[box type=”bio”] Learning Point of the Article: [/box]
This article demonstrates the effective management of leg length discrepancy, in melorhostosis, with epiphysiodesis using 8 plates.
Case Report | Volume 9 | Issue 5 | JOCR September – October 2019 | Page 7-10 | Nikolaos A Laliotis, Panagiotis Konstandinidis, Chrysanthos K Chrysanthou, Lizeta Papadopoulou. DOI: 10.13107/jocr.2019.v09i05.1508
Authors: Nikolaos A Laliotis[1], Panagiotis Konstandinidis[1], Chrysanthos K Chrysanthou[1], Lizeta Papadopoulou[1]
[1]Department of Orthopaedics, Interbalkan Medical Center, Thessaloniki- 57001. Greece.
Address of Correspondence:
Dr. Nikolaos A Laliotis,
Sp Lui 5, Thessaloniki – 54622, Greece.
E-mail: nicklaliotis@gmail.com
Abstract
Introduction: Melorheostosis is a rare bone dysplasia. It is mainly a radiographic diagnosis with distinct findings of endosteal or periosteal sclerosis along the axis of long bones, resembling the flowing wax. It is usually polyostotic and monomelic. Clinical manifestations are pain, limitation of joint movements, deformities, and contractures. Leg length discrepancy may be found, usually the affected limb being shorter.
Case Presentation: We present an adolescent boy, with melorheostosis of the lower limb. The affected limb was longer with equally divided discrepancy of the femur and tibia. There were no another symptoms. After a thorough investigation, we performed epiphysiodesis both medial and lateral of the distal femoral and proximal tibial growth plate, using8eight plates. At the end of the growth, there was almost complete equalization of the length of his lower limbs.
Conclusion: Melorheostosis may be present with leg length discrepancy leg length discrepancy, with an exception, being that the affected limb is longer. Epiphysiodesis with eight plates is an effective method of limb length equalization.
Keywords: Melorheostosis, hyperostosis, epiphysiodesis, leg length discrepancy limb length discrepancy LLD.
Introduction
Melhorheostosis is a rare benign sclerosing bone dysplasia. It is described as flowing hyperostosis resembling the flow of wax at the side of a candle. The term is derived from the Greek words melos that means limb, rheos that means flow, and oston that means bone. The disorder begins in childhood. It affects mainly the long bones of the upper or lower limb and is rare in the axial skeleton. Main symptom is pain, contractures, and deformity of the limb. Limb length discrepancy (LLD) has been reported as a clinical sign of the disease [1, 2, 3, 4]. We present a 12-year-s old boy, with melhorheostosis of his right lower limb affecting both femur and tibia. His LLD was equally distributed in the femur and tibia. The affected leg was longer, an exception for the usual presentation of the shorter affected limb. We managed this with epiphysiodesis with eight plates and achieved almost complete equalization for his legs.
Case Report
A healthy 12-year-s old adolescent was referred to evaluate his gait, as it was noticed that there was a painless limp. He was an active athlete in water polo. On examination, it was noticed that he was standing always with his right knee bent and trying to balance his pelvis. On lying with parallel pelvis, his right leg was longer, both femur and knee. A smaller difference in the transverse diameter was noticed, with the right leg also thicker. His feet were equal in length and diameter. There was skin pigmentation in a linear direction along the inner surface of his thigh. There was normal subcutaneous tissue, with no evidence of fibrosis throughout his body. His hip, knee, and ankle joints had full range of movement. There was negative family history for any known musculoskeletal problems.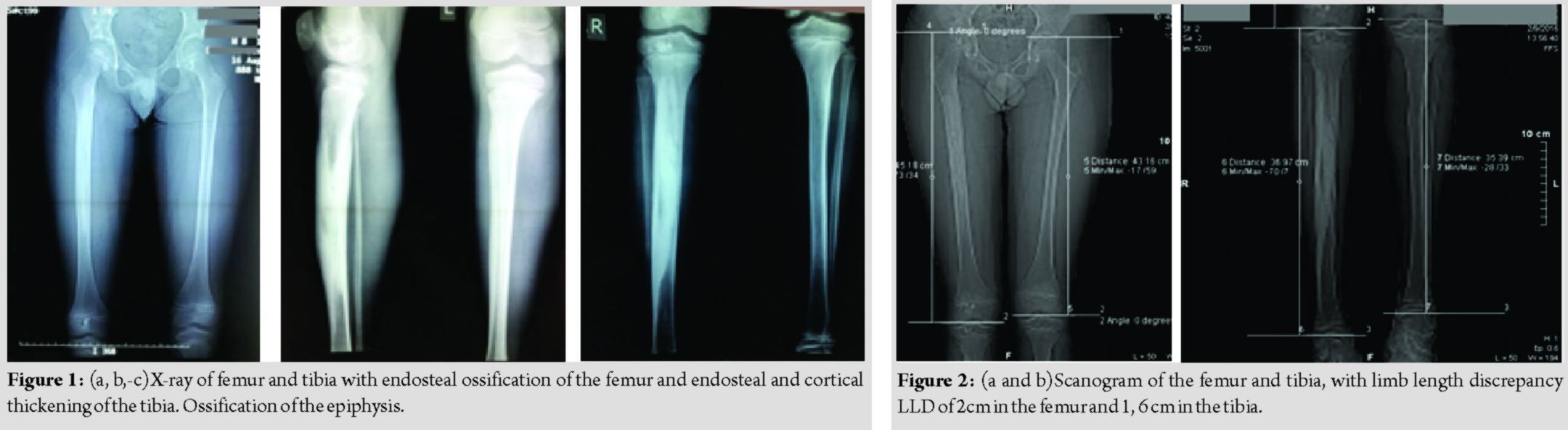
On X-ray examination of his legs, femur and tibia on the right leg had longitudinal diffuse hyperostosis, affecting the medullary canal. There was endosteal and cortical irregular thickening mainly of the tibia. There were irregular areas of ossification in the epiphysis of the femur and tibia. Endosteal ossification was present on the talus of the same foot. Growth plates were open and normal both for femur and tibia. Soft tissue was normal, with no signs of heterotopic ossification. Laboratory investigations including serum alkaline phosphatase, Ca, and P were within normal limits. We performed a scanogram that measured his discrepancy as 2 cm in the femur and 1, 6 cm in the tibia.
Radiological examination of his skull, upper limbs including hands and his spine was normal.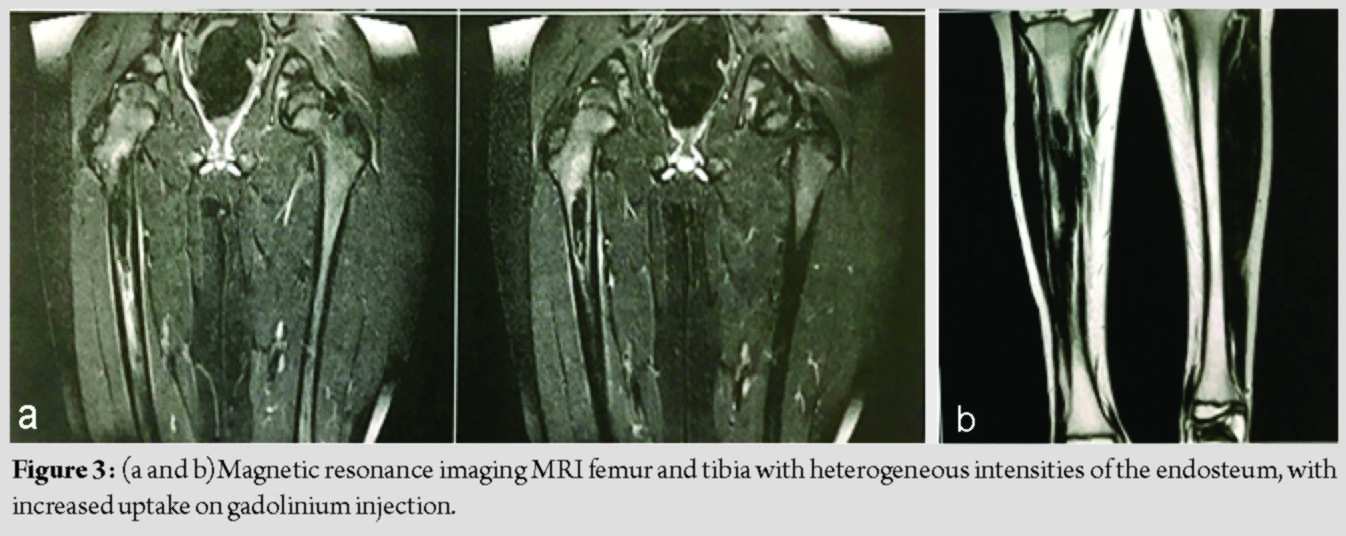
Magnetic resonance imaging (MRI) was performed for the lower limbs. On T1 and T2 images, the areas of ossification appeared as heterogeneous intensities that had uptake on gadolinium. Surrounding soft tissues appeared normal. Technetium-99 bone scan showed increased uptake of the femur and tibia and osteoblastic activity, corresponding to the radiological extension of the hyperostosis.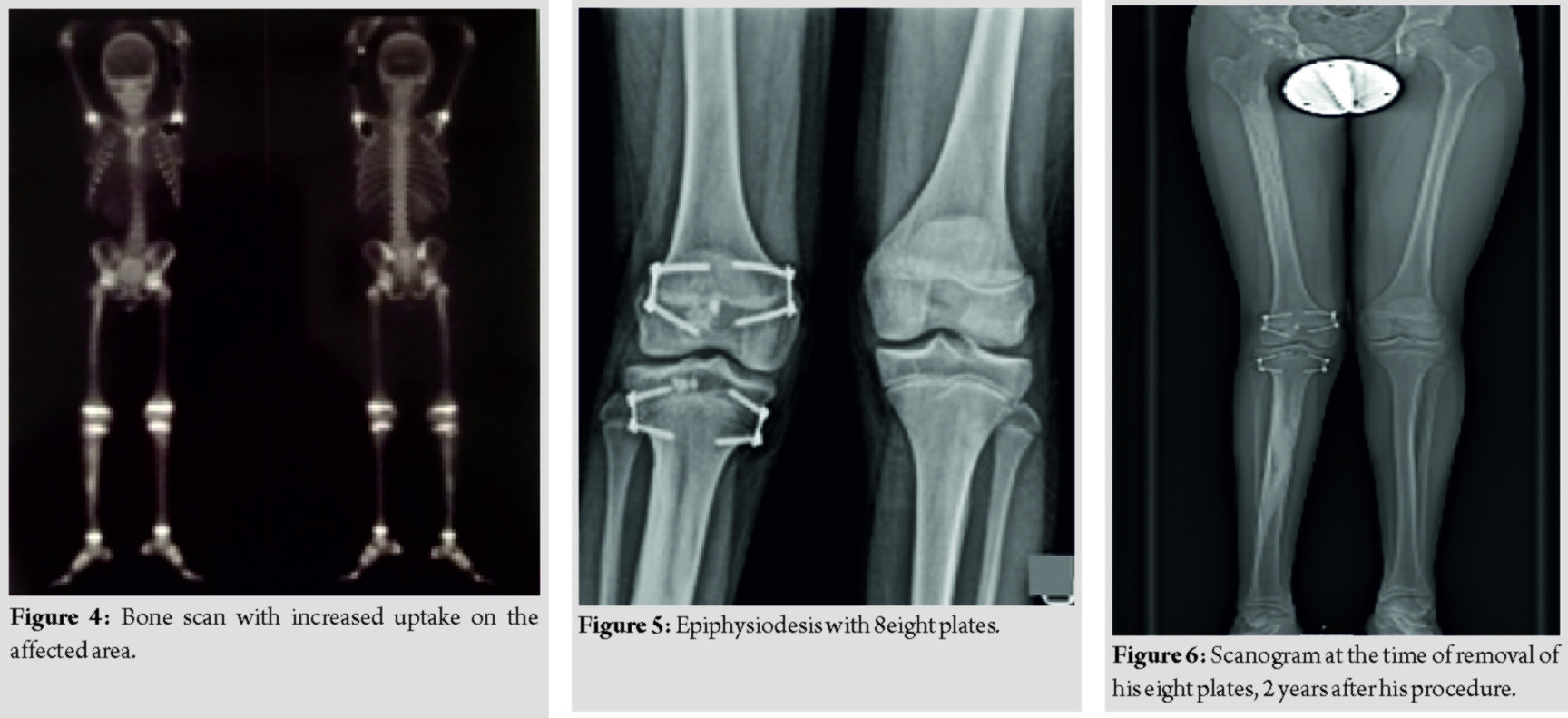
As an initial treatment, shoe raise was provided, in order to reevaluate his discrepancy after one 1 year. His new examination showed a steady length discrepancy. We proceeded in epiphysiodesis, using eight plates on both sides of the growth plate, in the distal femur and proximal tibia. We removed his eight plates with the completion of growth, 2 years after initial surgery, having complete equalization of the femur and 0,8 cm discrepancy of the tibia. The difference in the transverse plane remained the same. Our patient was very satisfied, thankful that we solved his problem of LLD and he could participate easily in all sports activities. His latest X-rays showed that there was no further increase of the hyperostosis. He remains in regular observation.
Discussion
Melorheostosis is a mesodermal bone sclerosing dysplasia. It is a rare condition with an incidence of 0.9 in 1,000,000. Several series have been reported, trying to define this rare entity with unknown etiology. In contrast to other bone dysplasia as osteopetrosis or osteopoikilosis, it is not a hereditary disease, having a sporadic presentation. There is a possible genetic basis with loss of function of LEMD3 gene, but this is not always found [1, 4, 5]. It affects the long bones rather the axial skeleton. Usually, it is a monomelic disease.The lower limbs are more often affected. The skull, spine, ribs, and facial bones are exceptions for been affected. It can be monostotic or polyostotic. Bilateral involvement is rare. In polyostotic cases, ossification may cross the joints.[1, 6, 7]. Melorheostosis is usually diagnosed in childhood, adolescent, or early adult life [1, 2, 8, 9]. It can be an incidental finding in an X-ray examination. Usually, it presents with pain, contractures, and deformity that may be initially confused with arthrogryposis, if they affect the hand or feet [9]. A variety of skin and vascular lesions may be associated. Artner et al. [1] reviewing 313 cases reported the presence of naevi, scleroderma, haemangiomas, and fibrosis. These lesions have usually a sclerotome distribution, similar to the radiological appearance [2]. Our patient had a linear pigmentation area in the inner surface of his thigh, not clearly corresponding in the similar sclerotome as his lesions in the femur and tibia. Melorheostosis is mainly diagnosed from radiographic examination. Freyschmidt [3] has described different radiographic patterns for the disease. He reviewed 23 cases over a 16-year period. The patients reported had a mean age of 34 years (range 7–70 years). In five cases, he describes the classical pattern of cortical thickening with the appearance of flowing wax. In seven cases, there was osteoma-like appearance with endosteal hyperostosis that was eccentrically located. A myositis ossificans pattern with soft tissue ossification around the hip and knee was reported in one patient. An osteopathia striata like pattern was found in six cases, with eccentric dense hyperostosis striatations. He describes also a mixed pattern for four patients. Younge et al. [10] underlined that children have endosteal sclerosis, in contrast to adults with the extraosseous flowing outside the diaphysis of the long bone. They also report mottled and patchy hyperostosis of the pelvis and of small bone of feet and hand. Our patient had characteristic endosteal ossification with the osteoma-like appearance in the femur and tibia and patchy hyperostosis in the talus and the epiphysis of femur and tibia. MRI and computed tomography (CT) scan are helpful as examinations for differentiating diseases with increased bone formation. MRI has low signal intensity in the affected areas that correspond to the areas affected inX-ray. MRI defines non-mineralized soft tissue involvement. CT scan has a clear demarcation of the affected from the normal bone [11, 12]. Bone scan is important to differentiate from other diseases that appear with increased ossification as osteopoikilia and osteopathia striata. These entities are negative on bone scan, but melorheostosis has a positive uptake [13]. Limb length discrepancy (LLD) was found in 49 of 182 cases from Artner et al. (27%). Morris described 35 cases of LLD with similar percentage. The short limb was the affected one and the exception was the elongation of the affected one.[1, 8]. In the series of Smith et al. from Mayo Clinic, in 24 patients, LLD was found in four patients. They report improvement of gait with shoe raiser. They further report good result with epiphysiodesis [2]. In the series of Younge et al. [10], from the records of the North America Shriner’ s Hospital, in their 14 children, LLD was present in all their patients. In 13 of them, the affected limb was shorter and only one of them had longer the affected limb. The discrepancy ranged from 1, 2 to 10 cm with average shortening 4 cm. Marshal and Bradish [14] reported a 27-year-old man with melorheostosis, with shortening of the affected limb of 4 cm that was equally divided into femur and tibia. He was initially diagnosed at the age of 11. They treated him with lengthening of the tibia, with 4 cm elongation, with a monolateral external fixator. The regenerated tibia had the same appearance as the melorheostosis. Since callus formation in lengthening is mainly intramembranous, they conclude that the disorder is an intramembranosous ossification disturbance. No lesion of the growth plate was found both in radiological examination and the MRI, in order to explain the leg length discrepancy of our patient. No vascular malformation was present in our patient. We treated our patient with epiphysiodesis with 8eight plates, since his active growth plate was normal and not affected from the melorheostosis. We achieved an almost complete equalization of the discrepancy. Our patient was very satisfied with the final result. We continue to review our patient, even though melorheostosis has a benign course. No further increase in his radiographic findings is expected.
Conclusion
Melorheostosis is a rare bone dysplasia. Leg length discrepancy can be one clinical manifestation of the disease in children. Diagnosis is based on the appropriate radiographic investigation. X-ray examination and scanogram measurements are used for the monitoring of the LLD. The affected limb in our patient was the longer one. Using eight plates, we performed epiphysiodesis of the distal femur and proximal tibia and achieved almost complete equalization of the LLD.
Clinical Message
Melorheostosis is a rare bone dysplasia that can be presented only with leg length discrepancy. It is an exception the affected limb to be the longer one. Management with epiphysiodesis using eight plates can equalize the LLD.
References
1. Artner J, Cakir B, Wernerus D, Reichel H, Nelitz M. Melorheostosis: Current concepts in diagnosis and treatment a review of literature (313 cases). J Musculoskeletal Res2012;15:1230002-18.
2. Smith GC, Pingree MJ, Freeman LA, Matsumoto JM, Howe BM, Kannas SN, et al. Melorheostosis: A Retrospective clinical analysis of 24 patients at the mayo clinic. PM R 2017;9:283-8.
3. Freyschmidt J. Melorheostosis: A review of 23 cases. Eur Radiol 2001;11:474-9.
4. Kotwal A, Clarke BL. Melorheostosis: A rare sclerosing bone dysplasia. Curr Osteoporos Rep 2017;15:335-42.
5. Kadhim M, Deardorff MA, Dubbs H, Zackai EH, Dormans JP. Melorheostosis: Segmental osteopoikilosis or a separate entity? J Pediatr Orthop 2015;35:e13-7.
6. Elsheikh AA, Pinto RS, Mistry A, Frostick SP. A unique case of melorheostosis presenting with two radiologically distinct lesions in the shoulder. Case Rep Orthop 2017;2017:9307259.
7. John B, Sharma A, Pandey RA. Managing recurrence in intraarticular melorheostosis involving the knee joint: A case report. J Orthop Case Rep 2017;7:29-33.
8. Morris JM, Samilson RL, Corley CL.Melorheostosis. Review of the literature and reportof an interesting case with a 19 year follow-up. J Bone Joint Surg Am. 1963;45:1191-206.
9. Campbell CJ, Papademetriou T, Bonfiglio M. Melorheostosis. A report of the clinical, roentgenographic, and pathological findings in fourteen cases. J Bone Joint Surg Am 1968;50:1281-304.
10. Younge D, Drummond D, Herring J, Cruess RL. Melorheostosis in children. Clinical features and natural history. J Bone Joint Surg Br 1979;61-B:415-8.
11. Sureka B, Mittal MK, Udhaya K, Sinha M, Mittal A, Thukral BB, et al. Melorheostosis: Two atypical cases. Indian J Radiol Imaging 2014;24:192-5.
12. Judkiewicz AM, Murphey MD, Resnik CS, Newberg AH, Temple HT, Smith WS, et al. Advanced imaging of melorheostosis with emphasis on MRI. Skeletal Radiol 2001;30:447-53.
13. Papadakis GZ, Jha S, Bhattacharyya T, Millo C, Tu TW, Bagci U, et al 18F-naF PET/CT in extensive melorheostosis of the axial and appendicular skeleton with soft-tissue involvement. Clin Nucl Med 2017;42:537-9.
14. Marshall JH, Bradish CF. Callotasis in melorheostosis: A case report. J Bone Joint Surg Br 1993;75:155.
 |
 |
| Dr. Nikolaos A Laliotis | Dr. Panagiotis Konstandinidis |
| How to Cite This Article: Laliotis N A, Konstandinidis P, Chrysanthou C K, Papadopoulou L. Melorheostosis in an Adolescent with Limb Length Discrepancy and Management with Epiphysiodesis with Eight Plates. Journal of Orthopaedic Case Reports 2019 Sep-Oct; 9(5): 7-10. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




