[box type=”bio”] Learning Point of the Article: [/box]
Infection should be ruled out in cases of metal-on-metal total hip replacement migration, with rare or usual pattern, while coexistence of metallosis and infection cannot be excluded in advance..
Case Report | Volume 10 | Issue 1 | JOCR January – February 2020 | Page 93-97 | Ioannis Papaioannou, Dimitrios Ntourantonis, Andreas Baikousis, Vasileios Syrimpeis, Panagiotis Korovessis. DOI: 10.13107/jocr.2020.v10.i01.1654
Authors: Ioannis Papaioannou[1], Dimitrios Ntourantonis[1], Andreas Baikousis[1], Vasileios Syrimpeis[1], Panagiotis Korovessis[1]
[1]Department of Orthopedic, General Hospital of Patras, Greece.
Address of Correspondence:
Dr. Ioannis Papaioannou,
Department of Orthopedic, General Hospital of Patras, Pavlou Pavlopoulou 15, Aroi, Patras, 26331.
E-mail: john-pane1984@hotmail.com
Abstract
Introduction: Total hip arthroplasty (THA) is one of the most successful and cost- effective surgical procedures developed during the last century. Although, chronic infection accompanied with granulomatous allergic reaction from Cobalt (Co),Chromium (Cr) debris after metal-on-metal (MoM) THA implantation can cause severe osteolysis, with subsequent loosening and migration of the implants. There are many cases with intrapelvic migration of these implants, however to best of our knowledge, there is no report of a complete horizontal migration (on frontal plane) of the whole THA prosthesis without disassembly accompanied with severe bone destruction.
Case Report: A 52-year-old female patient was admitted to the authors’ department with inability to weight bear. Because of bilateral developmental hip dysplasia (Type II, Hartofilakidis classification) she underwent THA bilaterally at another institution about 20 years ago. On admission, the initial plain roentgenogram of the hip was impressive, disclosing sclerotic, osteolytic lesions, associated with perforation of the lateral and medial cortices of the proximal femur, and migration to 90-degree horizontal position on the frontal plane of the whole prosthesis. Based on the preoperative planning, the implants were removed through a small medial longitudinal approach accompanied with lateral debridement. The patient denied revision surgery and the final result was a resection arthroplasty.
Conclusion: THA is one of the most clinically successful surgical procedures, although inappropriate patient or implant selection for primary hip arthroplasty can lead to the necessity of complex revision surgery after late-diagnosed postoperative complications such as infection, loosening, and migration of the prosthesis. A well-designed preoperative plan is mandatory when handling such cases. Clinicians when faced with THA migration, rare or common, should definitely rule out the infection. Adverse reactions to metal debris (ARMD) can also lead to significant displacement of a hip prosthesis, although coexistence of metallosis and infection cannot be excluded in advance.
Keywords: hip arthroplasty, septic, migration, horizontal, metal-on-metal.
Introduction
Total hip arthroplasty (THA) is one of the most successful and cost-effective surgical procedures developed during the past century [1]. The frequency of THA has risen dramatically over the past two decades, although this surgery may be associated with early and late complications. Periprosthetic joint infection (PJI) is a devastating surgical complication, both for the patient and surgeon [2]. More specifically, the implantation of cementless THAs with metal-on-metal (MoM) bearings was reported to be associated with a high failure rate due to hypersensitivity reaction to Cobalt (Co), Chromium (Cr) (Co-Cr) components of this articulation. In the early 2000, MoM THA articulation was globally abandoned due to the reported increased failure rate [3, 4]. It was shown that the allergic hip tissues reaction due to Co-Cr and increased debris causes focal periprosthetic osteolysis, with subsequent aseptic loosening and migration of the cup and stem THA implants. In this paper, we report a very rare type of septic loosening and subsequent migration of both cementless femoral stem and screw socket without disassembly following chronic deep infection and fistula formation of a Zweymuller-SLTHA with low carbide MoM bearing surfaces. The THA components were gradually migrated distally and took a horizontal position on the frontal plane, almost perpendicular to the longitudinal femoral axis. In revision surgery, the Alloclassic-Zweymuller stem was found to have perforated proximally the femoral canal wall. Through a medial approach close to the adductors muscles, the migrated screw socket cup was easily found and removed through a longitudinal incision. In the histological examination, no granulomatous reactions, typical for Co-Cr metal debris or pseudotumor, were found in the retrieved specimens around the removed hip implants, while no occult scratches and wear were found in the articulating surfaces. Both femoral stem (Alloclassic®Zweymüller® Hip Stem, Zimmer Biomet, Warsaw, Indiana, USA) and screw socket (BICON-PLUS™, Smiths and Nephew, London, United Kingdom) were easily removed. To the best of our knowledge, this type of THA migration has not been previously reported and emphasizes the significance of post-operative follow-ups, particularly in patients who received cementless THAs with MoM articulations and the value of an early revision surgery before such severe destruction of femoral and acetabulum anatomy occurs.
Case Report
A 52-year-old female patient was admitted to the authors’ department with hip and thigh pain associated with the inability to full weight bearing on her right leg. In the previous anamnesis, there was no trauma but bilateral congenital developmental hip dysplasia. She gradually became unable to walk during the past 2 weeks. On admission, physical examination revealed no restriction in passive hip motion, but the pain in her right groin.On inspection, there was drainage from a chronic sinus located laterally on the right thigh at the distal third of the previous surgical scar incision. Because of bilateral developmental hip dysplasia (Type B according to Hartofilakidis classification), she underwent THA bilaterally at another institution. Both THAs were performed through a modified anterolateral approach about 20 and 21 years ago. Both cementless THAs were of the type Zweymüller Alloclassic (Alloclassic®Zweymüller® Hip Stem, Zimmer Biomet, Warsaw, Indiana, USA) with Metasul Alloy MoM bearing surfaces and 32 mm ball head.The cup was a cementless titanium screw socket Alloclassic®Zweymüller®. 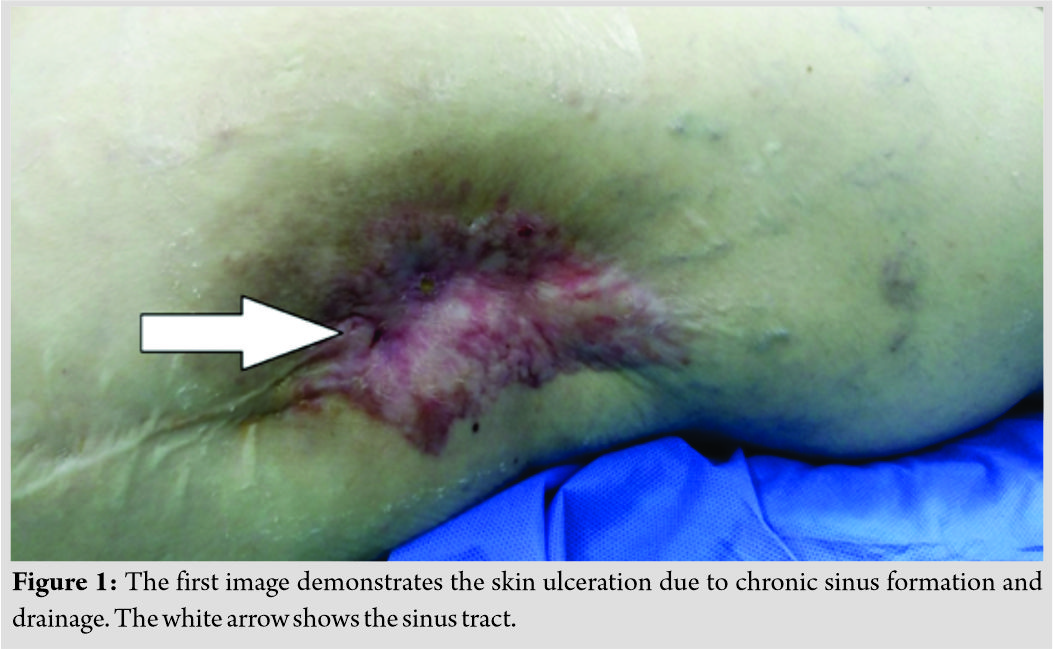 According to the patient’s report, sinus formation and subsequent drainage begun around 3 years before this admission and was treated with oral antibiotics. On admission, the patient had no fever, and the sinus showed a rather mild secretion (Fig. 1), the erythrocyte sedimentation rate (ESR) was elevated to 68 mm/h (normal limits: 0–20 mm/h), the C-reactive protein (CRP) was 3.2 mg/dL (normal limits: 0–0,5 mg/dL), and the white blood cell count was 8.14 K/μL (normal limits: 4–10 K/μL), while the neutrophils were 4.63K/μL (normal limits: 2–7,5 K/μL). On admission, the initial plainroentgenograms of the hip disclosed sclerotic and osteolytic lesionsin both femur and acetabulum, with perforations through the lateral and medial cortices of the proximal femur, and migration of the Zweymuller stem together with the screw socket and ball head to a 90° horizontal position in relation to the longitudinal femoral axis on the frontal plane of the whole prosthesis (Fig. 2).
According to the patient’s report, sinus formation and subsequent drainage begun around 3 years before this admission and was treated with oral antibiotics. On admission, the patient had no fever, and the sinus showed a rather mild secretion (Fig. 1), the erythrocyte sedimentation rate (ESR) was elevated to 68 mm/h (normal limits: 0–20 mm/h), the C-reactive protein (CRP) was 3.2 mg/dL (normal limits: 0–0,5 mg/dL), and the white blood cell count was 8.14 K/μL (normal limits: 4–10 K/μL), while the neutrophils were 4.63K/μL (normal limits: 2–7,5 K/μL). On admission, the initial plainroentgenograms of the hip disclosed sclerotic and osteolytic lesionsin both femur and acetabulum, with perforations through the lateral and medial cortices of the proximal femur, and migration of the Zweymuller stem together with the screw socket and ball head to a 90° horizontal position in relation to the longitudinal femoral axis on the frontal plane of the whole prosthesis (Fig. 2).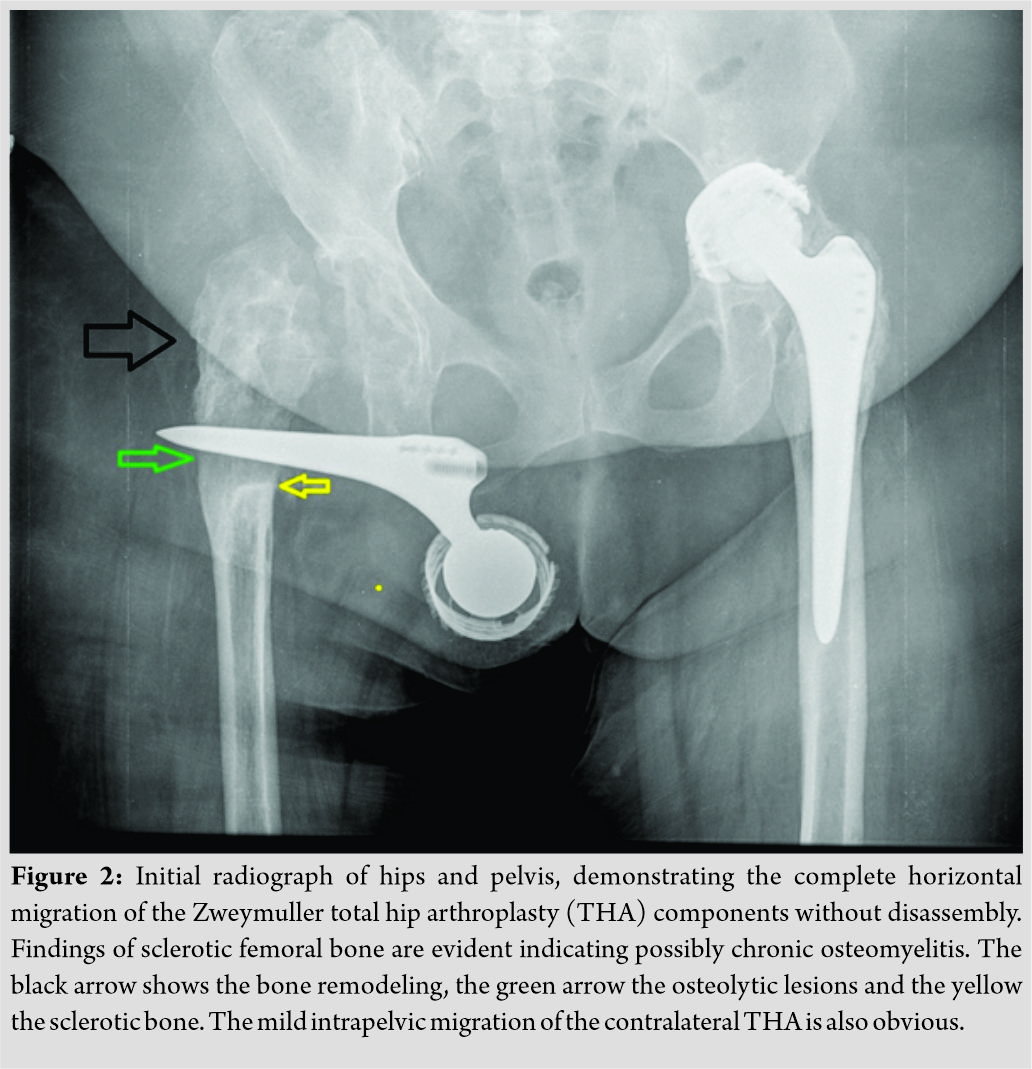 A computed tomography (CT) scan and a CT-angiography were performed, to evaluate the exact location of the migrated THA components and any proximity of them to the great leg vessels. CT scan disclosed that the stem and cup were located on the floor of the adductor femoral muscles, subcutaneously close to the medial third of the groin area. The proximal one-third of the femur was perforated by the stem in both medial and lateral cortices (Fig. 3).
A computed tomography (CT) scan and a CT-angiography were performed, to evaluate the exact location of the migrated THA components and any proximity of them to the great leg vessels. CT scan disclosed that the stem and cup were located on the floor of the adductor femoral muscles, subcutaneously close to the medial third of the groin area. The proximal one-third of the femur was perforated by the stem in both medial and lateral cortices (Fig. 3).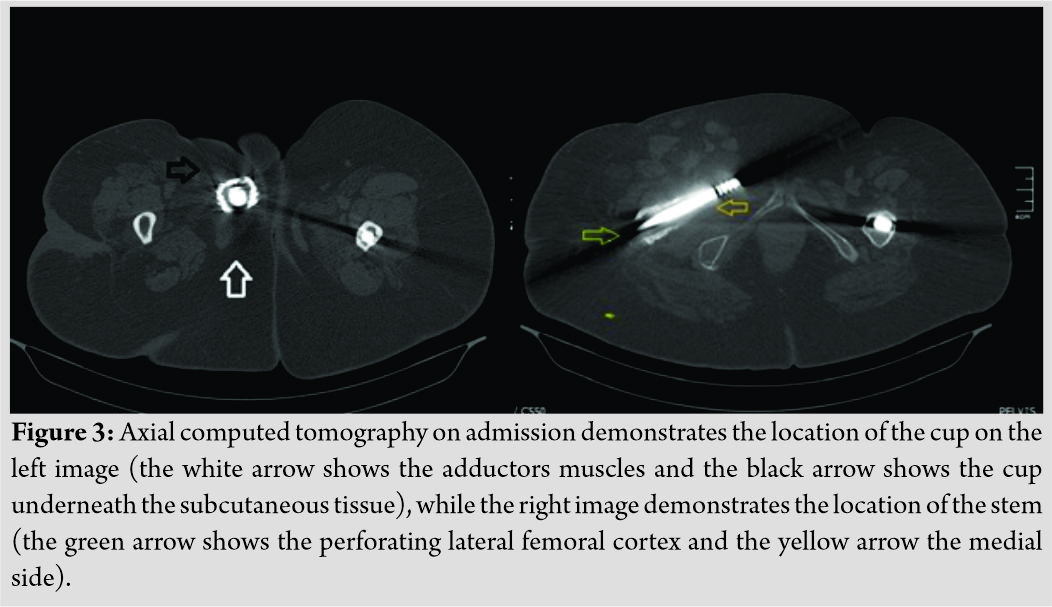 CT angiography revealed the proximity of the screw socket to the superficial branch of the common femoral artery (Fig. 4).
CT angiography revealed the proximity of the screw socket to the superficial branch of the common femoral artery (Fig. 4). 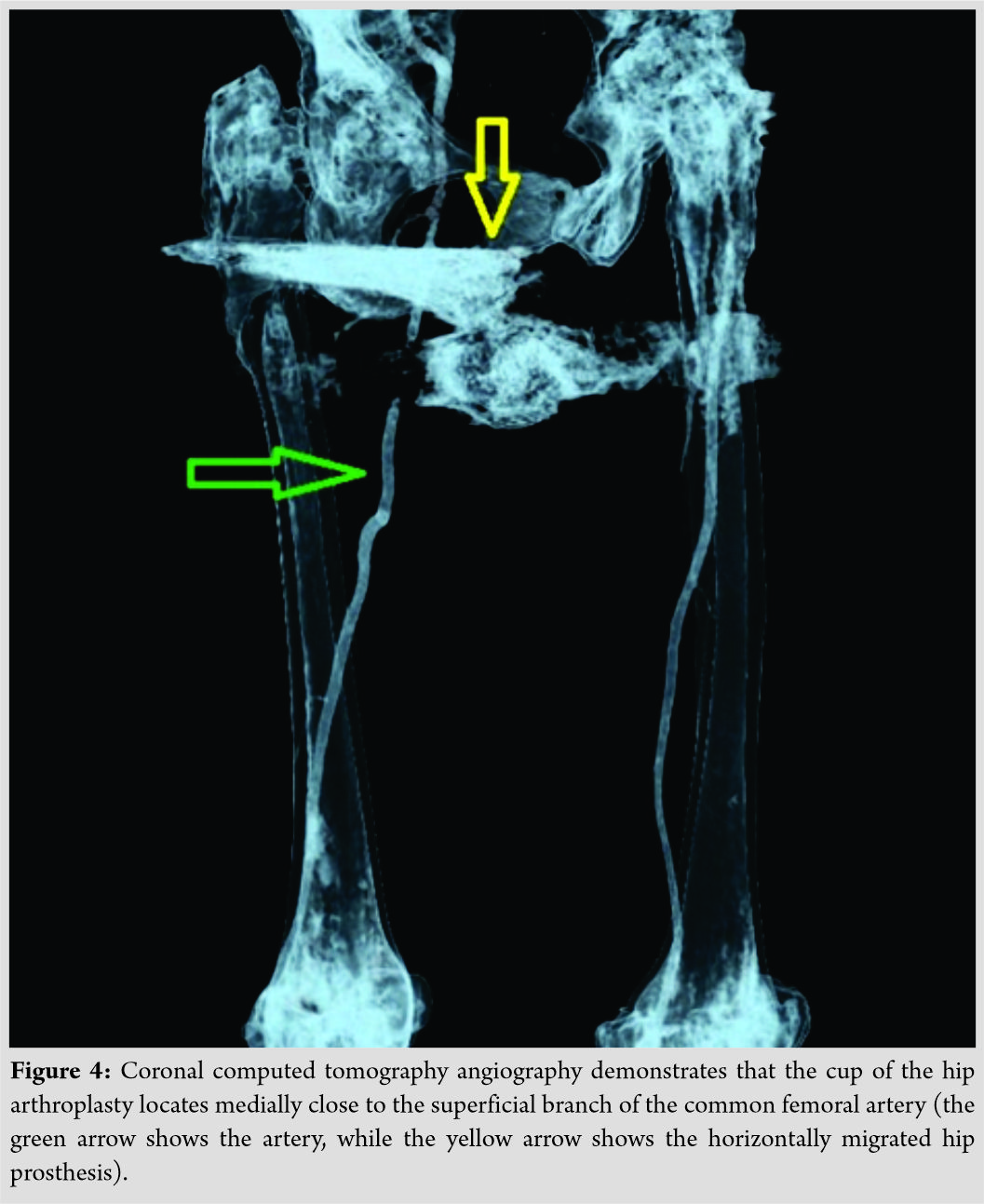 Through a short longitudinal incision above the dislocated THA, the cup and the femoral ball head were found without disassembly (Fig. 5).
Through a short longitudinal incision above the dislocated THA, the cup and the femoral ball head were found without disassembly (Fig. 5).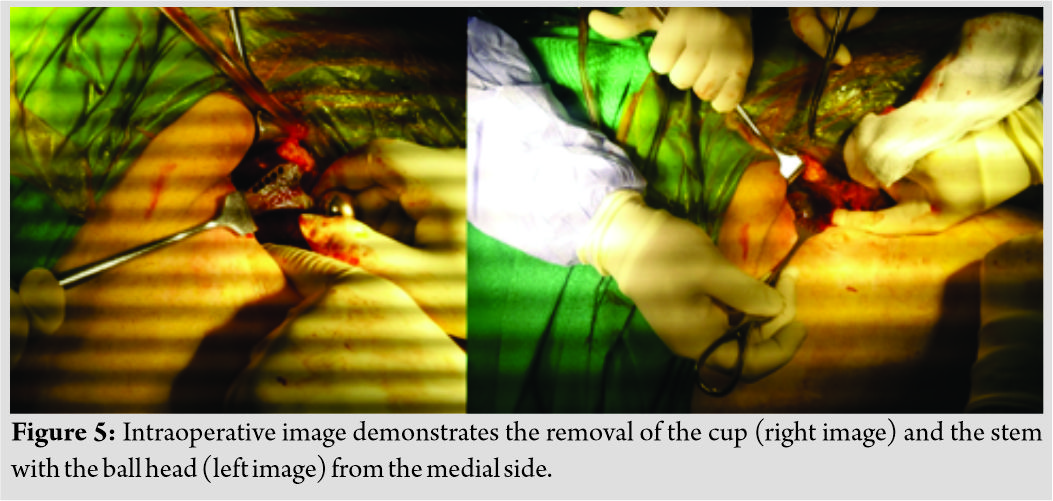 Samples from periprosthetic granulomatous tissues and fluid for culture and pathology were taken. Debridement with radical excision of the sinus was subsequently made and finally a continuous irrigation and drainage system were placed. Traces of tissue metallosis but no pseudotumor were found intraoperatively (Fig.6).
Samples from periprosthetic granulomatous tissues and fluid for culture and pathology were taken. Debridement with radical excision of the sinus was subsequently made and finally a continuous irrigation and drainage system were placed. Traces of tissue metallosis but no pseudotumor were found intraoperatively (Fig.6).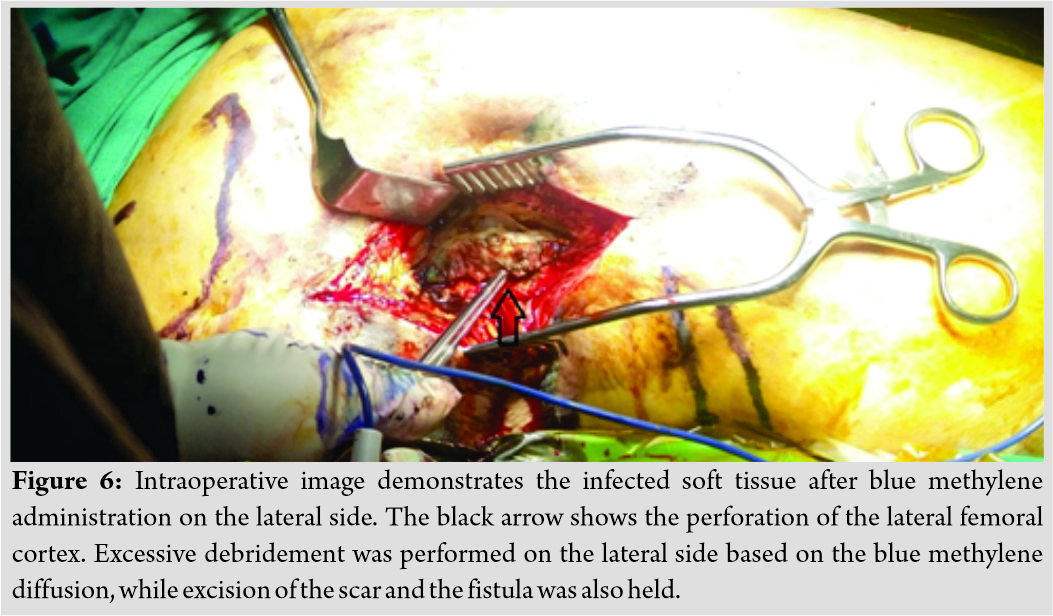 The wounds healed uneventfully. No cement spacer was placed, due to our patient’s refusal for revision THA surgery. The cultures of the retrieved specimens revealed a polymicrobial infection of Methicillin-resistant Staphylococcus aureus and proteus mirabilis, while biopsy revealed tissue infiltration of polymorphonuclear leukocytes and macrophage cells, due to both infection and adverse reaction to metal debris (ARMD). The histology of the thigh scar was negative for malignancy. We administrated 6 weeks of intravenous vancomycin and sulfamethoxazole plus trimethoprim followed by 6 weeks’ oral administration of linezolid plus trimethoprim and sulfamethoxazole. The final radiographic result was a resection arthroplasty (Fig. 7).
The wounds healed uneventfully. No cement spacer was placed, due to our patient’s refusal for revision THA surgery. The cultures of the retrieved specimens revealed a polymicrobial infection of Methicillin-resistant Staphylococcus aureus and proteus mirabilis, while biopsy revealed tissue infiltration of polymorphonuclear leukocytes and macrophage cells, due to both infection and adverse reaction to metal debris (ARMD). The histology of the thigh scar was negative for malignancy. We administrated 6 weeks of intravenous vancomycin and sulfamethoxazole plus trimethoprim followed by 6 weeks’ oral administration of linezolid plus trimethoprim and sulfamethoxazole. The final radiographic result was a resection arthroplasty (Fig. 7). 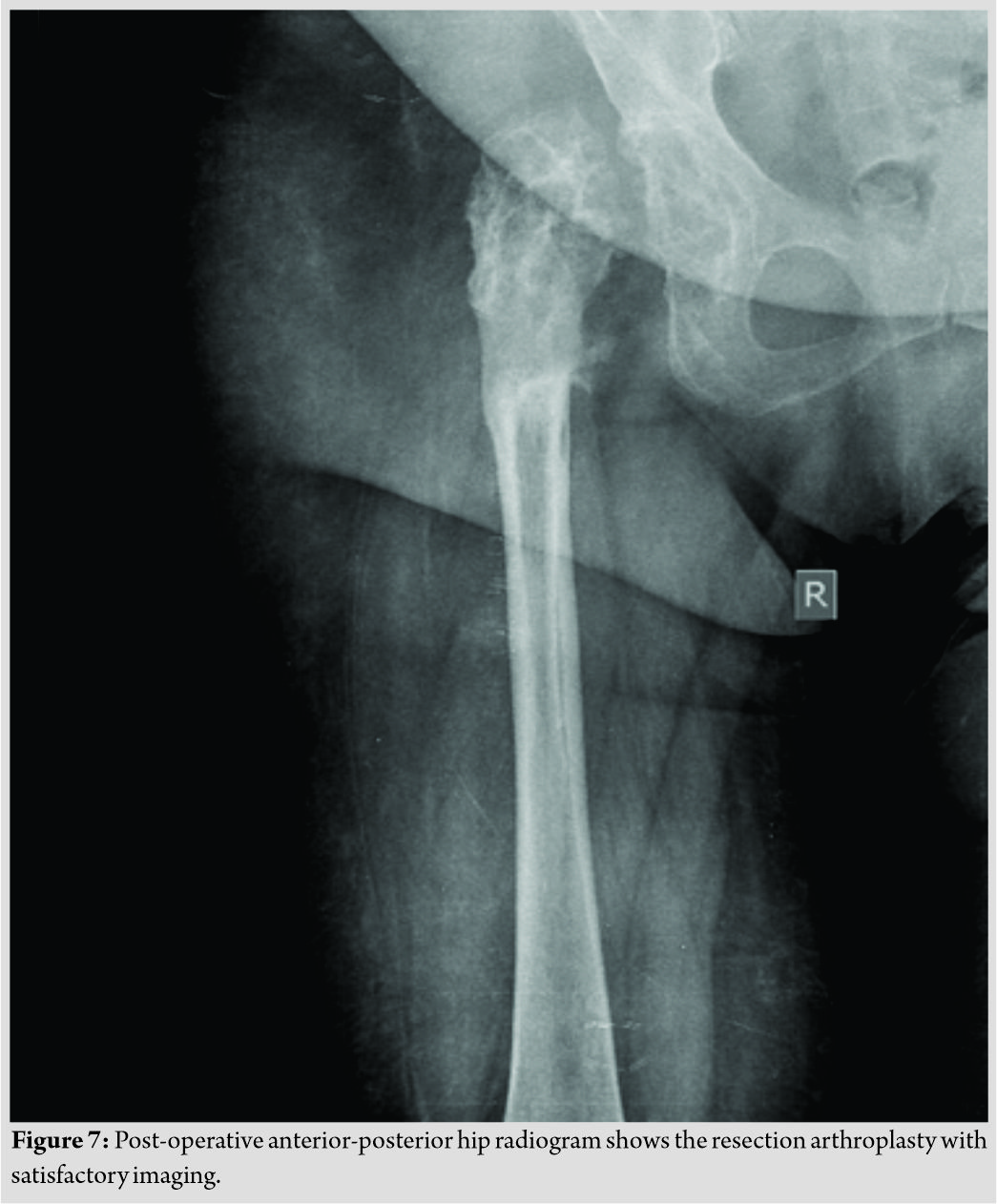 Fortunately, our patient was able to partially bear weight, with the aid of crutches, 1 month after surgery. The CRP and ESR returned to the normal levels, and our patient was discharged on day 51 after admission. Our patient had followed up, at 3 and 12 months postoperatively, with negative inflammation markers, no sinus formation, and satisfactory clinical and radiographic evaluation (Fig. 7).
Fortunately, our patient was able to partially bear weight, with the aid of crutches, 1 month after surgery. The CRP and ESR returned to the normal levels, and our patient was discharged on day 51 after admission. Our patient had followed up, at 3 and 12 months postoperatively, with negative inflammation markers, no sinus formation, and satisfactory clinical and radiographic evaluation (Fig. 7).
Discussion
THA is one of the most clinically successful and cost-effective medical procedures developed during the past century. Before 2011, there was no consistent, standard or universal report of the complications of this surgery. In 2011, the THA workgroup was established to summarize the complications and adverse events [2]. Based on this work, the hip society endorsed 19 complications/adverse events after THA, among them dislocation/instability, deep PJI, osteolysis, and implant loosening. To prevent complications associated with THA, intensive post-operative follow-up observation is mandatory. Patients who do not understand the risks and are not prepared to comply with the post-operative follow-up should be excluded from the surgical intervention. The same workgroup stratified these complications from Grades 1 to 5. Over Grade 2 is described that the complication requires a prolonged hospital stay, unplanned readmission with or without surgical intervention, limb-threatening or life-threatening event, and finally death. In 2018, the diagnostic criteria of PJI were updated based on the conclusions of an international consensus meeting on the musculoskeletal infection. Surgeons handling such cases should be aware of this algorithm to successfully diagnose a PJI [5]. Bearing surface choice is paramount of importance for good long-term survivorship of a THA and hip surgeons should be well informed. THAs with MoM weight-bearing surfaces have the shortest long-term survivorship among different bearings surfaces [4]. Patients who received MoM THA should be informed about the risk of becoming sensitive to the MoM articulation. Hypersensitivity reactions to these patients are possible. Willert et al. [3] found an immunological response that was characterized by a diffuse and perivascularly oriented infiltration of lymphocytes accompanied by plasma cells and eosinophilic granulocytes, swelling of the vascular endothelium, localized bleeding, fibrin exudation, necrosis, and macrophages with drop-like inclusions. This reaction is a delayed-type IV cell-mediated hypersensitivity response. These reactions, which are grouped under the term ARMD, have been called inflammatory pseudotumor, aseptic lymphocytic vasculitis associated lesion, and metallosis. The radiographic and clinical consequences of these reactions are the osteolysis and the aseptic loosening of the prosthesis. Constant follow-up and early revision surgery can prevent further more complex complications, such as prosthesis migration. Apart from the obvious deep infection, our patient had a unique migration pattern of both femoral and acetabular components without disassembly. Literature review did not reveal any similar case, although we found many cases with intrapelvic migration of all kinds of THA components, such as bone cement [6], femoral stem [7], hemiarthroplasty [8], acetabular cup, and entire total hip replacement (THR) migration. Until now, the most impressive case of hip prosthesis migration was one published in 1996, which concerned an entire hip prosthesis retroperitoneal migration to the subhepatic space, without any complications [9]. Most of these cases in the literature were accompanied by infection and sepsis. Infection should be first ruled out in cases of hip prosthesis migration, although acetabular protrusion can occur due to many bone disorders such as rheumatoid arthritis, ankylosing spondylitis, osteomalacia, Marfan’s syndrome, Paget and Otto diseases, and secondary to irradiation [10]. Several studies supported that high metal ion concentrations released by MoM bearings might promote bacterial infections in patients with MoM THR [11, 12]. MoM THR devices are associated with soft-tissue inflammatory reactions to metal debris, the ARMD. Τhe aforementioned soft-tissue reactions accompanied by infection-induced osteolysis can cause severe destruction of the joint [12]. The impressive migration of the prosthesis presented in our case is attributed to the concomitant bone loss due to the ARMD and the infection, as it turns out from the histology. Furthermore, we hypothesize that as the patient continued to bear weight, the THR migrated gradually to varus position and the stem perforated the damaged lateral femoral and medial cortex, to take the final horizontal position. The infection-induced osteolysis of the acetabulum and the proximal femur, accompanied by the bone loss due to the ARMD, led to this unique migration of the MoM THR. Before planning complex surgery to remove or to revise migrated hip prostheses, the anatomy of the acetabulum and the vascular structures must be well known. Hip arthroplasty revisions are responsible for 39% of the vascular injuries involving hip arthroplasties. The displacement of the prosthesis and the sharp outer surface of the screw socket in an infection milieu may theoretically increase the risk for possible great vascular injury [13]. CT angiography is the most appropriate examination to evaluate the integrity and patency of vascular structures. The urinary and digestive systems should also be evaluated in cases of intrapelvic migration. The surgeons should adjust their surgical approach according to the findings of the specific case. Infection should be ruled out, and bone loss should be taken into consideration in cases of revision [14]. The difficulty of managing such complex cases indicates the need for constant THA monitoring before life-threatening complications arise. The literature supports that improving patient selection for primary arthroplasty may reduce the burden of complex arthroplasty revision [15].
Conclusion
THA is one of the most clinically successful surgical procedures, although inappropriate patient or implant selection for primary THA can lead to the necessity of complex revision surgery after late-diagnosed post-operative complications such as infection, loosening, and migration of the prosthesis. A well-designed pre-operative plan is mandatory when handling such cases. Clinicians, when faced with THA migration, rare or common, should definitely rule out the infection. ARMD can also lead to significant displacement of a hip prosthesis, although the coexistence of metallosis and infection cannot be excluded in advance, as in our case.
Clinical Message
This unique pattern of THA migration emphasizes the necessity of post-operative follow-ups, particularly in patients received arthroplasties with MoM bearing surfaces and the value of an early revision surgery before a severe destruction of hip joint occurs. Proper pre-operative planning is mandatory as the coexistence of metallosis and infection cannot be excluded in advance, as in our case.
References
1. LearmonthID, YoungC, RorabeckC. The operation of the century: Total hip replacement.Lancet2007;370:1508-19.
2. HealyWL, IorioR, ClairAJ, PellegriniVD, DellaValle CJ, BerendKR. Complications of total hip arthroplasty: Standardized list, definitions, and stratification developed by the hip society.Clin OrthopRelat Res2016;474:357-64.
3. WillertHG, BuchhornGH, FayyaziA, FluryR, WindlerM, KösterG, et al. Metal-on-metal bearings and hypersensitivity in patients with artificial hip joints. A clinical and histomorphological study.J Bone Joint Surg Am2005;87:28-36.
4. KorovessisP, PetsinisG, RepantiM, RepantisT. Metallosis after contemporary metal-on-metal total hip arthroplasty. Five to nine-year follow-up.J Bone Joint Surg Am2006;88:1183-91.
5. ParviziJ, TanTL, GoswamiK, HigueraC, DellaValle C, ChenAF, et al. The 2018 definition of periprosthetic hip and knee infection: An evidence-based and validated criteria.J Arthroplasty2018;33:1309-14.e2.
6. ThompsonNW, CollearyG, WilsonDS, CroneMD, BeverlandDE. Migration of intrapelvic cement after total hip arthroplasty.J Arthroplasty2002;17:382-3.
7. YagdiS, KazimogluC, DirimB, BulutT, SenerM. Retroperitoneal migration of a septically loose femoral component.J Arthroplasty2011;26:977.e17-20.
8. LimJB, AngCL, PangHN. Acetabular prosthetic protrusio after bipolar hemi-arthroplasty of the hip: Case report and review of the literature.J Orthop Case Rep2016;6:28-31.
9. MuñozVives JM, MartíGarin D, GirventMontllor R. Subhepatic migration of a hip prosthesis.J Bone Joint Surg Br1996;78:152-3.
10. KindynisP, GarciaJ. Protrusioacetabuli. An update on the primary and secondary acetabular protrusion.J Radiol1990;71:415-24.
11. Pace F, Randelli F, Serrao LB. Infection rate in ASR metal on metal hip replacement: Possible correlation between high serum levels of metal ions and infection. Orthop Proc 2013;95-B Suppl 34:495.
12. JuddKT, NoiseuxN. Concomitant infection and local metal reaction in patients undergoing revision of metal on metal total hip arthroplasty.Iowa Orthop J2011;31:59-63.
13. CalligaroKD, DoughertyMJ, RyanS, BoothRE. Acute arterial complications associated with total hip and knee arthroplasty.J Vasc Surg2003;38:1170-7.
14. GirardJ, BlaironA, WavreilleG, MigaudH, SennevilleE. Total hip arthroplasty revision in case of intra-pelvic cup migration: Designing a surgical strategy.OrthopTraumatol Surg Res2011;97:191-200.
15. BottleA, ParikhS, AylinP, LoefflerM. Risk factors for early revision after total hip and knee arthroplasty: National observational study from a surgeon and population perspective.PLoS One2019;14:e0214855.
 |
 |
 |
 |
 |
| Dr. Ioannis Papaioannou | Dr. Dimitrios Ntourantonis | Dr. Andreas Baikousis | Dr. Vasileios Syrimpeis | Dr. Panagiotis Korovessis |
| How to Cite This Article: Papaioannou I, Ntourantonis D, Baikousis A, Syrimpeis V, Korovessis P. Unique Migration of a Septic Loosened Metal-on-metalCementless Total Hip Arthroplasty: A Case Report and Literature Review. Journal of Orthopaedic Case Reports 2020 Jan-Feb;10(1): 93-97. |
[Full Text HTML] [Full Text PDF] [XML]
[rate_this_page]
Dear Reader, We are very excited about New Features in JOCR. Please do let us know what you think by Clicking on the Sliding “Feedback Form” button on the <<< left of the page or sending a mail to us at editor.jocr@gmail.com




