[box type=”bio”] Learning Point of the Article: [/box]
Radiation-induced wound infection in operated soft tissue sarcoma beds present extremely challenging scenarios, which can be managed successfully by a multidisciplinary team (orthopedic surgeon specialist in soft tissue infections, plastic surgeon, microbiologist, infectious disease specialist, radiation and orthopedic oncologist)by following the principles of aggressive debridement, judicious use of NPWT, appropriate antibiotics, and soft tissue cover.
Case Report | Volume 10 | Issue 1 | JOCR January – February 2020 | Page 30-34 | Yash Wagh, Aditya Menon, Bimal Mody, Vikas M Agashe, Manish Agarwal. DOI: 10.13107/jocr.2020.v10.i01.1626
Authors: Yash Wagh[1], Aditya Menon[1], Bimal Mody[1], Vikas M Agashe[1],[2], Manish Agarwal[1]
[1]Department of Orthopedics, PD Hinduja Hospital and Medical Research Centre, Mahim, Mumbai, Maharashtra, India,
[2]Department of Orthopedics, Agashe’s Maternity and Surgical Nursing Home, Mumbai, Maharashtra, India.
Address of Correspondence:
Dr. Aditya Menon,
Department of Orthopaedics, PD Hinduja Hospital and MRC, Veer Savarkar Marg, Mahim (West), Mumbai-400016, Maharashtra, India.
E-mail: docmenon83@gmail.com
Abstract
Introduction: The standard modality for the treatment of soft tissue sarcomas is a wide excision followed by radiation therapy either in the form of external beam radiation or brachytherapy. Radiation therapy thus is an integral part of management and limb salvage in these cases. This, however, subjects the irradiated tissue to a greater risk for necrosis and local infection. This study suggests a protocol to manage these infections. A multimodal approach to these problems is important. Studies have shown that the use of negative pressure wound therapy (NPWT) in non-healing wounds significantly reduces edema by removing excessive fluid from the wound bed as well as facilitating removal of the infective pathogen after an aggressive wound debridement. The author has judiciously used NPWT in each of these patients with encouraging results. With no well-defined guidelines to manage radiation-induced wound infections, this retrospective study gives an overview and protocol for a systematic approach.
Case Report: This is a retrospective series of five cases managed between January 2014 and December 2016. All were men with a mean age of 30.6 years with a mean follow-up of 27 months. We analyzed their demographic, clinical data, history, wound locations, primary diagnosis on histopathology, organisms isolated on culture, surgical details, antibiotics administered, and special interventions such as skin flaps or grafting and clinical outcome.
Of the five, three patients received exclusive external beam radiation therapy (EBRT) and two were given intralesional brachytherapy and EBRT. Three received additional chemotherapy. 7/9 isolated organisms were multidrug-resistant mean 5.4 cycles of NPWT after aggressive debridement was needed to achieve healthy granulation tissue bed. Wounds were closed at median 31.5 days (three split-thickness split skin grafting, one local rotation flap, and one healing with secondary intention). We had two mortalities secondary to metastasis.
Conclusion: We recommend aggressive debridement, prolonged use of NPWT in infected irradiated wounds, and appropriate antibiotics with soft tissue cover by a multidisciplinary team to achieve good results.
Keywords: Radiation, infection, negative pressure wound therapy.
Introduction
The standard modality for the treatment of soft tissue sarcomas is a wide excision followed by radiation therapy either in the form of external beam radiation or brachytherapy. Radiation therapy, thus, is an integral part of management and limb salvage in these cases [1]. This, however, subjects the irradiated tissue to a greater risk for necrosis and local infection [2]. Radiation therapy works primarily on the principle of delivering high-dose linear energy to the tumor cells, thereby inducing DNA damage [3]. Recent studies have shown that targeted radiation therapy not only damages tumor cells but also causes loss of normal peripheral and distant tissues as well; Suzuki and Yamashita have described this as the “bystander effect” of radiation therapy [4]. External beam radiation therapy (EBRT) is a method that delivers high-energy rays to tumors, using a special X-ray machine called a linear accelerator. This machine allows concentrated radiation beams to be delivered from any angle and shapes radiation beams to the contour of the tumor. The machine moves around the body without touching the patient and aims radiation at the sarcoma or desired bed. Even with the advancement of intensity-modulated radiation therapy, radiation-induced skin damage is a common problem. High-dose-rate brachytherapy is a type of internal radiation therapy that delivers radiation from implants placed close to, or inside, the tumor(s) in the body. This technique ensures that maximum radiation dose is given to tumor cells and tissues, while minimizing exposure to the surrounding healthy tissue. Hollow catheters with pellets are temporarily inserted directly into an excised tumor bed to provide optimum delivery of radiation dosage. Brachytherapy is usually started 5 days post-surgery compared to external beam radiation therapy that is given 4 weeks after surgery [5]. Brachytherapy renders the tissue bed relatively avascular. Moreover, post-operative chemotherapy compounds the problem of wound healing by suppressing the patient immunity. These factors increase the risk of infection and make the wounds resistant to standard modalities of treatment. A multimodal approach to these problems is important. A team consisting of orthopedic surgeon specialized in soft tissue infections, medical, radiation and orthopedic oncologist, plastic surgeon, microbiologist, and infectious disease specialist is essential. Studies have shown that the use of negative pressure wound therapy (NPWT) in non-healing wounds significantly reduces edema by removing excessive fluid from the wound bed as well as facilitating removal of the infective pathogen after an aggressive wound debridement [6]. NPWT causes macro- and microdeformation of the wound bed, increases lymphatic outflow, causes neoangiogenesis, and thus enhances wound healing. The author has judiciously used NPWT in each of these patients with encouraging results. With no well-defined guidelines to manage radiation-induced wound infections, this retrospective study gives an overview and protocol for a systematic approach.
Case Report
We have retrospectively analyzed five patients who underwent excision of soft tissue sarcomas at a tertiary care center in Mumbai and developed surgical site infection with perioperative radiation therapy between January 2014 and December 2016.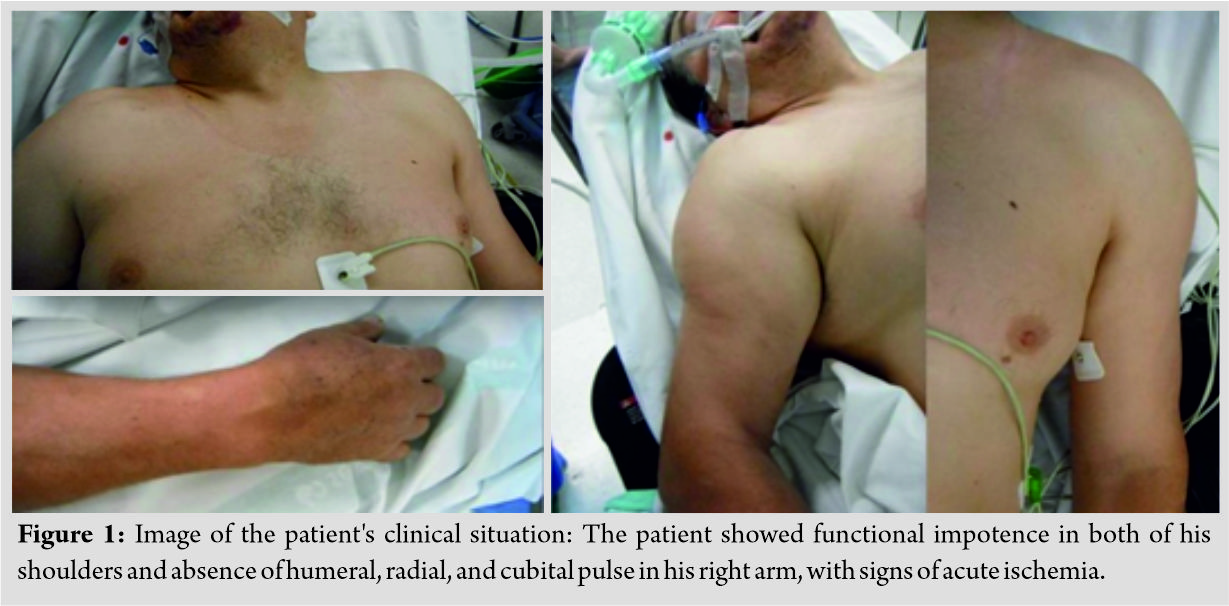
All were men with a mean age of 30.6 years (18–44) and a mean follow-up of 27 months (3–45). We analyzed their demographic, clinical data, history, wound locations, primary diagnosis on histopathology, organisms isolated on culture, surgical details, antibiotics administered, and special interventions such as skin flaps or grafting and clinical outcome.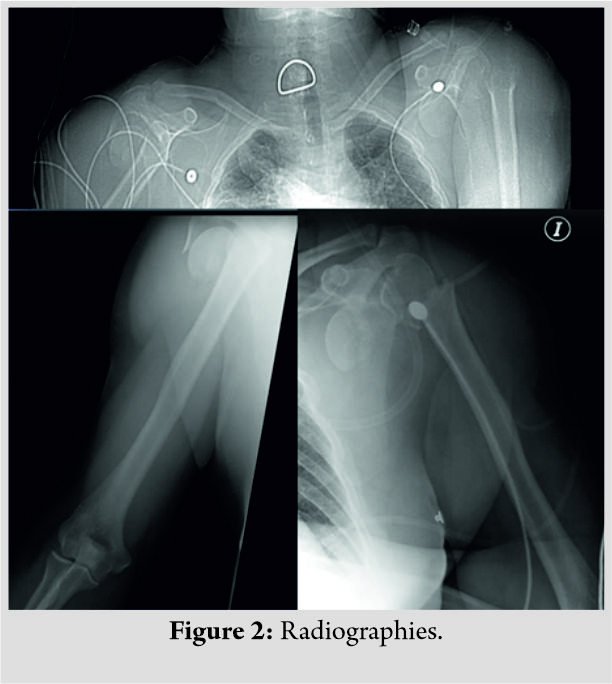
Of the five patients included in the study, three patients had primary tumors in the lower extremities, one patient was operated for a tumor in the iliac crest region, and one had a tumor in the inguinal region.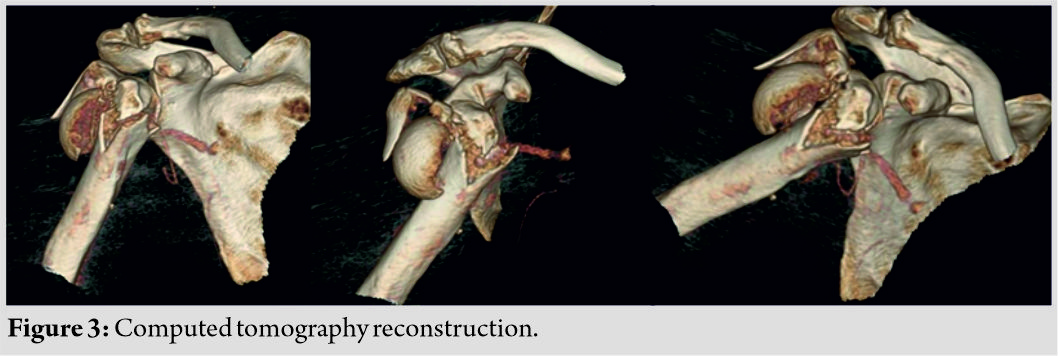
All the patients had histopathology-proven malignant soft tissue tumors (three leiomyosarcomas, one synovial sarcoma, and one pleomorphic sarcoma) for which they underwent wide excision.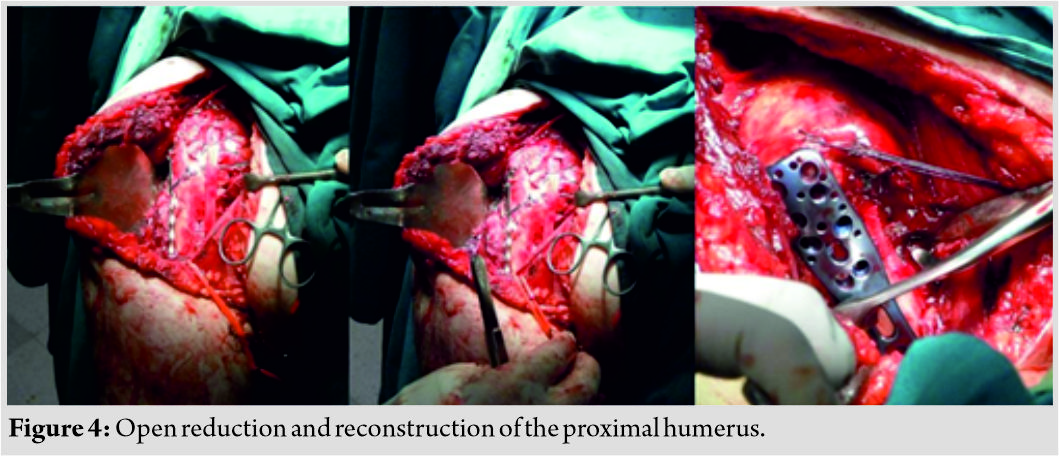
Three patients received exclusive external beam radiotherapy while two were given intralesional brachytherapy and radiation therapy. Three patients received chemotherapy post-surgery. Patients presented with wound infections at a mean 3 months after the primary surgery. Following aggressive debridement, a total of nine organisms were isolated from deep tissue samples with polymicrobial infections in 4/5 (Table 1). Mixed Gram-positive and negative infections were seen in 3/5. Seven of these nine isolates were multidrug resistant (Table 2). Appropriate antibiotics were administered by the infectious disease specialist. A mean 5.4 cycles of NPWT were needed to achieve a bed of healthy granulation tissue. A negative pressure of 125 mmHg at high intensity in continuous mode was used in all cases except one where the femoral vessels were exposed in the wound bed. The pressure was −25 and −50 mmHg in this patient to reduce the chances of vessel blowout. Three required split-thickness split skin grafting, one local rotation fasciocutaneous flap, and one healed with secondary intention at a median of 31.5 days (25–185). We had two mortalities secondary to metastasis. One had achieved complete wound healing and had a 24-month follow-up. The other had a recurrent wound dehiscence following split-thickness skin grafting which was managed with redebridement and NPWT. He, however, expired during the course of treatment at 6 months following the primary debridement. There were no complications due to NPWT.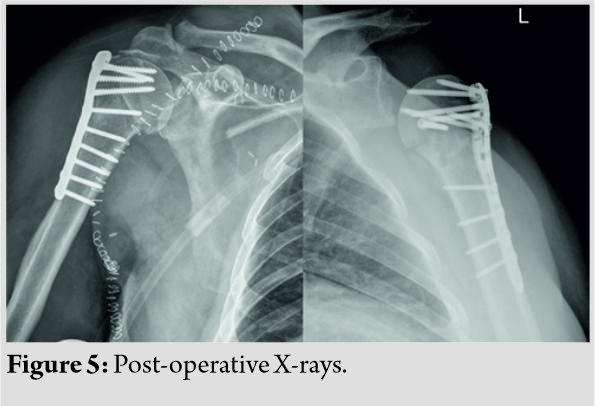
Of the remaining three, two patients had complete wound healing with no recurrence. The third case has a persistent small ulcer at the anterior margin of the local rotation flap over the iliac crest region at 41-month follow-up. The flap, however, has healed well, with no discharge from the ulcer and negative wound cultures.
Discussion
The efficacy of adjuvant radiation therapy in the management of soft tissue sarcomas is well established [7] compared to just a wide excision of the tumor [8]. Radiation therapy causes edema of the vessel walls around the wound which prevents influx of cytokines and platelets, leading to reduced angiogenesis. Reactive free radicals also cause damage to the surrounding vessels and tissues compounding the problems of wound healing and predispose them to infections that are resistant to standard modalities of treatment [9]. The greatest challenge for a surgeon is to establish a bed of healthy granulation tissue. The necrotic tissue gives rise to a great amount of slough that needs periodic debridements. NPWT provides a great tool for the treatment of these conditions as it reduces edema, aids in the control of bacterial infection, as well as promotes angiogenesis, thereby creating a bed of healthy granulation tissue. Our patients responded well to NPWT as they could carry out routine activities with the portable machine. The following illustrative case highlights the use of NPWT in such scenarios. An 18-year-old male patient with a leiomyosarcoma in the inguinal region underwent wide excision with post-operative EBRT and chemotherapy. He developed wound dehiscence with infection in the operative bed with an exposed but thrombosed femoral artery (Fig. 1) during vacuum-assisted closure. The patient underwent a total of five debridements followed by daily dressings (Fig. 2). Like most patients, he used to experience excruciating pain with daily dressing changes and was a challenge [10]. Deep tissue cultures grew multidrug-resistant Klebsiella pneumoniae. Another challenge was a thrombosed femoral artery which was exposed in the wound bed. Subsequently, NPWT was started with low pressures between − 25 and −50 along with close monitoring of vitals and hourly drain output to diagnose femoral artery dehiscence due to its close proximity at the earliest. He underwent 10 NPWT dressings every 4–5 days. The wound subsequently healed completely with secondary intention though the time needed was 185 days after the primary debridement. He has an infection-free follow-up of 22 months (Fig. 3). Literature suggests that on an average, it takes between 8 and 24 days for healthy granulation tissue to form [11]; however, no data are available in our subset of patients who needed 28–185 days in our study. Sarcomas around the axial skeleton such as the lumbar spine, iliac bone, or sacrum pose a challenge with reported wound healing problems in up to 29.2%. Factors such as deficient musculature and constant pressure on the wounds due to a supine posture further compound an already compromised tissue bed [12, 13]. Our second illustrative case was an 18-year-old male who underwent wide excision for synovial sarcoma of the iliac region. He received a total of 6 chemotherapy cycles post-surgery and EBRT and developed a frank discharge from the operated site secondary to a mixed multidrug-resistant infection (Fig. 4). He underwent multiple debridements and a total of 9 NPWT cycles with decortication of the iliac crest. A local rotation fasciocutaneous flap was done which healed well. There is, however, a persistent small ulcer at the anterior margin of the flap over the iliac crest region at 41-month follow-up (Fig. 5). Flap coverage for sarcoma wounds after radiation-induced skin damage is always a great option; however, a plastic surgeon trained in skin and soft tissue transposition is necessary with experience in managing flap necrosis and wound-related complications [14, 15]. The weakness of this study is its retrospective nature and small cohort of patients. The strength lies in the protocol suggested for managing such complex cases with a multimodal approach.
Conclusion
We have achieved good results in our small series by adhering to the following protocol:
1. Team approach comprising orthopedic surgeon specialized in soft tissue infections, medical, radiation and orthopedic oncologist, plastic surgeon, microbiologist, and infectious disease specialist
2. Very aggressive debridement with deep tissue cultures
3. NPWT with serial debridement which may be needed longer than in other cases
4. Appropriate antibiotic therapy based on antibiotic susceptibility
5. Wound cover after achieving a healthy granulating wound bed.
We recommend judicious use of NPWT in infected irradiated wounds as it enhances granulation tissue formation, allows them to ambulate with the portable machine, and reduces the duration of wound healing along with a multimodal approach to the problem.
Clinical Message
Radiation-induced wound infection in operated soft tissue sarcoma beds can be managed successfully by a multidisciplinary team following the principles of aggressive debridement, judicious use of NPWT, appropriate antibiotics, and soft tissue cover.
References
1. Emory CL, Montgomery CO, Potter BK, Keisch ME, Conway SA. Early complications of high-dose-rate brachytherapy in soft tissue sarcoma: A comparison with traditional external-beam radiotherapy. Clin OrthopRelat Res 2012;470:751-8.
2. Alektiar KM, Brennan MF, Healey JH, Singer S. Impact of intensity-modulated radiation therapy on local control in primary soft-tissue sarcoma of the extremity. J Clin Oncol 2008;26:3440-4.
3. Baskar R, Dai J, Wenlong N, Yeo R, Yeoh KW. Biological response of cancer cells to radiation treatment. Front Mol Biosci2014;1:24.
4. Suzuki K, Yamashita S. Radiation-induced bystander response: Mechanism and clinical implications. Adv Wound Care (New Rochelle) 2014;3:16-24.
5. O’Sullivan B, Davis AM, Turcotte R, Bell R, Catton C, Chabot P, et al. Preoperative versus postoperative radiotherapy in soft-tissue sarcoma of the limbs: A randomised trial. Lancet 2002;359:2235-41.
6. Siegel HJ, Long JL, Watson KM, Fiveash JB. Vacuum-assisted closure for radiation-associated wound complications. J Surg Oncol 2007;96:575-82.
7. Prosnitz LR, Maguire P, Anderson JM, Scully SP, Harrelson JM, Jones EL, et al. The treatment of high-grade soft tissue sarcomas with preoperative thermoradiotherapy. Int J Radiat Oncol Biol Phys 1999;45:941-9.
8. Cantin J, McNeer GP, Chu FC, Booher RJ. The problem of local recurrence after treatment of soft tissue sarcoma. Ann Surg 1968;168:47-53.
9. Iyer S, Balasubramanian D. Management of radiation wounds. Indian J Plast Surg 2012;45:325-31.
10. Janugade HB, Chabbra RS, Das AG, Surushe A, Saygaonkar H. Outcomes of VAC versus conventional dressings in patients with lower limb ulcer. Int Surg J 2018;5:1792.
11. Gabriel A, Shores J, Heinrich C, Baqai W, Kalina S, Sogioka N, et al. Negative pressure wound therapy with instillation: A pilot study describing a new method for treating infected wounds. Int Wound J 2008;5:399-413.
12. Ruggieri P, Angelini A, Pala E, Mercuri M. Infections in surgery of primary tumors of the sacrum. Spine (Phila Pa 1976) 2012;37:420-8.
13. Li D, Guo W, Qu H, Yang R, Tang X, Yan T, et al. Experience with wound complications after surgery for sacral tumors. Eur Spine J 2013;22:2069-76.
14. Mastorakos DP, Disa JJ, Athanasian E, Boland P, Healey JH, Cordeiro PG. Soft-tissue flap coverage maximizes limb salvage after allograft bone extremity reconstruction. PlastReconstr Surg 2002;109:1567-73.
15. Ver Halen JP, Yu P, Skoracki RJ, Chang DW. Reconstruction of massive oncologic defects using free fillet flaps. PlastReconstr Surg 2010;125:913-22.
 |
 |
 |
 |
 |
| Dr. Yash Wagh | Dr. Aditya Menon | Dr. Bimal Mody | Dr. Vikas M Agashe | Dr. Manish Agarwal |
| How to Cite This Article: Wagh Y, Menon A, Mody B, Agashe VM, Agarwal M. Radiation-Induced Wound Infections in Operated Soft Tissue Sarcomas: An Unbelievable Challenge in a Series of Five Cases. Journal of Orthopaedic Case Reports 2020 Jan-Feb;10(1): 30-34. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




