[box type=”bio”] Learning Point of the Article: [/box]
As Talus is having peculiar blood supply, its body fracture with a medial malleolar fracture (ankle dislocation) should be managed as soon as a diagnosis is made to achieve good functional outcome and with a proper preoperative and postoperative planning complications can be minimized.
Case Report | Volume 10 | Issue 7 | JOCR October 2020 | Page 11-14 | Nagaraj Manju Moger, J Pragadeeshwaran, Sushovan Banerjee, Pradeep Kumar Meena, Ankith K.V, Aman Verma. DOI: 10.13107/jocr.2020.v10.i07.1896
Authors: Nagaraj Manju Moger[1], J Pragadeeshwaran[1], Sushovan Banerjee[1] , Pradeep Kumar Meena[1], Ankith K.V[1], Aman Verma[1]
[1]Department of Orthopaedics, All India Medical Sciences, Rishikesh, Uttarakhand, India.
Address of Correspondence:
Dr. Pradeep Kumar Meena, MS, Department of Orthopaedics,
All India Medical Sciences, Rishikesh, Uttarakhand, India.
E-mail: dr.pradsms@gmail.com
Abstract
Introduction: Combined talar body fracture with a medial malleolar fracture is rare in literature.
Case Presentation: A 30-year-old female presented to our hospital with complaints of pain and swelling over the right ankle joint with difficulty in bearing weight following a motor vehicle accident. Investigation showed talar body fracture of type 2 Sneppen (classification) with an ipsilateral medial malleolar fracture. Fractured talus was openly reduced with the help of reduction clamp and appropriate sized Herbert screw applied to hold the reduction. The medial malleolar fracture was fixed with an appropriate-sized cannulated cancellous screw after confirming satisfactory reduction. The patient was followed up for wound complications, AVN changes, early osteoarthritic changes, and functional outcome.
Conclusion: The combined talar body fracture, ankle dislocation with a medial malleolar fracture, should be managed; as soon as, a diagnosis is made to get a good functional outcome, even though the incidence of skin complication, AVN risk, and post-traumatic ankle arthritis could not be predicted even though it was absent in our case.
Keywords: Talar body fracture, Sneppen classification, medial malleolar fracture.
Introduction
Talus fracture is a rare fracture in day-to-day practice, the second common after calcaneum in tarsal bones, with incidence, ranges from 0.1% to 0.85% of all fractures [1]. It requires high energy to cause fracture, such as in case of road traffic accident and fall from height involving forced dorsiflexion of the ankle. Due to its dubious blood supply, the operating surgeon should know the fracture pattern while managing [2]. Depending on the anatomical involvement, it may be neck, body, and head. The incidence of talar neck, head, and body fracture is 50%, 37%, and 13% of talus fracture [3, 4, 5, 6]. Talar body fracture is classified by Sneppens and Fortins, depending on fracture pattern [3]. Combined talar body fracture with a medial malleolar fracture is rare, commonly reported with significant soft-tissue injuries and complications such as avascular necrosis (AVN) and osteoarthritis. Due to the preservation of vascular branches from deltoid ligament, there is a slight decrease in AVN of the talus [7]. Here, we present a case report on talar body fracture with a medial malleolar fracture.
Case Presentation
A 30-year-old female presented to our hospital with complaints of pain and swelling over the right ankle joint with difficulty in bearing weight (injury hospital duration of 36 h) following a motor vehicle accident. According to history, the mechanism of injury was axial compression with the supination of the ankle. Initially, the patient was managed with analgesics for pain and trial of closed reduction of fracture followed with short leg cast somewhere else. Then, the patient was referred to our hospital for further management. On examination, there was swelling of the left ankle and foot, associated with no external injury noted; however, the skin over ankle was ecchymosed over medial malleolus. No neurovascular deficit was found. Radiographs of the ankle were taken in anteroposterior and lateral view (Fig. 1), which showed talar body fracture of type 2 Sneppen (classification) with an ipsilateral medial malleolar fracture.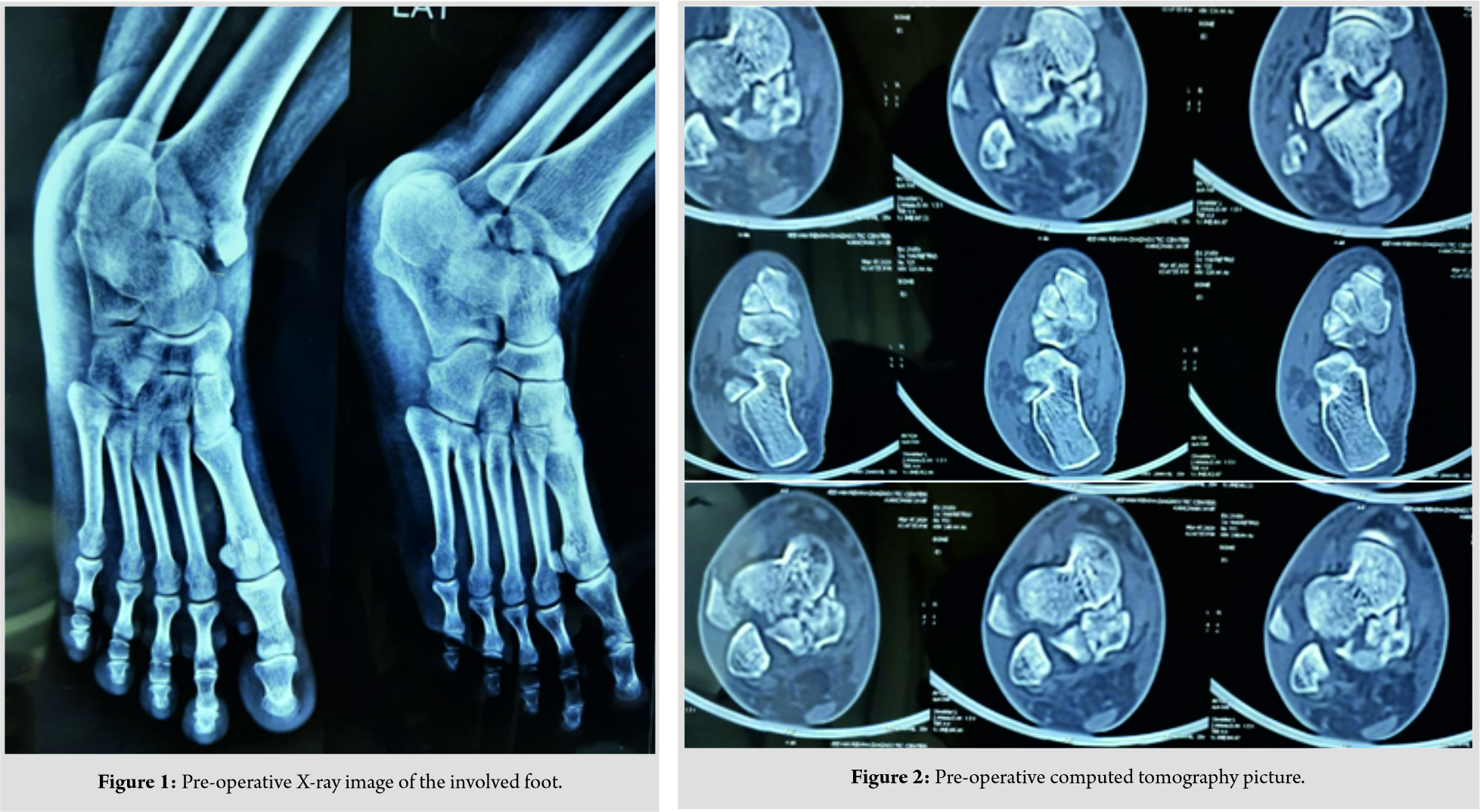
Computed tomography was done to the proper classification of fracture and pre-operative management planning (Fig. 2). An attempt to closed reduction was done in our hospital but was unsuccessful.
Surgical procedure
Surgery was performed by an orthopedic surgeon (foot ankle specialist). The patient was treated by open reduction internal fixation with cannulated cancellous screw fixation for medial malleolus fracture and Herbert screw for talus fracture.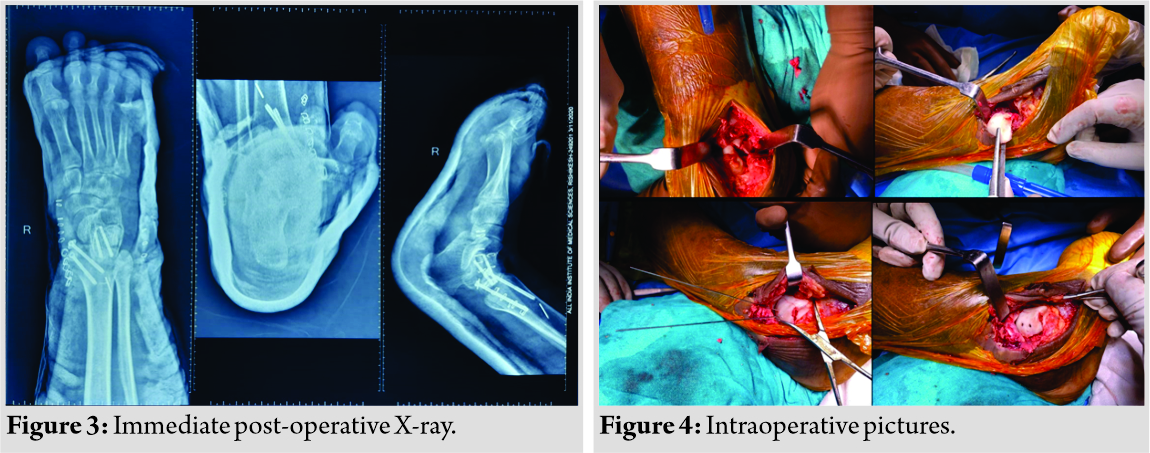
The patient was taken inside operation theater (OT), general anesthesia was given, and the patient was positioned on the OT table (supine), parts prepared, painted, and draped. Both the anteromedial approach, the anterolateral approach was used. The curvilinear incision was extended proximally to ease the reduction of the talar head. The incision was deepened tendons that were safely retracted throughout the procedure. The joint capsule opened. Fractured talus identified and reduction achieved with reduction clamp and found satisfactory on image intensifier appropriate sized Herbert screw applied to hold the reduction. The medial malleolar fracture was fixed with an appropriate sized cannulated cancellous screw after confirming satisfactory reduction (Fig. 3). The wound was washed thoroughly with saline joint congruity was checked and found satisfactory before closing the wound in the layer (Fig. 4).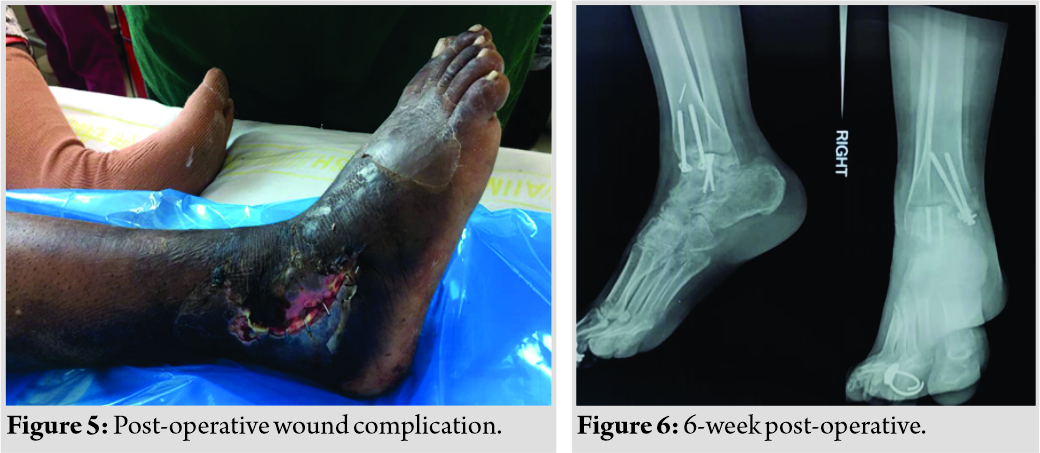
An aseptic sterile dressing is done. Well-padded dressing with below-knee short leg slab was applied. The patient was discharged on post-operative day 2 with advice to continue knee range of motion, static quadriceps exercises, and non-weight-bearing mobilization. The patient was called on post-operative day 14 for suture removal, and the slab was converted to cast. The patient was followed up after 6 weeks cast that was removed and advised to start partial weight-bearing. The patient was kept on a close follow-up after 12 weeks, which was started full weight-bearing. Wound complication (Fig. 5) was encountered on post-operative follow-up and was managed with alternate day sterile dressing, and the result was satisfactory. No signs of AVN appeared on radiographs at 6-week follow-up (Fig. 6), with an absent Hawkins sign and osteosclerosis of the talar dome. After follow-up of 6 months, the ankle showed early arthritic feature and her functional ROM of the ankle was 0−40°.
Discussion
Talus fracture is a rare fracture in day-to-day practice, the second common after calcaneum in tarsal bones, with incidence, ranges from 0.1% to 0.85% of all fractures [1]. High-energy trauma (road traffic accident and fall from height) involving forced dorsiflexion of the ankle cause fracture [2]. More frequently, talus fracture involves neck and body is the least [3, 4, 5, 6]. The combination of talar body fracture and ankle dislocation, along with ipsilateral medial malleolar fracture, is exceptionally rare. Few cases have been reported till now [7, 8, 9, 10]. Axial compression, along with dorsiflexion, is required to fracture talar body along medial malleolus [11]. Our case is of type 2 Sneppen classification, but this classification does not take of status of malleolus into account. If talus fracture is associated with malleolar fracture, the risk of post-traumatic necrosis will decrease due to the preservation of ligament-capsule complex between fractured fragment and malleolus [12] in case of the preserved vascular system and soft tissue. Complications such as skin complication, AVN risk, and post-traumatic arthritis are unpredictable [13]. Open reduction internal fixation with screw modality of treatment [7, 14]. This case reports a rare case of combined right talar body fracture and ankle joint dislocation with an ipsilateral medial malleolar ankle fracture that was successfully managed by open reduction internal fixation with Herbert screw and medial malleolus with a cannulated cancellous screw. Post-traumatic wound dehiscence, AVN of talus, and ankle arthritis were complication but was absent in our case. Patients functional score was satisfactory with a good range of motion.
Conclusion
Talus fracture combined with ankle dislocation is a dare to treating surgeon. Understanding the peculiar vascular supply of talus is a must to treat talus fracture. Our case report showed that the combined body fracture, ankle dislocation with a medial malleolar fracture, should be managed; as soon as, a diagnosis is made to get good functional outcome, even though the incidence of skin complication, AVN risk, and post-traumatic ankle arthritis could not be predicted even though it was absent in our case.
Clinical Message
Combined talar body fracture with a medial malleolar fracture to be managed; as soon as, its detected to get good clinical out.
References
1. Fortin PT, Balazsy JE. Talus fractures: Evaluation and treatment. J Am Acad Orthop Surg 2001;9:114-27.
2. Santavirta S, Seitsalo S, Kiviluoto O, Myllynen P. Fractures of the talus. J Trauma 1984;24:986-9.
3. Sundararajan SR, Badurudeen AA, Ramakanth R, Rajasekaran S. Management of talar body fractures. Indian J Orthop 2018;52:258-68.
4. Ziran BH, Abidi NA, Scheel MJ. Medial malleolar osteotomy for exposure of complex talar body fractures. J Orthop Trauma 2001;15:513-8.
5. Ahmad J, Raikin SM. Current concepts review: Talar fractures. Foot Ankle Int 2006;27:475-82.
6. Juliano PJ, Dabbah M, Harris TG. Talar neck fractures. Foot Ankle Clin 2004;9:723-36.
7. Lahrach K, El Kadi KI, Marzouki A, Boutayeb F. Talar body fracture combined with medial malleolar fracture: A case report and literature review. Pan Afr Med J 2019;32:1-6.
8. Radaideh AM, Audat ZA, Saleh AA. Talar neck fracture with dislocation combined with bimalleolar ankle fracture: A case report. Am J Case Rep 2018;19:320-4.
9. Verettas DA, Ververidis A, Drosos GI, Chatzipapas CN, Kazakos KI. Talar body fracture combined with bimalleolar fracture. Arch Orthop Trauma Surg 2008;128:731-4.
10. Saidi H, Ayach A, Fikry T. Fracture rare du corps du talus: À propos d’un cas et revue de littérature. Med Chir Pied 2008;24:22-4.
11. Alton T, Patton DJ, Gee AO. Classifications in brief: The Hawkins classification for talus fractures. Clin Orthop Relat Res 2015;473:3046-9.
12. Tehranzadeh J, Stuffman E, Ross SD. Partial Hawkins sign in fractures of the talus: A report of three cases. Am J Roentgenol 2003;181:1559-63.
13. Trillat A, Bousquet G, Lapeyre B. Displaced fractures of the neck or of the body of the talus. Value of screwing by posterior surgical approach. Rev Chir Orthop Reparatrice Appar Mot 1970;56:529-36.
14. Mendonca AD, Maury AC, Makwana NK. A simultaneous fracture of the tibia and talar body. Foot Ankle Surg 2004;10:45-7.
 |
 |
 |
 |
 |
 |
| Dr. Nagaraj Manju Moger | Dr. J Pragadeeshwaran | Dr. Sushovan Banerjee | Dr. Pradeep Kumar Meena | Dr. Ankith K.V | Dr. Aman Verma |
| How to Cite This Article: Moger NM, Pragadeeshwaran J, Banerjee S, Meena PK, Ankith K.V, Verma A. Combined Talus Fracture with Medial Malleolar Fracture: A Case report with Review of Literature. Journal of Orthopaedic Case Reports 2020 October;10(7):11-14 |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




