[box type=”bio”] Learning Point of the Article: [/box]
A dual plating technique is a reliable and easily reproducible technique in the treatment of a fracture in a long-term ankylosed hip.
Case Report | Volume 10 | Issue 1 | JOCR January – February 2020 | Page 8-10 | Tiago Pato, Filipe Sá Malheiro, Domingos Estrela, José Brenha. DOI: 10.13107/jocr.2020.v10.i01.1614
Authors: Tiago Pato[1], Filipe Sá Malheiro[1], Domingos Estrela[1], José Brenha[1]
[1]Department of Orthopaedics, Centro Hospitalar Baixo Vouga, Avenida Doutor Artur Ravara 3810-193, Aveiro, Portugal.
Address of Correspondence:
Dr. Tiago Pato,
Department of Orthopaedics, Centro Hospitalar Baixo Vouga, Avenida Doutor Artur Ravara 3810-193, Aveiro, Portugal.
E-mail: eutiagopato@gmail.com
Abstract
Introduction: The main objectives in the treatment of an intertrochanteric fracture in elderly population are to prevent medical complications, maintain mobility, independence, and relieve pain. When this fracture occurs in an arthrodesed hip, there is a significant lack of scientific evidence of optimal treatment and clinical results since only few case reports have been published so far.
Case Report: A Caucasian 83-year-old woman slipped and fell, complaining of the left hip pain. After radiographic evaluation, she was diagnosed with an intertrochanteric fracture that occurred in a long-term arthrodesed hip. We treated this rare presentation by open reduction and internal fixation with a proximal locking femoral plate and a pelvic reconstruction plate. No immobilization was needed in the post-operative care. Fracture healing occurred after 3 months.
Conclusion: Without motion on the hip, the lower extremity forms one long lever arm, creating an unusual instability at the fracture site. The authors decided that, to overcome this situation, the construction had to be reinforced and extended from the iliac wing to the proximal femur with two plates. This provided enough strength and stability to allow an uneventful fracture healing. This approach can be easily reproduced and can be considered in future similar patients.
Keywords: Ankylosed hip, hip arthrodesis, intertrochanteric fracture, open reduction, internal fixation.
Introduction
Intertrochanteric fractures are an important cause of morbidity and mortality, and its incidence is increasing as the population grows older. However, the occurrence of a trochanteric fracture in a long-term ankylosed hip is a very rare complication. There are only isolated cases published in literature, reflecting the diminished clinical experience, and absence of recommended treatment. These isolated cases of proximal femoral fractures are divided into two neck fractures [1, 2] and five trochanteric fractures [3, 4, 5, 6, 7], and in each case, the surgeons opted for a different surgical approach: Dynamic hip screw (DHS®) and cannulated screws, which were later converted into a total hip arthroplasty (THA) [2];reconstruction plates [6]; plating and cannulated screws [3]; costume made plating [4]; proximal femoral locking plate (PFLP) [7]; Gamma nail® [5]; and supracondylar intramedullary locked nail [1]. With this case, the authors present a different and viable approach to a rare fracture presentation, which can be easily reproduced and therefore considered in similar cases.
Case Report
An 83-year-old woman slipped and fell, complaining of the left hip pain and was unable to bear weight. She referred she was submitted to a hip arthrodesis 53 years ago, after an undiagnosed congenital hip dislocation. She also suffered from poliomyelitis and walked around with a cane. The radiographic and tomographic evaluation showed an intertrochanteric fracture in a long-lasting ankylosed hip (Fig. 1 and 2). 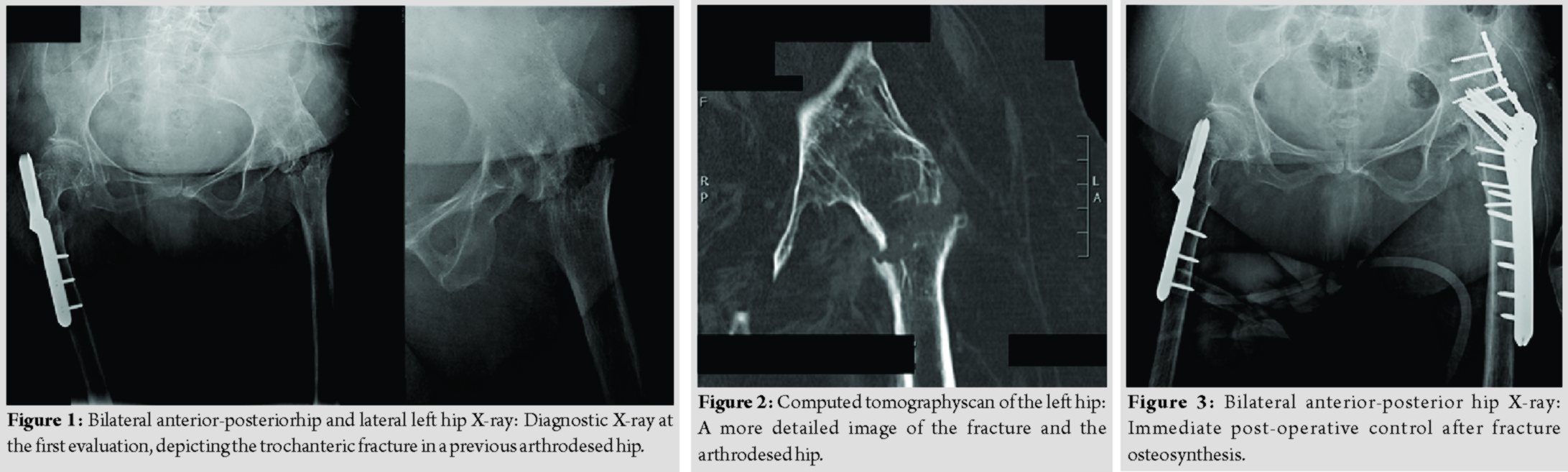 After carefully assessing scientific evidence and discussing the appropriate treatment strategy, the patient was prepared for surgery. She was positioned in lateral decubitus and a lateral approach was used, centered on the great trochanter. The fracture was exposed and fixated with two plates. One proximal locking femoral plate, with 6mm×4.5 mm cortical and 4mm×6.5 mm cannulated screws, was applied to the head and proximal femur. Expecting a great stress in the fracture site, this construction was reinforced with a 3.5 mm pelvic reconstruction plate, with 8mm×3.5 mm cortical screws, spanning from the iliac wing to the proximal femur (Fig. 3 and 4). Due to the poor bone quality and the unusual long lever arm, the patient was not permitted to walk until 3 weeks after the intervention (Fig. 5) and only partial weight-bearing afterward. Bone healing occurred after 3 months, allowing the patient to walk with a single cane and full weight-bearing (Fig. 6).
After carefully assessing scientific evidence and discussing the appropriate treatment strategy, the patient was prepared for surgery. She was positioned in lateral decubitus and a lateral approach was used, centered on the great trochanter. The fracture was exposed and fixated with two plates. One proximal locking femoral plate, with 6mm×4.5 mm cortical and 4mm×6.5 mm cannulated screws, was applied to the head and proximal femur. Expecting a great stress in the fracture site, this construction was reinforced with a 3.5 mm pelvic reconstruction plate, with 8mm×3.5 mm cortical screws, spanning from the iliac wing to the proximal femur (Fig. 3 and 4). Due to the poor bone quality and the unusual long lever arm, the patient was not permitted to walk until 3 weeks after the intervention (Fig. 5) and only partial weight-bearing afterward. Bone healing occurred after 3 months, allowing the patient to walk with a single cane and full weight-bearing (Fig. 6).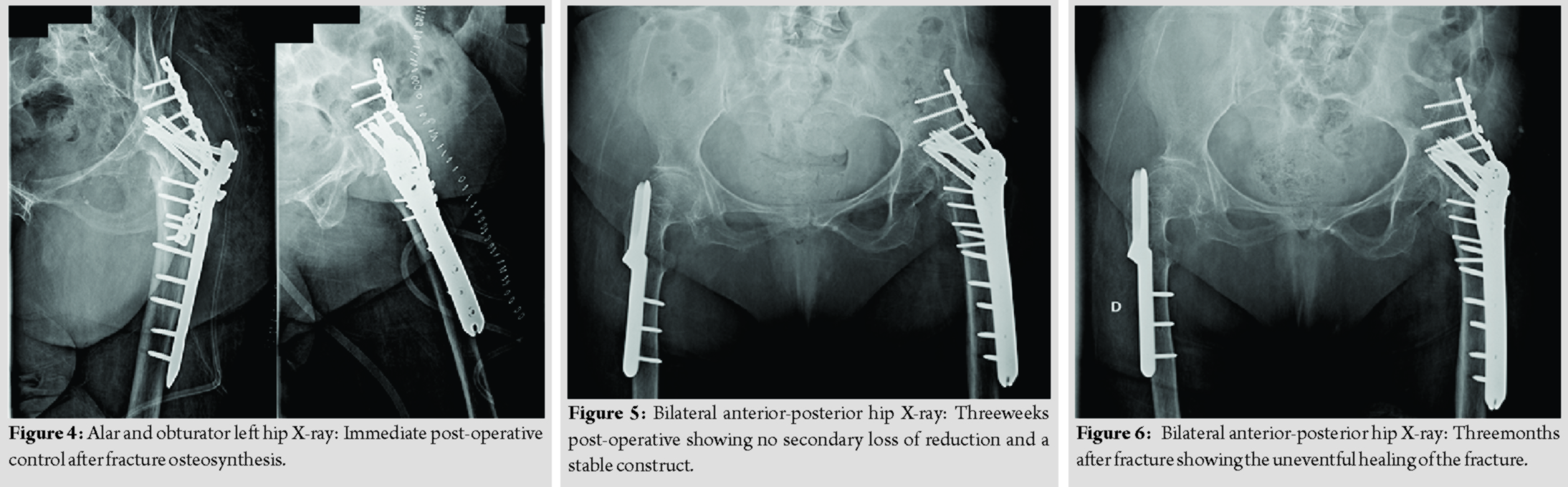
Discussion
When presented with a common proximal femoral fracture, we can consider the femoral head as one unit and the trochanteric area as another. This means that when we fix it, the disruption forces will be between the head and proximal femur. In the case presented here, this is not true. Since the hip is fused, the left hemipelvis works with the femur as a single unit. After the fracture, the left hemipelvis together the femoral head will be the proximal component of the fracture. In this scenario, the lever arm and stress generated at the fracture site are higher than in the common trochanteric fractures. Having this in mind, the authors assumed that it could not be fixed in the usual way. With the typical components – DHS®, nail, and PFLP – the fixation would be between the proximal femur and the femoral head. Therefore, since the left hemipelvis and femoral head act as a single unit, most of the proximal fracture component would not be fixed and stabilized into the construction. The long lever arm would impose a huge stress into the construction, making it likely to fail. To overcome this problem, the authors decided to reinforce and extend the construction from the iliac wing to the proximal femur. This was accomplished by adding an extrapelvic reconstruction plate to the proximal locking femoral plate (Fig. 3 and 4). The authors also discussed the conversion to a THA as a possible treatment. Although technically demanding, this approach is possible. Nevertheless, some key points were taken into consideration: Reports of conversions to a THA are usually worse than primary THA due to osteonecrosis; the poor quality of abductor musculature after 53 years of the hip fusion; the patient age; and her expectations. Therefore, despite providing the patient with a long-lost hip mobility, the conversion was not considered a viable option for this case.
Conclusion
There are very few cases reported in literature about fractures involving an ankylosed hip. There is no optimal treatment established for these situations, and as mentioned before, each surgeon had a different approach and choice of implants, with its pros and cons. In this report, the authors considered the left hemipelvis and femoral head as one unit, therefore, creating a long lever arm and submitting the fracture site to a huge stress, which implies that the fixation must be strong enough to overcome it. Conversion to a THA was possible, although technically demanding and with worse results than primary hip replacement. In this situation, this approach was excluded due to the age of the patient and the low quality of the abductor musculature. Using two plates into the construction, spanning from the hemipelvis to the proximal femur, the authors provided enough strength and stability to overcome the unusual long lever arm and allowed the fracture to heal uneventful after 3months. With this case, it is presented a different and viable approach to a rare fracture presentation, which can be easily reproduced and can be considered in similar patients.
Clinical Message
When treating a fracture in an ankylosed hip, we believe that it is crucial to consider the unusual long lever arm and thus increased stress and instability at the fracture site. The type of fixation chosen must be strong enough to withstand these forces while providing enough stability for the fracture to heal uneventful.
References
1. Wulke AP, Mader K, Pennig D. Femoral neck fracture in an arthrodesed hip treated by a supracondylar intramedullary locked nail. J Orthop Trauma 2004;18:116-8.
2. Jones LD, Hampton R, Ansari A. A treatment option for femoral neck fractures complicating hip arthrodesis: Conversion to a constrained total hip replacement. Eur J Orthop Surg Traumatol2007;17:203-5.
3. Darwish FM, Haddad W. Intertrochanteric fracture under an arthrodesed hip. Am J Case Rep 2013;14:150-2.
4. Fang C, Fang B, Wong TM, Lau TW, Pun T, Leung F, et al. Fixing a fractured arthrodesed hip with rapid prototype templating and minimal invasive plate osteosynthesis. Trauma Case Rep 2015;1:79-83.
5. Ishimaru D, Nozawa S, Maeda M, Shimizu K. Intertrochanteric fracture of the ankylosed hip joint treated by a gamma nail: A case report. Case Rep Orthop2012;2012:278156.
6. Manzotti A, Confalonieri N, Pullen C. Intertrochanteric fracture of an arthrodesed hip. J Bone Joint Surg Br 2007;89:390-2.
7. Deleanu B, Prejbeanu R, Vermesan D, Haragus H, Honcea L, Mioc ML, et al. Trochanteric fracture following hip arthrodesis: Case presentation. Clin Case Rep 2018;6:162-4.
 |
 |
 |
 |
| Dr. Tiago Pato | Dr. Filipe Sá Malheiro | Dr. Domingos Estrela | Dr. José Brenha |
| How to Cite This Article: Pato T, Malheiro FS, Estrela D, Brenha J. Intertrochanteric Fracture in a Long-term Ankylosed Hip: A Case Report. Journal of Orthopaedic Case Reports 2020 Jan-Feb;10(1): 8-10. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




