[box type=”bio”] Learning Point of the Article: [/box]
The key elements in management of polytrauma patient with complex fractures are proper staging and good implant choice.
Case Report | Volume 10 | Issue 3 | JOCR May – June 2020 | Page 95-99 | Amr Ahmed Hosny Abdo Selim, Nader M Diab, Ahmed S Barakat. DOI: 10.13107/jocr.2020.v10.i03.1766
Authors: Amr Ahmed Hosny Abdo Selim[1], Nader M Diab[1], Ahmed S Barakat[1]
[1]Department of Trauma and Orthopaedic Surgery, Faculty of Medicine, Cairo University, Giza, Egypt.
Address of Correspondence:
Dr. Amr Ahmed Hosny Abdo Selim,
Department of Trauma and Orthopaedic Surgery, Faculty of Medicine, Cairo University, Giza, Egypt.
E-mail: amrhosny70@gmail.com/amr.selim@nhs.net
Abstract
Introduction: Femoral neck fractures can complicate by non-union and/or hip avascular necrosis (AVN); moreover, the incidence of AVN remains obscure when it is accompanied by an ipsilateral acetabular fracture. Measures to reduce non-union or hip AVN with this complex injury pattern are not well addressed in the literature.
Case Report: We report a case of a young male patient who sustained ipsilateral acetabular, femoral neck, and shaft fractures in addition to a contralateral floating knee injury following a motor vehicle collision. To the best of our knowledge, this is the first report that describes the simultaneous occurrence of these fractures and their management. The patient attained an excellent functional outcome with union of all his fractures. We, therefore, propose a management flowchart for this rare case scenario.
Conclusion: The acute management of ipsilateral femoral shaft and neck fractures in such cases has to be prioritized. The use of a retrograde nail in addition to dynamic hip screw (DHS) with two cannulated anti-rotation screws and locking the DHS to the nail is likely to increase the healing potential of femoral neck fracture in these cases. Acetabular fixation is better to be performed in a second stage after the hyper-inflammation phase ends. The definitive management for the contralateral floating knee can be delayed to a third stage but should be completed within the 10-day limit of immunosuppression.
Keywords: Floating hip, polytrauma, floating knee, avascular necrosis.
Introduction
The concomitant occurrence of ipsilateral femoral neck, shaft, and acetabular fractures is uncommon and is usually caused by a significant high-energy trauma mechanism [1, 2, 3, 4, 5, 6, 7, 8, 9]. Moreover, the simultaneous occurrence of contralateral floating knee injury in the same patient is very rare. Despite the obvious technical and scientific progress in the past decades in treating fracture neck femur in young adults, the incidence of the most feared complications, namely, non-union and avascular necrosis still remains high and is reported to vary between 15% and 25%. They depend on various factors as fracture configuration, biological age, timing, and fixation technique applied [10]. Here, we present a case and its management of ipsilateral acetabular, femoral neck, and shaft fractures in addition to contralateral floating knee injury following a motor vehicle collision (MVC). This is the first report to describe the management of such an intricate injury.
Case Report
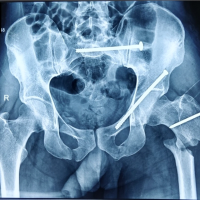
A 23-year-old man sustained an MVC and presented to our hospital emergency department with fractures of the left acetabulum, left neck of femur, left shaft femur, right shaft femur, and right shaft tibia. On arrival, the patient was agitated and in severe pain despite having received an IV morphine injection and being placed in an inflatable anti-shock trouser during his ambulance transport from the accident site to our tertiary trauma center. During the transport, 500 ml of normal saline were administered. After instigating advanced trauma life support, no other cerebral, spinal, neurovascular, or chest trauma could be verified by examination and polytrauma multislice computed tomography (CT). However, the multislice CT revealed a spleen contusion measuring 2 cm in its widest diameter and the patient had superficial abrasions on his left cheek and forehead. His vital signs were heart rate 118 bpm, blood pressure 90/55, respiratory rate 24/min, and temperature 36.5°C. His laboratories showed normocytic normochromic anemia with hemoglobin 8.8 g/dl and a pH of 7.41. The abbreviated injury score was 7, and therefore, the injury severity score amounted to 21. While in the emergency department, 1 L of normal saline was administered as a bolus followed by two packed red blood cells (RBC) units and two fresh frozen plasma units. Skin traction was applied to the left side and Thomas splint with an above knee back slab was applied to the right side. While still in the ER and in concordance with the abdominal trauma surgeon, it was decided to treat the 2 cm spleen contusion conservatively. The patient was admitted to a surgical intensive care unit (ICU) and remained there till the 1st post-operative day of the final operation. Radiographs showed fractures of the left acetabulum, left femoral neck (Garden IV) (AO/OTA 31B3), left femoral shaft (AO/OTA 32B3), right femoral shaft (AO/OTA 32A3), and right tibial shaft (AO/OTA 42A1). The multislice CT was reformatted and helped further in delineating the acetabular fracture which was of the associated both columns type (AO/OTA 62C2) (Fig. 1).

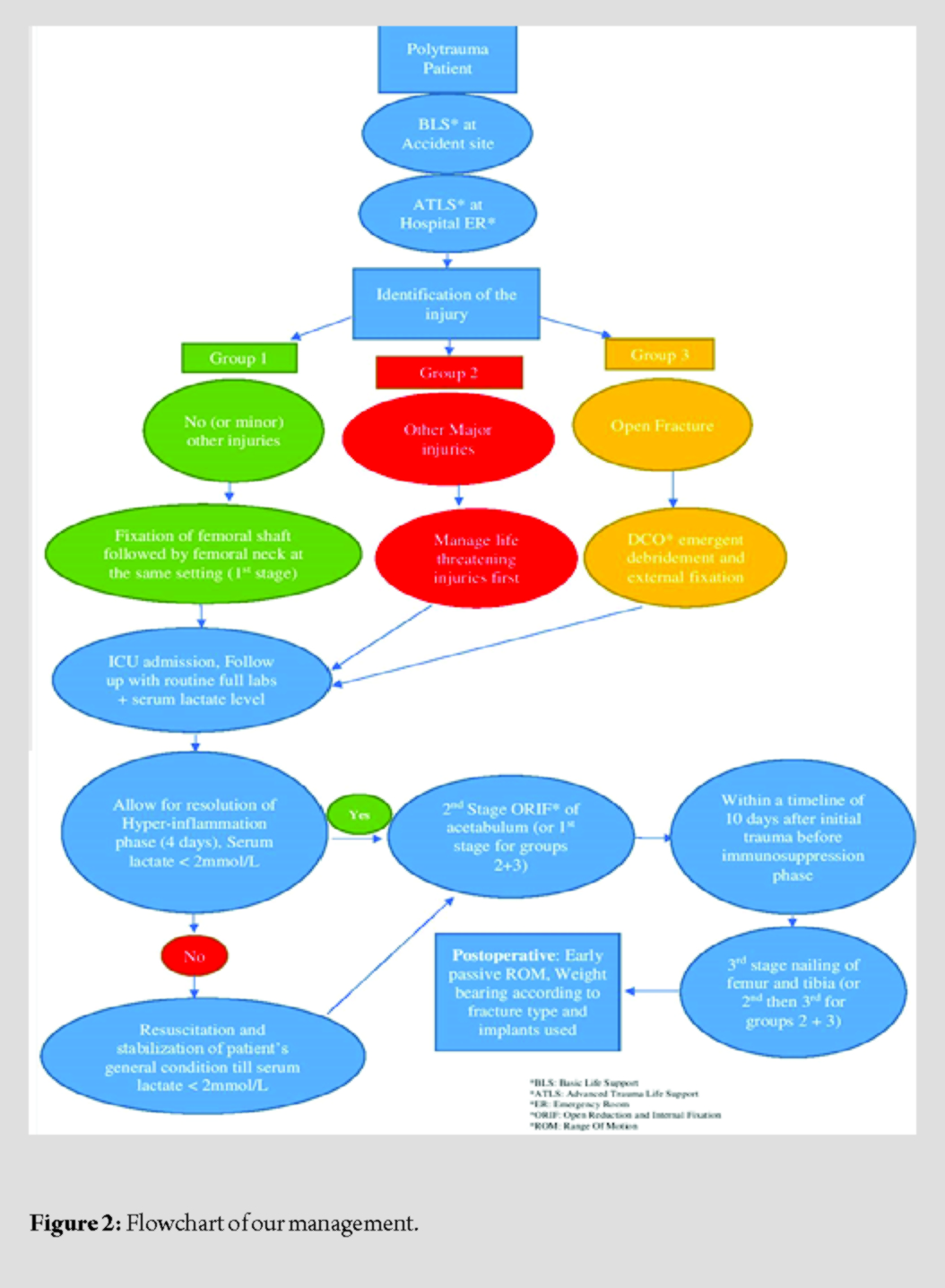
Four hours after admission after stabilization of the general condition and elevation of the hemoglobin to 10.1 g/dl, the patient was transferred to the operating room. He was positioned supine with the left knee semi-flexed to allow for retrograde intramedullary nailing of the left femoral shaft fracture with (12 mm × 34 cm steel retrograde femoral nail, Auxein Medical Pvt. Ltd., Delhi, India). Afterward, he was placed on a traction table, and after closed reduction, stabilization of the left neck femur fracture was performed by a dynamic hip screw (DHS) (135°, 4-hole steel DHS with a 95 mm lag screw, Auxein Medical Pvt. Ltd., Delhi, India) together with two cannulated partially threaded 6.5 mm screws. Moreover, one proximal nail locking screw was applied trough the DHS plate to the nail. The retrograde nail was inserted to the level of the lower border of the lesser trochanter. After having applied the distal locking screws, the lateral proximal drill holes were established with the implant-specific proximal aiming device. After a standard lateral approach to the proximal femur, the 4-hole DHS plate was placed so as to allow for proper placement of the lag screw in the neck and simultaneous overlap of the second DHS plate hole over the now apparent predrilled hole of the retrograde nail. Only three screws were applied to the DHS plate as the fourth was streaking the retrograde nail. The operative time was 4 h, and the estimated intraoperative blood loss was 500 ml. The patient received enoxaparin 40 mg/sc qd, ibuprofen 600 mg bds PO, omeprazole 40 mg IV qd, and ceftriaxone 2 g IV qd for the rest of his hospital stay. The patient-controlled analgesia device with 5 mg/ml of morphine with the patient dose of 2 mg and lockout time of 15 min was used during the first 36 h after each surgery. Five days later, after subsidence of the secondary hit (pH = 7.39, Hb 11.8 g/dl, CRP 59 mg/l, and serum lactate 1.314 mmol/L), the left acetabular fracture was addressed through the ilioinguinal approach and anatomical reduction was achieved by two reconstruction plates. The operative time was 3 h and the estimated intraoperative blood loss was 600 ml. Post-operative laboratories showed a hemoglobin of 9 g/dl, and the patient was given one unit of packed RBCs, elevating the hemoglobin to 9.9 g/dl. Two days later, after stabilization of the general condition, a third operation was performed for the right femoral and tibial shaft fractures. Antegrade closed intramedullary nailing was performed for the right femoral shaft fracture, together with closed intramedullary nailing of the right tibial shaft fracture (12 mm × 36 cm steel femoral interlocking and 11 mm × 33 cm steel tibial interlocking nail, Auxein Medical Pvt. Ltd., Delhi, India). The operative time was 3.5 h, and the estimated operative blood loss was 400 ml (Fig. 2).
The early post-operative period passed uneventfully. Passive and active hip and knee range of motion (ROM) was allowed after each operation as tolerated, sutures were removed 2 weeks after the operation and all wounds healed uneventfully. In the 8th post-operative week, partial weight-bearing was allowed on two crutches, Harris hip score (HHS) of the left hip was 75, callus formation started to appear at the shaft femurs and the shaft tibia, and both knees achieved full active and passive ROM without significant knee pain. In the 12th post-operative week, partial weight-bearing was continued, and HHS of the left hip increased to 80. In the 16th post-operative week, all fractures were fully united, full weight-bearing was allowed and the HHS was 90. The remaining follow-up period was uneventful, and at 1 year, HHS of the left hip reached 95, in addition, both knees achieved full ROM without knee pain (Fig. 3).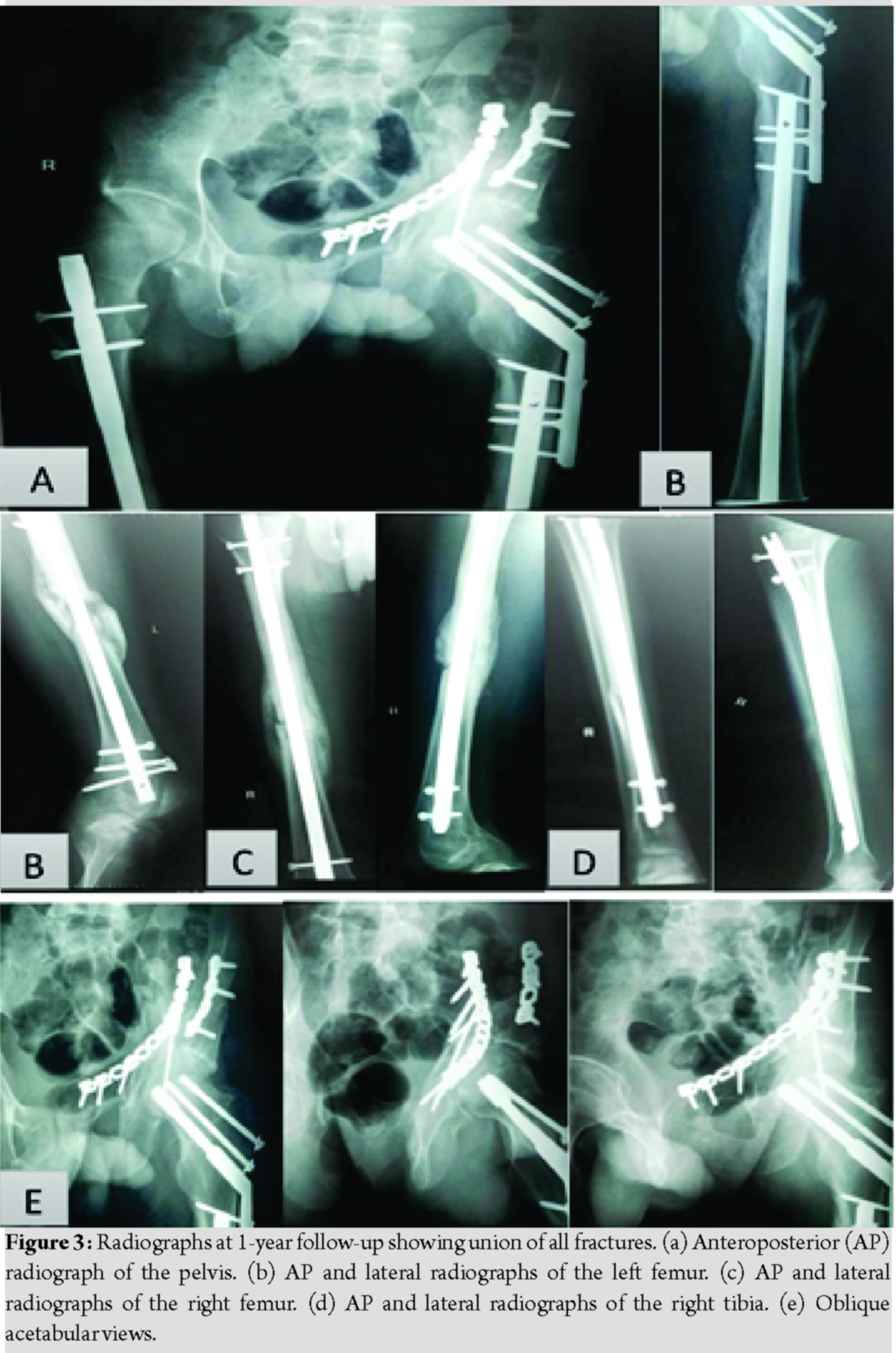
Discussion
Here, we report a case of ipsilateral acetabular, femoral neck, and shaft fractures together with contralateral floating knee injury following an MCV.
Complete radiological union and excellent functional outcome were achieved. We suggest a treatment outline for such complex injury patterns, in which the treatment sequence and timing still remain unclear. To date, only two published case reports have outlined the management of ipsilateral acetabular, femoral neck, and shaft fractures [1, 2, 3]. Irifune et al. recommended primary fixation of the femoral shaft using a retrograde nail followed by the fixation of the femoral neck using three cannulated screws and eventually by acetabular fixation. However, the case was complicated by femoral neck and shaft non-union [1]. Duygulu et al. suggested simultaneous fixation of the femoral neck and shaft using an antegrade reconstruction nail followed by open reduction and fixation of the acetabulum [3]. For the management of isolated floating hip injury, without femoral neck fracture, Kregor and Templeman proposed that fixation of the acetabular fracture should be performed first to protect the hip joint from any damage that may occur during mobilization of the femoral shaft fracture [7]. Nevertheless, Liebergall et al. prioritized fixation of the femoral shaft fracture because they suggested that reduction of the acetabulum would be easier by creating a solid manipulable base [4, 5]. Regarding the management of ipsilateral femoral neck, and shaft fractures, Oh et al. recommended retrograde nailing of the femoral shaft fracture and fixation of the femoral neck using cannulated screws [11]. However, others used an antegrade reconstruction nail for both the shaft and neck fractures [9, 10, 11, 12]. Chavda et al. examined over 52 patients with floating knee injury and recommended that definitive fixation is better to be delayed after stabilization of the general condition; furthermore, intramedullary nailing of both the femoral and tibial shaft fractures had the best outcome [13]. In the underlying case, the floating hip and femoral neck fractures were prioritized. By providing definite primary fixation of the femoral shaft fracture using a retrograde nail and thus creating a stable femoral foundation, femoral neck fracture fixation by a DHS augmented by two anti-rotation cannulated screws can be performed easier and more accurately. The usage of a DHS system with the addition of two anti-rotation screws for the femoral neck fracture instead of three cannulated screws only is biomechanically superior by decreasing micromotion and displacement forces on the femoral neck fracture, particularly if the femoral shaft fracture should unite first [14]. Furthermore, locking the nail to the DHS plate will help to distribute the forces more evenly across the whole femur and reduce the incidence of non-union which is common to segmental fractures. Nevertheless, many authors in light of the concept of damage control orthopedics (DCO) do not recommend to perform definite total fracture fixation in the same setting as this may add a significant harm, or a second hit, to the patient [15]. Other authors, however, claim that definite single-stage fracture fixation in polytraumatized patients is feasible. DCO versus early total care, therefore, constitute a large field for ongoing research and dispute, and clear-cut treatment strategy recommendations are not sufficiently validated or not universally accepted [16]. Achieving early hemostasis is essential in the early management of the polytrauma patient, although aggressive transfusion practices may have a detrimental effect due to fluid shift phenomena, and hence, restricted fluid replacement protocols and the use of vasopressor in the absence of traumatic brain injury have become a widely accepted strategy [17]. Early versus delayed surgical action has often been anchored to acid-base balance and especially serum lactate levels. Other pivotal laboratory markers include hemoglobin and/or hematocrit, fibrinogen, prothrombin time, activated partial thromboplastin time, and platelet count [17]. The second stage consisted of stabilization of the acetabular fracture by open reduction and internal fixation. Ideally, the definite acetabular fixation should be done 4–5 days after the primary operation in the safe window to allow for subsidence of the polytrauma hyper-inflammation phase [18]. The last stage is stabilization of the floating knee injury ideally by closed intramedullary nailing of both the femoral and tibial shaft fractures within 10 days from the date of trauma. It is critical to end the definitive management of all fractures within this timeline before the immunosuppressive phase of polytrauma sets in Vallier [18]. In a single-center study including 155 patients, the occurrence of fever in polytraumatized ICU patients was found to be strongly associated with wound infection, whereas open fractures, surgeries, or abdominal trauma were not [19]. The described patient was admitted in the ICU and kept there in the “clean” section under continuous non-invasive monitoring, nonsteroidal anti-inflammatory drugs, and ceftriaxone 2 g IV QDS since the patient was initially vitally stable and had no other major organ affection except for the spleen contusion. This reflected also in the compulsory interdisciplinary approach for such cases and importance of daily team meetings encompassing intensivists, anesthesiologists, trauma surgeons, and physiotherapists. Zelle et al. claimed that trauma below the knee in polytrauma patients was strongly associated with a poorer functional outcome [20]. Nevertheless, this patient’s functional outcome was excellent, and we explain this by the judicious surgical intervention, the absence of other major organ trauma, the young age of the patient, and the absence of open fractures.
Conclusion
The acute management of ipsilateral femoral shaft and neck fractures in such cases has to be prioritized. The use of a retrograde nail in addition to DHS with two cannulated anti-rotation screws and locking the DHS to the nail is likely to increase the healing potential of femoral neck fracture in these cases. Acetabular fixation is better to be performed in a second stage after the hyper-inflammation phase ends. The definitive management for the contralateral floating knee can be delayed to a third stage but should be completed within the 10-day limit of immunosuppression.
Clinical Message
Management of such complex injuries should be properly staged. Adherence to the updated relevant recommendations in the contemporary literature, a comprehensive interdisciplinary approach, and proper implant choice are decisive in the management of such complex cases.
References
1. Irifune H, Hirayama S, Takahashi N, Narimatsu E. Ipsilateral acetabular and femoral neck and shaft fractures. Case Rep Orthop 2015;2015:351465.
2. Hung SH, Hsu CY, Hsu SF, Huang PJ, Cheng YM, Chang JK, et al. Surgical treatment for ipsilateral fractures of the hip and femoral shaft. Injury 2004;35:165-9.
3. Duygulu F, Calis M, Argun M, Guney A. Unusual combination of femoral head dislocation associated acetabular fracture with ipsilateral neck and shaft fractures: A case report. J Trauma 2006;61:1545-8.
4. Liebergall M, Mosheiff R, Safran O, Peyser A, Segal D. The floating hip injury: Patterns of injury. Injury 2002;33:717-22.
5. Liebergall M, Lowe J, Whitelaw GP, Wetzler MJ, Segal D. The floating hip. Ipsilateral pelvic and femoral fractures. J Bone Joint Surg Br 1992;74:93-100.
6. Müller EJ, Siebenrock K, Ekkernkamp A, Ganz R, Muhr G. Ipsilateral fractures of the pelvis and the femur–floating hip? A retrospective analysis of 42 cases. Arch Orthop Trauma Surg 1999;119:179-82.
7. Kregor PJ, Templeman D. Associated injuries complicating the management of acetabular fractures: Review and case studies. Orthop Clin North Am 2002;33:73-95.
8. Barei DP, Schildhauer TA, Nork SE. Noncontiguous fractures of the femoral neck, femoral shaft, and distal femur. J Trauma 2003;55:80-6.
9. Jain P, Maini L, Mishra P, Upadhyay A, Agarwal A. Cephalomedullary interlocked nail for ipsilateral hip and femoral shaft fractures. Injury 2004;35:1031-8.
10. Han S, Oh M, Yoon S, Kim J, Kim JW, Chang JS, et al. Risk stratification for avascular necrosis of the femoral head after internal fixation of femoral neck fractures by post-operative bone SPECT/CT. Nucl Med Mol Imaging 2017;51:49-57.
11. Oh CW, Oh JK, Park BC, Jeon IH, Kyung HS, Kim SY, et al. Retrograde nailing with subsequent screw fixation for ipsilateral femoral shaft and neck fractures. Arch Orthop Trauma Surg 2006;126:448-53.
12. Watson JT, Moed BR. Ipsilateral femoral neck and shaft fractures: Complications and their treatment. Clin Orthop Relat Res 2002;399:78-86.
13. Chavda AG, Lil NA, Patel PR. An approach to floating knee injury in Indian population: An analysis of 52 patients. Indian J Orthop 2018;52:631-7.
14. Zhang LL, Zhang Y, Ma X, Liu Y. Multiple cannulated screws vs. dynamic hip screws for femoral neck fractures: A meta-analysis. Orthopade 2017;46:954-62.
15. Guerado E, Bertrand ML, Cano JR, Cerván AM, Galán A. Damage control orthopaedics: State of the art. World J Orthop 2019;10:1-3.
16. Bates P, Parker P, McFadyen I, Pallister I. Demystifying damage control in musculoskeletal trauma. Ann R Coll Surg Engl 2016;98:291-4.
17. Rossaint R, Bouillon B, Cerny V, Coats TJ, Duranteau J, Fernández-Mondéjar E, et al. The European guideline on management of major bleeding and coagulopathy following trauma: Fourth edition. Crit Care 2016;20:100.
18. Vallier HA, Wang X, Moore TA, Wilber JH, Como JJ. Timing of orthopaedic surgery in multiple trauma patients: Development of a protocol for early appropriate care. J Orthop Trauma 2013;27:543-51.
19. Steinmetz S, Uçkay I, Cohen C, Abrassart S. Fever and its association with infection in severely injured polytrauma patients. Mathews J Orthop 2016;1:1-11.
20. Zelle BA, Brown SR, Panzica M, Lohse R, Sittaro NA, Krettek C, et al. The impact of injuries below the knee joint on the long-term functional outcome following polytrauma. Injury 2005;36:169-77.
 |
 |
 |
| Dr. Amr Ahmed Hosny Abdo Selim | Dr. Nader M Diab | Dr. Ahmed S Barakat |
| How to Cite This Article: Selim AAHA, Diab NM, Barakat AS. A Rare Case of Ipsilateral Floating Hip with Femoral Neck Fracture and Contralateral Floating Knee Injury – Proposal for a Management Flowchart and Literature Review. Journal of Orthopaedic Case Reports 2020 May-June;10(3): 95-99. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com