[box type=”bio”] Learning Point of the Article: [/box]
Loose bodies may be concealed by the plica during routine knee arthroscopy. Successful arthroscopic removal of loose bodies in the separated suprapatellar compartment requires careful study of pre-operative imaging and can effectively be performed.
Case Report | Volume 10 | Issue 2 | JOCR March – April 2020 | Page 17-20 | Shi Ming Tan, Ing How Moo, Kesavan Sitampalam, Joyce Suang Bee Koh, Tet Sen Howe. DOI: 10.13107/jocr.2020.v10.i02.1678
Authors: Shi Ming Tan[1], Ing How Moo[1], Kesavan Sitampalam[2], Joyce Suang Bee Koh[1], Tet Sen Howe[1]
[1]Department of Orthopedic Surgery, Singapore General Hospital, Outram Road, Singapore 169608, Singapore,
[2]Department of Anatomical Pathology, Singapore General Hospital, Outram Road, Singapore 169608, Singapore.
Address of Correspondence:
Dr. Ing How Moo,
Department of Orthopedic Surgery, Singapore General Hospital, Outram Road, Singapore 169608, Singapore.
E-mail: zell53@hotmail.com
Abstract
Introduction: A complete suprapatellar plica of the knee is a rare condition that separates the suprapatellar pouch from the rest of the knee cavity. Synovial osteochondromatosis is a rare benign monoarticular arthropathy affecting synovial joints that are clinically manifested as intra-articular multiple loose bodies. Isolated synovial osteochondromatosis within a concealed suprapatellar pouch caused by complete suprapatellar plica is an exceptionally rare occurrence. There is no well-documented report in literature on the diagnosis and arthroscopic approach to osteochondromatosis within a separated suprapatellar pouch.
Case Report: We report the case of a 61-year-old man who presented with a 3-month history of atraumatic right knee pain localized to the suprapatellar region. Pre-operative magnetic resonance imaging confirmed the presence of loose bodies at the suprapatellar region behind the complete septum. Loose bodies were concealed in a sealed suprapatellar pouch and could not be detected by routine arthroscopic examination of the knee cavity. The suprapatellar plica was punctured and loose bodies trapped within the enclosed suprapatellar compartment were arthroscopically removed. Histological examination of the loose bodies confirmed the diagnosis of osteochondromatosis. The patient postoperatively experienced complete relief of knee pain.
Conclusion: Successful arthroscopic removal of loose bodies in the separated suprapatellar compartment requires careful study of pre-operative imaging and can effectively be performed through the standard anteromedial and anterolateral arthroscopic portals.
Keywords: Arthroscopic removal, loose body, osteochondromatosis, plica, suprapatellar pouch.
Introduction
Plicae are intra-articular synovial septa that remain in adulthood, formed during the developmental period of the knee joint in the early fetal life. Plicae are classified into the following four types: Suprapatellar, infrapatellar, mediopatellar, and lateral [1]. The most common type is suprapatellar plica (also known as plica synovialis suprapatellaris), which divides the suprapatellar pouch from the remainder of the knee. A suprapatellar plica varies from a complete, intact septum to a small crescentic fold, typically superior to the patella and posterior to the quadriceps tendon [2]. An enclosed suprapatellar pouch formed by a complete synovial plica is a rare anatomical variant and rarely causes any symptoms [3, 4].
Synovial osteochondromatosis is a rare, benign, idiopathic disease affecting the synovium of the synovial joints [5]. It is likely that the synovium undergoes cartilage metaplasia and produces small nodules of cartilage. Secondary calcification and ossification can occur and form multiple cartilaginous loose bodies. The knee is the most commonly affected synovial joint.
To the best of our knowledge, only one case of isolated synovial osteochondromatosis of the suprapatellar pouch has been reported. However, there are no clear descriptions of an efficient method of diagnosis and arthroscopic technique for the removal of loose bodies. In the present study, we describe a case involving the arthroscopic removal of osteochondromatosis in an isolated, completely enclosed suprapatellar pouch.
Case Report
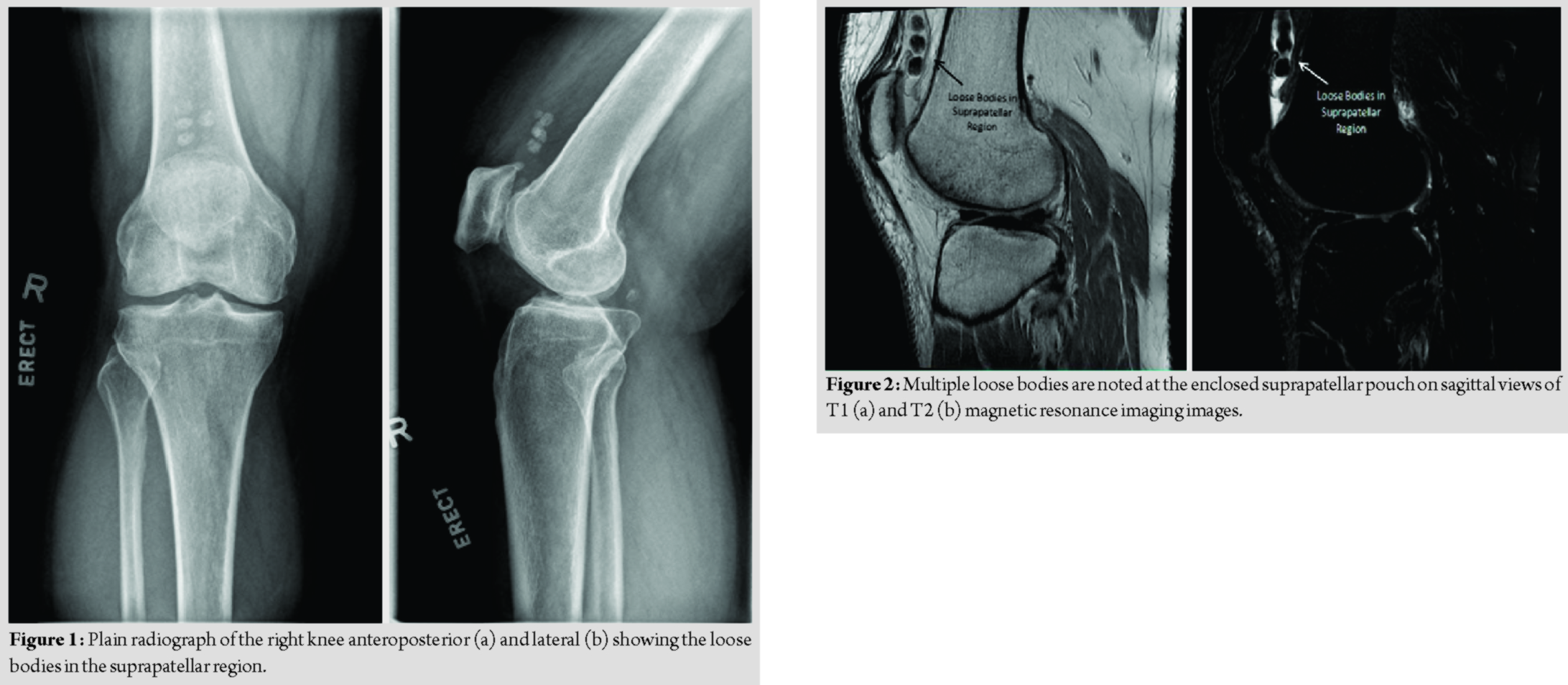
A 61-year-old man was referred to our tertiary center for atraumatic right knee pain lasting for 3 months. The pain was localized to the suprapatellar region and was worse with the knee in flexion. The knee pain was associated with occasional locking. On examination, mild quadriceps wasting was noted and moderate effusion was present. The medial and lateral joint lines were non-tender. The patient had a full knee range of motion of 0–120°. The patellar grind test was positive. The right knee radiographs revealed five loose bodies in the suprapatellar region, which were observed on sequential sets of radiographs performed 3 months apart. In addition, radiographic signs of osteoarthritic changes included narrowed medial joint space, mild osteophyte formation, and subchondral sclerosis (Fig.1). Differentials for the intra-articular loose bodies or calcification include synovial osteochondromatosis, chondrosarcoma, osteochondral fractures, and osteochondritis dissecans. Pre-operative magnetic resonance imaging (MRI) of the right knee revealed multiple loose bodies within the enclosed suprapatellar pouch with knee joint effusion (Fig. 2). There was a suprapatellar plica dividing the suprapatellar pouch into two cavities. There were foci of full-thickness cartilage wear in the medial tibiofemoral and patellofemoral joints, although the meniscus was intact. The patient underwent arthroscopic removal of the loose bodies in the suprapatellar pouch and debridement of suprapatellar plica.
Surgical technique
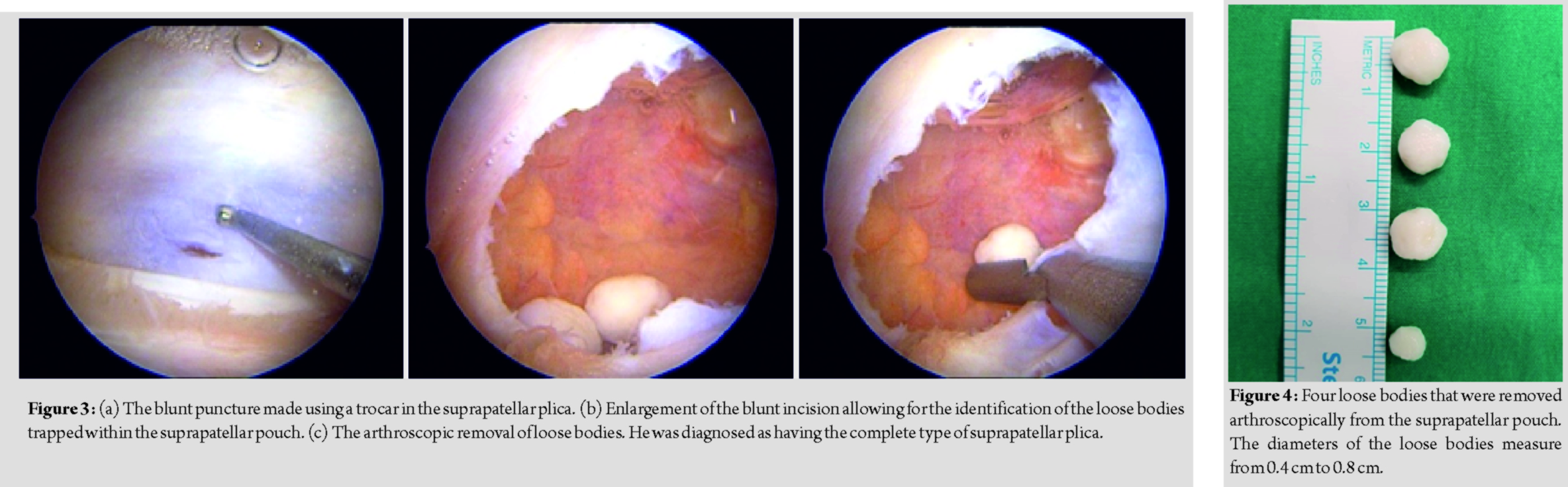
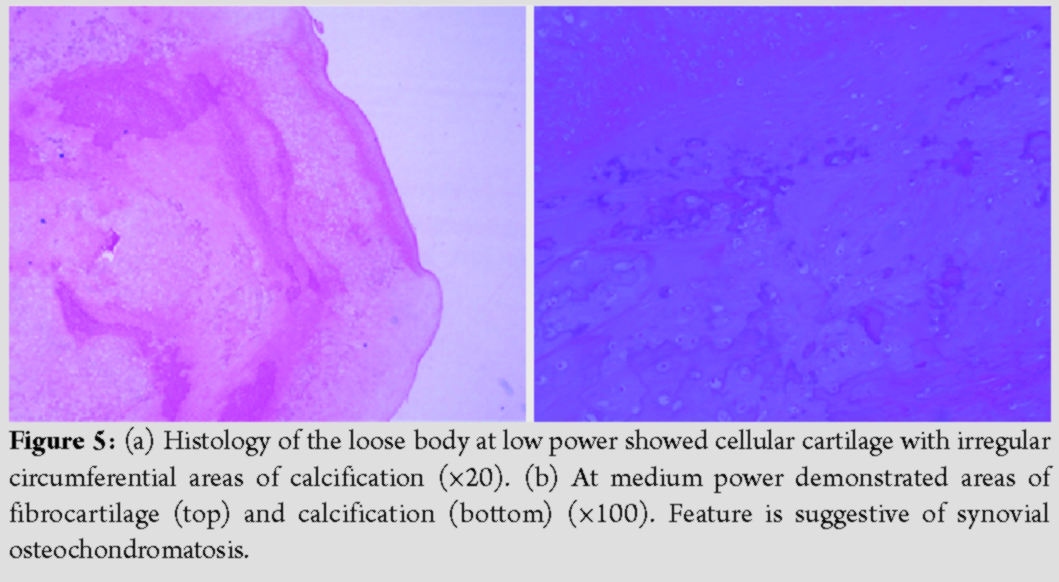
Under general anesthesia, standard knee arthroscopy was performed through the anteromedial and anterolateral portals. The findings reported on MRI were confirmed during the initial routine arthroscopy, including full-thickness cartilage wear on the medial, tibiofemoral, and patellofemoral joint surfaces and intact meniscus. Routine arthroscopic examination did not detect any loose bodies in the suprapatellar pouch or medial and lateral gutters. However, radiographic images consistently showed few loose bodies trapped in the sealed suprapatellar pouch behind the plica. Thereafter, a blunt trocar was introduced into the working anteromedial portal and directed toward the suprapatellar plica. A blunt puncture was made on the suprapatellar plica using the trocar, and the blunt incision was enlarged to allow the identification of the loose bodies trapped within the enclosed suprapatellar compartment. On identification, the loose bodies were uneventfully removed (Fig. 3). The suprapatellar plica is then excised arthroscopically. In total, five loose bodies were arthroscopically removed (Fig. 4) and one loose body was sent for histology. Histology revealed irregular circumferential areas of calcification around the central cartilage, which confirmed the diagnosis of osteochondromatosis (Fig. 5). The patient’s post-operative recovery was uncomplicated and all symptoms resolved. Post-operative plain radiograph showed that the loose bodies had disappeared (Fig. 6). At 1-year follow-up, the patient remained asymptomatic and had resumed all activities.
Discussion
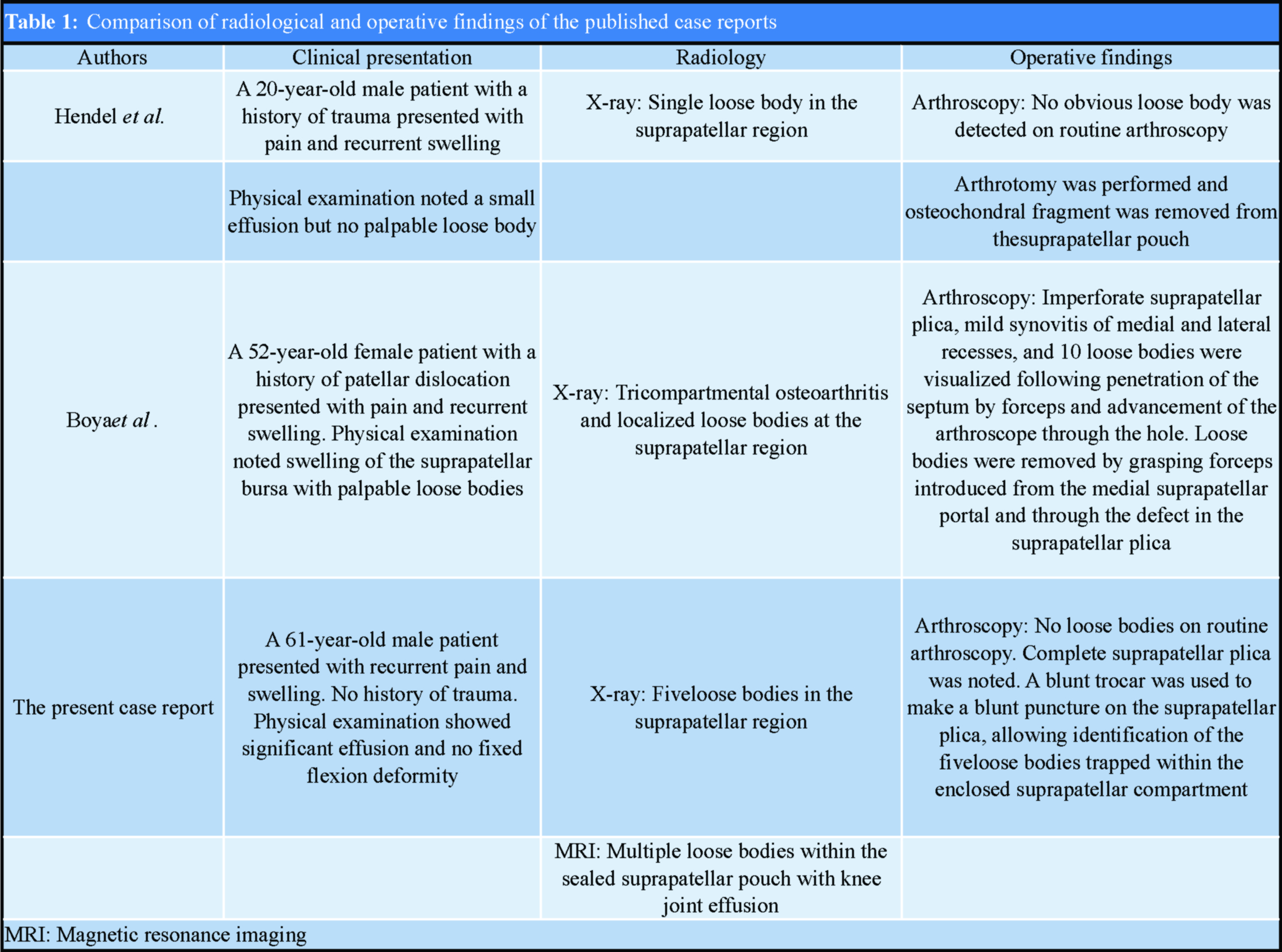
Suprapatellar plicae are observed in various forms by arthroscopy. In 1990, Dandy studied 500 knees by arthroscopy and reported the complete type of suprapatellar plicae in only 4.2% of patients [6]. The existence of an incomplete involuted or entire suprapatellar plica is believed to be primarily asymptomatic. A complete suprapatellar plica forming an enclosed compartment with entrapped osteochondromatosis is an exceptionally rare occurrence. There are no well-documented reports in literature on the diagnosis and arthroscopic approach to osteochondromatosis within the separated suprapatellar pouch. In 1988, Hendel and Halperin et al. first published the case of a young soldier with osteochondral fragment trapped by a plica with a valve-like orifice [7]. As arthroscopy failed to identify the loose body, arthrotomy was performed to remove it. In 2002, Boya et al. reported an osteochondromatosis of the knee characterized by multiple isolated loose bodies in the suprapatellar bursa caused by imperforate suprapatellar plica in a 52-year-old woman [8]. However, pathologic examination was not performed in the study. Table 1 shows a comparison of the relevant radiological and operative findings of the published case reports. Various theories have been proposed regarding the development of an isolated suprapatellar pouch. One theory is that the pre-existing isolated suprapatellar pouch was included in the process of chondrocalcinosis. An inflammatory episode could provoke excessive fluid production, and loose bodies develop when suprapatellar effusion persists for several months. Another theory suggests that chondrocalcinosis produces synovial inflammation, leading to adhesions between the incomplete involuted suprapatellar membrane and synovial lining of the joint, closing the port between them. Surgical removal of loose bodies in symptomatic patients remains the treatment of choice because they tend to cause synovitis and plicae inflammation due to constant impingement between the femoral condyle and patella. Because the compartment formed by the suprapatellar plica is completely enclosed, successful arthroscopic removal of loose bodies is often challenging as the plica prevents complete routine arthroscopy and identification of the loose bodies through the infrapatellar approach. As such, a high index of suspicion of the presence of a plica is necessary to prevent missed identification of loose bodies on arthroscopy. In our patient, MRI revealed the presence of a plica dividing the suprapatellar compartment and multiple loose bodies in close proximity. It is vital that an enclosed suprapatellar compartment is suspected when the following factors are present: (1) Multiple loose bodies in close proximity within the suprapatellar region on radiograph, (2) recurrent suprapatellar effusion, and (3) presence of a plica on MRI. Radiographically, a suprapatellar plica can be identified as a band of low signal intensity within high signal intensity joint fluid and is best evaluated on T2-weighted or proton density-weighted MRI [9]. The size and morphological features of a given plica on MRI do not necessarily indicate its clinical significance. MRI can differentiate between an isolated pouch and a soft tissue tumor or between an isolated and connecting suprapatellar pouch and may show the extent of an incomplete involuted septum. Boya et al. recommended creating another medial suprapatellar portal to visualize the suprapatellar pouch [8]. Thus, we recommend that the anterolateral portal is sufficient for visualizing the plica, and it is not necessary to create another suprapatellar portal for visualization. Furthermore, a plica can be bluntly punctured to identify the enclosed compartment, and grasping forceps introduced through the anteromedial portal can effectively remove the loose bodies.
Conclusion
Synovial osteochondromatosis within the enclosed suprapatellar compartment is exceedingly rare but may cause recurrent pain and effusion. Successful arthroscopic removal of entrapped loose bodies can be easily achieved with careful evaluation of the pre-operative MRI and performed through the standard arthroscopic portals.
Clinical Message
A complete suprapatellar plica of the knee separates the suprapatellar pouch from the rest of the knee cavity. Loose bodies may be concealed by the plica during routine knee arthroscopy. To identify the loose bodies, the suprapatellar plica must be punctured and arthroscope be placed within the enclosed suprapatellar compartment. Successful removal of these loose bodies will allow the resolution of symptoms.
References
1. Al-HadithyN, GikasP, MahapatraAM, DowdG. Review article: Plica syndrome of the knee.J Orthop Surg (Hong Kong)2011;19:354-8.
2. BolesCA, MartinDF. Synovial plicae in the knee.AJR Am J Roentgenol2001;177:221-7.
3. DeutschAL, ResnickD, DalinkaMK, GilulaL, DanzigL, GuerraJ Jr., et al.Synovial plicae of the knee.Radiology1981;141:627-34.
4. BaeDK, NamGU, SunSD, KimYH.The clinical significance of the complete type of suprapatellar membrane.Arthroscopy1998;14:830-5.
5. MilgramJW. Synovial osteochondromatosis: A histopathological study of thirty cases.J Bone Joint Surg Am1977;59:792-801.
6. DandyDJ. Anatomy of the medial suprapatellar plica and medial synovial shelf.Arthroscopy1990;6:79-85.
7. HendelD, HalperinN.An unusual loose body hidden in a sealed suprapatellar pouch.Arthroscopy1988;4:282-3.
8. BoyaH, PinarH, OzcanO. Synovial osteochondromatosis of the suprapatellar bursa with an imperforate suprapatellar plica.Arthroscopy2002;18:E17.
9. García-ValtuilleR, AbascalF, CerezalL, García-ValtuilleA, PeredaT, CangaA, et al.Anatomy and MR imaging appearances of synovial plicae of the knee.Radiographics2002;22:775-84.
 |
| Dr. Shi Ming Tan |
| How to Cite This Article: Tan SM, Moo IH, Sitampalam K, Koh JSB, Howe TS. Isolated Synovial Osteochondromatosis in a Completely Enclosed Suprapatellar Pouch: A Rare Case Report. Journal of Orthopaedic Case Reports 2020 Mar-Apr;10(2): 17-20. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




