[box type=”bio”] Learning Point of the Article: [/box]
Complete Extra-articular ankylosis of hip is rare and CT angiography is beneficial if bony mass is in vicinity of neurovascular bundle. Good functional results can be obtained with excision of bony mass after ruling out bony malignancy.
Case Report | Volume 10 | Issue 1 | JOCR January – February 2020 | Page 74-77 | Kunal A Shah, Mohan M Desai, Radhakrishna Kantanavar, Swapneel Shah. DOI: 10.13107/jocr.2020.v10.i01.1644
Authors: Kunal A Shah[1], Mohan M Desai[1], Radhakrishna Kantanavar[1], Swapneel Shah[1]
[1]Department of Orthopedics, Seth GS Medical College and KEM Hospital,Mumbai, Maharashtra, India.
Address of Correspondence:
Dr. Kunal A Shah,
Department of Orthopedics, Seth GS Medical College and KEM Hospital, Parel, Mumbai, Maharashtra, India.
E-mail: kunalajitshah@gmail.com
Abstract
Introduction: Myositis ossificans (MO) is a benign ossifying lesion. It is also known as heterotopic ossification of muscle, in which lamellar bone is formed in the muscle most commonly due to trauma or neurological injury. Complete extra-articular ankylosis due to extensive MO is rare.
Case Report: We report a case of 22-year-old female with post-traumatic MO following head injury. The patient developed extensive MO in iliopsoas and brachialis muscle leading to complete extra-articular ankylosis of hip and stiffness of elbow which lead to severe functional disability to the patient. Hematological parameters were normal. Surgical excision of the bony mass was done in two stages– hip followed by an elbow. The patient had marked functional improvement in hip and elbow.
Conclusion: Complete extra-articular ankylosis of hip is rare in the case of MO. The massive size of bony mass connecting the femur to pubis is not common and computed tomography angiography is beneficial if bony mass is in the vicinity of neurovascular bundle. Good functional results can be obtained with excision of bony mass after ruling out bony malignancy.
Keywords: Myositis ossificans, extra-articular ankylosis, heterotopic ossification.
Introduction
Myositis ossificans (MO) is defined as a benign ossifying lesion that can affect any type of soft tissue, including subcutaneous fat, tendons, and nerves which are self-limiting in nature. It is found as solitary lesion most commonly in muscles [1]. It is considered to be of unknown etiology and was first reported in 1749. It is classified into three types; MO progressiva, MO circumscripta, and MO traumatica [2]. MO traumatica is the most common type. It usually occurs following head injury, encephalitis, spinal cord injury, polytrauma, major hip surgery, and burns. Presentation is well-circumscribed lesion occurring in muscle hematoma. We report a case of post-traumatic MO involving hip and elbow in a 22-year-old female. It manifested as extra-articular bony ankylosis in hip and stiffness in elbow. We excised both the heterotopic ossification in two different stages to achieve good functional results.
Case Report
A 22-year-old female presented with complaints of restriction of movements in her left hip and left elbow. She had history of head injury due to road traffic accidents 2 years back. She was in coma for 2 months. When she recovered to ambulatory status, she developed stiffness in her left hip and left elbow. Gradually, stiffness increased to an extent of inability to squat or sit cross-legged. 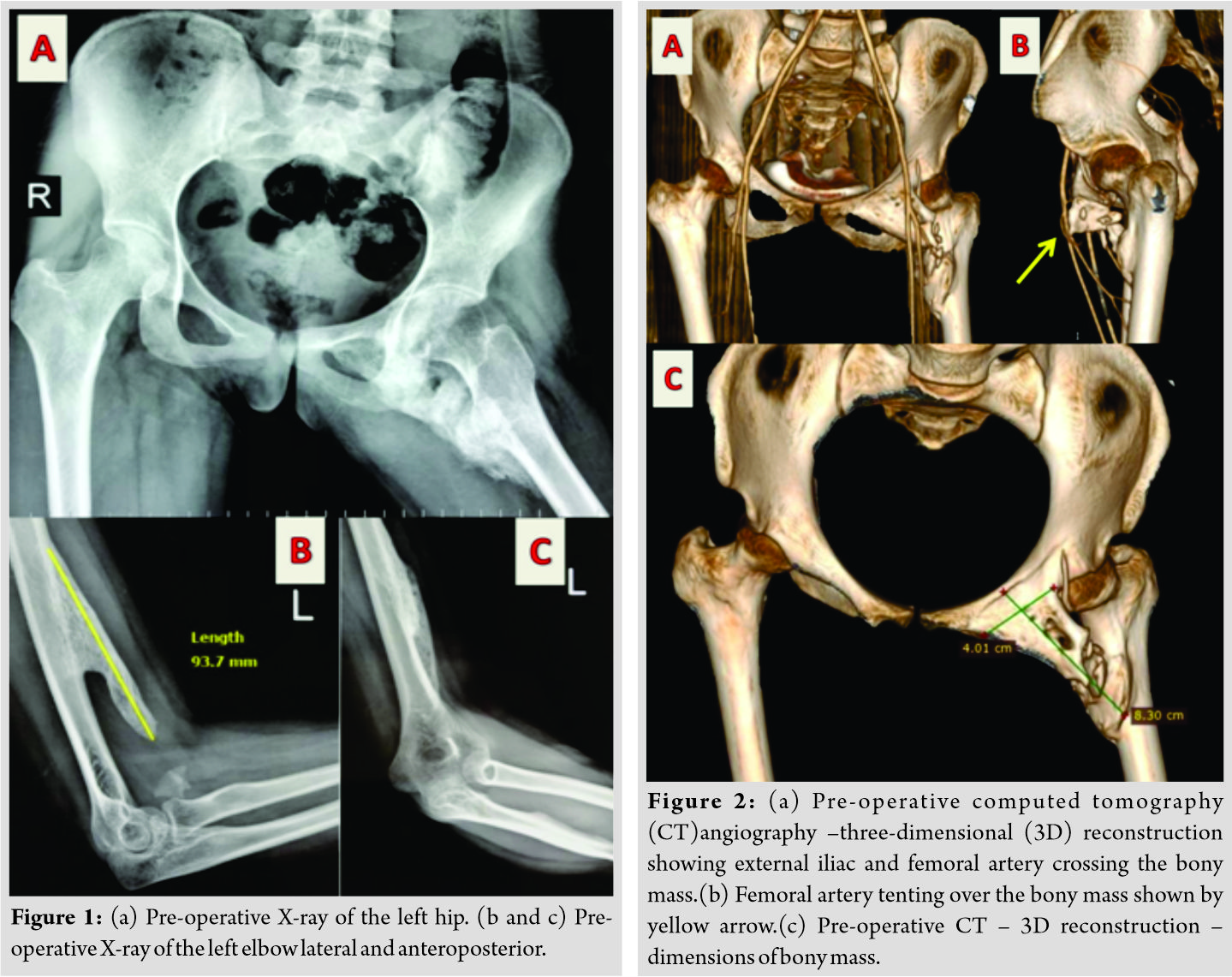 Examination revealed loss of all movements at hip. Hip was ankylosed with flexion deformity of 30 degrees, external rotation deformity of 20 degrees, and abduction deformity of 20 degrees. On palpation, a well-defined bony mass was felt in the femoral triangle. It was non-tender and fixed to underlying bone. There was no local rise of temperature. There was a 20 degree postural flexion deformity at ipsilateral knee. On examination of the left elbow, non-tender, and bony mass was present on anterior aspect of arm. Bony mass was fixed to underlying bone. Flexion deformity of 50 degree with further flexion up to 80degree was present. X-ray of the left hip showed bar of mature bone connecting the lateral part of superior pubic ramus to the lesser trochanter (Fig. 1). There was no bony destruction or periosteal reaction. Computed tomography (CT)angiography and three-dimensional reconstruction of CT images showed femoral artery tenting over the bony mass and complete extent of mass over left hip, respectively. Bony mass had dimensions of length 8.3 cm × 4 cm (Fig. 2). X-ray of the left elbow showed bony mass arising from anterior aspect of humerus directed distally with length of 9.3 cm (Fig. 1). On hematological examination, serum alkaline phosphatase was normal (117 U/L). The excision of bony mass at hip and elbow was planned in two stages. In the first stage, the left hip was operated. Subinguinal approach was used for excision. The femoral neurovascular bundle was carefully separated from the mass. The bony mass was detached from pubis and femur with an osteotome (Fig. 3). After complete excision of mass, full range of hip movement was possible under anesthesia. The mass was sent for histopathological examination and MO was confirmed. Full weight-bearing mobilization was started from 1st post-operative day.
Examination revealed loss of all movements at hip. Hip was ankylosed with flexion deformity of 30 degrees, external rotation deformity of 20 degrees, and abduction deformity of 20 degrees. On palpation, a well-defined bony mass was felt in the femoral triangle. It was non-tender and fixed to underlying bone. There was no local rise of temperature. There was a 20 degree postural flexion deformity at ipsilateral knee. On examination of the left elbow, non-tender, and bony mass was present on anterior aspect of arm. Bony mass was fixed to underlying bone. Flexion deformity of 50 degree with further flexion up to 80degree was present. X-ray of the left hip showed bar of mature bone connecting the lateral part of superior pubic ramus to the lesser trochanter (Fig. 1). There was no bony destruction or periosteal reaction. Computed tomography (CT)angiography and three-dimensional reconstruction of CT images showed femoral artery tenting over the bony mass and complete extent of mass over left hip, respectively. Bony mass had dimensions of length 8.3 cm × 4 cm (Fig. 2). X-ray of the left elbow showed bony mass arising from anterior aspect of humerus directed distally with length of 9.3 cm (Fig. 1). On hematological examination, serum alkaline phosphatase was normal (117 U/L). The excision of bony mass at hip and elbow was planned in two stages. In the first stage, the left hip was operated. Subinguinal approach was used for excision. The femoral neurovascular bundle was carefully separated from the mass. The bony mass was detached from pubis and femur with an osteotome (Fig. 3). After complete excision of mass, full range of hip movement was possible under anesthesia. The mass was sent for histopathological examination and MO was confirmed. Full weight-bearing mobilization was started from 1st post-operative day. 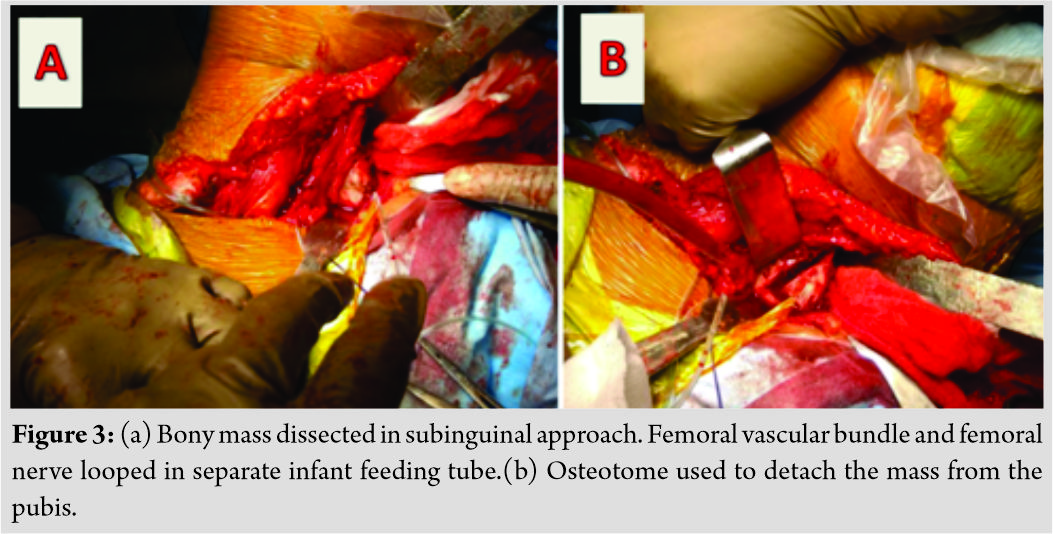 Intermittent active and passive exercises of hip were performed. Oral indomethacin was given for 3 weeks to avoid recurrence. At 2-year follow-up, the patient had 120 degree of flexion, 30 degree of abduction-adduction, and 20 degree of internal and external rotation. The patient could perform all activities of daily living comfortably. X-ray taken at 2-year follow-up showed no recurrence (Fig. 4).
Intermittent active and passive exercises of hip were performed. Oral indomethacin was given for 3 weeks to avoid recurrence. At 2-year follow-up, the patient had 120 degree of flexion, 30 degree of abduction-adduction, and 20 degree of internal and external rotation. The patient could perform all activities of daily living comfortably. X-ray taken at 2-year follow-up showed no recurrence (Fig. 4).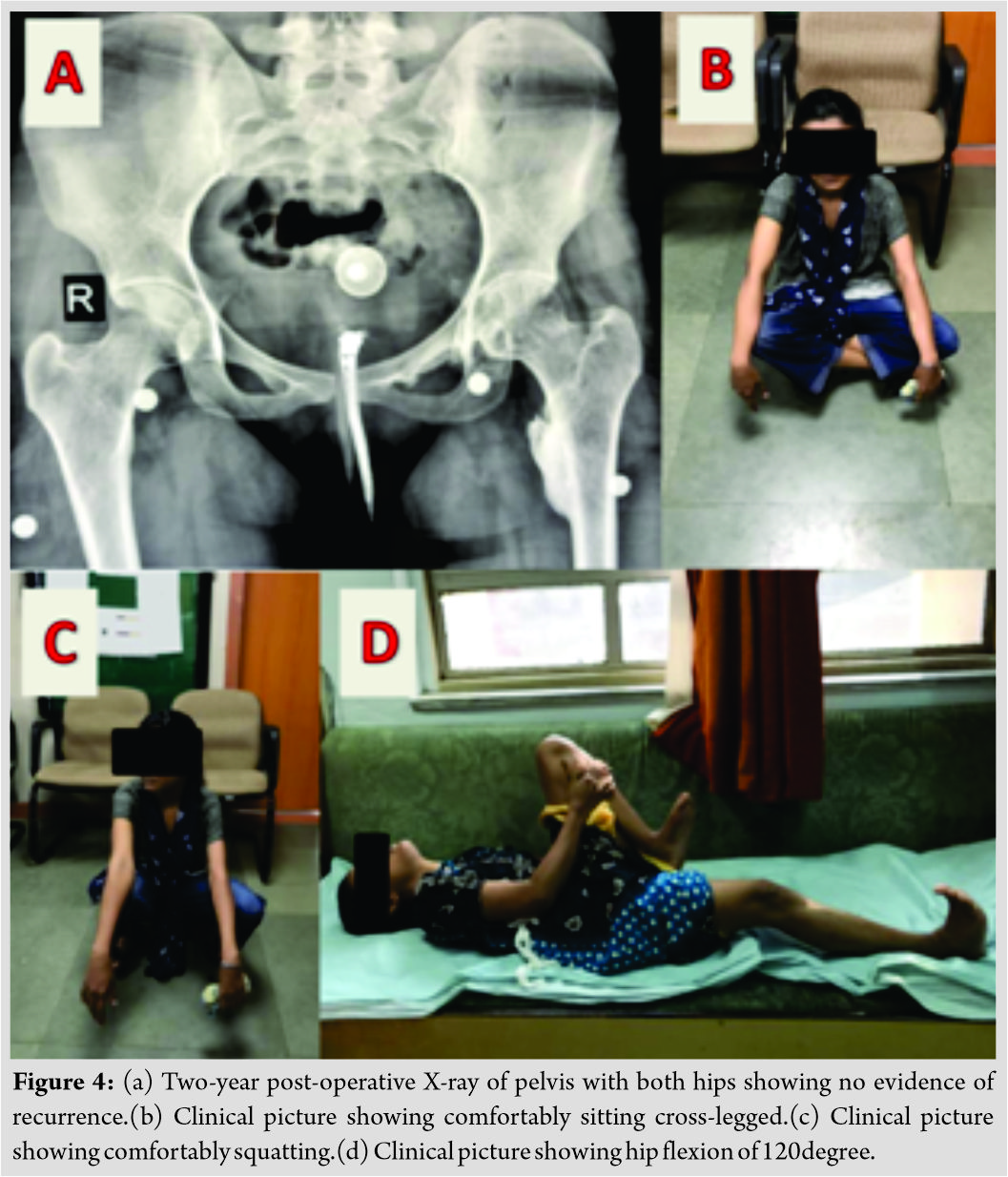
In the second stage, 3 months after hip surgery, stiffness in the left elbow was addressed. Alkaline phosphatase levels before elbow surgery were 135 U/L. The anterolateral incision was taken over the lateral margin of biceps. Biceps belly was retracted and brachialis was split. The bony mass was detached from the anterior aspect of humerus with the help of osteotome. Elbow arthrotomy was done through lateral approach and anterior capsule was excised. Articular surface was examined. Above elbow splint was given in full extension during 1st post-operative week. Oral indomethacin was given for 3 weeks. Full range of movement was started after 1 week. At 2-year follow-up, elbow range was 0–120 degree of flexion, 80 degree of supination, and 60 degree pronation. The patient could perform all activities including heavy daily activities. X-ray at 2-year follow-up showed no recurrence and serum alkaline phosphatase levels were 90 U/L (Fig. 5).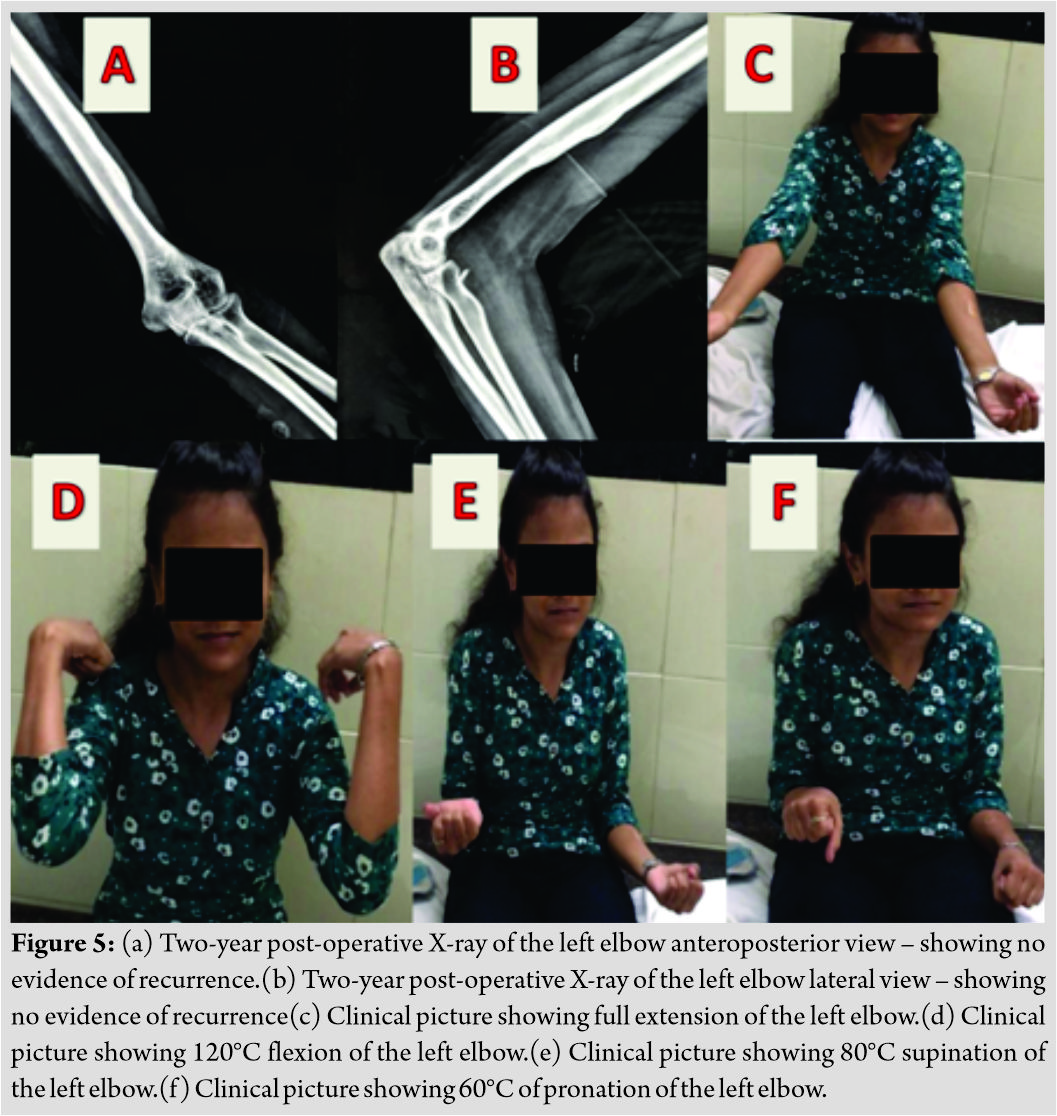
Discussion
MO is benign and well-differentiated bone formation in muscle tissue. It can also be called heterotopic ossification of muscle tissue. After trauma, there are tissue necrosis and hematoma which can stimulate vascular and fibroblastic activity resulting in bone formation [3]. It consists of inappropriate differentiation of mesenchymal cells into chondroblasts and osteoblasts in the presence of inflammation [1]. Three conditions that are necessary for formation of MO are osteogenic precursor cells, inducing agents, and a permissive environment. Head injury provides permissive environment by inducing bone morphogenetic protein 4 which acts on osteogenic precursor cells. These cells later differentiate into osteoblasts [4]. MO of hip occurs more frequently in cases with palsy, epidural or subdural hematoma, and hip surgery. Our case had history of head injury with coma.
In post-traumatic MO, the formation of painful mass occurs with 7–10 days. Irregular osseous fragments form up to 6 weeks. Cortical bone production occurs by 6 months. Maturation of mass takes place between 6 and 8 months [5, 6, 7]. The plain X-ray shows floccular calcification up to 6 weeks after which maturation occurs, which is seen as sharply delineated areas of calcification [5]. It is important to differentiate from bony malignancy. Features favoring the diagnosis of MO are diaphyseal location, intact underlying cortex, lucent zone between lesion and adjacent bone, and dense calcification in the periphery. Features favoring bony malignancy, such as bony destruction, aggressive periosteal reaction, and soft tissue mass were absent in our case [5]. Three-dimensional reconstruction allows us to know the exact extent of the mass and plan the surgical approach. While CT – angiography helps us to study anatomic relationship of mass with the neurovascular bundle. Magnetic resonance imaging findings suggestive of maturation of bony mass are hyperintense ring surrounding the hypointense core [6]. The biopsy may be required in some cases for differential diagnosis. MO is self-limiting and there is possibility of spontaneous regression. Surgical excision is not the primary choice of treatment by most of the surgeons [8]. Surgical indications are pain due mechanical irritation of nearby tendon or bursa, compression of neurovascular structures, and mechanical block in the movement of joints compromising activities of daily living [9]. Our patient had severe disability due to extra-articular ankylosis of the left hip and stiffness of the left elbow. Hence, we planned to surgically excise both the mass. We report this case due to the large size of bony mass and rare presentation of extra-articular ankylosis of the left hip along with stiffness of the left elbow.
Conclusion
Complete extra-articular ankylosis of hip is rare in the case of MO. Furthermore, the massive size of bony mass connecting the femur to pubis is not common. CT angiography is beneficial if bony mass is in the vicinity of neurovascular bundle. Good functional results can be obtained with excision of bony mass after ruling out bony malignancy.
Patient Declaration Statement
The authors certify that they have obtained all appropriate patient consent forms. In the form, the patient has given his consent for his images and other clinical information to be reported in the journal. The patient understands that their names and initials will not be published and due efforts will be made to conceal identity.
Clinical Message
Complete extra-articular ankylosis of hip is rare and CT angiography is beneficial if the bony mass is in vicinity of neurovascular bundle. Good functional results can be obtained with excision of bony mass after ruling out bony malignancy.
References
1. Walczak BE, Johnson CN, Howe BM. Myositis ossificans. J Am AcadOrthop Surg 2015;23:612-22.
2. Fay O. Traumatic paraosteal bone and callus formation: The so-called traumatic ossifying myositis. Surg GynecolObs1914;19:174-90.
3. Nishio J, Nabeshima K, Iwasaki H, Naito M. Non-traumatic myositis ossificans mimicking a malignant neoplasm in an 83-year-old woman: A case report. J Med Case Rep 2010;4:270.
4. Chalmers J, Gray DH, Rush J. Observations on the induction of bone in soft tissues. J Bone Joint Surg Br 1975;57:36-45.
5. Bagaria V, Rasalkar D. Extensive myositis ossificans with extra-articular ankylosis of the hip joint. Hong Kong J Radiol2011;14:35-8.
6. Parikh J, Hyare H, Saifuddin A. The imaging features of post-traumatic myositis ossificans, with emphasis on MRI. Clin Radiol2002;57:1058-66.
7. Saussez S, Blaivie C, Lemort M, Chantrain G. Non-traumatic myositis ossificans in the paraspinal muscles. Eur Arch Otorhinolaryngol2006;263:331-5.
8. Aneiros-Fernandez J, Caba-Molina M, Arias-Santiago S, Ovalle F, Hernandez-Cortes P, Aneiros-Cachaza J. Myositis ossificans circumscripta without history of trauma. J Clin Med Res 2010;2:142-4.
9. Ellerin BE, Helfet D, Parikh S, Hotchkiss RN, Levin N, Nisce L, et al. Current therapy in the management of heterotopic ossification of the elbow: A review with case studies. Am J Phys Med Rehabil1999;78:259-71.
 |
 |
 |
 |
| Dr. Kunal A Shah | Dr. Mohan M Desai | Dr. Radhakrishna Kantanavar | Dr. Swapneel Shah |
| How to Cite This Article: Shah K A, Desai M M, Kantanavar R, Shah S. Complete Extra-articular Ankylosis of Hip and Stiff Elbow in a Case of Extensive Myositis Ossificans: A Rare Presentation. Journal of Orthopaedic Case Reports 2020 Jan-Feb;10(1): 74-77. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




