[box type=”bio”] Learning Point of the Article: [/box]
Calcific tendonitis of the elbow is a rare condition and awareness about it, as a possible cause of refractory elbow pain must be essential, so as to reach to an early diagnosis. Surgical evacuation of the calcified material in resistant cases leads to full recovery.
Case Report | Volume 10 | Issue 5 | JOCR August 2020 | Page 57-60 | Raju Vaishya, G. I. Siddalingeshwara, Abhishek Vaish. DOI: 10.13107/jocr.2020.v10.i05.1838
Authors: Raju Vaishya[1], G. I. Siddalingeshwara[1], Abhishek Vaish[1]
[1]Department of Orthopaedics, Indraprastha Apollo Hospital, New Delhi, India.
Address of Correspondence:
Dr. Abhishek Vaish,
Attending Consultant Orthopaedics, Indraprastha Apollo Hospitals, Sarita Vihar, New Delhi, India.
E-mail: drabhishekvaish@gmail.com
Abstract
Introduction: Calcific tendonitis occurs most commonly in the shoulder, and it is a rare entity in other parts including the elbow. We report a symptomatic case of calcific tendonitis of common extensor origin of the non-dominant elbow in a young female.
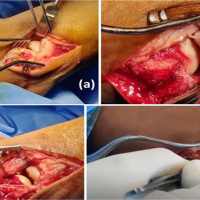
Case Presentation: A 39-year-old female (right hand dominant) presented with the left elbow pain for the past 1 year. The diagnosis was achieved by radiography and confirmed by histopathology. Her pain did not respond to conservative treatment of analgesics, physiotherapy, and elbow support and a local steroid injection. She, therefore, underwent surgical exploration of the elbow, under general anesthesia. There was white-colored paste like a collection within the common extensor tendon origin, with dystrophic calcification of the tendon. The histology of the excised tissue revealed focal nodular aggregates of plump fibroblasts and osteoclastic giant cells around microcalcific foci. Large areas of fibrosis and calcific nodular deposits seen suggestive of calcific tendonitis.
Conclusion: Calcific tendonitis is not a common condition around elbow joint. The diagnosis may be delayed due to its rarity. Hence, a high degree of suspicion in the absence of trauma, along with relevant investigations, leads to a definitive diagnosis and treatment. A review of literature also becomes important since it is not a day-to-day case.
Keywords: Calcific tendonitis, Elbow, Lateral epicondylitis, common extensor origin, tennis elbow, dystrophic calcification.
Introduction
Calcific tendinitis frequently occurs in the shoulder, and its incidence is about 2.7% in the adult population[1]. While it may also occur in other joints such as hip, knee, wrist, and finger joints, its occurrence in elbow joint is relatively rare. Only 6 out of 329 cases of calcific tendonitis occurred in the elbow[2]. Due to its rarity, it is quite vulnerable for delayed diagnosis or misdiagnosis at first instance. The treatment of calcific tendonitis is usually conservative, including nonsteroidal anti-inflammatory drugs (NSAIDs), rest, immobilization of the elbow, physiotherapy, and local steroid injection. When conservative therapy fails, needle aspiration or surgery is considered. Calcific tendonitis of the elbow is extremely rare condition, which is not known to many orthopedic surgeons. Awareness about it is essential to make a correct diagnosis and plan management. Here, we presented such a rare case of calcific tendinitis of the elbow, in an adult female and reviewed the literature related to this problem.
Case Report
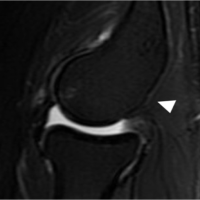
A 39-year-old female (right hand dominant) presented with the left elbow pain for the past 1 year. There was no history of any associated injury to the elbow. Local examination revealed tenderness over the lateral epicondyle of humerus and Cozen’s test was positive, suggesting the clinical diagnosis of lateral epicondylitis of the elbow. The plain radiograph showed heterotopic bone formation, in the region of lateral humeral epicondyle (Fig. 1). Magnetic resonance imaging (MRI) revealed hypointense signal at the region of common extensor tendon origin, on T1/STIR images (Fig. 2). Non-contrast computed tomography (NCCT) showed a well-corticated calcified density at the common extensor tendon origin in the proximity to the lateral humeral epicondyle common extensor tendon origin (Fig. 3), suggestive of calcific common extensor tendinosis. Since there was a bony mass noted around the lateral epicondylar region of the elbow, the CT and MRI scans were done to rule out the extent and characteristic of this lesion and to rule out any sinister pathology like malignancy.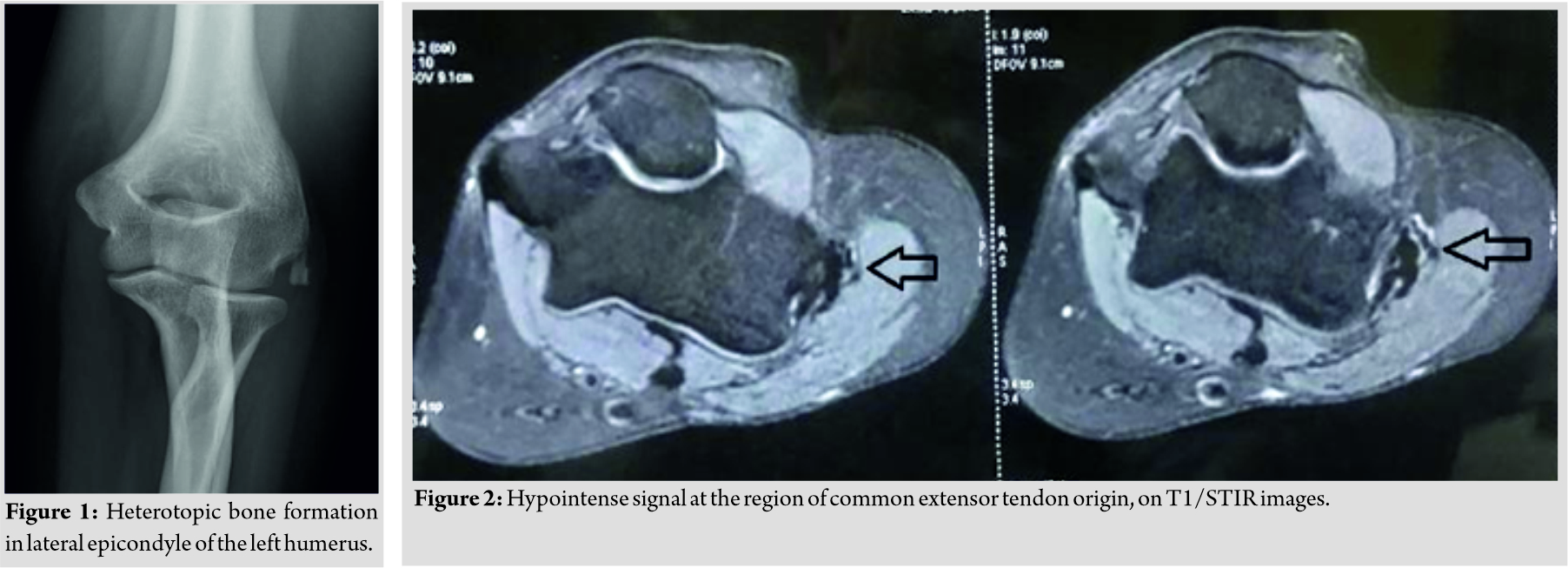
The patient had a trial conservative treatment, for almost 1 year. His visual analog score (VAS) before surgery was 7/10.Her pain did not respond to conservative treatment of analgesics, physiotherapy, and elbow support. Hence, she had a local steroid injection of triamcinolone 20mgwhich was given in the lateral epicondylar area. It helped her for about 3 months, but then pain recurred more intensely, to the extent that she could not use her left upper limb to do the activities of daily living and her night sleep was also disturbed. She, therefore, underwent surgical exploration of the elbow, under general anesthesia. There was white-colored paste like a collection (Fig. 4) within the common extensor tendon origin, with dystrophic calcification of the tendon (Fig. 5). Decompression of the involved tendons was done, and dystrophic calcification was debrided, thoroughly. The split tendon was then repaired using 3-0 Vicryl sutures. The elbow was kept in a broad arm sling for 2 weeks, followed by active physical therapy. The Gram stain of the collected material was negative, and there was no microorganism grown on aerobic culture. The histology of the excised tissue revealed focal nodular aggregates of plump fibroblasts and osteoclastic giant cells around microcalcific foci(Fig. 7). Large areas of fibrosis and calcific nodular deposits seen. The post-operative plain radiograph showed complete abolition of the heterotopic bony growth from the lateral epicondylar region (Fig. 6).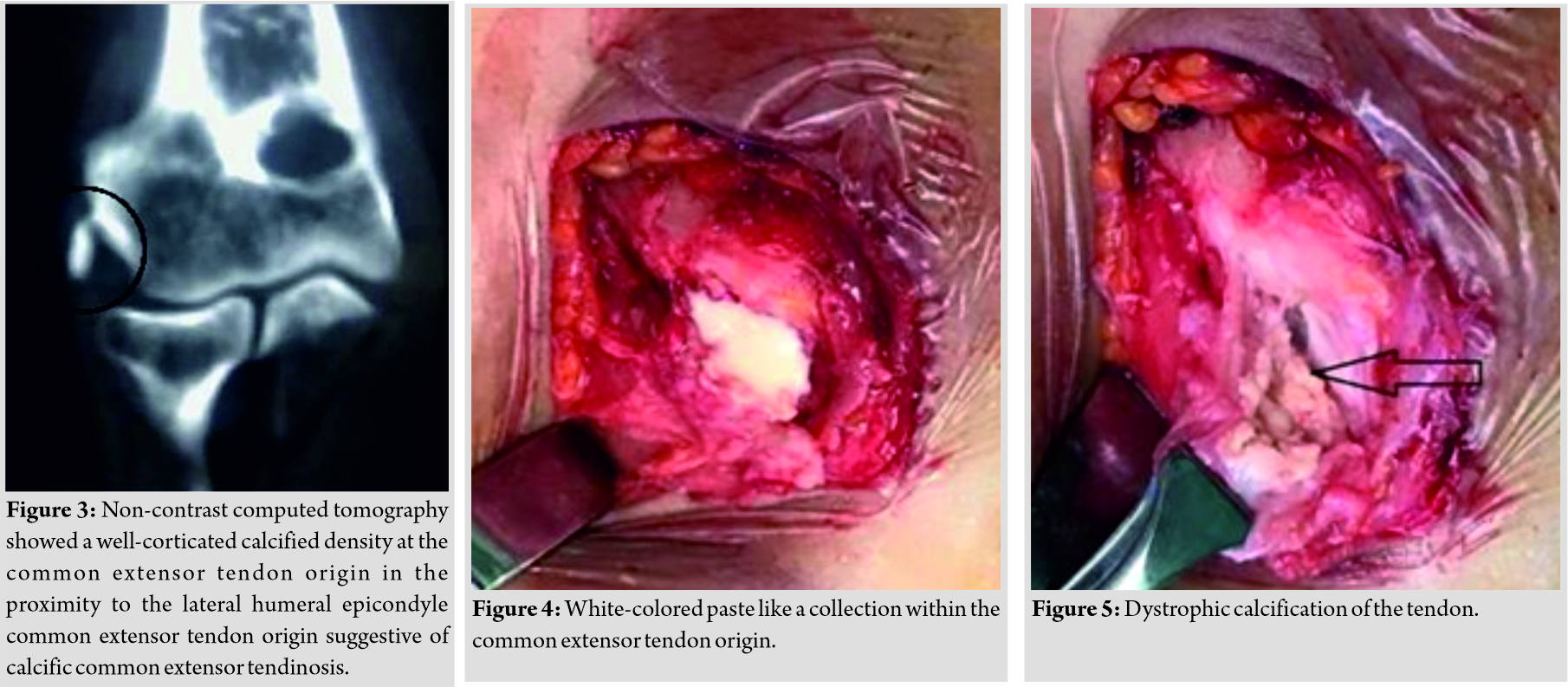
The patient had complete abolition of the elbow pain (VAS score 0/10) and at the follow-up of 12 months, had no pain and full function of the elbow. The radiographs also did not show any recurrence of heterotopic bone formation around the elbow joint.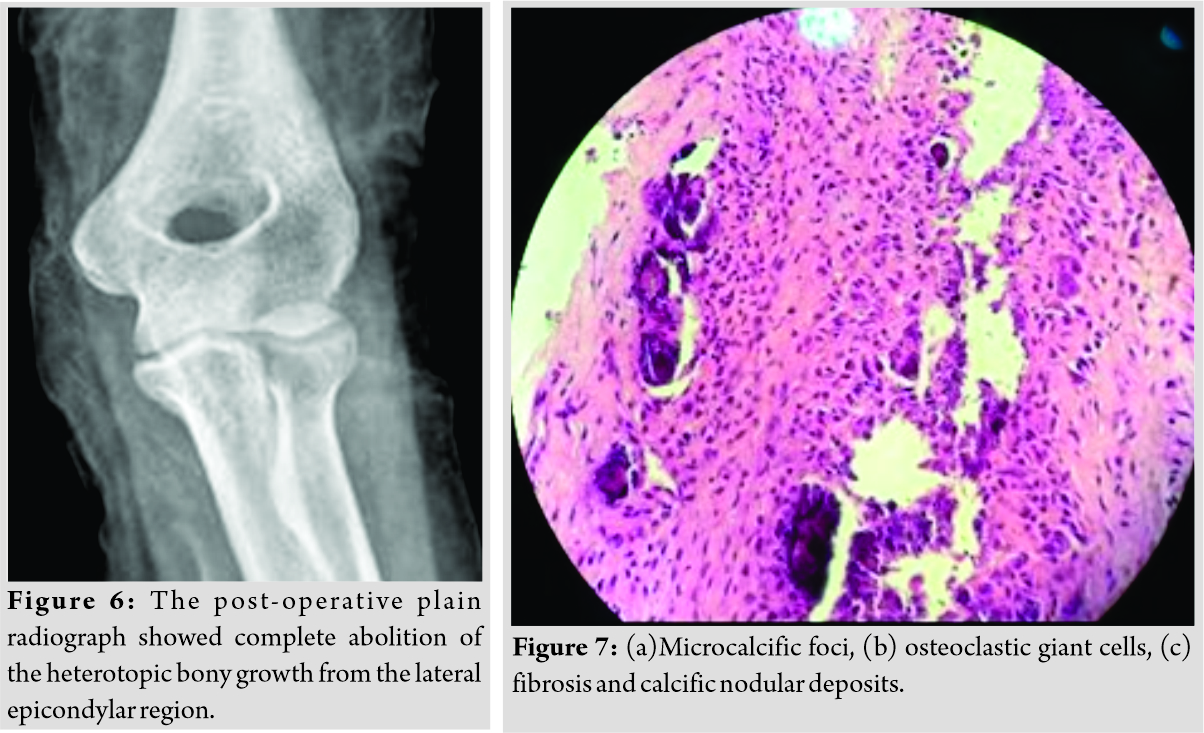
Discussion
Calcific tendonitis is known to occur frequently in the shoulder, and it mostly involves a single joint. Its prevalence is highly variable (3–22% in the general population), depending on the location within the body [3]. The involvement of the elbow joint is extremely rare [2]. Due to paucity of large series on such cases, exact incidence of involvement of the elbow joint is not known, in the literature. In this condition, calcium deposits tend to occur in the tendons, ligaments, capsules of the joint, and surrounding connective tissues [2]. Sandstrom divided the course of calcific tendonitis into acute, chronic, and latent forms [4]. Our patient had type I calcification, as per Gartner and Heyer classification. Acute cases are associated with acute pain, swelling, tenderness, restricted mobility, and fever sometimes. Calcium deposits though seen in radiographs may finally absorb spontaneously. One-third of these cases may give a history of trauma [5]. The radiographic features of ossified calcification around the lateral epicondylar regionmay confuse these lesions with an avulsion fracture from the lateral humeral condyle, as was apparent in this case on radiographs. The chronic cases may present with less inflammation and a long history of the disease, similar to our case. Calcific tendinitis may be diagnosed by plain radiographs if the calcification is significant and matured. The computed tomography (CT) and magnetic resonance imaging (MRI) may help in reaching the diagnosis if the plain radiographs are non-conclusive. Calcific tendonitis is a cell-mediated disease in which metaplastic transformation takes place into chondrocytes subsequently inducing calcification. Several theories have been suggested for its etiopathogeneses such as ischemia [5], degeneration [6], and involvement of factors such as anti-inflammatory agents, metabolic disorders, and genetic predisposition [7]. We believe that degeneration in the common extensor origin tendon was responsible for the calcification in our case. There are several treatment options for this condition. These include conservative management such as NSAIDs, orally administered cimetidine[8], rest, immobilization of the affected joint, and local steroid injection. Other treatment options include needle aspiration of calcium deposits [9], shockwave therapy [10], and surgical excision. Steroidal injections may be helpful in acute cases, but repetitive injections should be avoided as it may lead to adverse effects such as tendon rupture, post-injection pain, subcutaneous atrophy, and skin pigmentation. High recurrence (37%) at 1 year has been reported in patients with lateral epicondylitis who underwent local steroid injection [11]. Recently, oral administration ofcimetidine has been studied in which calcium deposits disappeared in 56% of patients, decreased by 25%, did not change in only 19% of patients. Although a detailed mechanism of the action of cimetidine on periarticular calcifications remains to be understood, it appears to be beneficial in such cases. Cimetidine is supposed to act on PTH and promotes absorption of calcium deposits and also has an anti-inflammatory analgesic action [8]. However, it requires long-term study for side effects of the drugs and treatment response. Percutaneous aspiration is helpful only in soft calcifications [12]. Shockwave therapy is a newer modality but lacks efficacy in the complete removal of deposits [10]. Surgery is indicated in chronic and refractory cases. It may overcome the drawbacks of the non-operative treatments, as it allows complete removal with adequate sample collection for histopathological examination and may be associated with reduced recurrence rate. We suggest that the surgical evacuation of the calcific deposits, if proven by appropriate imaging like MRI.
Conclusion
Calcific tendonitis is not a common condition around the elbow joint, and hence, its diagnosis may be delayed due to its rarity. A high degree of suspicion and awareness about this entity is required to reach an early diagnosis and offer treatment.
Clinical Message
Calcific tendonitis is a rare entity around the elbow. Hence, its diagnosis may be missed or delayed. Awareness about this condition would help in reaching to prompt diagnosis and proper treatment. Surgical removal of the dystrophic calcification is required in chronic responding cases, as it may offer a complete resolution of the symptoms and reduce the recurrence rate.
References
1. Bosworth BM. Calcium deposits in the shoulder and subacromial bursitis: A survey of 12, 122 shoulders. JAMA 1941;116:2477-82.
2. Sandstrom C. Peritendinitis calcarea, a common disease of middle life: Its diagnosis, pathology and treatment. AJR 1938;40:1-21.
3. Holt PD, Keats TE. Calcific tendinitis: A review of the usual and unusual. Skeletal Radiol 1993;22:1-9.
4. McCarthy GM, Carrera GF, Ryan LM. Acute calcific periarthritis of the finger joints: A syndrome of women. J Rheumatol 1993;20:1077-80.
5. Rathbun JB, Macnab I. The microvascular pattern of the rotator cuff. J Bone Joint Surg Br 1970;52:540-53.
6. Refior HJ, Krödel A, Melzer C. Examinations of the pathology of the rotator cuff. Arch Orthop Trauma Surg 1987;106:301-8.
7. Harvie P, Pollard TC, Carr AJ. Calcific tendinitis: Natural history and association with endocrine disorders. J Shoulder Elbow Surg 2007;16:169-73.
8. Kimura H, Iwamoto T, Oki S, Matsumura N, Nakamura M, Matsumoto M, et al. Chronic calcific periarthritis of the elbow treated by cimetidine administration: Five cases. J Orthop Surg (Hong Kong) May-Aug 2017;25(2):2309499017717193. doi: 10.1177/2309499017717193.
9. Abate M, Salini V, Schiavone C. Ultrasound-guided percutaneous lavage in the treatment of calcific tendinopathy of elbow extensor tendons: A case report. Malays Orthop J 2016;10:53-5.
10. Loew M, Daecke W, Kusnierczak D, Rahmanzadeh M, Ewerbeck V. Shock-wave therapy is effective for chronic calcifying tendinitis of the shoulder. J Bone Joint Surg Br 1999;81:863-7.
11. Smidt N, Van Der Windt DA, Assendelft WJ, Devillé WL, Korthals-de Bos IB, Bouter LM. Corticosteroid injections, physiotherapy, or a wait-and-see policy for lateral epicondylitis: A randomised controlled trial. Lancet 2002;359:657-62.
12. De Zordo T, Ahmad N, Ødegaard F, Girtler MT, Jaschke W, Klauser AS, et al. US-guided therapy of calcific tendinopathy: Clinical and radiological outcome assessment in shoulder and non-shoulder tendons. Ultraschall Med 2011;32:S117-23.
 |
 |
 |
| Dr. Raju Vaishya | Dr. G. I. Siddalingeshwara | Dr. Abhishek Vaish |
| How to Cite This Article: Vaishya R, Siddalingeshwara GI, VaishA. Calcific Tendonitis of the Elbow in an Adult – A Case Report and Review of the Literature. Journal of Orthopaedic Case Reports 2020 August;10(5): 57-60. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com