[box type=”bio”] Learning Point of the Article: [/box]
Persistent limitation in tendon’s range of motion after trauma might be associated with the presence of intratendinous foreign bodies, potentially surrounded by cystic lesions.
Case Report | Volume 10 | Issue 3 | JOCR May – June 2020 | Page 100-102 | Dimitrios Giotis, Nikolaos K. Paschos, Georgios C. Drosos, Vikram V. Kadu, Michael-Alexander Malahias. DOI: 10.13107/jocr.2020.v10.i03.1768
Authors: Dimitrios Giotis[1], Nikolaos K. Paschos[2], Georgios C. Drosos[1], Vikram V. Kadu[3], Michael-Alexander Malahias[4]
[1]Department of Orthopaedics, General Hospital of Grevena, Region Military Camp, Grevena, Greece,
[2]Department of Orthopaedics and Biomedical Engineering, University of California, Davis, California, United States,
[3]Sancheti Institute of Orthopaedics and Rehabilitation, Pune, Maharashtra, India,
[4]Department of Orthopaedic, HYGEIA Hospital, Marousi, Athens, Greece.
Address of Correspondence:
Dr. Vikram Kadu,
Orthopaedic Surgeon, Sancheti Institute of Orthopaedics and Rehabilitation, Pune, Maharashtra, India.
E-mail: vikram1065@gmail.com
Abstract
Introduction: Intratendinous epidermal cysts are extremely rare soft-tissue lesions. Apart from traumatic occasions which are usually painful, in asymptomatic cases, they can be easily overlooked. The purpose of our study was to report the formation of an intratendinous epidermoid cyst after traumatic penetration and irritation of a wooden foreign body.
Case Report: A 79-year-old man proceeded in the emergency department, with a skin cut in the dorsal side of the right hand from a sharp wooden segment. After surgical lavage and investigation for soft-tissue damages or subcutaneous foreign bodies, skin closure was performed. Ten months after trauma, the patient came again with persistent pain and limitation in range of motion of the ring finger. Ultrasonography demonstrated an intratendinous foreign body surrounded by the cystic lesion. Both the identified wooden fragment and the cyst, which were histopathologically verified as an epidermoid cyst, were removed.
Conclusion: Clinicians should be aware that a tendon injury, along with chronic irritation from a foreign body, might result in the formation of an intratendinous epidermoid cyst.
Keywords: Epidermoid cyst, Foreign body, Intratendinous cyst, Case report.
Introduction
Epidermoid cysts are typically benign intradermal or subcutaneous tumors which are most commonly diagnosed in scalp, face, trunk, and extremities. They mostly regard hair-bearing areas [1, 2]. The occurrence of these cysts in anatomic regions without hair could be attributed to implantation and the proliferation of squamous epithelium into the dermis after trauma [1, 2]. Almost solely ganglion cysts are reported in the literature as intratendinous masses [3, 4, 5]. Intratendinous epidermal cysts are only sporadically mentioned [6, 7]. To the best of our knowledge, there is only one case report published regarding an intratendinous epidermoid cyst after trauma [8]. The purpose of our study was to present the first-ever reported case regarding the formation of an epidermal cyst within the extensor digitorum tendon of the ring finger after the traumatic intrusion of a wooden foreign body.
Case Report
A 79-year-old man proceeded in the emergency department with skin cut 2 x 1.5 cm in the dorsal side of the right hand from a sharp wooden segment during logging. After surgical lavage and exploration for soft-tissue damages or subcutaneous foreign bodies (under local anesthesia), it was found that both the extensor digitorum tendons and the neurovascular structures of the dorsal hand were intact. No foreign body was identified. Thus, a skin closure with polypropylene non-absorbable sutures was performed. Antitetanic serum injection at once and antibiotics (cefuroxime 500 mg) for 7 days was given to the patient. Two weeks postoperatively, following sutures removal, there was no sign of local pain, skin irritation, edema, or inflammation. However, 2 months post-traumatically, the patient returned to the hospital with mild pain and local swelling over the traumatized area. No neurovascular or functional deficits were diagnosed. Laboratory tests did not reveal any sign of infection, while the X-ray control was negative for bone lesions or the existence of foreign bodies. The patient was treated with non-steroidal anti-inflammatory drugs for 5 days. One week later, the patient was almost free of symptoms.
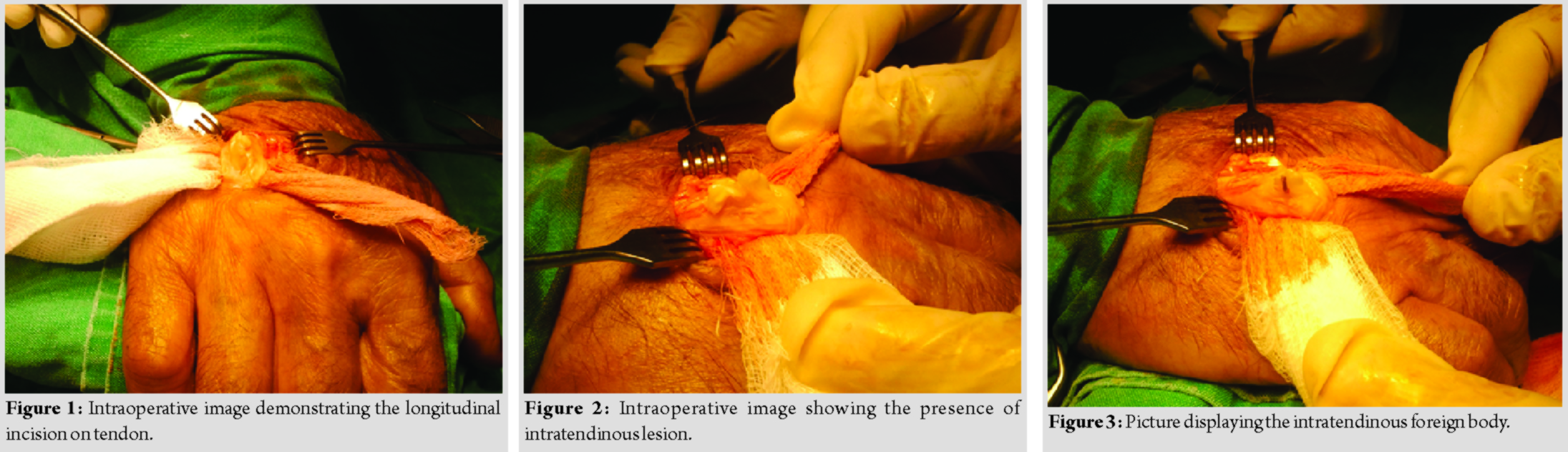
Ten months after the initial injury, the patient visited again the orthopedic department displaying limitation in the range of motion (RoM) of the right ring finger and persistent deteriorating pain, both in extension and flexion. The clinical examination demonstrated a palpable mass at the route of the common extensor tendon of the fourth finger. An ultrasonographic (U/S) evaluation revealed the presence of a well-defined hypoechoic cystic mass within the tendon, surrounding an echogenic lesion 0.6 x 0.2 cm, presumably intratendinous foreign body. A surgical investigation was executed, initially with a longitudinal skin incision just above the U/S finding. No sign of any tendon inflammation was observed. Taking care not to critically damage the tendon, a longitudinal incision on the dorsal surface of the tendon was carried out. An intratendinous cystic lesion was revealed (Fig. 1, 2). The thickness of the cyst wall was measured around 0.2 cm. Afterward, a cyst incision revealed the existence of a small wooden piece, which was removed along with the cystic layer [Fig. 3]. The dimensions of the foreign body were identical with those of the pre-operative sonographic measurement. As the last step, the tendon was carefully repaired, and trauma was closed in layers. The post-operative histopathological examination illustrated the presence of a cyst filled with keratinous material and lined with stratified non-keratinized squamous epithelium diagnosed as an epidermoid cyst. The accelerated rehabilitation protocol included passive RoM of the involved finger for 10 days followed by progressive active mobilization for another 2 weeks. Three weeks postoperatively, the patient was free of symptoms without any functional deficits, managing to fully restore the normal RoM, and return to proinjury daily activities.
Discussion
The most important finding of our study was that it presented the first-ever reported case of an intratendinous epidermal cyst caused by the existence of a foreign body after trauma. There is one sole similar article reported by O’Hara and Stone [8], demonstrating the appearance of intratendinous epidermoid cyst after tendon traumatic damage. Concerning our case, the intratendinous epidermal cyst was caused by another extremely rare entity, the intratendinous penetration, and maintenance of foreign material [9]. Soft-tissue penetration of foreign bodies is commonly the outcome of laceration injuries [10]. Foreign material in tendons can be organic, wood, glass, metal, plastic, or gravel [9, 10]. They can be asymptomatic and undiagnosed [10] or they are likely to cause problems such as purulent tendonitis, fibrosis, peritendinitis, foreign body granuloma, infection, calcification, or necrosis [9]. If we exclude metal foreign bodies, most of the other materials are radiolucent, a fact that makes their detection relatively difficult [10]. In such cases, a high-resolution, real-time U/S as a non-invasive, non-radiated, low-cost technique can accurately localize the foreign material with a sensitivity and specificity of more than 90% [11, 12]. The most frequent intratendinous cystic lesions are ganglionic cysts, which originate within the tendon substance itself and cause soft-tissue swelling [13, 14]. They are thought to develop from the mucoid degeneration of connective tissue caused by chronic irritation or chronic repetitive injury [2, 3, 4, 5]. Regarding the formed intratendinous epidermoid cyst, its etiology is unclear and cannot be attributed to certain causes. The only O’Hara and Stone had correlated the formation of these lesions with trauma [8]. Similarly, in our case, tendon injury, along with chronic irritation from the foreign body, might be associated with the formation of the cyst, which entrenched the wooden remnant. On the other hand, when there is no traumatic history, the occurrence of intratendinous epidermal cysts might be connected to the congenital anomaly [6, 15]. As presented in our case, these cysts might be painful or interfere with mechanical symptoms, and their removal usually leads to resolution of the symptoms [6, 8, 15].
Conclusion
Intratendinous epidermoid cysts are very rare soft-tissue lesions, which can be the outcome of overlooked intratendinous foreign bodies. Clinicians should be aware that a tendon injury, along with chronic irritation from a foreign body, might result in the formation of an intratendinous epidermoid cyst.
Clinical Message
Clinicians must be aware of cases where persistent limitation in tendon’s RoM after trauma might be associated with the presence of intratendinous foreign bodies. In such cases, the occurrence of cystic lesions surrounding the foreign body could not be excluded from the study.
References
1. Pehlivan M, Özbay PÖ, Temur M, Yilmaz Ö, Gümüs Z, Güzel A. Epidermal cyst in an unusual site: A case report. Int J Surg Case Rep 2015;8C:114-6.
2. Nigam JS, Bharti JN, Nair V, Gargade CB, Deshpande AH, Dey B, et al. Epidermal cysts: A clinicopathological analysis with emphasis on unusual findings. Int J Trichology 2017;9:108-12.
3. Robinson C, Kocialkowski C, Bhosale A, Pillai A. Intratendinous ganglion cyst of the extensor digitorum longus tendon: A case report. Foot (Edinb) 2016;27:46-9.
4. Lee HJ, Kim PT, Chang HW. Intratendinous ganglion of the extensor tendon of the hand. Hand Surg 2015;20:316-8.
5. Endo J, Yamaguchi S, Sasho T. Tendoscopic excision of an intratendinous ganglion in the flexor hallucis longus tendon: A case report. J Foot Ankle Surg 2016;55:345-7.
6. Saito H, Tajima T, Watanabe H, Yamamoto H. An epidermoid cyst of the tendon. J Hand Surg Am 1979;4:448-50.
7. Berkheiser SW. Epithelial inclusion cysts (epidermoid) of tendon. Guthrie Clin Bull 1955;24:147-9.
8. O’Hara JJ, Stone JH. An intratendinous epidermoid cyst after trauma. J Hand Surg Am 1990;15:477-9.
9. Jozsa L, Reffy A, Demel S, Balint JB. Foreign bodies in tendons. J Hand Surg Br 1989;14:84-5.
10. Budhram GR, Schmunk JC. Bedside ultrasound AIDS identification and removal of cutaneous foreign bodies: A case series. J Emerg Med 2014;47:e43-8.
11. Jacobson JA, Powell A, Craig JG, Bouffard JA, Van Holsbeeck MT. Wooden foreign bodies in soft tissue: Detection at US. Radiology1998;206:45-8.
12. Bray PW, Mahoney JL, Campbell JP. Sensitivity and specificity of ultrasound in the diagnosis of foreign bodies in the hand. J Hand Surg Am 1995;20:661-6.
13. Seidman GD, Margles SW. Intratendinous ganglia of the hand. J Hand Surg Am 1993;18:707-10.
14. Jose J, O’Donnell K, Lesniak B. Symptomatic intratendinous ganglion cyst of the patellar tendon. Orthopedics 2011;34:135.
15. Nahra ME, Bucchieri JS. Ganglion cysts and other tumor related conditions of the hand and wrist. Hand Clin 2004;20:249-60.
 |
 |
 |
 |
 |
| Dr. Dimitrios Giotis | Dr. Nikolaos K. Paschos | Dr. Georgios C. Drosos | Dr. Vikram V. Kadu | Dr. Michael-Alexander Malahias |
| How to Cite This Article: Giotis D, Paschos NK, Drosos GC, Kadu VK, Malahias M. Intratendinous Epidermoid Cyst After Traumatic Penetration of Foreign Body: A Very Rare Case Report. Journal of Orthopaedic Case Reports 2020 May-June;10(3): 100-102. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




