Streptococcus Pyogenescan be responsible for very aggressive infections [4]Early and precise diagnosis is the key to good clinical outcome and therefore increased survival rates [13]. Cellulitis often shows a slower clinical course than fasciitis and recovery with conservative treatment is possible, without aggressive surgical intervention(Gundeslioglu). It is important to understand that apparently healthy patients with no chronic diseases are also possible targets for these devastating infections. CT scan or magnetic resonance imaging may be useful to find collections and to delimit the deepness of the infection. However, no image study should delay surgical management [15]. Bisno and Stevens [4] described three clinical stages regarding toxic-shock syndrome. Symptoms tend to be unspecific in the first two stages at least. Third stage involves extreme disproportionate pain and multiorganic failure. In this index case, the patient suffered unspecific symptoms (fever, tachycardia, and paleness) according to stages one and two plus the rapid onset of stage three. . Patients evolve fast from stage one to stage three, in which survival rates decreased drastically. Antibiotic therapy is still one of the main treatments but hypoxia followed by local ischemia may act as a barrier which prevents the active principle to reach the infection area. Antibiotics alone represent an insufficient treatment [6, 8, 16]. Khanna et al. [17] published a series of 118 lower limb fasciitis. Mortality was 15%, based on early surgical management. 24 patients suffered amputation of the limb. The authors referred that early diagnosis combined with fast and aggressive surgical procedures are the key to success. Goh et al. [18] performed a systematic review, from which they selected nine works involving more than 1400 patients trying to establish early onset symptoms. They reached the conclusion that disproportionate pain, edema, and erythema were responsible for the majority of cases and also lead to diagnostic errors. Seventy-Five percent of the patients suffered from poor diagnosis leading to inadequate treatment. The authors concluded that early surgical treatment must be considered even if the diagnosis is unclear. Regarding fasciotomy techniques, Mubarak and Owen proven to be satisfactory to decompress all leg compartments [12]. Vacuum-assisted closure is also a proven method for surgical wounds and post-operative management [6].
Conclusion
Streptococcal toxic-shock syndrome and limb fasciitis have no specific early signs or symptoms. It seems that clinical dissociation (disproportionate pain together with a minor wound) should become an alarm sign to trauma surgeons. It is important to contemplate this serious condition as differential diagnosis in every patient undergoing trauma with torpid evolution. Aggressive surgical management is the gold standard treatment and should not be delayed.
Clinical Message
Streptococcus Pyogenes can cause a wide range of diseases, including some serious conditions. Early diagnosis is challenging due to unspecific symptoms. When suspected, surgical management should be considered as first-line treatment.
All investigations were conducted in conformity with ethical principles of research. Informed consent was obtained from the patient for the use of all images and publication of this report.
All authors certify that their institution has approved the reporting of this case.
All authors declare that there are no competing interests regarding the publication of this paper.
The study was performed at the Italian Hospital of Buenos Aires, Argentina.
References
1. Chira S, Miller LG. Staphylococcus aureus is the most common identified cause of cellulitis: A systematic review. Epidemiol Infect 2010;138:313-7.
2. Raff AB, Kroshinsky D. Cellulitis: A review. JAMA2016;316:325-37.
3. Gunderson CG, Martinello RA. A systematic review of bacteremias in cellulitis and erysipelas. J Infect2012;64:148-55.
4. Bisno AL, Stevens DL. Streptococcal infections of skin and soft tissues. N Engl J Med 1996;334:240-5.
5. Stamenkovic I, Lew PD. Early recognition of potentially fatal necrotizing fasciitis. The use of frozen-section biopsy. N Engl J Med 1984;310:1689-93.
6. Misiakos EP, Bagias G, Patapis P, Sotiropoulos D, Kanavidis P, Machairas A, et al. Current concepts in the management of necrotizing fasciitis. Front Surg 2014;1:36.
7. Stone HH, Martin JD Jr.Synergistic necrotizing cellulitis. Ann Surg 1972;175:702-11.
8. Wang KC, Shih CH. Necrotizing fasciitis of the extremities. J Trauma 1992;32:179-82.
9. Tang WM, Ho PL, Fung KK, Yuen KY, Leong JC. Necrotizing fasciitis of a limb. J Bone Joint Surg [Br] 2001;83-B:709-14.
10. Defining the group A streptococcal toxic shock syndrome. Rationale and consensus definition. The working group on severe streptococcal infections. JAMA 1993;269:390-1.
11. Fernández Guerrero ML, Quesada GM, Borja MB,Corral JL. La gangrena estreptocócica y la así llamada “enfermedad de las bacterias devoradoras de carne” una infección rara y devastadora. Rev ClínEspañola 1999;199:84-8.
12. Mubarak SJ, Owen CA. Double-incision fasciotomy of the leg for decompression in compartment syndromes. J Bone Joint Surg Am1977;59:184-7.
13. Gauzit R. Necrotizing skin and soft tissue infections: Definitions, clinical and microbiological features. Ann Fr AnesthReanim2006;25:967-70.
14. Gundeslioglu AO, Selimoglu MN, Toy H. Is it necrotizing fasciitis or necrotizing cellulitis after varicella zoster infection? Two case reports. Ann Plast Surg 2014;73:202-4.
15. Struk DW, Munk PL, Lee MJ,Ho SG, Worsley DF. Imaging of soft tissue infections. RadiolClinNorth Am 2001;39:277-303.
16. Marron CD. Superficial sepsis, cutaneous abscess and necrotizing fasciitis. In: Brooks A, Mahoney PF, Cotton BA, Tai N, editors. Emergency Surgery. Oxford, UK: Blackwell Publishing; 2010. p. 115-23.
17. Khanna AK, Tiwary SK, Kumar P, Khanna R, Khanna A. A case series describing 118 patients with lower limb necrotizing fasciitis. Int J Low Extrem Wounds 2009;8:112-6.
18. Goh T, Goh LG, Ang CH,Wong CH. Early diagnosis of necrotizing fasciitis. Br J Surg 2014;101:119-25.
 |
 |
 |
 |
 |
| Dr. Mariano Oscar Abrego | Dr. Mariano Oscar Abrego | Dr. Carolina Halliburton | Dr. Danilo Roger EricTaype | Dr. Carlos Federico Sancineto |
| How to Cite This Article: Abrego M O, Sanchez Saba J E, Halliburton C, TaypeD R E, Sancineto C F. Fasciitis and Streptococcal Toxic-shock Syndrome: The Importance of Early Diagnosis and Surgical Management. Journal of Orthopaedic Case Reports 2018 Sep-Oct; 8(5): 57-60. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




