[box type=”bio”] Learning Point of the Article: [/box]
Acute compartment syndrome, if not treated in a timely fashion, can have devastating consequences.
Case Report | Volume 10 | Issue 1 | JOCR January – February 2020 | Page 1-3 | Andrew Jimenez, Barton R Branam, Kimberly A Hasselfeld, Kathryn A Hasselfeld. DOI: 10.13107/jocr.2020.v10.i01.1610
Authors: Andrew Jimenez[1], Barton R Branam[1], Kimberly A Hasselfeld[1], Kathryn A Hasselfeld[1]
[1]Department of Orthopaedic Surgery, Division of Sports Medicine, University of Cincinnati College of Medicine, Cincinnati, Ohio.
Address of Correspondence:
Dr. Andrew Jimenez,
Department of Orthopaedic Surgery, Division of Sports Medicine, University of Cincinnati College of Medicine, MSBRoom 5553, 231 Albert Sabin Way, Cincinnati, OH45267-0212.
E-mail: andrew.esteban.jimenez@gmail.com
Abstract
Introduction: Acute following a chronic exertional compartment syndrome (CECS) is a known but uncommonly encountered complication of sports activity and its physiologic profile remains unclear to date. Failure to recognize and promptly treat this condition can lead to disastrous sequelae.
Case Report: We present the case of a 13-year-old lacrosse player with a history of CECS who developed unprovoked acute compartment syndrome. Despite emergent fasciotomy, she experienced intermittent episodes of peroneal nerve deficits. A peroneal nerve neurolysis was later performed which resulted in full resolution of her symptoms.
Conclusion: This case stresses the importance of a high index of suspicion for compartment syndrome which if not treated in a timely fashion can have devastating consequences.
Keywords: Compartment syndrome, exertional compartment syndrome, sports medicine.
Introduction
Compartment syndrome is an orthopedic emergency that is typically associated with trauma. A well-documented but rare form of compartment syndrome is exertional compartment syndrome, which can occur in both acute and chronic forms. The usual clinical course of chronic exertional compartment syndrome (CECS) is pain and at times, neurologic symptoms which are associated with strenuous exercise and relieved by rest [1, 2, 3]. In addition, acute exercise-induced compartment syndrome is similar in presentation, but the symptoms are not relieved by rest and require surgical intervention [4, 5, 6]. We present a case of acute following a case of CECS in a young athlete who later developed peroneal nerve palsy requiring neurolysis.
Case Report
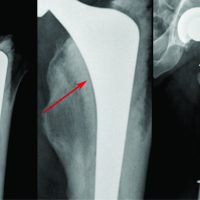
We report the case of an otherwise healthy 13-year-old female lacrosse player who had a remote history of intermittent foot drop associated with pain several years prior. She had undergone extensive workup at that time with X-ray of the knee, which was only significant for osteochondritis dissecans of the lateral femoral condyle, and magnetic resonance imaging (MRI) of the brain, leg, knee and ankle. The MRI revealed no significant findings, including no visible abnormality of the peroneal nerve but did show mild tenosynovitis of the flexor hallucis longus and flexor digitorum longus. It was believed that she suffered from CECS, and she was treated conservatively with foot orthotics and physical therapy. Several years later, she experienced foot drop twice in 6 months which brought her back to the orthopedic office for reevaluation. Physical examination at that time was significant for 3/5 strength with dorsiflexion and 4+/5 strength in her extensor hallucis longus (EHL). In addition, she exhibited hyperesthesia in her deep peroneal nerve distribution and tenderness to palpation throughout her anterior leg musculature. A right lower extremity MRI was performed, which showed no evidence of neuropathy or compressive lesion. She re-presented 2 days later with complaints of severe pain, persistent foot drop and a cool leg in the absence of a clear etiology. At that time, she was sent to the emergency room for evaluation of acute compartment syndrome. In the emergency department, compartment pressures were measured with a Hand-Held Stryker compartment monitor (Stryker, Kalamazoo, Michigan). Compartment pressures were 51 mm Hg in the anterior compartment and 45 mm Hg in the lateral compartment. She was promptly taken to the operating room for an anterior and lateral compartment fasciotomy and a muscle biopsy of the anterior compartment. Intraoperatively, she was found to have thick fascia, but no other abnormalities were noted. In the post-anesthesia care unit, she had improvement in her foot dorsiflexion and EHL strength. The muscle biopsy returned as normal and she had complete resolution of her symptoms on her post-operative visit 8 days later.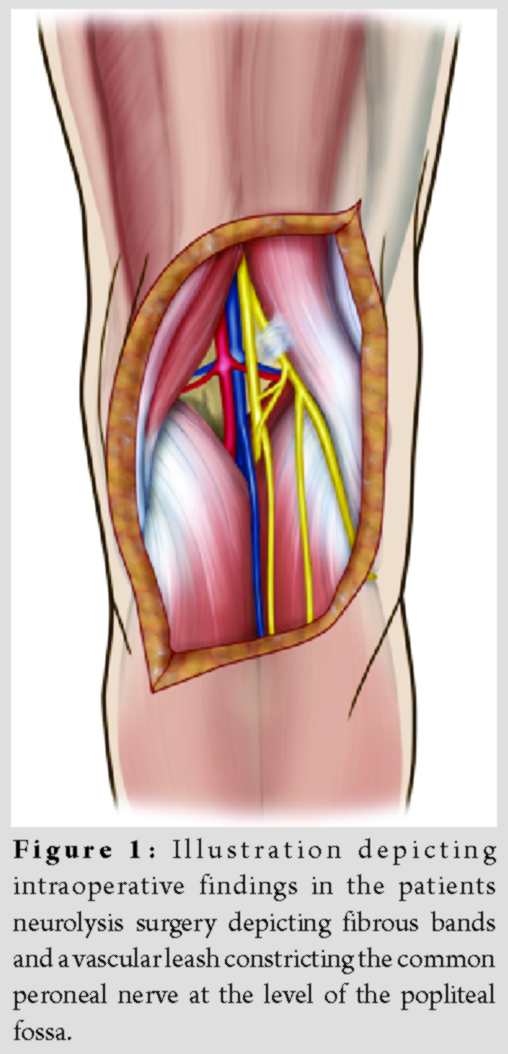
At a 5-month post-operative follow-up, she complained of recent onset of numbness and tingling in her superficial and deep peroneal nerve distributions. On physical exam, she had a positive Tinel’s sign over her common peroneal nerve at the fibular head. MRI was negative for pathology, but electromyography revealed slowed conduction velocity of the peroneal nerve across the fibular head. It was decided to proceed with neurolysis and exploration of her peroneal nerve. Intraoperatively, fibrous constricting bands and a vascular leash were discovered around her peroneal nerve in the popliteal fossa (Fig. 1). The nerve was freed from any points of tethering in a 12 cm window from the fibular head to the popliteal fossa. Immediately postoperatively, the patient showed no evidence of peroneal nerve palsy with full dorsiflexion and eversion of the foot. She has been recently seen for follow-up 5 years postoperatively, and she is symptom-free with full strength and no neurologic symptoms. She has experienced excellent recovery and she is playing Division I varsity collegiate lacrosse as a senior in college.
Discussion
Compartment syndrome is a dangerous and potentially disastrous condition. Increased pressures in the compartment overcome capillary perfusion pressure that can lead to permanent disability and muscle ischemia. It can easily be missed in a young athlete due to its rarity and the characteristic pain can be delayed by several hours after exercise [7, 8]. The diagnosis of compartment syndrome mainly relies on clinical assessment. Most notably pain out of proportion to injury is an early finding concerning compartment syndrome. If there is high clinical suspicion, intra-compartmental pressure can be measured to confirm the diagnosis. Other features that occur if left untreated include paresthesia, pallor, pulselessness, and paresis. As in our case, the diagnosis of compartment syndrome can be confirmed with intra-compartmental pressures. Normal pressures range from 0 mm Hg to 15 mm Hg, and in general, fasciotomy is recommended for pressures >30 mm Hg [9]. Several studies have illustrated the possibility of progression of CECS to its acute form [6, 10]. Unlike CECS, acute compartment syndrome (ACS) is unrelieved by rest and causes severe unrelenting pain. It generally occurs after intense, prolonged exercise but it may occur without a clear inciting event [11]. It has been proposed that acute following a chronic compartment syndrome may have a unique course where pressures build slowly initially with a sudden increase in pressures later[12]. There has been no definitively established mechanism for acute exercise-induced compartment syndrome, but the increased pressures are likely secondary to muscle hypertrophy and fluid accumulation [13]. In this case, the patient developed ACS due to an unknown etiology. Interestingly, in our case, it is likely that her clinical picture was further complicated by the presence of compressing fascial bands and a vascular leash around her peroneal nerve. Of note, Soffer et al. [14] have described a case of chronic compartment syndrome caused by aberrant fascial bands which compressed the anterior compartment of her leg. Our patient was noted to have particularly thick fascia intraoperatively during her fasciotomy; however, no compressing fascial band was noted.
Surgical intervention is critical for these patients in the management of acute compartment syndrome. Timely diagnosis and treatment are of the utmost importance as well. Several studies have shown the relationship between increased duration and pressures with increasing debilitation. Of note only 8% of patients regain full function when delay of fasciotomy is delayed over 12 h[15]. Matsen et al. [16] demonstrated that irreversible damage to nervous tissue could occur after 6–12 h of elevated compartment pressures.
Conclusion
Our patient had experienced symptoms of foot drop but had complete resolution of these symptoms after surgical intervention, which is attributable to a timely diagnosis and surgical treatment. A unique aspect of this case is that our patient presented to the clinic 5 months after her anterior and lateral compartment release with recurrent numbness and tingling in her peroneal nerve distribution. It is likely that the initial neurologic symptoms experienced by our patient were a combination of both her increased compartment pressures with concomitant compression of her peroneal nerve by constricting fascial bands and vascular leash. In addition, this patient presented with an unprovoked case of acute compartment syndrome independent of exercise, which is atypical in the setting of CECS.
Clinical Message
Timely treatment of acute compartment syndrome is of the utmost importance given its potentially devastating consequences. A high clinical suspicion must be maintained even in atypical presentations.
References
1. Abramowitz AJ, Schepsis AA. Chronic exertional compartment syndrome of the lower leg. Orthop Rev1994;23:219-25.
2. Hutchinson MR, Ireland ML. Common compartment syndromes in athletes. Treatment and rehabilitation. Sports Med1994;17:200-8.
3. Klodell CT, Pokorny R, Carrillo EH, Heniford BT. Exercise-induced compartment syndrome: Case report. Am Surg1996;62:469-71.
4. Brodsky M, Bongiovanni MS. Bilateral lower leg acute exertional compartment syndrome. Orthopedics2000;23:607-9.
5. Fehlandt A, Micheli L. Acute exertional anterior compartment syndrome in an adolescent female. Med Sci Sports Exerc1995;27:3-7.
6. Leach RE, Hammond G, Stryker WS. Anterior tibial compartment syndrome. Acute and chronic. J Bone Joint Surg Am1967;49:451-62.
7. McHale KM, Prahinski JR. Acute exertional compartment syndrome occurring after performance of the army physical fitness test. Orthop Rev1994;23:749-53.
8. Willy C, Becker HP, Evers B, Gerngross H. Unusual development of acute exertional compartment syndrome due to delayed diagnosis. A case report. Int J Sports Med1996;17:458-61.
9. Bourne RB, Rorabeck CH. Compartment syndromes of the lower leg. Clin OrthopRelat Res1989;240:97-104.
10. Reneman RS. The anterior and the lateral compartmental syndrome of the leg due to intensive use of muscles. Clin OrthopRelat Res1975;113:69-80.
11. Stollsteimer GT, Shelton WR. Acute atraumatic compartment syndrome in an athlete: A case report. J Athl Train1997;32:248-50.
12. Esmail AN, Flynn JM, Ganley TJ, Pill SG, Harnly H. Acute exercise-induced compartment syndrome in the anterior leg. A case report. Am J Sports Med2001;29:509-12.
13. Rorabeck CH, Macnab I. The pathophysiology of the anterior tibial compartmental syndrome. Clin OrthopRelat Res1975;113:52-7.
14. Soffer SR, Martin DF, Stanish WD, Michael RH. Chronic compartment syndrome caused by aberrant fascia in an aerobic walker. Med Sci Sports Exerc1991;23:304-6.
15. Sheridan GW, Matsen FA. Fasciotomy in the treatment of the acute compartment syndrome. J Bone Joint Surg Am1976;58:112-5.
16. Matsen FA, Winquist RA, Krugmire RB. Diagnosis and management of compartmental syndromes. J Bone Joint Surg Am1980;62:286-91.
 |
 |
 |
 |
| Dr. Andrew Jimenez | Dr. Barton R Branam | Mrs. Kimberly A Hasselfeld | Dr. Kathryn A Hasselfeld |
| How to Cite This Article: Jimenez A, Branam B R, Hasselfeld K A, Hasselfeld K A. A Case Report of a Case of Acute Exertional Compartment Syndrome with Peroneal Nerve Palsy in an Adolescent Athlete. Journal of Orthopaedic Case Reports 2020 Jan-Feb;10(1): 1-3. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com