[box type=”bio”] Learning Point of the Article: [/box]
An alternative surgical treatment for patient with soft tissue defect at anterior aspect of knee joint by using the distally based sartorius flap.
Case Report | Volume 9 | Issue 3 | JOCR May-June 2019 | Page 43-45 | Sunyarn Niempoog, Yot Tanariyakul. DOI: 10.13107/jocr.2250-0685.1412
Authors: Sunyarn Niempoog[1], Yot Tanariyakul[1]
[1]Department of Orthopedics, Faculty of Medicine, Thammasat University, Thailand.
Address of Correspondence:
Dr. Yot Tanariyakul,
95 Moo 8, Phaholyothin Road, Tambon Khlong Nung, Amphoe Khlong Luang, 10120, Chang Wat Pathum Thani, Thailand.
E-mail: y.tanariyakul@gmail.com
Abstract
Introduction: The coverage of soft-tissue defects around the knee joint has many reconstructive techniques depending on the size, location, and depth. We report a case with large soft-tissue defect at anterior knee joint that primary closure cannot be done with successfully used distally based sartorius flap and full-thickness skin graft to cover this defect.
Case Report: A 30-year-old man had a large skin defect at the knee following a motorcycle accident. The patella tendon and patella were exposed. We use the sartorius muscle flap to cover the wound defect. First, a skin incision was done on the muscle alignment. Then, the sartorius muscle was dissected, and the proximal set of segmental vessels was identified and ligated. Afterward, the sartorius was moved into subcutaneous tunnel and expanded to provide coverage for the wound defect. Finally, we used the full-thickness skin graft to cover over the muscle flap. The flap and graft were survived. The patient could return to work after 1 month after the operation.
Conclusion: In the case with soft-tissue defects around knee joint, there are many operative techniques. Our case has a large wound at anterior aspect of knee joint. We used the distally based sartorius flap to cover the wound defect. Following the transposition, the sartorius remained viable through out its length, and the patient had full post-operative recovery.
Keywords: Distally based sartorius flap, soft-tissue defect, knee joint.
Introduction
The coverage of soft-tissue defects around the knee joint has many reconstructive techniques depending on the size, location, and depth of the defects. One of which was the sartorius muscle flap which was first used in 1978 to close an exposed knee joint [1]. The sartorius muscle is the longest muscle in the body. It lies superficially in the anterior compartment of thigh and runs from anterior superior iliac spine of the pelvic bone to the anteromedial surface of the uppertibia. It assists iliacus and psoas major to flex the hip joint. The sartorius muscle differences over the other thigh muscle are that the sartorius is supplied by many segmental vessels from the femoral artery which could be considered an advantage [2].
Case Report
A 30-year-old Thai male presented to Thammas at University Hospital with a motorcycle accident. On examination, he has a large 8 cm wound at the anterior aspect of his left knee on the patellar tendon level. A large contusion was presented. Few days later, the wound develops into a necrotic tissue which leads to a debridement being done on the patient. Following the debridement, he lost skin and subcutaneous tissue cover of the knee. A primary suture cannot be done to close the wound due to the nature of the large wound (Fig. 1).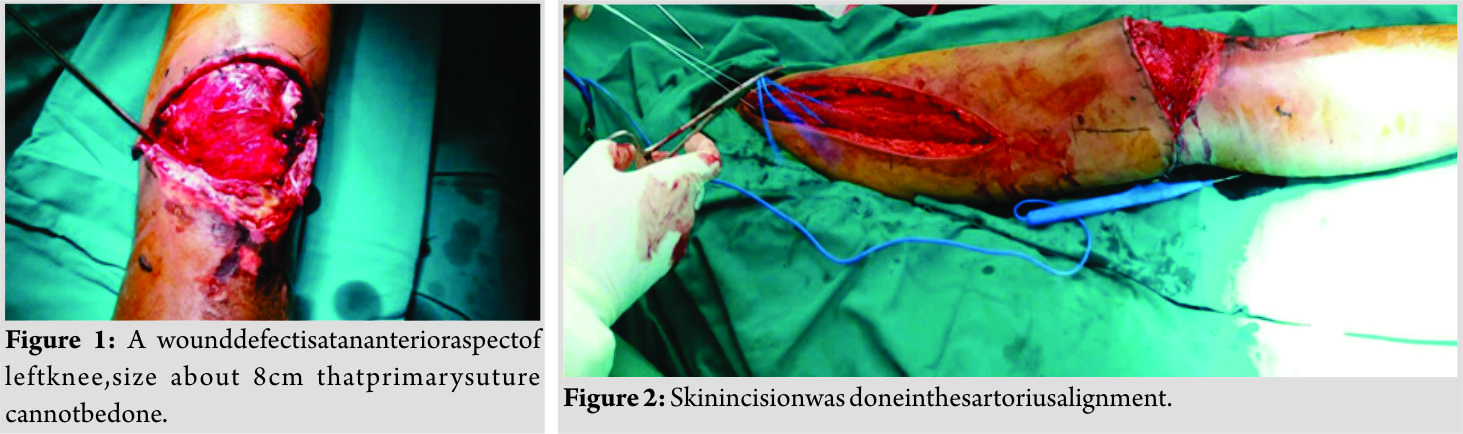 The large vessels, nerves, and muscles remain intact, and the plain film shows no fracture. Because of the location of wound is in the anterior aspect of the knee, we cannot use the gastrocnemius myocutaneous flap. Hence, we use the sartorius muscle flap to cover the wound defect. First, a skin incision was done on the muscle alignment. Then, the sartorius muscle was dissected (Fig. 2 and 3), and the proximal set of segmental vessels was identified and ligated. Afterward, the sartorius was moved into subcutaneous tunnel and used to provide coverage for the wound defect (Fig. 4). Finally, we used the skin graft to cover over the muscle flap (Fig. 5).
The large vessels, nerves, and muscles remain intact, and the plain film shows no fracture. Because of the location of wound is in the anterior aspect of the knee, we cannot use the gastrocnemius myocutaneous flap. Hence, we use the sartorius muscle flap to cover the wound defect. First, a skin incision was done on the muscle alignment. Then, the sartorius muscle was dissected (Fig. 2 and 3), and the proximal set of segmental vessels was identified and ligated. Afterward, the sartorius was moved into subcutaneous tunnel and used to provide coverage for the wound defect (Fig. 4). Finally, we used the skin graft to cover over the muscle flap (Fig. 5). 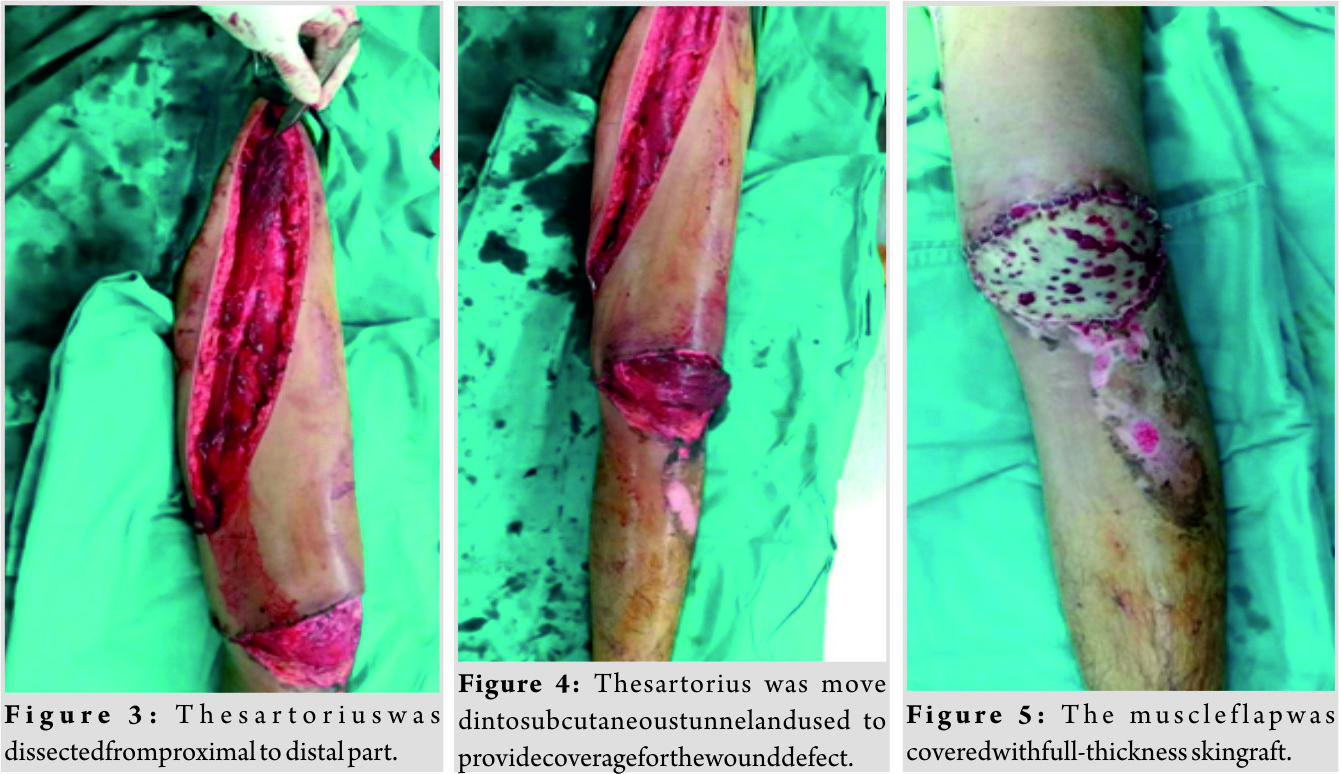 The patient was then followed up at out patient department after surgery. The operation results showed a successful reconstruction without any complications. At 1 year after surgery, his knee healed completely (Fig. 6). He can ambulate with his own legs without any gait aid. The range of motion of the knee is also normal (Fig. 7).
The patient was then followed up at out patient department after surgery. The operation results showed a successful reconstruction without any complications. At 1 year after surgery, his knee healed completely (Fig. 6). He can ambulate with his own legs without any gait aid. The range of motion of the knee is also normal (Fig. 7).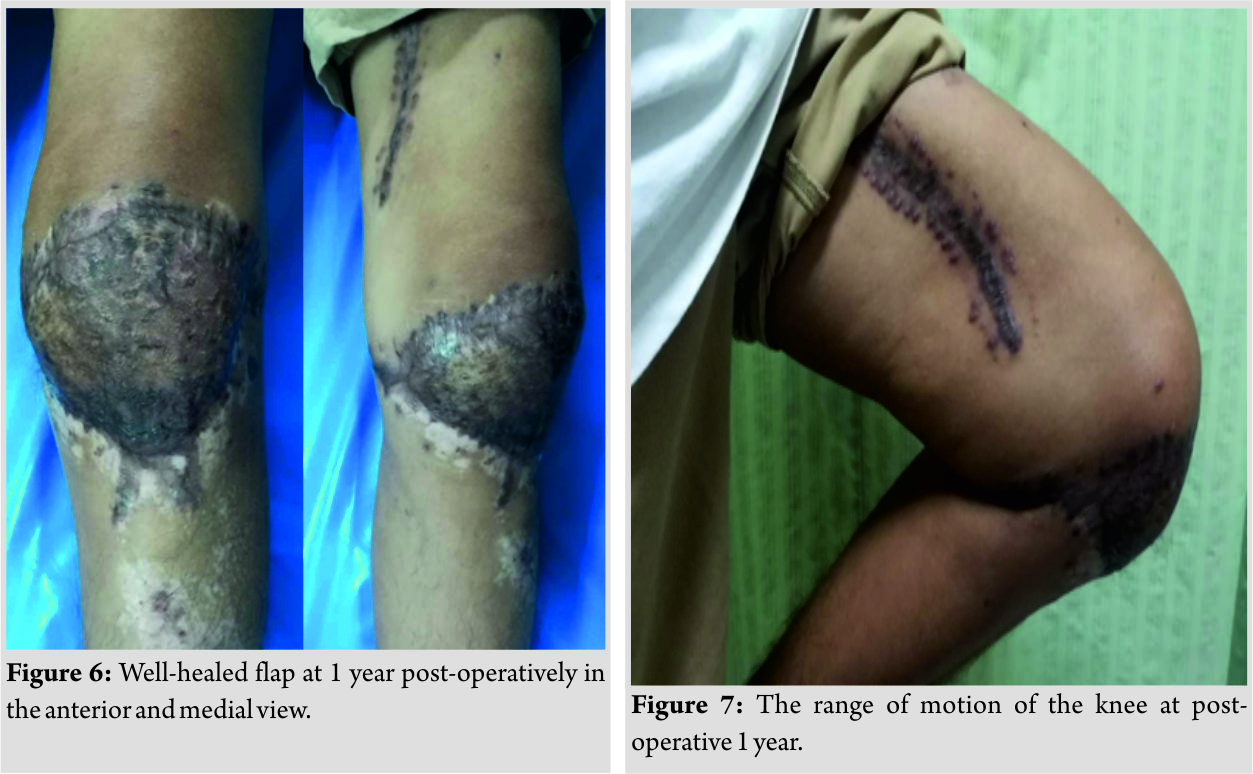
Discussion
Numerous operative methods have been used to reconstruct soft-tissue defects around the knee joint [1, 3, 4]. One of which includes the local fasciocutaneous flap, a regional muscle flap, and free flap transfer. A local flap is simple and has a low risk of flap necrosis [3]. However, it cannot be used to cover a large wound. So instead, the regional sartorius muscle flap was used. With the length of sartorius, we can transpose a flap to cover the wound defect with minimal stress of muscle flap. Furthermore, we use the regional sartorius muscle flap since it is the preferred method when the wound is located at the knee which in this case is located at the medial of the knee [3]. The sartorius is the longest muscle of the body, and it has been used as a reconstructive flap for many regions such as abdominal wall, groin, thigh, and knee [1, 3, 4, 5, 6, 7]. From a study of Clavert et al. about anatomical basis for distal sartorius muscle flap for reconstructive surgery below the knee, the mean muscle length was 52.2 cm and has a rich blood supply from many vascular pedicles that come from the femoral artery [8]. In Mathes and Nahai classification of the vascular anatomy of muscle, sartorius is a Type IV classification [7]. It has 6–10 segmental pedicle arising from the superficial femoral artery [2]. According to previous study, a distal third of the sartorius has a mean mobile length of 5.6 cm. Therefore, the sartorius has greater arc of rotation that easily to rotate a muscle flap to cover the knee joint. In 2014, Gravvanis et al. show knee reconstructive algorithm [3]. For small and deep soft-tissue defect (<4 cm) which is exposed to the patella, bone, or joint, free flap coverage is necessary. A muscle flaps such as sartorius are useful for deep infection because they obliterate the dead space arising from debridement and bring stability to the wound. They suggest to use the sartorius or other distally based thigh muscle flap such as gracilis to cover a suprapatellar infected wound. The difference between this algorithm and our case is the size of wound. For our case, the wound was large (>6 cm) that they suggest to use a free flap such as free anterolateral thigh flap or free latisimus dorsi flap to reconstruct a large, deep, and infected wound. These flaps are useful in large, deep, and infected wound, but they are associated with variable donor site morbidity and need the pre-operative vascular imaging to select the recipient vessel. In some study, the technique of“prefabricated, distally based sartorius muscle flap”was used for coverage the wound around knee joint [4, 6]. This technique improves the viability of cutaneous flap before their transfer. Hong et al. reported two cases with a complex wound at the knee [4]. They used these two-stage procedures to reconstruct a wound, and the result is successful. However, for our case, the wound is simple. Hence, the two-stage procedure is not necessary. Instead, we can use the distally based sartorius flap to cover wound defect and finish it in one operation.
Conclusion
We have reported a case with acute wound injury at the knee following a motorcycle accident. The wound developed from a contusion to a necrotic tissue. The wound was large, and hence, a primary suture cannot be done. We use the distally based sartorius flap to cover the wound defect around the knee. Following the transposition, the sartorius remained viable throughout its length, and the patient had full post-operative recovery.
Clinical Message
The soft-tissue defect at knee joint is one of the complications in traumatic knee injury. There are many operative techniques to reconstruct the defects depending on size, location, depth, and complexity of the wound. The technique using the distally based sartorius flap is one of the most useful treatments to cover a large anterior soft-tissue defect of knee joint.
References
1. Petty CT, Hogue RJ Jr. Closure of an exposed knee joint by use of a sartorius muscle flap: Case report. Plast Reconstr Surg 1978;62:458-61.
2. Mathes SJ, Nahai F. Classification of the vascular anatomy of muscles: Experimental and clinical correlation. Plast Reconstr Surg 1981;67:177-87.
3. Gravvanis A, Kyriakopoulos A, Kateros K, Tsoutsos D. Flap reconstruction of the knee: A review of current concepts and a proposed algorithm. World J Orthop 2014;5:603-13.
4. Hong JP, Lee HB, Chung YK, Kim SW, Tark KC. Coverage of difficult wounds around the knee joint with prefabricated, distally based sartorius muscle flaps. Ann Plast Surg 2003;50:484-90.
5. Khalil IM, Sudarsky L. Sartorius muscle “twist” rotation flap: An answer to flap necrosis. J Vasc Surg 1987;6:93-4.
6. Manushakian HS, Mc Diarmid JG. Reconstruction of a large anterolateral knee defect using a delayed distally based total sartorius flap and a medial gastrocnemius flap. Plast Reconstr Surg 1998;101:1065-9.
7. Apfelberg D, Finseth F. Double-muscle gracilis and sartorius myocutaneous flap. Br J Plast Surg 1981;34:41-3.
8. Clavert P, Cognet JM, Baley S, Stussi D, Prevost P, Babin SR, et al. Anatomical basis for distal sartorius muscle flap for reconstructive surgery below the knee. Anatomical study and case report. J Plast Reconstr Aesthet Surg 2008;61:50-4.
 |
 |
| Dr. Sunyarn Niempoog | Dr. Yot Tanariyakul |
| How to Cite This Article: Niempoog S, Tanariyakul Y. Distally Based Sartorius Flap to Cover Knee Joint Defect. Journal of Orthopaedic Case Reports 2019 May-June; 9(3): 43-45. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




