[box type=”bio”] Learning Point of the Article: [/box]
Compartment syndrome can occur during an acute appendicular flare-up of fibrodysplasia ossificans progressiva.
Case Report | Volume 10 | Issue 3 | JOCR May – June 2020 | Page 103-107 | Frederick S. Kaplan, Mona Al Mukaddam, Robert J. Pignolo. DOI: 10.13107/jocr.2020.v10.i03.1770
Authors: Frederick S. Kaplan[1],[2],[3], Mona Al Mukaddam[1],[2],[3], Robert J. Pignolo[4]
[1]Department of Orthopaedic Surgery, The Perelman School of Medicine of The University of Pennsylvania, Philadelphia, PA 19104, USA,
[2]Department of Medicine, The Perelman School of Medicine of The University of Pennsylvania, Philadelphia, PA 19104, USA,
[3]The Center for Research in FOP and Related Disorders, The Perelman School of Medicine of The University of Pennsylvania, Philadelphia, PA 19104, USA,
[4]Department of Medicine, The Mayo Clinic, Rochester, MN 55905, USA.
Address of Correspondence:
Dr. Frederick S. Kaplan,
Department of Orthopaedic Surgery, Division of Orthopaedic Molecular Medicine, Perelman School of Medicine, The University of Pennsylvania, Penn Musculoskeletal Center – Suite 600 3737, Market Street, Philadelphia, PA 19104.
E-mail: Frederick.Kaplan@pennmedicine.upenn.edu
Abstract
Introduction: The severe pain that commonly accompanies appendicular flare-ups of fibrodysplasia ossificans progressiva (FOP) is often ascribed to compartment syndrome, but no documentation exists.
Case Report: We revisited the case of an adult with classic FOP who underwent measurement of compartment pressure of the thigh during an acute, severely painful flare-up of the thigh. The intracompartmental pressure of the thigh was measured at 95-–110 mm of mercury (normal compartment pressure is 0-–8 mmHg). A fasciotomy of the thigh was performed. Despite immediate post-operative relief of pain, progressive heterotopic ossification and loss of function of the hip and knee occurred.
Conclusion: This unique case documents and confirms the suspected presence of compartment syndrome during an acute flare-up of FOP and has vital implications for understanding the pathophysiology and care of patients with acute appendicular flare-ups of FOP and for the design of emerging clinical trials.
Keywords: Fibrodysplasia ossificans progressivaa (FOP), compartment syndrome, heterotopic ossification, bone morphogenetic protein signaling, activin receptor A, type I (ACVR1).
Introduction
Fibrodysplasia ossificans progressiva (FOP; MIM135100) is a progressively disabling genetic disorder of extraskeletal ossification caused by activating mutations in activin receptor A, type I (ACVR1) a bone morphogenetic protein (BMP) type I receptor, in all affected individuals. FOP leads to the progressive postnatal formation of a second skeleton of heterotopic bone [1, 2, 3, 4]. Individuals with FOP appear normal at birth except for characteristic malformations of the great toes that are present in all classically affected individuals [1]. During the first decade of life, episodic soft-tissue swellings (or flare-ups) that arise traumatically or spontaneously undergo pathological metamorphosis into mature heterotopic bone through an endochondral pathway [1, 5, 6]. The pathophysiology of the disorder is multifactorial with immune activation, abnormal cellular response to hypoxia, and dysregulation of multiple signaling pathways [7, 8, 9, 10]. Bone formation in FOP is episodic, but disability is cumulative [11]. Most patients are confined to a wheelchair or immobilized in a standing position by the third decade of life and require lifelong assistance with activities of daily living [1, 5, 6]. The estimated median survival age is 56 years; death often results from complications of thoracic insufficiency syndrome [12]. At present, there is no definitive treatment for FOP, but a number of targeted therapies show promise in pre-clinical studies [13]. Standard of care medical management is currently supportive. High-dose glucocorticoids have limited use in the symptomatic management of the early inflammatory flare-ups [14]. The severe pain that commonly accompanies appendicular flare-ups of FOP is often ascribed to compartment syndrome, a potentially disastrous complication, in which the circulation and function of skeletal muscle within a closed fascial space are compromised by increased pressure within that space. However, to the best of our knowledge, no direct documentation exists of intracompartmental pressure measurements during an acute, painful flare-up of FOP. We revisited the case of an adult with classic FOP who underwent measurement of intracompartmental pressure of the anterior thigh during an acute, painful flare-up of FOP.
Case Report
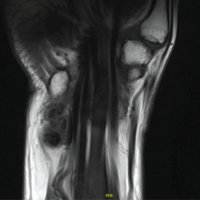
A 40-year-old woman with a well-established clinical diagnosis of classic FOP presented to the emergency department of a local hospital with intractable pain of the right thigh and a several week history of a spontaneous FOP flare-up of the right thigh unresponsive to prolonged prednisone therapy and narcotic analgesia. The right thigh was massively swollen and tense. Passive flexion of the knee caused extreme discomfort. Distal pulses were intact. The neck, back, both shoulders, and both elbows were fused. The left hip showed slight decreased motion, especially in rotation. The left knee and ankle had a normal active range of movement. The great toes were short with hallux valgus malformations (Fig. 1), and the interphalangeal joints were fused. Doppler ultrasonography was performed for the evaluation of deep vein thrombosis and was negative. Plain films showed developmental dysplasia of both hips but no heterotopic ossification. A computed tomographic scan of the thighs revealed swelling and heterogeneity of the quadriceps musculature. The iliopsoas was enlarged (according to official radiographic reports; radiographs and scans are no longer available). Complete blood count and clotting factors were normal. The alkaline phosphatase was 147 IU/L (normal: 43–122 IU/L). The sedimentation rate was 30 mm/h (normal: 0–25 mm/h). Creatine kinase levels were not obtained.
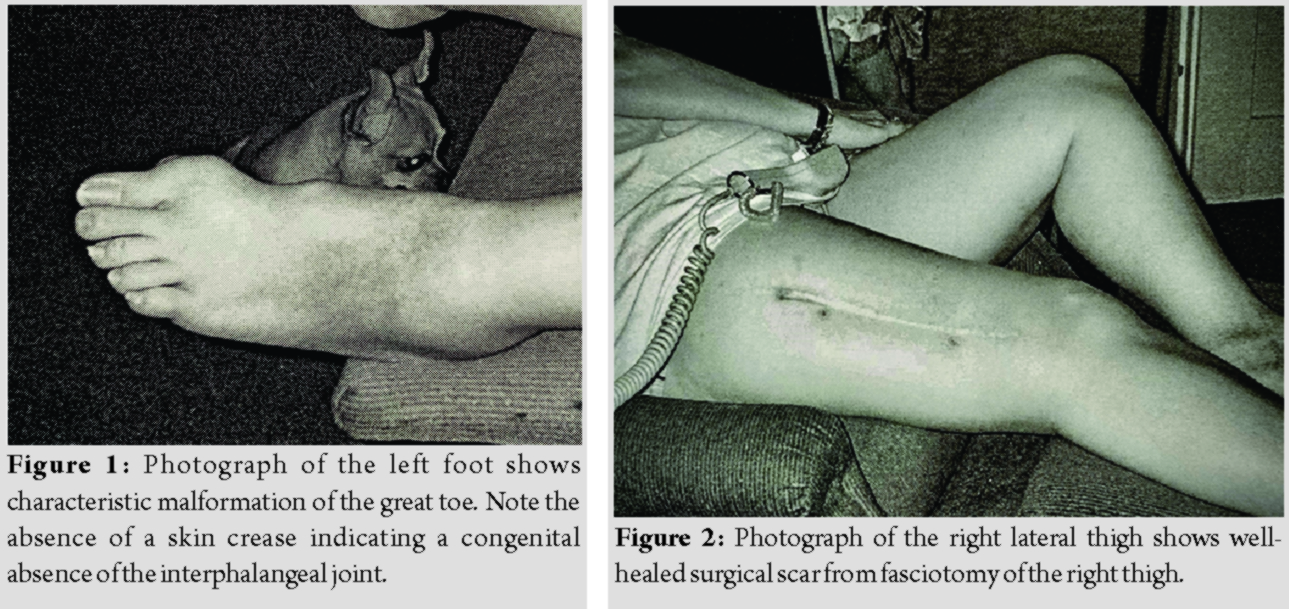
An acute compartment syndrome of the anterior thigh was suspected. Intracompartmental pressures of the right thigh were measured and recorded at 110 mm of mercury in the right mid-quadriceps and 95 mm of mercury in the right distal quadriceps. The device used to measure the intracompartmental pressures was not listed in the emergency room records. An extensive fasciotomy and decompression of the anterior and posterior compartments of the thigh were performed from a single lateral incision with immediate post-operative relief of pain. A secondary closure of the skin and fascia was performed 2 days later (Fig. 2). The patient was sent to a rehabilitation facility for ambulatory therapy. Radiographs performed 7 months after the fasciotomy were reported as showing extensive heterotopic ossification of the lateral thigh musculature from the anterior inferior iliac spine across the hip joint down to the knee. The hip and the knee were functionally ankylosed.
Discussion
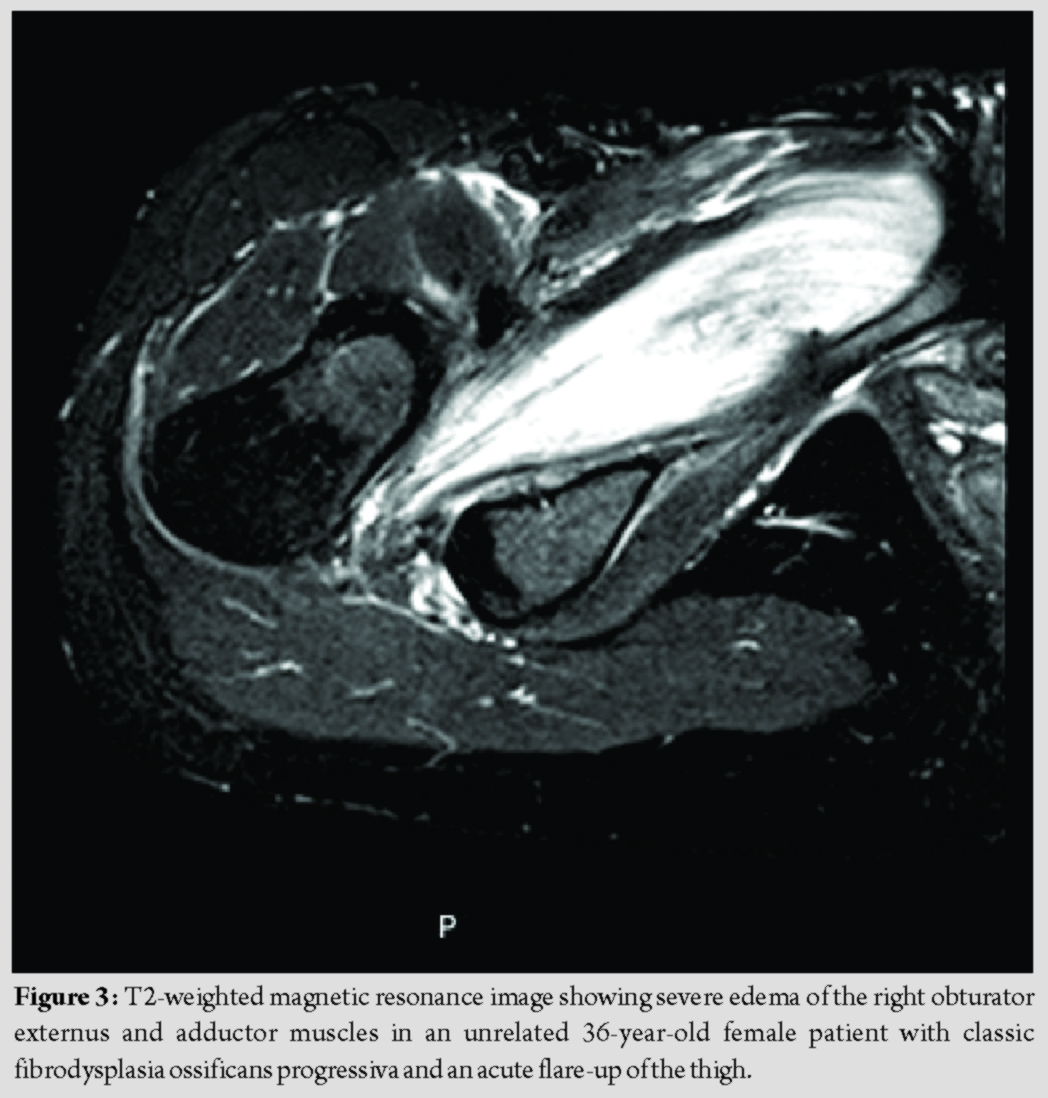
This unique case illustrates conclusively what has long been suspected – that intracompartmental pressures that dramatically exceed capillary filling pressure exist in an acute flare-up of FOP involving the thigh [15]. The normal pressure of a tissue compartment is between 0 and 8 mm of mercury. Capillary blood flow becomes compromised and severe pain may develop when tissue pressure increases to 30 mm of mercury. Muscle and nerve ischemia occur when tissue pressures approach diastolic pressure [16, 17, 18]. In the FOP patient reported here, the compartment pressure greatly exceeded the threshold for acute compartment syndrome.It is plausible that intracompartmental pressures were modulated by the extended period of treatment with corticosteroids and that rebound swelling and severe pain recurred when the corticosteroids were tapered and discontinued. This is the only case to our knowledge that specifically measured the pressure within a closed fascial compartment and documented an acute compartment syndrome during a flare-up of FOP. However, compartment syndrome may be more common than previously considered in painful appendicular flare-ups. Unfortunately, the diagnosis of FOP was probably unknown to the medical team who evaluated the patient in the emergency room [16]. It is difficult to determine the temporal emergence of the compartment syndrome as severe edema may occur throughout the evolution of an FOP flare-up. The early catabolic phase of an appendicular FOP lesion, regardless of whether it is induced by trauma or occurs spontaneously (as in our patient), is characterized clinically by increasing pain and histologically by extensive inflammation and extreme vascular permeability [1]. This early phase is often responsive symptomatically to a brief course of high-dose corticosteroids, but commonly subject to rebound edema with tapering or cessation of steroids [14]. The later anabolic phases of a symptomatic FOP lesion – specifically the transition from the fibrotic to the pre-osseous chondrogenic stage and eventually to the ossification stage – are often characterized by obstructive edema best seen on magnetic resonance imaging as the lesion increases in volume. In the very late stages of lesion formation, reactive edema may occur at the periphery of the lesion, where it is in contact with uninvolved tissue [19]. Thus, soft-tissue swelling and edema may occur throughout all stages of lesion evolution, lead to increased intracompartmental pressure that threatens the viability of the soft tissues within the compartment, precipitate cellular hypoxia of local tissues, amplify the BMP signaling pathway, and exacerbate the progression of heterotopic ossification [9, 19]. It is unfortunate that the patient underwent intracompartmental pressure measurement and fasciotomy as invasive procedures such as these are contraindicated in FOP. However, many important lessons may be learned from this case, not the least of which is that FOP patients must make it abundantly clear to treating physicians that invasive procedures must be assiduously avoided. While emergency fasciotomy is the treatment of choice for acute compartment syndrome, the diagnosis of FOP is a contraindication to such a therapeutic maneuver, as the operative intervention will inevitably exacerbate the flare-up or be futile. It might be appropriate to consider non-operative approaches such as intravenous corticosteroids, although there is no evidence that such measures affect the outcome of acute flare-ups of FOP. Second, this unique case suggests that acute compartment syndrome exists during flare-ups of FOP, especially at appendicular sites, and may be more common than previously appreciated. The patient described here had a typical presentation for acute flare-ups involving the hip or thigh – with severe edema noted clinically at presentation. Her clinical picture is consistent with many FOP patients and similar to an unrelated FOP patient shown here where T2-weighted images on magnetic resonance imaging showed severe edema of the obturator externus and adductor muscles during an acute flare-up of FOP (Fig. 3) [20]. Third, the presence of severe swelling and resultant tissue hypoxia in a closed fascial compartment will release endogenous damage-associated molecular patterns, stimulate endogenous toll-like receptors and exacerbate, and amplify the response to the formation of heterotopic ossification in FOP [9, 10]. The recognition of that principle should propel efforts to study compartment syndrome in FOP in a relevant animal model so that efforts can be developed to intervene non-invasively in an attempt to reduce compartment pressures [21, 22, 23]. Fourth, the recognition that extreme compartment pressures may exist during a flare-up of FOP – especially within tight fascial compartments – may severely impair the delivery of therapeutic agents to the skeletal muscles within the compartment and thereby jeopardize the potential efficacy of drugs in clinical trials. Thus, chronic therapy with agents under development may be needed to prevent the onset of acute flare-ups and resultant compartment syndromes. Fifth and finally, one wonders why acute and severely swollen flare-ups involving the back during childhood are accompanied by little pain and no consideration of compartment syndrome [5, 6]. One might speculate that perhaps, the fascial/aponeurotic compartments of the back are capacious and can accommodate the acute swelling of FOP flare-ups at those axial locations?
Conclusion
This unique and illustrative case documents and confirms the presence of compartment syndrome during a flare-up of FOP and has important implications for the care of FOP patients with acute flare-ups of FOP at appendicular sites and for the design of emerging clinical trials.
Clinical Message
Elevated intracompartmental pressures and compartment syndrome can occur in acute flare-ups of FOP; however, invasive procedures such as fasciotomy are contraindicated in FOP.
References
1. Pignolo RJ, Shore EM, Kaplan FS. Fibrodysplasia ossificans progressiva: Diagnosis, management, and therapeutic horizons. Pediatr Endocrinol Rev 2013;10:437-48.
2. Shore EM, Xu M, Feldman GJ, Fenstermacher DA, Cho TJ, Choi IH, et al. A recurrent mutation in the BMP Type I receptor ACVR1 causes inherited and sporadic fibrodysplasia ossificans progressiva. Nat Gen 2006;38:525-7.
3. Kaplan FS, Xu M, Seemann P, Connor JM, Glaser DL, Carroll L, et al. Classic and atypical fibrodysplasia ossificans progressiva (FOP) phenotypes are caused by mutations in the bone morphogenetic protein (BMP) Type I receptor ACVR1. Hum Mutat 2009;30:379-90.
4. Kaplan FS, Pignolo RJ, Shore EM. The FOP metamorphogene encodes a novel Type I receptor that dysregulates BMP signaling. Cytokine Growth Factor Rev 2009;20:399-407.
5. Pignolo RJ, Bedford-Gay C, Liljesthrom M, Durbin-Johnson BP, Shore EM, Rocke DM, et al. The natural history of flare-ups in fibrodysplasia ossificans progressiva: A comprehensive global assessment. J Bone Miner Res 2016;31:650-6.
6. Pignolo RJ, Baujat G, Brown MA, DeCunto C, DiRocco M, Hsiao EC, et al. Natural history of fibrodysplasia ossificans progressiva: Cross-sectional analysis of annotated baseline phenotypes. Orphanet J Rare Dis 2019;14:98.
7. Kaplan FS, Pignolo RJ, Shore EM. Granting immunity to FOP and catching heterotopic ossification in the act. Semin Cell Dev Biol 2016;49:30-6.
8. Convente MR, Chakkalakal SA, Yang E, Caron RJ, Zhang D, Kambayashi T, et al. Depletion of mast cells and macrophages impairs heterotopic ossification in an ACVR1 (R206H) mouse model of fibrodysplasia ossificans progressiva. J Bone Miner Res 2018;33:269-82.
9. Wang H, Lindborg C, Lounev V, Kim JH, McCarrick-Walmsley R, Xu M, et al. Cellular hypoxia promotes heterotopic ossification by amplifying BMP signaling. J Bone Miner Res 2016;31:1652-65.
10. Wang H, Behrens EM, Pignolo RJ, Kaplan FS. ECSIT links TLR and BMP signaling in FOP connective tissue progenitor cells. Bone 2018;109:201-9.
11. Pignolo RJ, Durbin-Johnson BP, Rocke DM, Kaplan FS. Joint-specific risk of impaired function in fibrodysplasia ossificans progressiva (FOP). Bone 2018;109:124-33.
12. Kaplan FS, Zasloff MA, Kitterman JA, Shore EM, Hong CC, Rocke DM. Early mortality and cardiorespiratory failure in patients with fibrodysplasia ossificans progressiva. J Bone Joint Surg Am 2010;92:686-91.
13. Kaplan FS, Pignolo RJ, Al Mukaddam MM, Shore EM. Hard targets for a second skeleton: Therapeutic horizons for fibrodysplasia ossificans progressiva (FOP). Expert Opinion Orphan Drugs 2017;5:291-4.
14. Kaplan FS, Al Mukaddam M, Baujat G, Brown M, Cali A, Cho TJ, et al. The medical management of fibrodysplasia ossificans progressiva: Current treatment considerations. Proc Int Clin Council FOP 2019;1:1-111.
15. Moriatis JM, Gannon FH, Shore EM, Bilker W, Zasloff MA, Kaplan FS. Limb swelling in patients who have fibrodysplasia ossificans progressiva. Clin Orthop Rel Res 1997;336:247-53.
16. Perron AD, Brady WJ, Keats TE. Orthopedic pitfalls in the ED: Acute compartment syndrome. Am J Emerg Med 2001;19:413-6.
17. Melamed E, Angel D. Myositis ossificans mimicking compartment syndrome of the forearm. Orthopedics 2008;31:32936.
18. Ojike NI, Roberts CS, Giannoudis PV. Compartment syndrome of the thigh; a systematic review. Injury 2010;41:133-6.
19. Al Mukaddam M, Rajapakse CS, Pignolo RJ, Kaplan FS, Smith SE. Imaging assessment in fibrodysplasia ossificans progressiva: Qualitative, quantitative and questionable. Bone 2018;109:147-52.
20. Kaplan FS, Al Mukaddam M, Pignolo RJ. Acute unilateral hip pain in fibrodysplasia ossificans progressiva (FOP). Bone 2018;109:115-9.
21. Chakkalakal SA, Zhang D, Culbert AL, Convente MR, Caron RJ, Wright AC, et al. An acvr1 knock-in mouse has fibrodysplasia ossificans progressiva. J Bone Miner Res 2012;27:1746-56.
22. Kaplan FS, Chakkalakal SA, Shore EM. Fibrodysplasia ossificans progressiva: Mechanisms and models of skeletal metamorphosis. Dis Model Mech 2012;5:756-62.
23. van den Brand JG, Nelson T, Verleisdonk EJ, van der Werken C. The diagnostic value of intracompartmental pressure measurement, magnetic resonance imaging, and near-infrared spectroscopy in chronic exertional compartment syndrome: A prospective study in 50 patients. Am J Sports Med 2005;33:699-704.
 |
 |
 |
| Dr. Frederick S. Kaplan | Dr. Mona Al Mukaddam | Dr. Robert J. Pignolo |
| How to Cite This Article: Kaplan FS, Al Mukaddam M, Pignolo RJ. Compartment Syndrome of the Thigh in a Patient with Fibrodysplasia Ossificans Progressiva Journal of Orthopaedic Case Reports 2020 May-June;10(3):103-107. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com